Abstract
Study Design
Case report.
Objective
To highlight the diagnostic and treatment dilemma associated with chronic invasive fungal sinusitis (CIFS) in the immunocompetent individual.
Methods
The patient was initially treated for chronic bacterial sinusitis with antibiotic therapy and multiple surgical debridement with no evidence of fungal organisms. Following the completion of the left partial maxillectomy, mucormycosis was finally identified on histopathology, and the appropriate antimicrobial therapy was initiated. During this time, the patient received an interim maxillary obturator for speech and oral function. Following the resolution of CIFS, a computed tomography (CT) of the face was obtained for computer-aided surgical planning for a vascularized fibula flap reconstruction with endosseous dental implants using patient-specific surgical cutting guides and a reconstruction plate.
Results
Optimal esthetic and functional outcomes were achieved following the placement of the definitive dental prosthesis. The patient remained free of disease and without pain 2 years postoperatively.
Conclusions
Chronic invasive fungal sinusitis in the immunocompetent patient remains rare; however, delayed diagnosis can lead to inadequate treatment and extensive soft and hard tissue necrosis. Obtaining sufficient tissue sampling is essential for a definitive diagnosis of CIFS. This report demonstrates the challenge in diagnosing CIFS and the importance of the multidisciplinary approach to treat CIFS associated with extensive involvement of the maxilla.
Keywords
Introduction
Fungal sinusitis is a rare but serious infection that is associated with the inhalation of certain types of fungus. It is a relatively rare infection and is mostly seen in immunocompromised patients. However, there has been an increase in cases more recently. In immunocompromised patients, the most common type of fungal sinusitis seen is acute invasive fungal sinusitis (AIFS), however, with the advancement of medicine, chronic invasive fungal sinusitis (CIFS) rates have also increased in this subpopulation of patients. CIFS is diagnosed through histopathological evidence of fungal invasion in the sinus lining and soft tissue. 1 The most common fungal sources for CIFS arise from the order Mucorales, with the most common genera being Mucor and Rhizopus. 2 These fungi are generally found in soil and manure and the most common pathway of infection is through inhalation. The organism initially colonizes the oropharynx, nasopharynx, and sinuses and begins to progress through the structures through both direct invasion and vessels. 2
Once the organism has colonized the vasculatures of the face, it promotes thrombi formation causing the characteristic feature of the disease, a necrotic ulcer with black eschar. CIFS can also invade the orbit causing visual disturbances, intracranially leading to motor and sensory deficits. CIFS tends to progress over weeks to even months. Due to this gradual progression of symptoms, early diagnosis of this condition is difficult to obtain, thus delaying the time to provide appropriate surgical and medical intervention. Due to this delay in diagnosis, patients often must go through riskier surgical procedures and stay on intravenous medication regimens. This further contributes to increased morbidity and mortality rates for patients diagnosed with CIFS.
Case Report
A 59 year-old male with a medical history significant for hypertension and renal cell carcinoma who was treated with partial nephrectomy initially presented to an otolaryngologist for recurrent rhinosinusitis involving the right maxillary sinus. He reported recurrent sinus infections with nonpurulent drainage that had been present for most of his adult life. These were treated with multiple courses of antibiotics including clarithromycin and clindamycin. He Denied** any history of tobacco, alcohol, or substance use. He had also previously undergone 2 functional endoscopic sinus surgeries (FESS) without symptomatic improvement. He also reported completing an 8-month course of oral steroids which induced diabetes mellitus with a hemoglobin A1C of 11.5% but has improved to 5.5% following its discontinuation. A nasoendoscopy was performed and showed a large inferior septal perforation extending the length of the nasal septum, bilateral posterior fontanelles (between the middle and lower concha and behind the uncinate process and anterior to the palatine bone), with streaming mucopurulence in the nasopharynx, and surrounding boggy erythematous mucosa. Additionally, there was exposed non-vital bone around an oroantral fistula of the right maxilla. Based on these exam findings, a biopsy of the right vestibular sulcus was performed, and the patient was subsequently started on a 10-day course of trimethoprim/sulfamethoxazole 875 mg/125 mg twice daily and chlorhexidine .12% mouth rinses. The biopsy showed ulcerated benign squamous mucosa with acute and chronic inflammation, and was negative for malignancy and fungal organisms. Microbiology showed very minimal growth of normal microflora including Staphylococcus haemolyticus and Prevotella melaninogenica. A magnetic resonance imaging (MRI) of the face was then obtained to evaluate for osteomyelitis and the patient was subsequently referred to our unit for further treatment.
