Abstract
Introduction
Background
Pain is a multidimensional experience that is highly subjective and is dependent on the individual's lived experience and tolerance of pain.1–3 The pain experience encapsulates physiological, emotional, and cognitive components, and can be classified as acute, a transient dynamic pain associated with intense emotions, or chronic, persistent pain that lasts longer than 3 months.1,2,4,5 Nociception refers to the process that leads to an individual perceiving pain. Nociceptors are sensory receptors present in human tissue, that recognise and alert the brain to pain.4–6 When noxious stimuli cause direct tissue damage, nociceptors are activated and the pain pathway, or nociception, takes place.4,5
Paramedicine refers to the provision of medical care in the out-of-hospital setting, in both an emergency and non-emergency capacity.7,8 The paramedics who operate in this space are exposed to a dynamic, uncontrollable environment, in which they need to be capable of managing and treating a vast range of presentations; from life-threatening to acute conditions; to mental health and socially challenging situations.7–10
Paramedicine is a steadily evolving field with many variations across different services around the world.9,11,12 Where traditionally, ambulance services accepted vocationally trained paramedics, there has been a gradual shift in paramedics requiring tertiary qualifications to enter the workforce.8,9,13 Many services allow paramedics to complete further training or study to become specialist clinicians, in which their scope of practice increases to encompass more specialised skills. 10 Some services allow paramedics to engage in independent decision making without contemporaneous medical oversight, whilst others require consultation with medical professionals to direct treatment decisions. 11 This variation in education and scope means that the care provided from paramedic to paramedic may vary.
Paramedics are frequently contacted to alleviate pain for those afflicted in the community.14–16 In both paramedicine and healthcare as a whole, a range of pain assessment and measurement approaches are utilised including the visual analogue scale, verbal rating scale, Wong Baker FACES pain rating scale, and pain drawing.17–21 The most used tool for quantifying pain severity in paramedicine is the verbal numeric rating scale (vNRS) which takes less than a minute to conduct and allows for pain to be expressed as a number.17,18,20 Patients are instructed ‘on a scale of zero to ten, with zero being no pain at all and ten being the worst pain you could imagine, where would you rate the pain you are experiencing right now?’ (p. 67) 22 These pain measurement tools are seemingly sex-neutral, and do not consider the subjective nature of the pain experience, nor the biological, psychological or sociocultural influence that sex has on pain expression.23,24 Whilst, paramedics rely on a patients symptoms and reporting of pain to inform analgesic decisions, a clinicians’ subjective clinical judgment that is influenced by their experiences and scope of practice may at times override the severity of a patients reported pain score. 25 For clinicians, being aware of subconscious biases that may impact the quality of care they provide is imperative, whilst patients who receive unbiased pain management have increased trust and confidence in ambulance services and the paramedics who care for them. 26
It is therefore evident that pain is a complex phenomenon that is not only dictated by the innate biological process of nociception, but by an individual's lived experiences and understanding of pain. In turn, analgesic decisions are informed off both a patient's response to objective clinical measures and the paramedic's subjective clinical judgement. A patient's sex is therefore imperative to investigate in the context of pain and it's management, as males and females inherently perceive, tolerate and express pain differently.1–5,24 Sex therefore challenges equitable pain management practices as a whole. It is of note, that the terms sex and gender are used interchangeably throughout this article however both are used to describe a person's biological sex at birth.
The current research conducted into the effect of sex on paramedic management of pain has not been well summarised. This review was intended to inform understanding of a subsequent observational study into actual pain management practice by paramedics. As such, this rapid review aimed to evaluate current literature on gender biases in paramedicine, to identify the influence of sex on analgesic pain management practices.
Methodology
Design
A rapid review methodology was adopted due to time constraints arising from the study being a precursor to a broader epidemiological research project. Rapid reviews are a recognised, robust review typology particularly suited to contexts in which results are required in a more timely fashion than those arising from a systematic review, to identify and critically appraise current studies in paramedicine. 27 This review was conducted in accordance with the Cochrane Guidance on Rapid Reviews. 28 Prior to conducting the research, a protocol outlining the aims, objectives, methodology, and timeline of this review was uploaded to Open Science Framework. 29 The protocol is located at https://osf.io/nkfxc. Changes have since been made to the a priori document in relation to methodology and outcomes. This rapid review is reported in adherence with that PRISMA 2020 statement. 30
Eligibility criteria
Articles were eligible for inclusion in the rapid review if they: (i) investigated patients who presented with pain to an ambulance service; (ii) analysed pharmacological analgesic management; (iii) provided comparative analyses based on sex; and (iv) reported on at least one of the following outcomes: medication type, medication dosage, time to administration, or pain score.
