Abstract
Objectives:
This study aimed to assess healthcare professionals’ awareness and acceptance of telemedicine residing in Pakistan.
Materials and Methods:
A cross-sectional study was conducted across Pakistan from November 2021 to March 2022. Data entry was done through a self-administered questionnaire. In this survey, the non-probability purposive sampling method was adopted. Medical doctors from all specialties that fall into the age category of 20–60 years were included in this study. Statistical Package for Social Sciences (SPSS) version 22.0 was used for univariate data analysis.
Results:
Among the 860 healthcare professionals who received the survey, 198 responded (23.0% response rate). The mean ± SD age of the participants was 31.16 ± 8.56. The results were found to be statistically significant for knowledge about telemedicine among healthcare professionals workplace, that is, healthcare professionals working in the private sector indicated a high level of awareness regarding telemedicine as compared to those in the public sector (p = 0.03). A significant difference (p-value ⩽ 0.05) in knowledge was seen among doctors working in the public sector and those working in a private setup. Results indicate significant positive associations between telemedicine utilization and perceived benefits over disadvantages (β = 1.03, p = 0.017), reliance among healthcare professionals (β = 1.22, p = 0.008), and enhancement in healthcare quality (β = 1.42, p = 0.001). Moreover, familiarity with telemedicine correlates strongly with its usage (β = 2.56, p < 0.000).
Conclusion:
Overall, healthcare professionals exhibited satisfactory knowledge regarding telemedicine and showed an accepting attitude toward telemedicine. Our study recommends enhancing the importance of Telemedicine training at the Healthcare professionals’ level to produce quality service delivery in healthcare organizations.
Plain Language Summary
The aim of this study, was to evaluate healthcare professionals’ knowledge and acceptance of telemedicine in Karachi, Pakistan. A cross-sectional survey was carried out between November 2021 and March 2022, and 198 out of 860 healthcare professionals responded (representing a 23.0% response rate). The participants’ average age was 31.16 years. The results showed that healthcare professionals in the public and private sectors differed significantly in their awareness of telemedicine, with the former group having higher awareness levels. Most of the medical professionals showed adequate understanding and acceptance of telemedicine. However, in order to improve service delivery in healthcare organizations, the study emphasizes the necessity for improved telemedicine awareness and training among healthcare providers, especially in the public sector. The findings highlighted how crucial it is to integrate telemedicine within medical education.
Background
Telemedicine represents a pivotal aspect of digital healthcare delivery, situated within the broader realm of digital health, which encompasses the utilization of electronic devices and digital data across various healthcare domains. Specifically, telemedicine involves the provision of medical services across distances or time zones, facilitated by information and communication technologies. 1 In addition to these remote care approaches, a plethora of mobile-based applications have emerged, offering invaluable support to healthcare professionals (HCPs) in their daily duties. These applications streamline tasks such as time management, information access and storage, health promotion, education, communication, monitoring, data organization, and decision-making. 2
The landscape of digital health applications is rapidly expanding, with approximately 97,000 health-related apps available on platforms such as Apple and Google, and this number continues to grow by about 1000 apps monthly, projecting a 25% annual increase. 3 Leveraging Information and Communication Technology (ICT) and mobile interventions prove to be not only cost-effective but also operationally efficient, fostering advancements in healthcare services. Recognizing the transformative potential of mobile technologies, the World Health Organization (WHO) highlights their role in enhancing public health service delivery, attributing this to factors such as user-friendliness and widespread acceptance among both healthcare providers and recipients. 4
