Abstract
Paramedic education programs play a critical role in preparing future paramedics to deliver high-quality care to diverse patient populations. However, the integration of social responsiveness, a key principle identified in the Paramedic Chiefs of Canada (PCC) report, Principles and Enabling Factors Guiding Paramedicine in Canada, remains inconsistent within paramedic academic programs. Social responsiveness emphasizes the profession's responsibility to address health disparities and promote social accountability, aligning with broader healthcare trends, including the CanMEDS 2025 framework and the World Health Organization's (WHO) global strategy for medical education. Despite its recognition in competency frameworks such as the Paramedic Association of Canada's (PAC) National Competency Framework for Paramedics (NCFP) and the Canadian Organization of Paramedic Regulators' (COPR) Canadian Paramedic Competency Framework (CPCF), a standardized approach to embedding social responsiveness in paramedic education has yet to be established. This manuscript proposes a conceptual framework for integrating social responsiveness into paramedic education, drawing on best practices from allied medical fields. Informed by a systemic literature review and analysis this framework identifies key structural reforms in recruitment, curriculum development, faculty training, continuous quality improvement, and institutional policies. A structural social responsiveness approach embeds equity and justice into the design, delivery, evaluation, and support systems of paramedic education, creating a learning environment that not only teaches social responsiveness but also embodies it in practice. By embedding social responsiveness into the foundational structures of paramedic education, this framework aims to institutionalize social accountability within academic programs, ensuring that paramedic graduates are not only clinically proficient but also equipped to champion health equity and social justice. This paper underscores the need for a transformative approach to paramedic education, positioning the profession alongside other healthcare disciplines in addressing systemic health disparities.
Keywords
Introduction
In 2023, the Paramedic Chiefs of Canada (PCC) released a report titled Principles and Enabling Factors Guiding Paramedicine in Canada, identifying Social Responsiveness as one of ten key principles critical to the growth of the paramedic profession. This principle emphasizes the responsibility of paramedics to address the root causes of health disparities and promote social accountability in both education and practice. 1 Initiatives such as the Paramedic Association of Canada's (PAC) National Competency Framework for Paramedics (NCFP), the Canadian Organization of Paramedic Regulators’ (COPR) Canadian Paramedic Competency Framework (CPCF), and The World Health Organization's (WHO) global strategy for medical education, acknowledge the importance of social responsiveness in healthcare.2–4 However, questions remain regarding how completely social responsiveness has been integrated into paramedic education and whether current efforts have gone far enough.5,6
Achieving true social responsiveness requires academic institutions delivering paramedic education to practice social accountability. This requires embedding social responsiveness within the foundational structures of their programs, such as recruitment strategies, quality improvement initiatives, faculty development, policies, support systems, and in curriculum. 7 This comprehensive approach of structural social responsiveness, embeds equity and justice into all aspects of paramedic education, shaping how learning is designed, delivered, evaluated, and supported. Such programs support the diversity of learners and prepare them to recognize and address health disparities that affect their future patients in real-world settings.8–10 This practice of social accountability and responsiveness aligns with broader healthcare trends seen in other medical professional frameworks and initiatives, such as the CanMEDS 2025 framework in medicine, which includes DEI and social justice elements, and nursing, which has taken strides in advancing social justice and equity, and within the WHO's global strategy for medical education.3,11–13 These examples highlight the importance of integrating social responsiveness in paramedic education, ultimately strengthening the profession's role and alignment with allied professions in addressing health disparities.