Articles were excluded from analysis if they: (i) specifically investigated pregnant populations, older people (>65) or younger people (<16); (ii) provided no analysis of pharmacological interventions; (iii) had no comparisons based on sex; (iv) did not report on any of the primary outcomes; (v) were either conference abstracts, commentaries, clinical trial registrations, and editorials; and (vi) were not published in English.
Search strategy
Five electronic databases were searched on 8 November 2023. These were MEDLINE (Ovid), CINAHL (EBSCOhost), Cochrane, Embase (Ovid) and Scopus (Elsevier). Search results were restricted to full text and English language with no date restrictions applied. A further nine paramedic specific journals were hand searched for relevant articles due to these journals not being indexed in the listed databases. Grey literature was not searched for this review due to time constraints. The paramedic search filter optimised for sensitivity created by Olaussen et al. 31 was used to inform the search strategy. A preliminary search on MEDLINE was also conducted to identify further relevant terms. A full search strategy for each database and the list of paramedic specific journals can be found in Supplemental Appendix 1. In adherence with rapid review methodology, the literature search was conducted by one researcher (SD).
Study selection
Identified articles were uploaded into the systematic review software Covidence 32 via the reference manager software EndNote. 33 Screening of the selected studies was undertaken via a two-step process. Step one had two of the researchers (SD and NN) individually screen the titles and abstracts of all articles. Step two comprised of SD screening the full text of all shortlisted articles, whilst NN screened all excluded full texts. Reasons behind exclusion of full texts are documented in Figure 1. Any discrepancies were settled by a third researcher (PS).
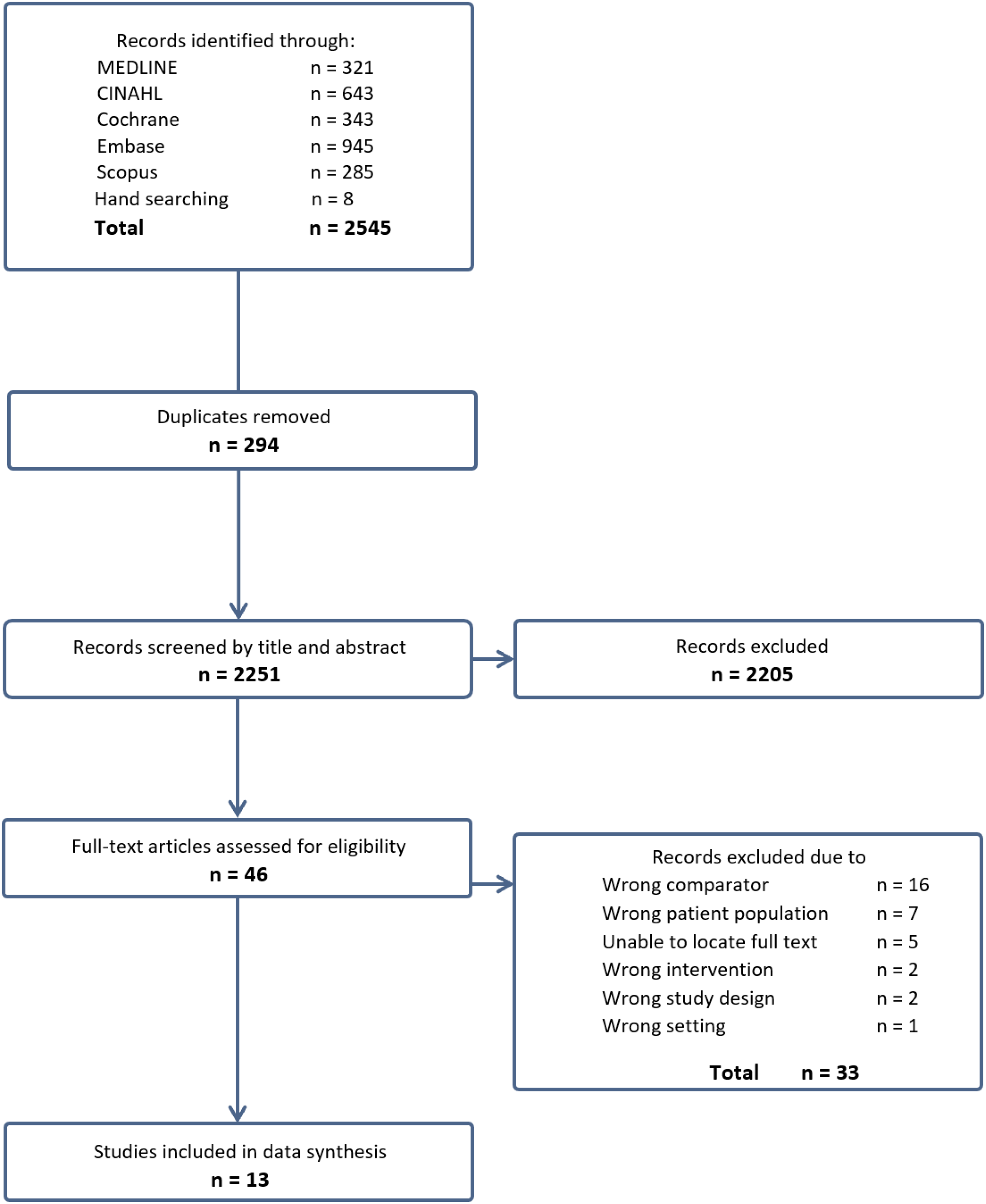
PRISMA flowchart of included and excluded studies.
Data extraction
Data were extracted by SD with NN and PS checking for accuracy. The following data were extracted from each article: title, author, publication date, country, study design, sample size (sex %) and study results. Data were in turn subject to narrative synthesis. Tables and figure were created using Microsoft Word. 34
Assessment of risk of bias
