Abstract
The Emergency Medical Services (EMS) landscape is at a critical inflection point, requiring strategic transformation to address complex healthcare challenges. The evolution is imperative to enhance clinical service delivery, optimise patient outcomes and successfully integrate emerging technologies within the unique South African context. The paramedicine profession faces multifaceted challenges, including accelerated urbanisation patterns, increasing population density, and the distinctive quadruple burden of disease profile characteristics of South Africa. Through applying a future studies framework, this commentary explores key drivers influencing both probable and preferable future trajectories of EMS in South Africa. Implementation of clinically reflexive methodologies, specifically designed to understand and respond to patient-specific needs, represents a fundamental requirement for service enhancement. However, such approaches remain difficult to operationalise without structured mechanisms that effectively incorporate localised contextual insights and community-based intelligence. The paramedicine profession in South Africa continues to experience significant attrition of highly skilled and experienced personnel, exacerbating systemic challenges. Addressing these critical gaps requires multidimensional interventions – through strategic adaption to a living healthcare system, adaptive capacity development, and fostering a culture of inclusivity and methodologies to mitigate institutional knowledge erosion. These strategic interventions collectively contribute to a preferable trajectory of EMS in South Africa – one characterised by equitable and accessible healthcare to meet the unique needs of the population. Furthermore, contemporary analysis suggests a fundamental misalignment between the traditional EMS paradigm and actual population healthcare needs, with evidence suggesting many patients primarily require access to healthcare services rather than immediate emergency interventions. This distinction calls for a recalibration of EMS’ core functional parameters to achieve greater congruence with South Africa's broader healthcare priorities.
Introduction
Paramedicine as a discipline in South Africa (SA) has undergone significant evolution, transitioning from a physician-led first aid and rapid transportation model in the 1970s to a more complex system supported by prehospital providers with advanced tertiary qualifications. 1 This transformation has facilitated an expanding scope of practice and a diversification of professional roles for prehospital care providers. Concurrent with the ongoing evolution of the Emergency Medical Services (EMS) profession, there has been a notable increase in research outputs and academic capacity development within the discipline, supported by higher education institutions (HEIs).2,3 To effectively align the progressive advancements in paramedicine with the dynamic healthcare requirements of South African society, the establishment of an inclusive community of practice is essential for setting a forward-looking agenda.1,4
This commentary aims to provide a historical overview of paramedicine in SA while employing an argument for the future of the profession. To establish a future EMS model characterised by clinically reflexive and responsive adaption to patient needs, the systemic incorporation of patient perspectives into service design represents a critical imperative. 5 However, understanding and operationalising these needs presents significant challenges, particularly in the context of continuous attrition of experienced personnel who possess the institutional knowledge essential for implementing a patient-centred approach. 6 Through the application of an analytical future studies framework, we will explore both the probable (based on current trends) and preferred (aspirational outcomes) futures, facilitating an examination of the current trajectory and identifying necessary modifications to achieve an optimal future state for the paramedicine profession in SA. This approach enables the identification of key drivers influencing professional evolution while providing structured pathways for intervention and system optimisation.
Paramedicine as an evolving profession in SA
The South African prehospital milieu stands at a critical inflection point, reflecting three decades of transformative change. This profession has evolved from a physician-led model that emphasised first aid and rapid transportation to a sophisticated system characterised by a diverse array of undergraduate and postgraduate qualification holders. 1 A pivotal development in this evolution was the introduction of basic EMS training, which laid the groundwork for delivering prehospital EMS to vulnerable communities across SA. 1 The evolution of paramedicine education and training can be conceptualised as a context-specific response to SA's unique socio-political landscape, most notably the structural impact of the apartheid system that entrenched disparities in healthcare access and delivery, resulting in significant inequities between emergency services intended for white citizens, versus citizens of colour. 7 Following the country's transition to democracy, universal suffrage was granted in 1994, and with the end of apartheid, new challenges within the prehospital space required adaptive solutions.
During the 1980s, a vocational education model for EMS was initiated, supported by short courses for Basic Ambulance Assistance, Ambulance Emergency Assistants and Critical Care Assistance programmes. 1 These programs established the foundation for providing prehospital emergency medical care to previously disadvantaged communities as a consequence of the apartheid regime. 1 The establishment of a tiered EMS system gained momentum in 1999 with the introduction of standardised scopes of practice by the Professional Board for Emergency Care at the Health Professions Council of South Africa, enabling some paramedics to operate as independent practitioners. 1 This shift represented a crucial advancement in the professionalisation of prehospital care.