The evolving landscape of ICT has ushered in various systems tailored for healthcare settings, facilitating tasks such as appointment scheduling via mobile devices. 5 Consequently, stakeholders across diverse sectors, including HCPs, Information Technologists, Social Scientists, Public and Private Organizations, and Policy makers, are actively seeking avenues to harness mobile health (m-Health) technologies, opening up new dimensions in healthcare provision. Notably, the proliferation of mobile phones over the past decade has been remarkable, with global subscriptions exceeding 5.11 billion and projected to surpass 50 billion by 2020. 6 According to WHO, this accessibility extends beyond developed nations, permeating even into underserved regions, marking a significant juncture wherein technology drives transformative shifts in healthcare organizational frameworks. 7
The trajectory of telemedicine has been marked by rapid development, yielding cost-effective interventions and expanded functionalities. Consequently, both developed and developing nations have embraced mobile health interventions, albeit with sparse literature on user knowledge and experiences. For instance, studies assessing knowledge levels regarding mobile health applications have been conducted, revealing varying degrees of awareness and adoption rates. In Ghana, a medical college survey demonstrated a noteworthy level of awareness and potential incorporation of m-Health into mainstream healthcare systems. 8 Similarly, in Korea, although the utilization of m-Health among older adults is increasing globally, some individuals still encounter challenges due to limited expertise, despite their self-confidence in usage. 9
Exploring HCPs’ perspectives, studies in Finland and Lithuania underscore nurses’ familiarity with mobile health technologies and emphasize the importance of features such as automated data recording and transmission. 6 In Ethiopia, a significant proportion of health professionals exhibited good knowledge and awareness of telemedicine services, with factors such as information sources, information technology (IT) support, and training influencing their proficiency and awareness levels. 10
Telemedicine applications in underdeveloped nations could be a powerful tool for delivering basic health care to large populations and bridging the gap between rural areas and specialist institutions, which are mainly located in metropolitan areas. 11 Since the onset of COVID-19 in Pakistan, there has been a noticeable surge in demand for telehealth services. 12 Despite telemedicine’s ability to overcome many barriers to healthcare delivery in developing countries, Pakistan has yet to fully capitalize on this progress. 13 The exponential growth of the population, coupled with a disorganized healthcare system, has led to an unequal distribution of healthcare services. Telemedicine has the potential to enable Pakistan’s healthcare system to employ innovative and cost-effective techniques to revolutionize healthcare delivery across the country. 14
Given the pivotal role of user knowledge in driving mobile technology adoption, there is a pressing need to continually assess and enhance the general population’s understanding and proficiency in utilizing these technologies. Hence, this study aimed to assess HCPs’ awareness and acceptance of telemedicine residing in Pakistan.
Materials and methods
Summary
This cross-sectional study conducted in Pakistan between November 2021 and March 2022 aimed to investigate the awareness and acceptance of telemedicine among HCPs aged 20 to 60. Out of 860 professionals surveyed, 198 responded, resulting in a 23.0% response rate. The participants, with a mean age of 31.16 ± 8.56, displayed statistically significant differences in telemedicine knowledge based on their workplace, with those in the private sector exhibiting higher awareness (p = 0.03) than their counterparts in the public sector. Overall, most HCPs demonstrated satisfactory knowledge and a positive attitude toward telemedicine. Notably, this study underscores the importance of telemedicine training for HCPs to enhance service quality in healthcare organizations. Bridging the knowledge gap between public and private sector HCPs is crucial for promoting the widespread adoption of telemedicine and improving healthcare delivery in Pakistan.
Study design, study population, and setting
This study adopted a cross-sectional study design to assess the knowledge and attitude of HCPs toward telemedicine, across Pakistan from November 2021 to March 2022. The study site was Jinnah Sindh Medical University (JSMU) where health professionals such as medical doctors and affiliated medical professionals from all specialties that fall into the age category of 20–60 years were included. However, medical doctors who retired and lacked smartphone and Internet exposure were excluded from the study.