Selected articles were in turn assessed for risk of bias (ROB) using the JBI Critical Appraisal Tool for Analytical Cross-Sectional Studies. 35 This tool consists of eight criteria that can be answered as yes, no, unclear, or not applicable. Studies were included as part of this rapid review if they received a “yes” response to five or more out of the eight domains. This would indicate that included studies have a greater than 60% methodological quality rating, which was deemed sufficient for this review. There was a lack of consensus in the existing literature on quality rating thresholds and thus 60% was selected based on consensus from the research team and a rapid review conducted by Pap et al. 36 that had similar setting and structure as this present research. SD and NN individually assessed the ROB for each study, with disputes settled by PS. Certainty of evidence was not assessed in adherence with accepted methodological guidance for rapid reviews.
Results
Study selection
A yield of 2537 studies were identified through the database searching with an additional 8 studies located with the searching of non-indexed journals, resulting in a total of 2545 articles. From these, 294 duplicates were removed with 2205 articles excluded for not meeting the inclusion criteria. The remaining 46 articles were assessed for study eligibility by reviewing the full texts. Articles where full texts were unable to be located online were excluded, after emailing authors twice with no response. Subsequently, 33 studies were excluded with reasons provided, while 13 articles remained for analysis. Figure 1 depicts a PRISMA flowchart that details article identification and selection. Critical appraisal was conducted on these 13 articles with all articles meeting the a priori ROB threshold score of at least 60%.
Study characteristics
The 13 included studies were conducted in ambulance services in multiple countries:
USA (n = 5),37–41 Australia (n = 3),42–44 England (n = 1), 45 Italy (n = 1), 46 South Africa (n = 1), 47 Switzerland (n = 1) 48 and Sweden (n = 1). 49 All but one of the articles, 49 were conducted retrospectively, analysing data that had been routinely collected by an ambulance service as part of patient management. All the included studies analysed paramedic analgesic practices, with eight articles specifically investigating sex as a primary outcome.38–43,45,48 Study results are listed in Table 1.
Characteristics and results from included studies (n = 13).