This document proposes a conceptual framework to improve social accountability within institutions that deliver paramedic academic education by enhancing social responsiveness within various aspects of the programs (Figure 1). Drawing on best practices from allied medical education, it emphasizes recruitment strategies, curriculum development, faculty training, continuous quality improvement initiative, and institutional policies. These best practices were identified through a systematic literature review and an analysis of frameworks such as CanMEDS in medicine and nursing curricula, which emphasize DEI and social justice elements. The selection process involved evaluating peer-reviewed studies, accreditation standards, and recommendations from professional regulatory bodies to ensure relevance and applicability.14–16
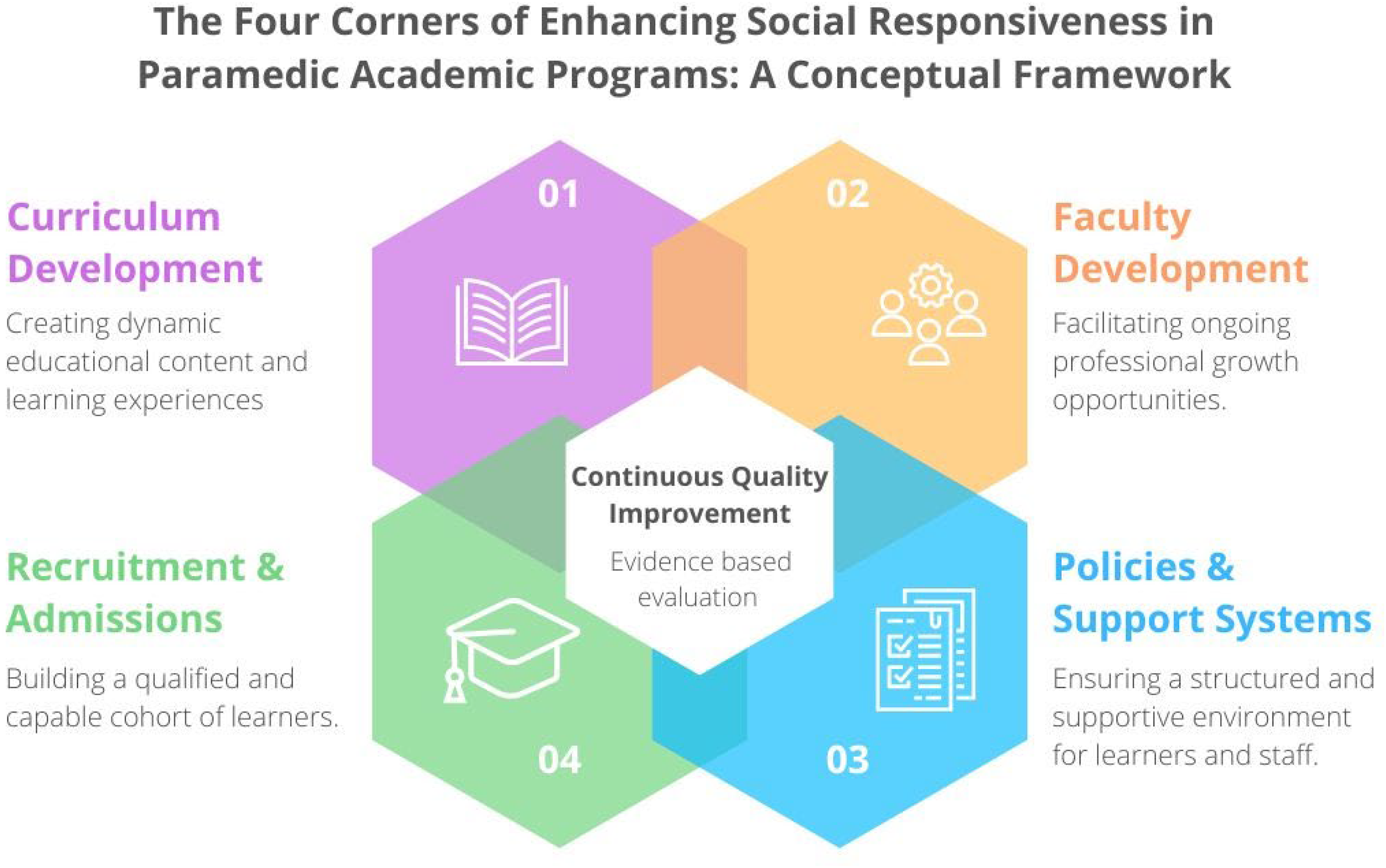
Visual representation of the conceptual framework for enhancing social responsiveness in Paramedic academic programs, illustrating its key components.