The governance of public EMS has also evolved, transitioning from local municipal oversight to a provincially governed model, while the National Department of Health sets EMS regulations and standards.8,9 Historically, under the apartheid regime, healthcare systems (including EMS) were deliberately segregated by racial classification, resulting in inequitable service distribution and systemic disparities in healthcare access. Post-apartheid reforms have sought to address these inequities by improving the accessibility of prehospital care, particularly in historically disadvantaged communities. 8 While these reforms have facilitated progress, particularly in the formalisation of the prehospital education framework, the profession continues to encounter substantial challenges. Notably, barriers to access persist, as the professionalised education framework remains largely inaccessible to individuals from disadvantaged communities and those already embedded within the prehospital workforce who hold vocational qualifications. 1 This limited accessibility risks marginalising individuals who have historically contributed to capacity-building efforts in the sector-efforts that have played a critical role in the profession's development and expansion. Furthermore, the gradual shift away from traditional volunteer-based models, which have been instrumental in shaping the EMS landscape, poses additional challenges in sustaining workforce development. 10 As a result, the EMS system remains fragmented, inequitable, and, for many communities, inaccessible, reinforcing disparities in prehospital emergency care and limiting the profession's ability to effectively serve the broader healthcare needs of the population. 11 Addressing these systemic challenges requires a holistic and inclusive approach that ensures the sustainability, accessibility and equity of EMS within SA's evolving healthcare frameworks.
The EMS system in SA currently labels itself as emergency-focused, although a substantial proportion of its work is dedicated to patients requiring access to primary healthcare rather than urgent, life-threatening interventions. 8 This discrepancy between service name and service need highlights a critical gap in system design and strategic orientation. Current EMS structures remain inadequately positioned to address broader healthcare demands, particularly in resource-limited settings where prehospital services provide a primary entry point into the healthcare system. While this is a global challenge, in SA, the failure to bridge this gap has led to workforce attrition, increasing service inefficiencies, and limited professional development opportunities.8,12 Without targeted reforms, EMS risks becoming unsustainable, losing its clinical credibility, and being sidelined in broader healthcare policy and funding decisions. If these systemic discrepancies remain unaddressed, they are likely to exacerbate existing inefficiencies and ultimately jeopardise the future of paramedicine in our country. 8
To navigate these challenges, the Future Studies framework, commonly referred to as foresight, provides a structured methodology for anticipating and preparing for potential future scenarios. 13 In the context of paramedicine, foresight offers a comprehensive analytical lens through which to assess emerging trends, technological advancements, service delivery models, and broader societal transformations that may influence healthcare provision in SA. 13
Foresight differentiates between two key perspectives: ‘probable future’ and ‘preferred future’. Probable futures refer to scenarios projected based on prevailing trends, empirical data and observable social dynamics. 14 Conversely, preferred futures represent aspirational outcomes aligned with professional and community values. Juxtaposing probable and preferred futures enables the South African paramedicine profession to identify strategic gaps, foster innovation and align policy and practice with the specific needs of its communities.13,14 This integrative and future-oriented approach not only addresses current systemic challenges but also ensures that the profession remains adaptive, community-centric and forward-looking. By integrating foresight methodologies, paramedicine in SA can transition from a reactive crisis-response model to a proactive, patient-centred and sustainable healthcare service that strengthens system resilience through inclusivity, enhancing patient outcomes and fostering the long-term development of an equitable and adaptive healthcare ecosystem.