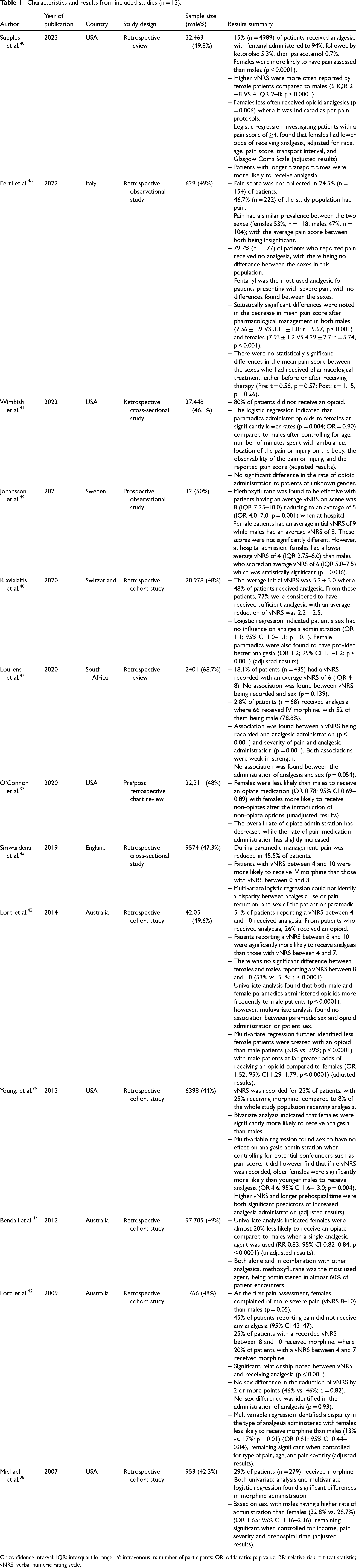
CI: confidence interval; IQR: interquartile range; IV: intravenous; n: number of participants; OR: odds ratio; p: p value; RR: relative risk; t: t-test statistic; vNRS: verbal numeric rating scale.
Summary of the studies
Effect of patient sex on provision of analgesia
Seven of the studies indicated some form of sex disparity in the administration of analgesia.37,38,40–44 This disparity was predominantly in favour of males, with females having a significantly higher risk of oligo-analgesia. That is, females are statistically less likely to receive analgesia, specifically opioids in majority of these studies, in comparison to their male counterparts. This disparity remained significant in these studies when confounders including type of pain, age, pain severity, and time under prehospital care, were controlled.38,40–43 Lord et al. 42 identified that there was no sex disparity in the administration of methoxyflurane and/or morphine as a whole, however when looking at morphine specifically, males were significantly being administered morphine at a higher rate. O’Connor et al. 37 investigated non-opiate and opiate administration, with the results indicating that males had a higher rate of being administered an opiate whereas females had a higher rate of non-opiate administration. Supples et al. 40 noted that whilst females were more likely to have their pain assessed and reported higher pain scores overall, males had statistically higher likelihoods of receiving analgesia. Wimbish et al. 41 found sex to be a statistically significant factor on opioid administration, however found opioid administration was not influenced by patients classified as ‘unknown gender’.
The study by Young et al. 39 investigating patients presenting with blunt trauma, found that older females were more likely than younger males to receive analgesia if no pain score was recorded. However, in the entire study population it was found that sex had no effect on analgesia. This understanding was further highlighted in the other included studies which indicated that analgesic administration was not influenced by the sex of the patient, even after controlling for potential confounders.39,45–48
Effect of paramedic sex on provision of analgesia
Three studies investigated paramedic sex and its influence on analgesic administration.43,45,48 Kiavialaitis et al. 48 found that female paramedics provided better analgesia overall than male paramedics, whereas Lord et al. 43 and Siriwardena et al. 45 found that the sex of the paramedic was not a relevant factor for the rate of analgesic administration.
Effect of pain score on analgesic administration and effectiveness
While the study by Johansson et al. 49 did not comment on the difference in analgesic administration, it identified that females reported a higher vNRS for their pain at the beginning of a patient interaction and a statistically significant lower vNRS at hospital admission. Supples et al. 40 and Lord et al. 42 also reported on females having higher initial vNRS, whereas Lourens et al. 47 was unable to find an association with pain score and sex.
Consistent throughout the studies, was that the higher the vNRS, the greater the likelihood of receiving analgesia.39,42,43,45,47 This relationship was found to be statistically significant in two of the studies.42,47 For patients who were administered analgesia, three of the studies indicated that the analgesia was effective in reducing patients’ vNRS by the time of hospital admission.45,48,49 Lord et al. 42 found that there was no significant difference in analgesic administration and no difference in the reduction of vNRS by 2 or more points when comparing females and males.