This framework aims to create a comprehensive learning environment that supports learners, actively addresses health disparities, and prepares future paramedics to champion social justice in their communities. Embedding social responsiveness into the structure of paramedic education ensures that social accountability is woven into the fabric of professional identity, transforming it from a supplementary goal to a foundational component of paramedic practice.
Methods
This is a conceptual framework developed through a systemic and iterative process grounded in a comprehensive literature review and a review of current efforts in the field. This approach was taken to ensure that the framework is both evidence-based and pragmatically relevant.
The literature review involved searches in Novanet and academic databases such as PubMed, CINAHL, and Google Scholar, selected for their extensive coverage of healthcare, healthcare education, and paramedicine-related research. Search terms included “Social Responsiveness,” “Best Practices,” “Framework,” “Diversity, Equity, Inclusion” (DEI/EDI), “Cultural Humility,” “Structural Social Responsiveness,” “Health, Equity, and Justice,” “Justice in Healthcare,” “Healthcare Training,” and “Social Accountability.” Boolean operators (AND, OR) were applied to refine search results and ensure comprehensiveness. Initially, 9135 articles and reports were identified. Further refinement using filters for title/abstract relevance, peer-reviewed status, language (English), and publication date (2000–2024) reduced the results to 360. After a thorough screening for relevance, methodological rigor, and applicability, the final selection was narrowed down to 41 sources that provided the most relevant insights into social accountability and responsiveness in healthcare education.
A Framework Analysis approach was used to systematically review and categorize best practices from paramedicine and allied professions, including nursing and medicine. Best practices were identified through a systematic literature review and an analysis of frameworks such as CanMEDS in medicine and nursing curricula, which emphasize DEI and social justice elements.3,13 The selection process included evaluating peer-reviewed articles, accreditation standards, and recommendations from professional regulatory bodies to ensure relevance and applicability. This involved identifying existing models of social responsiveness in education and practice, extracting key principles, and structuring them into a framework tailored to paramedicine education. This approach ensured that the conceptual framework was evidence-based while allowing flexibility for adaptation and future refinement.
Recruitment and admissions
The healthcare system increasingly serves vulnerable populations, including the unhoused, individuals with mental illness, people with disabilities, and those in rural communities. To meet the complex needs of these diverse groups, paramedic graduates must be equipped to work effectively across a wide range of communities. 17 Achieving this requires actively recruiting learners from underrepresented backgrounds. Diversity within the paramedic profession is essential for improving health outcomes. 18 Clinicians from varied backgrounds bring perspectives that help dismantle barriers, foster culturally relevant care, and build trust with patients. Adopting an intersectional approach, acknowledging how overlapping social identities like race, gender, socioeconomic status, and culture shape experiences, further enhances the ability of providers to deliver equitable, informed care. 19 A paramedic workforce that mirrors the diversity of its communities is better positioned to address health disparities, strengthen patient relationships, and deliver meaningful, inclusive care.20,21 This transformation begins with educational institutions dismantling barriers to equitable access. Equity in paramedic education is not just an aspiration; it is the foundation of a profession committed to health justice and social accountability. 22
Effective recruitment and admissions strategies are essential for attracting a diverse pool of learner applicants and addressing barriers to paramedic academic programs. 23 This includes comprehensive admissions processes, financial assistance programs, and pipeline programs.24,25
Comprehensive admissions processes
Implementing comprehensive admissions processes allow paramedic programs to value a range of applicant qualities beyond academic metrics. In addition to academic achievements, admissions committees should consider applicants’ socioeconomic backgrounds, cultural experiences, language proficiencies, and personal qualities that align with the values of patient-centered care. Including experiences such as community involvement, resilience, and overcoming adversity allows programs to recognize candidates with the potential to connect meaningfully with diverse populations and contribute to innovative approaches to care. 24
Financial assistance programs