Study sampling
The non-probability purposive sampling was employed, which targeted HCPs from primary, secondary, and tertiary healthcare centers across Pakistan. The sample size of 180 was calculated using Open Epi version 3.01, with an 86.5% prevalence 15 and 95% confidence interval. In the sample size, 10% was added for missed responses and incomplete forms, and the final sample size was calculated to be 198. 16
Data collection tool and procedure
We utilized a pre-existing data collection tool 17 that had been previously validated and tailored it to suit the context of our study, ensuring it was more applicable to our sample. Data entry was accomplished through a self-administered questionnaire created on Google Forms. The questionnaire was structured into four sections: a consent form, demographics, and questions assessing knowledge and attitude. We assigned six categories to assess participants’ responses to telemedicine services. Each category had different questions, and participants’ response to each item was recorded through a “Yes or No” answer choice. The categories were reliability of telemedicine, benefits of telemedicine, data storage, and sharing, perceived limitations of telemedicine, training need of HCPs, and willingness to use telemedicine services in the future.
This instrument was validated by two community health experts and one biostatistician. For each question, the experts rated its relevance and clarity on a 4-point Likert-type scale. A Content Validity Index (CVI) rating of 0.8 or higher was deemed acceptable for both individual items and the overall scale. Items that did not meet this threshold were either revised for clarity or eliminated from the questionnaire entirely.
Following the content validity assessment, we conducted a pilot study involving 20 individuals to identify any ambiguous questions and to gauge the reliability of the questionnaire. The Cronbach’s alpha coefficient for internal consistency was calculated to be 0.73, indicating that the questionnaire possessed acceptable internal reliability.
A research coordinator, a medical student involved in a university research project, was appointed to oversee the data collection process and provide training to the individuals responsible for collecting the data.
Data analysis
The collected data were de-identified to maintain the confidentiality of the participants. The data were then thoroughly reviewed, and any missing variables or wrong entries were identified, and the respondents were reached for those variables. If the missing variables were greater than 30% in the dataset of a respondent, then that dataset was excluded from the final data analysis. We define awareness of telemedicine as “Any person who is aware of Telemedicine (TM) or telehealth as healthcare services at a distance using electronic means” and Acceptance of telemedicine as who is willing to use it in the future. Statistical Package for Social Sciences (SPSS) version 22.0 was used for univariate data analysis. Descriptive statistics were calculated in the form of frequency and percentages and presented in the form of tables. Mean and standard deviation was calculated for continuous variables, that is, age of participants. Composite variables for knowledge and attitude sections were created in SPSS. For knowledge, the variables incorporated were location-independent access to healthcare services, reliability of these services, and they do upgrade the quality of healthcare delivery to create a single variable with outcomes of high- and low-awareness levels. Similarly, for the attitude of HCPs, the variables were the integration of telemedicine in the medical curriculum, and future implications to create an outcome variable with high- and low-acceptability levels. The Chi-square test was applied to assess any associations between categorical variables. A p-value less than 0.05 was considered significant. The study reporting adheres to the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) checklist (Annexure 1).
Results
We circulated the electronic questionnaire to different JSMU medical doctors and affiliated medical professionals from all specialties on social media platforms (WhatsApp), which comprised a total of 860 HCPs, 198 responded (23.0% response rate), out of which 196 were used for final data analysis as two forms were excluded due to incomplete data. Among them 31.6% (n = 62) were males and 68.4% (n = 134) were females. The highest number of responses were received from the age group 20–29 (n = 112, 57.1%). The age of the participants who took part in this study ranged from 20 to 60 years (mean ± SD age of the participants was 31.16 ± 8.56). From urban areas, 94.9% (n = 186) participants took part in this study, and about 70.4% (n = 138) participants belonged to a public health facility (see Table 1). Table 2 describes the response to telemedicine services.
Demographic characteristics of the healthcare professionals.

Response to questionnaire by healthcare professionals.

Reliability of telemedicine
All participants (100%) are familiar with the term telemedicine. In addition, 91.8% of them possess a device capable of using telemedicine services. However, only 34.2% are aware of hospitals or organizations offering proper telemedicine services in Pakistan. Among the respondents, 77% consider telemedicine services to be reliable, and 71.9% believe it leads to a comparatively reduced financial burden on hospital administration. Opinions are divided evenly on whether HCPs rely on telemedicine applications, with 50% affirming and 50% negating this reliance.