Risk of bias
All studies met the methodological quality rating threshold of 60% with four studies having a quality rating of 100%,38,40–42 seven having a quality rating of 75%37,43–48 and two having a quality rating of 62.5%.39,49 All ROB scores are listed in Table 2.
Risk of bias assessment of included studies (n = 13) using the JBI critical appraisal tool. 50
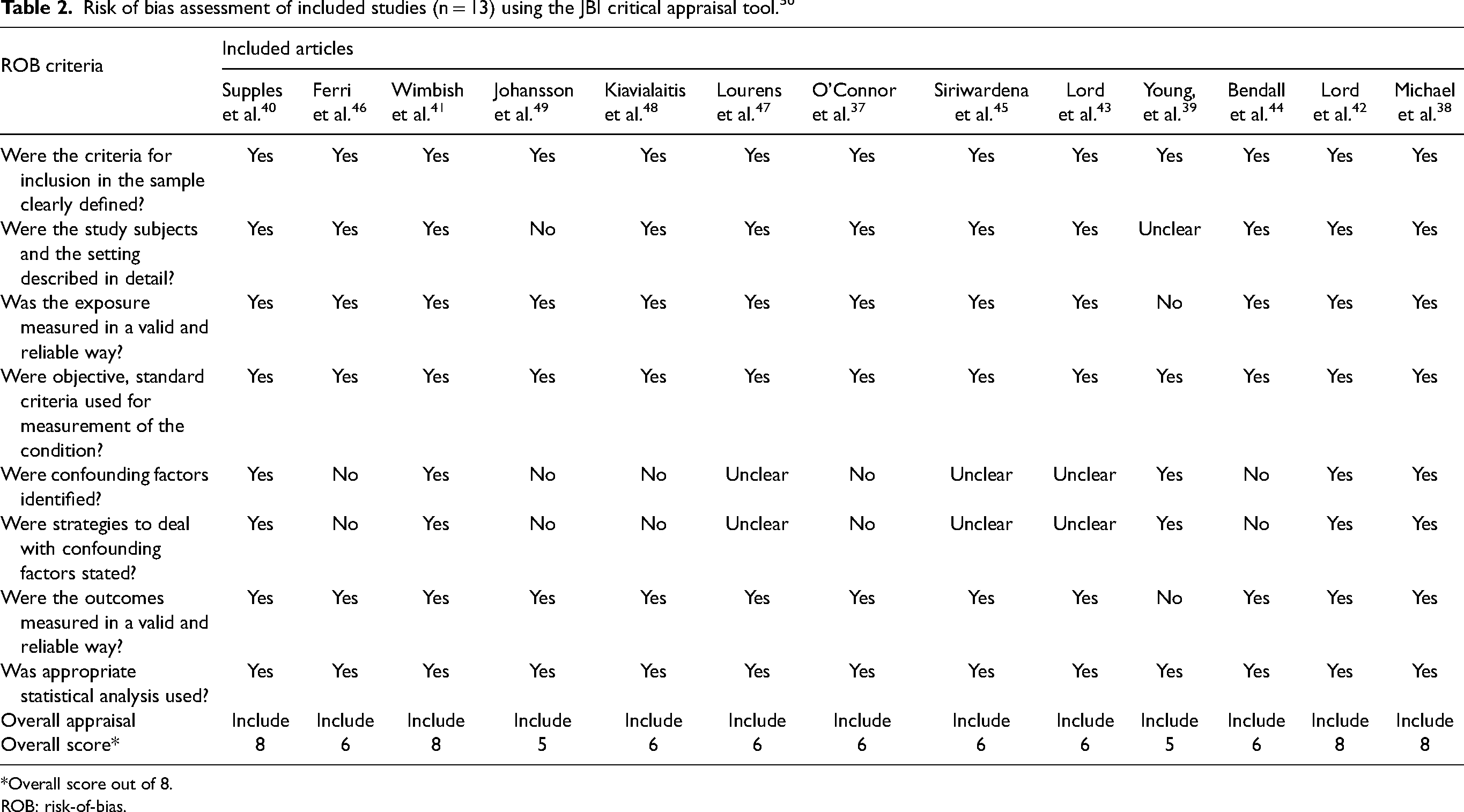
*Overall score out of 8.