Socioeconomic barriers often prevent qualified applicants from accessing education. To address this, paramedic programs should develop financial assistance programs that alleviate expenses such as tuition, textbooks, certification fees, and equipment. Scholarships, grants, loan forgiveness programs, and work-study opportunities can reduce financial barriers, ensuring that qualified learners from lower-income backgrounds can pursue paramedicine. Supporting underrepresented learners in this way aligns with the commitment to health equity, making careers in paramedicine accessible to a broader demographic. Funding for these initiatives could be derived from institutional budgets, government subsidies, external grants, or philanthropic contributions. Collaboration with healthcare organizations and community partners may also provide sponsorships or tuition reimbursement programs.23,26,27
Pipeline programs
Effective pipeline programs are integral to promoting paramedicine among underrepresented communities. Partnerships with community leaders, knowledge keepers, local organizations, healthcare institutions, and high schools can establish pathways that introduce people to paramedicine, through mentorship initiatives, hands-on training, and career exploration workshops tailored to underrepresented learners. These programs not only help identify potential candidates but also foster early mentorship and exposure to the profession, making it a viable career option for anyone looking to pursue paramedicine.23,25
Curriculum development
Integrating social responsiveness into paramedic education requires moving beyond isolated discussions or modules; it calls for embedding these principles throughout the curriculum in a way that prepares learners to recognize and address the diverse and complex needs of the populations they will serve.28,29 A socially responsive curriculum encompasses an understanding of healthcare's historical inequities, systemically driven disparities, understanding of inclusive representation, trauma-informed care, the dangers of race-based medicine, and the integration of experiential learning within community-led initiatives.30–32
Historical context of healthcare
Paramedic learners must examine the historical injustices that have shaped healthcare access and outcomes for equity-deserving communities. For instance, in the United States, systemic discrimination against Black communities includes egregious events like the Tuskegee Syphilis Study. 33 In Australia and Canada, Indigenous peoples have endured profound health inequities rooted in colonization, including the forced removal of children, medical experimentation, and neglect.34,35 Similarly, in the United Kingdom, aversion therapy was inflicted on LGBTQ+ individuals as a result of pathologizing identities.36,37 These historical injustices have eroded trust in healthcare systems among marginalized communities worldwide. Understanding these histories is crucial for paramedic learners to grasp the barriers many communities face today. By appreciating the broader context in which they practice, learners can develop the cultural awareness and empathy needed to rebuild trust, address inequities, and become effective advocates for their patients.38–40
Systemic inequities in healthcare
Systemic inequities within healthcare often stem from biases in research, exclusionary policies, and legacy protocols that still impact patients today.41,42 Integrating critical thinking and problem-solving discussions about healthcare inequities can help future providers better understand the context in which they will work, the systems they will represent, and their responsibility as patient advocates. This approach fosters a deeper awareness of how to navigate and address inequities within the healthcare system. 43 Providers will be better equipped to identify and address systemic barriers, positioning them as agents of change and advocates for more equitable care.
For example:
Gender Disparities: Due to underrepresentation of women in medical research, cardiovascular symptoms women experience during a myocardial infarction (MI), are poorly understood. This has led to frequent misdiagnosis or delayed treatment, resulting in higher mortality rates compared to men. By discussing these disparities, learners can better recognize the limitations of existing medical knowledge and seek more inclusive, evidence-based practices.44,45 Medical Technology: Oxygen saturation probes, which were designed without adequate testing on different skin tones, inaccurately read oxygen levels in patients with higher melanin, resulting in potentially dangerous undertreatment.
46
Developing an awareness and engaging in critical discussions on how to navigate these limitations enables future providers to better advocate for patients and work within these constraints to improve quality of care and patient outcomes.
Representation
True representation in paramedic education extends beyond diverse imagery in slides or mannequins. 47 It involves equipping learners with the skills to effectively treat a range of bodies and understand diverse perspectives and intersectionality of identities.
For example:
Assessment on Different Skin Tones: Skin conditions like cyanosis or jaundice may appear differently on darker skin tones, so paramedic learners must learn to assess symptoms accurately across a spectrum of skin tones.48,49 Cultural Humility: Beyond cultural competence, which can imply a fixed knowledge, cultural humility encourages lifelong learning and self-reflection about one's biases and assumptions. Paramedic learners should be taught to recognize their own positionality and how it might affect patient interactions.