Benefits of telemedicine
Regarding the benefits of telemedicine, 67.3% of participants believe it leads to an upgraded quality of healthcare. A majority (91.3%) acknowledge that telemedicine provides location-independent access to healthcare services. However, opinions are split on whether telemedicine is efficacious in avoiding multiple diagnoses, with 33.7% agreeing and 66.3% disagreeing. Participants are also divided on whether a more “hands-off” telemedicine-based approach might turn patients off, with 59.2% expressing concern. Moreover, 71.4% of respondents believe that telemedicine has more benefits than disadvantages.
Data storage and sharing
A significant majority (66.3%) support the idea that telemedicine services help collect data for the diagnosis of chronic illness or disability. Similarly, 79.6% favor the exchange of electronic information between HCPs and patients.
Perceived limitations of telemedicine
Concerns about increased workload on hospital administration are shared by 34.2% of participants. A notable 79.6% of respondents think that telemedicine can lead to increased misinterpretation during diagnosing. Privacy concerns associated with the use of telemedicine are acknowledged by 64.8% of participants. In addition, 91.8% believe that telemedicine has limited coverage in both urban and rural populations. A majority (71.4%) perceive technology savviness as a barrier to the acceptance of telemedicine among general patients.
Training needs of HCPs
Approximately 34.2% of participants feel sufficiently trained to use telehealth effectively, while 33.7% believe HCPs can use telemedicine services.
Willingness to use telemedicine in the future
About 73% of participants think that telemedicine should be integrated into the medical school curriculum. Similarly, 73.5% believe that telemedicine will become more acceptable for doctor–patient interaction in the future. Furthermore, 73.5% of participants think that telemedicine can contribute to developing better health electronic data for future health decision-making.