Probable future of paramedicine in SA
If the current trajectory persists, the future of the EMS profession in SA is likely to perpetuate entrenched issues of exclusion and inequality, reflecting a society increasingly divided by socioeconomic disparities. The historical evolution of EMS has primarily been driven by academic frameworks that inadequately consider the lived experiences and needs of marginalised communities. 15 As a result, the prehospital education model remains largely disconnected from the realities of those it serves. This exclusion not only limits workforce diversity but also perpetuates inequities in access to EMS, particularly in underserved regions of SA.8,11
The ongoing push for professionalisation within EMS has at times deepened divisions among prehospital providers rather than fostering inclusivity. Expanding scopes of practice and diversifying roles have primarily benefited those with greater access to education and resources, limiting opportunities for professional advancement among disadvantaged individuals. The evolution of paramedicine—through specialised roles, expanded scopes of practice and increased research engagement—has largely been driven by practitioners based in urban centres, where access to education and resources is more readily available. 15 This trend has unintentionally reinforced existing inequities by limiting opportunities for professional advancement among providers from disadvantaged backgrounds. Consequently, the perspectives and needs of rural and low-income communities – often served by these underrepresented clinicians – remain marginalised in research, policy discourse and service design. As a result, service models and system developments frequently reflect the priorities of more resourced settings, rather than addressing the unique challenges faced by underserved populations. 16 Unintentionally, barriers to equitable access to prehospital services persist, and the system remains ill-equipped to respond effectively to the complex healthcare demands of vulnerable populations. 7 This ongoing lack of inclusivity in workforce representation and research initiatives will likely worsen disparities in the availability of high-quality prehospital care, entrenching social inequities in health outcomes.17,18 The ability to remain clinically responsive and reflexive allows for EMS system adaptability – while this remains under pressure from ongoing intellectual loss. 6 The departure of skilled providers not only compromises continuity in patient care strategies but also reduces opportunities for nuanced, patient-informed service delivery, which is essential for long-term service adaptability. 6