50
Social determinants of health
Clinical and technical skills are essential components of paramedic education. However, without also learning about the impact of social determinants of health, learners learn to treat medical conditions without fully understanding the implications of the broader context of a patient's life. This includes factors such as housing instability, food insecurity, and systemic discrimination. 51 Including social determinants of health into case studies, and simulations, paramedic programs enable learners to recognize and connect presenting illnesses to broader health indicators, creating more comprehensive and sustainable care plans. 5
Example:
A call comes in for a patient who frequently calls 911 for hyperglycemia. But this time the paramedic responding to the call recognizes that the patient being unhoused may be a factor in their medication compliance. With this knowledge the paramedic engages in a thoughtful conversation with the patient about factors impacting their compliance with medication and find out the patient can not always afford their medication leading to inconsistent compliance with their medication. With this insight, the paramedic treats the immediate health concern and connects the patient with resources to help cover medication costs. This approach addresses both the immediate health concern and the broader factors affecting the patient's health and well-being.
The myths and dangers of race-based medicine
Race-based medicine reinforces harmful stereotypes by misattributing biological differences to race, which is a social construct, and using this flawed assumption to guide treatment decisions. This approach risks reproducing inequalities and fails to acknowledge the social determinants that significantly influence health outcomes. For instance, the misconception that Black individuals have higher pain tolerance has historically led to the undertreatment of pain in Black patients. Teaching paramedic learners to recognize and reject these myths is crucial. This can involve discussions on how socio-economic factors, access to care, and lived experiences, rather than race, better explain health disparities.52,53
Experiential learning
Experiential learning, such as community placements and high-fidelity simulations fosters deep understanding and growth but is often postponed until the final stages of paramedic programs. Introducing these experiences earlier allow learners to integrate theoretical knowledge with practical insights throughout their training. This approach enhances critical thinking, problem-solving, and confidence, leading to greater engagement and readiness for preceptorship and ultimately resulting in better patient care outcomes.
Community placements with organizations that are led by and serve equity deserving groups, allow learners to learn firsthand about the challenges communities face. By working in equity-deserving community settings, whether a clinic in an underserved neighborhood or a harm reduction center, learners gain valuable exposure to the social determinants of health in real-world contexts. 54 These placements encourage learners to engage with community leaders and patients, promoting understanding empathy and cultural humility, while developing technical skills. Through reflection exercises following these experiences, learners can critically examine biases and learn adaptive strategies for patient-centered care.40,55
Moving toward a socially responsive paramedic curriculum
A socially responsive paramedic curriculum requires programs to adopt a comprehensive approach that intertwines technical training with cultural, social, and historical awareness and strategies to improve health equity and patient outcomes. By systematically embedding social responsiveness into curriculum, paramedic learners will not only be skilled clinicians, but also compassionate, equity-oriented practitioners equipped to advocate in partnership with their patients.3,56,57
Third-party accreditation often emphasizes meeting minimum standards, which can inadvertently discourage paramedic programs from adopting innovative approaches to social responsiveness. To achieve meaningful integration of social responsiveness, paramedic education should establish robust learning objectives, evaluation methods, and teaching activities that prioritize cultural humility, understanding social determinants of health, and recognizing biases. This approach ensures a curriculum that cultivates learners’ growth as socially aware practitioners. By transitioning from a competency-based approach to one that is integrated, reflective, and community-centered, paramedic education programs can better prepare learners to provide socially responsive care for diverse populations.30,31
True social responsiveness requires active partnership with individuals who have lived experience from equity deserving communities. Establishing advisory committees that reflect these perspectives ensures the curriculum addresses the real needs and challenges of the population's paramedics serve. Meaningful collaboration requires transparency, respect, and a commitment to honoring community insights, which must be approached thoughtfully to avoid tokenism. By building trust and fostering long-term partnerships, paramedic programs can ensure that social responsiveness principles are authentically embedded in the curriculum, creating a socially responsive foundation that resonates with both learners and the communities they will serve. 58
Faculty development