ROB: risk-of-bias.
Discussion
From the results of this rapid review, it is evident that there is an inadequate amount of research to indicate if paramedics are treating patients equally when analgesic options are considered. Some studies have indicated that females are disproportionality treated less for their pain, even when the complaints of pain are similar to males.37,38,40–44 This may create an equity of care and patient safety problem in prehospital care, as female patients may go longer without adequate pain relief. This is important to note as some research shows that females experience more severe, longer lasting and recurrent pain.24,51–53 This may therefore indicate that a mismatch in pain presentation and subsequent pain management may exist. This finding is in line with the understanding that pain is subjective and encompasses lived experiences, as well as interactions between biological, psychological and sociocultural factors.2,3,24 Females experiencing higher pain scores was noted in studies by Supples et al. 40 and Lord et al., 42 however both studies found that females were still disproportionally administered analgesia. Bendall et al. 44 identified a sex-specific disparity in their study, however did not list the descriptive statistics and univariate results, nor did they conduct multivariate regression to test for confounders, detracting from the reliability of their results. Only three articles that identified a gender discrepancy posited brief justification as to why this may exist.41–43 However, none of the included studies that identified a sex-specific difference in analgesic administration provided any recommendations on tools or methods to mitigate these differences. All articles made comment on the need for further research into pain management practice in paramedicine.
Three of the included studies indicated that analgesic administration is not affected by a patient's sex and is instead based on the severity of pain described by the patient.39,45,47 These findings therefore give rise to the understanding that although pain is subjective, and is described and experienced differently by different sexes, patients are treated equally in relation to pain management. That is, if an individual is expressing their pain in such a way that it would be considered mild, moderate or severe, regardless of their gender, analgesia was administered appropriately. Two of the studies that identified a sex disparity also supported this same finding, of a higher vNRS corresponding to better analgesia.42,43 This may indicate that in these specific studies, males may have articulated their pain as more severe than their female counterparts, in turn, receiving higher rates of analgesia and creating a de facto sex disparity. However, only two of the studies that identified an analgesic administration and pain score relationship commented on this relationship being statically significant,42,47 with the other studies only identifying vNRS and analgesic administration as an association, detracting from this conclusion. Three of the included studies did comment on the analgesic management provided to patients being effective in reducing vNRS.45,48,49
Only five studies explicitly identified confounding variables and subsequently controlled for them in their regression model.38–42 From these, four found sex-specific disparities in analgesic administration.38,40–42 A further three studies conducted multivariable regression analyses, however did not explicitly state which confounders they were testing for and if they were first found significant using univariate analyses.43,45,48 Two of these studies found no disparity between the genders, in turn affecting the reliability of the study conclusions.45,48
The prospective study by Johansson et al. 49 found, that females had a higher initial pain score, and when treated with the same analgesia methoxyflurane, had statistically significant lower pain scores at hospital in comparison to their male counterparts. This, as a single study, indicates that methoxyflurane may be more effective in reducing pain in females than in males. However, due to this study's small sample size, its conclusion may lack statistical reliability, and therefore requires further investigation.
O’Connor et al. 37 highlight that with the introduction of non-opiates such as paracetamol and ibuprofen, the rate at which analgesia was administered increased. This finding suggests that prehospital services may need to increase the variety of analgesic types, as to better allow paramedics to treat pain more specifically. For example, being able to provide a non-steroidal anti-inflammatory drug for muscular pain as to take advantage of its anti-inflammatory properties in comparison to, or in combination with, an opioid. However, O’Connor et al. 37 made no analysis on the paramedic practices prior to the introduction of the new medications. The study did identify a sex-specific disparity that males had higher rates of opioid administration, however it is unclear if this disparity existed prior to the new medication introductions. An analysis of this would have strengthened conclusions on sex-specific disparities by O’Connor et al. 37
Lourens et al. 47 found an association with higher analgesic administration among higher qualified paramedics, which may be due to access to a wider range of medications. This was similar to Ferri et al. 46 who found that statistically lower rates of analgesic administration were noted in nurse-staffed ambulances, as opposed to ambulances staffed by both a doctor and nurse acting in a paramedic capacity. These findings indicate the need to increase scope of practice through further inter-professional training and education, thorough investigation into how certain medications act differently in males and females, and how to incorporate sex-specificity in analgesic decision making.