As depicted in Figure 1, the ‘brain drain’ – a phenomenon that has plagued SA for the better part of the last two decades – is characterised by the migration of healthcare professionals from the SA to international markets. This exodus presents significant challenges to service sustainability.19–23 The loss of knowledgeable and skilled prehospital providers has weakened leadership continuity, compromised the development of long-term patient care strategies and reduced opportunities for patient-centred, adaptive service delivery. Moreover, the South African EMS profession struggles to meet salary expectations and compete with international employment standards, further incentivising the migration of highly trained professionals. 19 Studies indicate that structural conditions within the South African EMS – working conditions, its worrisome leadership, safety at work and being undervalued – were among key factors suggested to contribute to the departure of advanced prehospital providers.20,24,25 These factors further curtail EMS development and erode institutional knowledge. The continued loss of skilled personnel disrupts strategic planning, impairs operational efficiency, hinders progress and ultimately jeopardises the long-term viability of the profession.
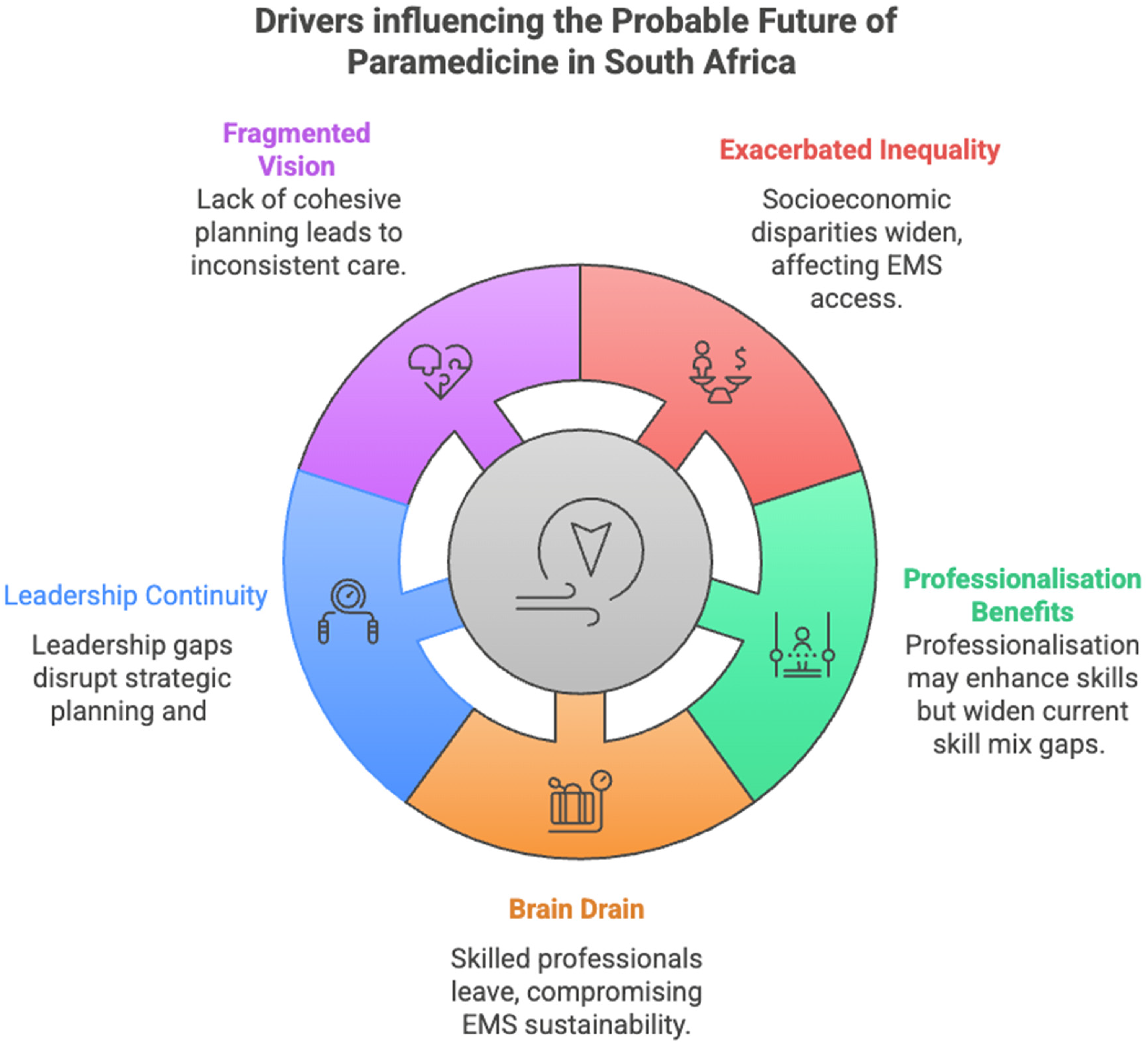
Mechanisms shaping the probable future of paramedicine.
The leadership of the South African EMS currently consists predominately of prehospital providers with varying levels of qualification, including those with postgraduate education. These professionals play a crucial role in shaping the future trajectory of EMS. The need and value of retaining and developing leaders in EMS are undisputable,10,26 and the continued loss threatens the future viability of EMS, placing critical knowledge and best practices at risk of being lost during personnel transitions or organisational changes. The departure of skilled prehospital providers reduces opportunities for shared learning, resulting in inconsistent care and diminished operational efficiency.19,22 Moreover, the EMS profession is marked by a pronounced absence of a cohesive vision for its future. 8 Advancements in EMS often stem from a narrow range of professional and system-level perspectives – primarily shaped by clinicians, policymakers or dominant stakeholders – resulting in a fragmented landscape that struggles to respond to the diverse needs of the broader population. The development of the unified vision for SA EMS should include consideration of established and well-defined healthcare frameworks. The adaption of these frameworks to the EMS setting should be done through collective sense-making with all actors within the system, specifically focussing on the end-user accessing healthcare through the prehospital service.27,28
Envisioning the preferred future of paramedicine in SA
To cultivate a brighter future for paramedicine in SA, it is crucial to focus on inclusivity.8,16,29,30 Actively engaging and incorporating the perspectives of marginalised communities could enrich the ongoing development of the profession; engaging these groups during EMS development fosters trust, enhances accessibility and informs inclusive policies. Ultimately, this leads to a more adaptable and equitable emergency care system.9,31–33 This engagement should extend beyond traditional stakeholders, such as regulatory authorities and HEIs, to include the diverse voices of those currently underrepresented. A key step towards a preferable future should enable marginalised community representation in the form of societies and/or unions.