Effective faculty development is essential to prepare paramedic educators to integrate and model social responsiveness in their teaching practices. This includes addressing both the formal curriculum and the “hidden curriculum"- the implicit values, attitudes, and behaviors conveyed through institutional culture and educator actions. The hidden curriculum significantly shapes learners’ understanding of social responsiveness, often influencing perceptions of equity and care more than the explicit curriculum. Faculty must be intentional not only about what they teach but also how they teach, as unspoken behaviors, subtle biases, or institutional norms can inadvertently reinforce inequities, even in programs emphasizing social justice, equity, diversity, and inclusion. Faculty development initiatives should empower educators to recognize and challenge these implicit messages, ensuring consistent reinforcement of social responsiveness across all aspects of the educational experience. By addressing the hidden curriculum, educators can align implicit and explicit teaching to provide cohesive messaging about equity and inclusivity. Faculty should exemplify socially responsive teaching practices, such as: Creating inclusive learning environments, foster spaces where all learners feel valued, enabling open dialogue, and embracing diverse perspectives. This may include adapting teaching strategies to accommodate varied learning styles and cultural contexts. 59
Aligning the explicit and hidden curricula ensures a unified and impactful learning experience, equipping graduates with the knowledge and skills to deliver equitable, patient-centered care and advocate for systemic change. By doing so, faculty development not only enhances the quality of education but also strengthens paramedicine's broader mission to address health inequities and promote health justice. This approach reinforces paramedicine's commitment to advancing systemic change, advocating for underserved populations, and delivering care that acknowledges and addresses the social determinants of health.
Institutional policies and support systems
Social responsiveness initiatives must be supported by robust institutional policies and systems. 31 This includes implementing anti-discrimination policies, establishing an equity steering committee, and dedicating resources to Social Justice, Diversity, Equity, and Inclusion (JDEI) efforts. 60 In addition, providing support services such as mentorship programs and mental health resources is essential to ensuring the well-being and success of learners.61,62
Continuous quality improvement
Ongoing assessment and evaluation of recruitment, faculty development, support systems and policies, and curriculum are essential to ensuring that paramedic academic institutions remain socially accountable. Continuous Quality Improvement (CQI) efforts should focus on two key areas: fostering the success of all learners and ensuring that the curriculum reflects principles of social responsiveness.
CQI processes must create an inclusive and equitable environment for all learners. This includes developing assessment tools to monitor how well the institution supports Diversity, Equity, and Inclusion (DEI) in learner experiences and outcomes, such as retention, graduation rates, and access to support services. Regular feedback from learners, faculty, and staff should be used to identify gaps in support for equity deserving learners. Based on this feedback, adjustments to admissions policies and procedures, learner support systems, and inclusive teaching practices should be made to ensure that all learners have the resources and mentorship they need to succeed. 63
CQI efforts must also continuously assess the curriculum to ensure that it remains relevant and socially responsive. This includes regularly updating course materials to reflect best practices and current terminology. Assessment tools such as written exams, practical skills evaluations, and reflective portfolios should be designed to measure learners’ understanding of key concepts and their ability to apply them in real-world scenarios.
This commitment to continuous improvement ensures that paramedic programs not only foster an inclusive learning environment but also produce clinicians who are well-prepared to deliver socially responsive care. Ultimately, this fosters structural social accountability in paramedic education and contributes to more equitable health outcomes. 64
Literature review
A thorough literature review was conducted to gather existing knowledge, theories, and models relevant to social accountability in healthcare academic education through social responsiveness. The review included peer-reviewed journal articles and authoritative reports. The search strategy involved the use of multiple academic databases, with search terms such as “Social Responsiveness”, “Diversity, Equity, Inclusion”, “cultural humility”, “structural social responsiveness”, “health, equity, and justice”, and “social accountability.” Studies were selected based on their relevance, methodological rigor, and contribution to the understanding of social accountability and responsiveness. The literature review was structured to address key themes and concepts that emerged from the data. This allowed for the identification of gaps in the current knowledge and the synthesis of diverse perspectives, which informed the development of the framework. Importantly, the review also incorporated key findings from neighboring fields like medical education, where frameworks such as CanMEDS have integrated Equity, Diversity, Inclusion, and Social Justice into clinical practice.13,65 Nursing literature informed the focus on social justice in healthcare education. 66 These insights provided a foundation for adapting similar strategies within paramedic education, ensuring that best practices from other healthcare fields inform this framework.