The decision to administer analgesia is ultimately made by the paramedic, and therefore a paramedic's personal bias may affect analgesic options. However, as demonstrated in three of the included articles, paramedic sex had no influence on the likelihood of a patient receiving analgesia.43,45,48 Although these findings cannot definitively rule out sex-disparity in pain management, it is evident that patients complaining of severe pain do ultimately receive more analgesia.39,42,43,45,47
Save for the value of equity in healthcare, the authors did not hold any theoretical premise to avoid undue cognitive bias. A posteriori, the authors are aligned with the Swedish researchers Risberg et al. 54 who developed a theoretical model that outlined how gender bias may present in medicine, how it is understood, and how it can be avoided. This is demonstrated by analysing the assumptions surrounding the similarities and differences, and equities and inequities, that exist between males and females in relation to biology, disease, stereotypes, and life experiences. 54 The model has been expanded to other categories of diversity, such as paramedicine, and is suggestive of future research and other conscience raising activities.
Limitations
The first limitation is the dearth of available literature on the topic. This is unsurprising given the neophyte research culture in paramedicine as an emerging profession. This is evident in this review as there was only a small number of studies that were eligible for inclusion, with only eight of them investigating sex as a primary outcome.38–43,45,48 A second limitation is that all but one of the studies that were included for review were retrospective studies and therefore confounding factors that may have affected pain management could not have been proactively controlled for. This means that some results may have been statistically insignificant if controlled for appropriately. A third limitation was that included studies were from a range of ambulance services from all around the world, where prehospital standards of pain management may lack homogeneity. That is, every ambulance service has different paramedic qualification levels, clinical scopes, medications, and protocols that they work within. Therefore, it cannot be determined here whether results are due to ambulance service governance, or innate sex-specific biases. A final limitation of this research was time. As this type of review is rapid in nature, the researchers were limited in the number of databases they could search, and the amount of time spent analysing selected articles.
Conclusion
The research into equitable pain management practice among paramedics is limited. This rapid review highlighted that while some studies have found no sex-specific discrepancy in analgesic administration, half of the included studies identified that males are unduly privileged (rather than placed at risk) with higher rates of analgesic administration, specifically opioids, in comparison to females, and that females were prejudiced with a higher risk of oligo-analgesia. Moreover, many of the studies reported that the higher the pain score, the higher the likelihood of receiving analgesia, with some studies indicating that paramedic administered analgesia was effective in reducing pain score. None of the included studies that identified sex differences provided recommendations on how to mitigate sex-specific discrepancies. Further research needs to be conducted to better analyse sex disparities in pain management in the interest of promoting gender-equity in pain care responses in paramedicine.
Supplemental Material
sj-docx-1-pam-10.1177_27536386241240286 - Supplemental material for Influence of patient sex on pain management practices in Paramedicine: A rapid review
Supplemental material, sj-docx-1-pam-10.1177_27536386241240286 for Influence of patient sex on pain management practices in Paramedicine: A rapid review by Sooaad Dahoud, Paul Simpson and Navindhra Naidoo in Paramedicine
Footnotes
Acknowledgements
The authors would like to express their appreciation to Lily Collison the Medical and Health Science Librarian at Western Sydney University, for her wealth of knowledge and guidance in the creation of the search strategy and navigation of the databases.
Author contributions
This research emanates from the Master of Research thesis by Sooaad Dahoud. The thesis was supervised by Dr Navindhra Naidoo and Associate Professor Paul Simpson. All authors contributed to and approved the manuscript with thesis reference of: Dahoud S. The Influence of Patient Sex on Paramedic Administration of Analgesia for Acute Abdominal Pain [thesis]. [Sydney (Au)]: Western Sydney University; 2023. All authors of this article therefore meet the requirements for authorship.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research and/or authorship of this article. In respect to publication, Paul Simpson is the Editor in Chief of Paramedicine and Navindhra Naidoo is an Associate Editor at Paramedicine. Neither played any role in the review process nor in the editorial decision making process. The paper underwent double-blinded review in adherence to the journal’s peer-review policy.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