As it stands, vocationally trained providers constitute the largest portion of the prehospital workforce in both the public and private sectors in SA.8,34 The preferred future of EMS must prioritise accessible education pathways and career progression opportunities within paramedicine that will empower a wider range of individuals, particularly those already in the profession and from historically disadvantaged backgrounds. 16 This proactive approach will ensure that the EMS profession is better equipped to meet the diverse needs of South Africans, ultimately benefiting all communities. To cultivate a fair, effective and adaptive EMS system, it is essential to integrate diverse viewpoints and ensure equitable distribution of improvements across all community segments. The establishment of communities of practice in which diverse stakeholders collaborate to shape EMS policy, practice and research will be instrumental in guiding the sustainable growth of EMS and ensuring that its evolution is responsive to healthcare and system needs. Without such inclusivity, paramedicine risks stagnation, potentially leaving a significant portion of the population without adequate emergency medical care.
As depicted in Figure 2, envisioning a preferred future that is clinically adaptive to the needs of all communities, EMS must engage in active dialogue with the public it serves. This collaboration is especially important given that the majority of patients require accessible healthcare rather than emergency intervention, yet EMS has traditionally structured its services around emergency care models.35–37 By evolving beyond an ‘emergency-only’ approach, EMS can better align its core function to address SA's broader healthcare needs. 10
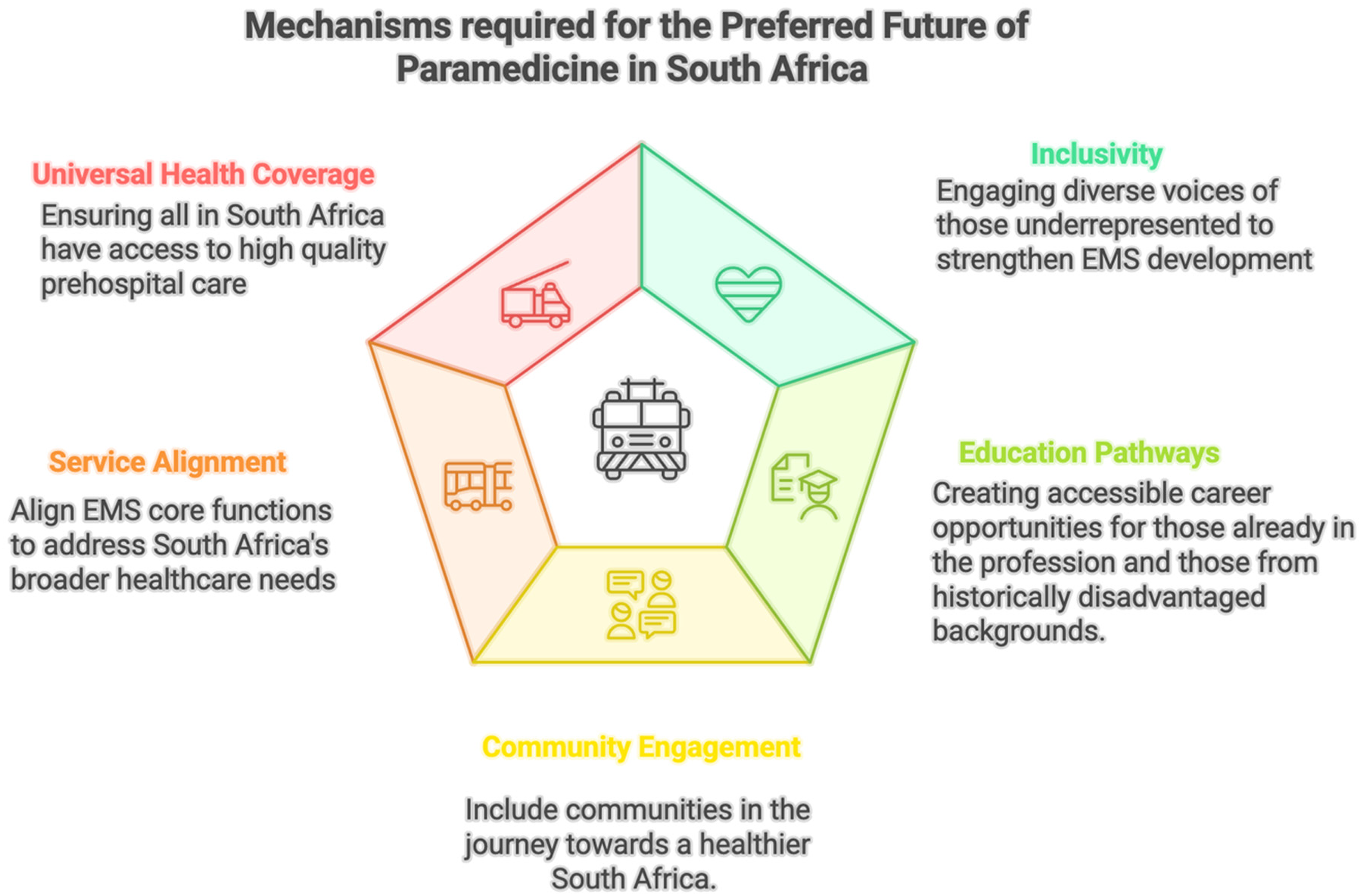
Elements required to shape the preferred future in South African paramedicine.