Review of current efforts
In addition to the literature review, a review of current efforts in social responsiveness was undertaken. This review involved analyzing existing programs, policies, and initiatives related to social responsiveness in academic healthcare programs. Sources included grey literature, reports from relevant organizations, and case studies of best practices. The review aimed to identify practical approaches and strategies currently in use, as well as to assess their effectiveness and alignment with the goals of the framework.
The genesis of this topic sparked a critical review of current efforts of social responsiveness within paramedicine. This review included an analysis of initiatives such as the Paramedic Association of Canada's (PAC) National Competency Profile (NCFP) and the Canadian Organization of Paramedic Regulators’ (COPR) Canadian Paramedic Competency Framework (CPCF).2,4 Both initiatives emphasize the role of social accountability in paramedic practice. The review also examined ongoing faculty development programs, curriculum reforms, and quality improvement initiatives currently in use in healthcare education. These programs provide tangible examples of how embedding equity and social justice into the education of healthcare professionals improves not only learner outcomes but also community health outcomes.
Synthesis and framework development
The insights from the literature review and the review of current efforts were synthesized to develop the conceptual framework. This process involved identifying recurring themes such as the importance of socially responsive teaching, diverse learner support, and structural social responsiveness in the development of healthcare professionals. The synthesis also considered barriers identified in the literature, such as resistance to change and the need for ongoing faculty training, as well as enabling factors like institutional commitment and external partnerships with communities served by paramedics.58,67 The resulting framework is structured to be grounded in the best available evidence while remaining flexible enough to accommodate future developments. It draws upon strategies from nursing and medical education to ensure that the proposed initiatives are not only theoretically sound but also have practical applicability in paramedic education.
Barriers and enabling factors
While the framework presents a structured approach to social accountability of paramedic programs and the educational institutions that provide them by integrating social responsiveness, we acknowledge certain barriers, such as potential resource constraints and institutional resistance. However, enabling factors such as support from leadership, ongoing faculty development, and community engagement can drive success. Continuous improvement cycles, informed by feedback from partners, will ensure the framework's ongoing relevance and effectiveness.
Limitations
While this framework provides a structured approach, it has limitations. Firstly, although it incorporates best practices from various healthcare disciplines, its direct application to paramedicine education may require further adaptation and evaluation. Secondly, since the framework relies on existing literature and case studies, it may not fully capture emerging or innovative strategies. Lastly, differences in institutional resources and policies could affect the feasibility of implementing certain recommendations. Future research should focus on piloting the framework in diverse paramedic programs to evaluate its practical effectiveness and adaptability.
Conclusion
The Paramedic Chiefs of Canada (PCC) emphasize Social Responsiveness as a cornerstone of paramedicine's accountability, leadership, and clinical frameworks. 1 This framework aligns with the profession's commitment to addressing structural inequities, social challenges, and gaps in services for at-risk and underserved populations. By promoting socially accountable learning environments, it integrates key principles into curricula and foundational structures to support its mission. This framework emphasizes identifying, designing, implementing, and evaluating initiatives that address both social injustice and health inequities. It advocates for patients, communities, paramedicine professionals, and the broader profession, with particular attention to traditionally underserved groups. Integrating ongoing faculty development, quality improvement systems, and supportive policies ensures the framework not only enhances individual learning but also contributes to more equitable and responsive patient care. Drawing on lessons from medical and nursing education, this interdisciplinary approach leverages best practices to enhance paramedic education's capacity to address health disparities and foster meaningful improvements in outcomes for underserved communities. 1
Next steps
This document serves as a conceptual framework for enhancing social responsiveness in paramedic academic programs. External and ongoing evaluation of the framework and additional research and collaboration will further strengthen the framework, ensuring it remains responsive to the needs of both learners and the communities they serve.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