All participants were familiar with the term telemedicine and had a device that could provide them with telemedicine services. Although most participants (77%) believed that telemedicine services are reliable, many of them (65.8%) had yet to learn of any hospital that employs proper telemedicine services in Pakistan. A significant percentage (67.3%) of the studied population believed telemedicine upgrades healthcare quality and has more advantages than disadvantages. Another interesting finding was that 80% of the participants supported the idea that patients are likely to get turned off by telemedicine’s more “hands-off” approach. Almost a similar percentage (79.6%) believed telemedicine services are most likely to misinterpret the diagnosis.
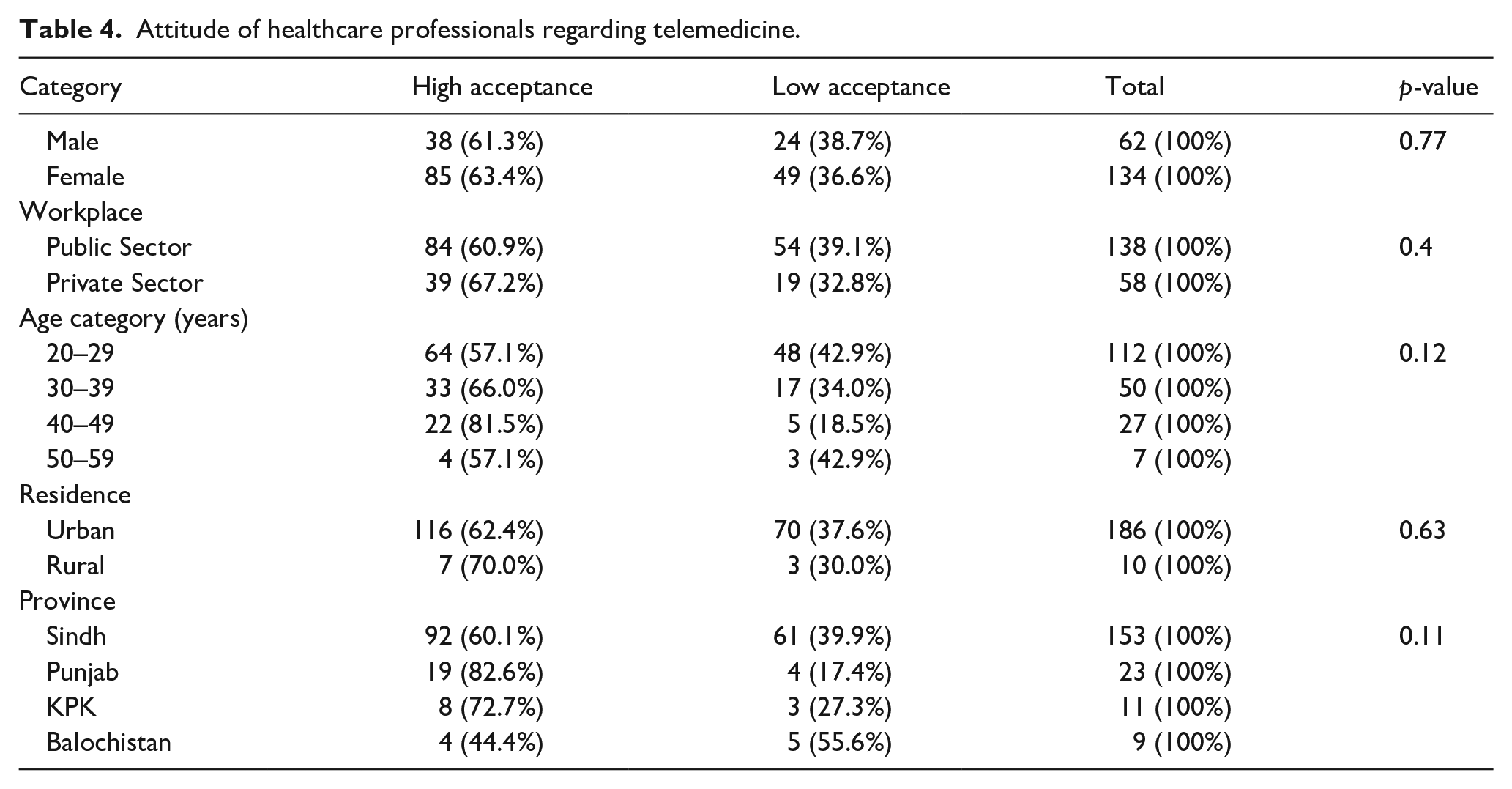
Despite the perceived limitations of telemedicine among the participants, most (79.6%) of them favored exchanging information between HCPs and patients via e-services like telemedicine. Most participants (71.4%) believed that a lack of technical knowledge is a barrier to the mass acceptance of telemedicine services. Hence, more HCPs (65%) rightfully accepted that they do not have confidence in their abilities to use telehealth facilities effectively. χ2 was performed to analyze any statistical differences in knowledge and attitude of HCPs toward telemedicine. Responses to the questions were structured in a manner to differentiate participants’ knowledge and attitude about telemedicine into high/low awareness or high/low acceptance. Independent p-values were determined for gender, workplace, age category, residence, and ethnicity. The results were found to be statistically significant for knowledge about telemedicine among HCPs in the workplace, that is, HCPs working in the private sector indicated a high level of awareness regarding telemedicine as compared to those in the public sector (p = 0.03; see Table 3). For all the categories in the attitude section, the results were not found to be statistically significant (p-value > 0.05; see Table 4).
Knowledge of healthcare professionals regarding telemedicine.

Attitude of healthcare professionals regarding telemedicine.
Logistic regression was also run to know how many participants think that telemedicine is reliable: so the model shows that 28.83% telemedicine reliability is explained by participants who think that telemedicine has more benefits than disadvantage, HCPs relying on telemedicine has found telemedicine to upgrade the quality of care, and those who are familiar with telemedicine after controlling for other variables (see Table 5).
Multivariable logistic regression model for telemedicine reliability.