This shift is increasingly necessary as persistent challenges within the primary healthcare system – such as limited access to clinics, healthcare worker shortages and service delivery gaps in rural and underserved areas – drive community reliance on EMS for non-urgent and primary care needs. 38 Leveraging EMS in this way may be effective, as community-based healthcare models that extend services beyond traditional facilities have been shown to improve access, enhance health outcomes and reduce overall healthcare costs in resource-limited settings.5,39 Incorporating such an approach into the South African paramedicine landscape could offer a more contextually relevant solution to these persistent challenges.
Addressing barriers to inclusivity and career advancement within EMS will also help curb the ongoing migration of prehospital providers to international markets and mitigate brain drain in the healthcare sector. Brain drain is a recognised phenomenon impacting the broader workforce in SA and the sustainability of healthcare delivery. 23 Looking ahead, it is vital to adopt a more inclusive EMS framework – one that prioritises workforce retention, professional development and equitable service distribution – crucial for ensuring the long-term stability of EMS.
Long-term stability of EMS needs to address the system segregation legacies shaped by the apartheid system. 40 Some of its effects are still seen in SA's health system today, hereby further compounding existing disparities in EMS. Prehospital services remain starkly divided between public and private entities, and may continue on this trend. The public EMS system, which serves the majority of the population, is severely under-resourced, struggling with staff shortages, infrastructure limitations and operational deficiencies. 41 In contrast, the private sector features well-equipped systems capable of delivering high-quality care, yet remains accessible to less than 14% of the population.40,42–44
One of the strategies aimed at addressing this disparity comes from the World Health Organization's call for Universal Health Coverage and the South African National Department of Health's proposed implementation of National Health Insurance represent critical steps towards addressing the aforementioned systemic imbalances. However, ensuring that the paramedicine profession embodies all five dimensions of healthcare access – affordability, availability, acceptability, appropriateness and accommodation, remains essential and will be fundamental in achieving prehospital access across the country.45,46 This requires deliberate integration into EMS policy, workforce planning and service delivery to enhance equitable access and patient outcomes.
By embracing diverse perspectives and prioritising equity in healthcare resource distribution, we can guide the future growth of EMS to be more inclusive. This will enable the profession to better serve all communities, ensuring that both individuals and communities are included in the journey towards a healthier SA.
Conclusion
The contrast between the probable and preferable future of EMS argues for the need to readjust our current trajectory and underscores why inclusivity and collaboration are pivotal in this process. While the pursuit of professionalism is commendable, it has unintentionally resulted in certain vocational EMS providers becoming a marginalized community, potentially further fragmenting the field. Redressing the current trajectory of EMS demands a commitment to inclusivity and the preservation of collective memory within EMS, as it serves as a powerful catalyst for meaningful change.
To build an EMS system that is both inclusive and clinically reflexive, it is essential to engage actively with the communities served, aligning the system to address their actual healthcare needs – not just those classified as emergencies. The current framework prioritizes emergencies as its core function, even though a significant portion of EMS work involves patients who require general healthcare access rather than acute emergency interventions. Failing to address this fundamental misalignment may hinder EMS from evolving into a system that truly reflects and meets the diverse needs of South African society.
Furthermore, the ongoing loss of well-versed and experienced staff adds to the challenge of developing an EMS system that is adaptable to patient needs, as this expertise is invaluable in shaping services that are responsive and community centric. A future-ready EMS system must, therefore, not only foster inclusivity but also retain skilled professionals to ensure continuity in care quality, shared learning and the development of a responsive, adaptable and accessible emergency care system for all communities.
Footnotes
Author contribution(s)
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