Discussion
Telemedicine applications in underdeveloped nations could be a powerful tool for delivering basic health care to large populations and bridging the gap between rural areas and specialist institutions, which are located mainly in metropolitan areas. 8 Since the onset of COVID-19 in Pakistan, there has been an observable rush for telehealth services. This is Nurses’ knowledge and attitudes about using mobile health applications in Finland and Lithuania Nurses are familiar with mobile health technology and the regulatory agencies can monitor it. According to a qualitative finding participants shared that the most essential mHealth features were to automatically record data and send it to electronic health record. 6 Knowledge, attitudes, and behaviors related to the use of mobile health technology to treat tuberculosis in Indonesia revealed people’s willingness to learn about these technologies, their open and receptive attitude toward treatment, and their willingness to support a government-supported mobile Health programming. 9 In Iran, the level of willingness to use mobile health was considered as a score in percentage, with 0%–20% as being very weak, 21%–40% being weak, 41%–60% being average, 61%–80% being good, and above 80% being excellent. Approximately, 91.1% of participants were female and the majority (96.4%) of physicians owned a smartphone. The mean age and mean years of experience of the participating physicians were 45.05 ± 6.58 and 12.45 ± 5.77 years. There was a reverse relation between the physicians’ age and years of experience with their willingness to use mobile health technology.
In KSA, a cross-sectional study evaluated the Intensive Care Unit (ICU) staff members’ knowledge, attitudes, and perceptions of robotic remote presence technology in telemedicine during large-scale gatherings, which showed positive mindsets toward telemedicine but little expertise. Knowledge and attitude had mean values of 2.55 and 3.51 out of 5. Patient confidentiality and privacy were among the issues raised. 18 Moreover, in Malaysia, 288 healthcare workers (HCWs) participated in the study. Results showed that 66.3% of respondents thought new technologies may enhance existing procedures. Nonetheless, 29.1% were hesitant to employ telemedicine in the absence of previous in-person patient contact. Although cybersecurity and clinical competence deficiencies were issues for 56.6% of respondents, telemedicine as a clinical practice was accepted. Participants raised concerns about data security and expressed doubts about how telemedicine might affect doctor–patient interactions. Free-text comment analysis revealed recurring themes, including information trustworthiness, doctor–patient communication, responsibility, and data privacy and security. A total of 905 participants—48.4% staff and 51.6% students—participated in the survey to learn more about how HCPs at the Medical University of Vienna, Austria, felt about health technology.17,19
In 2021, study conducted in the United States identified various factors influencing the adoption and use of telehealth in critical access hospitals which included altering workflow and infrastructure, ensuring practitioner acceptance & availability, and providing technical assistance and support during deployment. 20 However, obstacles included concerns with equipment malfunction as well as a lack of experience with robotic systems and telemedicine. These results emphasize how critical it is to satisfy training demands and guarantee technology dependability in healthcare environments. 18 Similarly, a study conducted in 2021 looked at how doctors understood and felt about telemedicine and its applications, about 46.1% participants who understood telemedicine and 77% of professionals believe that the training is essential for efficient telemedicine usage (p = 0.01). 21 India unveiled the Telemedicine Practice Guidelines in 2020 which reported that the majority of the 602 HCPs polled showed strong awareness, understanding, and favorable opinions regarding telemedicine. Only 39.53%, though, had strong telemedicine-related skills. Furthermore, even while many were eager for training to advance telemedicine practice, many were unaware that the guidelines even existed. 22
Our research and another study by Kazmi et al. 23 , were aimed to evaluated HCPs’ knowledge and perceptions of telemedicine in Pakistan and found that most participants were familiar with telemedicine that could improve healthcare quality. Furthermore, Kazmi et al. 23 reported that telemedicine could be cost-effective and reduce the burden on tertiary care hospitals. In contrast, our study suggested it could increase the hospital administration’s financial burden. Our study found a significant association that private sector HCPs had a higher level of awareness regarding telemedicine, while the study by Kazmi et al. 23 found no significant associations with awareness. Similarly, our study and the study by Alghamdi et al. 24 that took place in Saudi Arab showed positive attitudes toward telemedicine but with concerns about privacy risks. Our study again contrasted with theirs as we found that private sector HCPs had higher awareness of telemedicine while no significant differences were found in attitudes based on demographics in their study. The study by Weisenfeld et al. in Germany also showed positive attitudes toward telemedicine but with concerns about patient acceptance and privacy. However, unlike our study, they also found no significant associations with awareness. 25 The healthcare sector of Pakistan has been in a state of dilapidation, with the country having spent only 1.2% of its GDP (Gross Domestic Product) on the healthcare field in 2021. 26 Although telemedicine has surpassed many of the barriers hindering healthcare delivery in developing countries, still Pakistan has not been able to accurately benefit from this progress. The exponential growth of the population, coupled with a disorganized healthcare system, has resulted in an unequal distribution of healthcare services. In 2019, there were 1.1 doctors per 1000 residents. 27 Telemedicine would help Pakistan’s healthcare system to utilize unorthodox and cost-effective techniques to revolutionize healthcare delivery across Pakistan. 14 In Pakistan and Afghanistan, using the mHealth app as Zaidi et al. 28 suggested had a positive impact on health education sessions, made it simpler to communicate with parents or clients, tracked routine immunization defaulters and followed up on them, improved data validity, made vaccination schedules easily accessible, and sped up registration. In another review, Jabeen et al. highlighted how mHealth might be utilized to enhance maternal health in low- and middle-income countries, particularly Pakistan. The author offers four major new techniques, including using mobile phones to improve communication, teleconsultation, and community HCP accessibility, offering free pharmaceutical supplies to mothers during health emergencies, and lobbying for safe abortion services. 29 Hoodbhoy et al. 30 suggested that mHealth has the potential to improve human resource management, training, and quality service delivery and absence of a specialized graduate-level program in low-resource areas suggests a scarcity of skilled personnel to create these insights. Thus, our study also identifies to enhance the importance of Telemedicine trainings at HCPs’ level to produce quality services delivery in health care organizations.
This study serves as a useful tool in spreading awareness at undergraduate, graduate, and post-graduate levels for medical professionals regarding telemedicine, and builds the evidence for the future rollout of any digital health intervention or program in public and private hospitals. This study had some limitations. The generalizability of the results was not possible due to the smaller sample size. The data were collected only from doctors, no paramedical staff was involved, and otherwise, we would have known how much uptake of telemedicine is there in the health system of Pakistan. Finally, there was no patient perspective related to telemedicine considered. While most HCPs exhibited satisfactory knowledge regarding telemedicine, it is still important to conduct regular training and education programs to keep them updated with the latest developments in this field. Such programs can help bridge the knowledge gap among doctors working in public sector setups.
1. Encourage the adoption of telemedicine:
The research revealed that doctors working in private practices were more accepting of telemedicine. As a result, efforts should be made to support and promote telemedicine usage in public sector settings as well. This can be accomplished through a variety of means, including providing incentives to doctors who use telemedicine, providing them with the required infrastructure and equipment, and boosting patient awareness about the benefits of telemedicine.
2. Address concerns regarding telemedicine:
HCPs may still have concerns regarding the use of telemedicine, such as issues related to data security, privacy, and quality of care. Hence, it is important to address these concerns and provide reassurance to HCPs about the safety and efficacy of telemedicine.
3. Foster collaboration between public and private HCPs:
Given the disparity in acceptance of telemedicine among doctors working in public and private setups, efforts should be made to foster collaboration between these two sectors. This can be achieved through partnerships and collaborations that promote knowledge sharing and exchange of best practices.
Conclusion
Many of the HCPs exhibited satisfactory knowledge regarding telemedicine and showed an accepting attitude toward it. A significant difference (p-value ⩽ 0.05) in knowledge was seen among doctors working in the public sector and those working in a private setup, with the latter showing higher acceptance (67.2%) when it comes to the use and application of telemedicine in the modern healthcare system.