Clinical Examination
When he presented to our clinic, he complained of issues with articulation, nasal regurgitation, velopharyngeal insufficiency, and bilateral maxillary sinus pain. On examination, there was no facial swelling or asymmetry. Intraoral examination showed bilateral palatal swelling with purulent drainage at the right maxillary cuspid. Exposed and necrotic alveolar bone was also evident bilaterally with the right being worse than the left (Figure 1). Clinical photo of maxilla with exposed necrotic bone (a), CT face, coronal view (b), and MRI face, coronal view (c).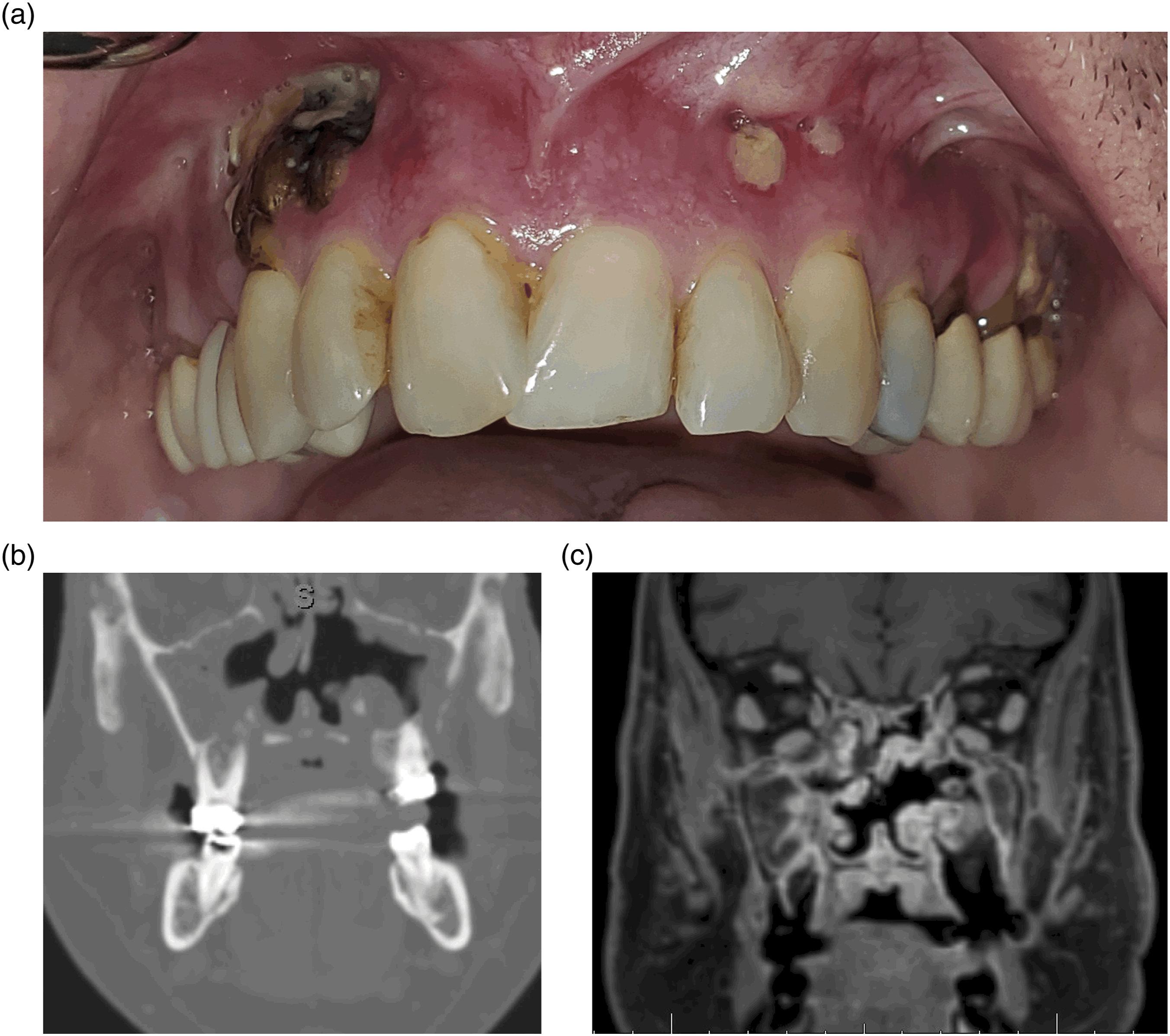
Preoperative Imaging
A computed tomography (CT) of the neck and soft tissue with contrast was performed and showed extensive destructive changes of the maxilla and hard palate with diffuse sclerosis and thickening of the maxillary sinus walls indicative of chronic sinusitis (Figure 1(b)). There was also a lack of soft tissue coverage involving the alveolar ridges with small foci of gas and fragmentation of the hard palate which was suggestive of osteonecrosis in the setting of chronic osteomyelitis. The MRI of the facial bones showed the development of bilateral soft tissue enhancement in bilateral molar eminences with the right side being worse (Figure 1(c)).
Infectious Disease Evaluation
Based on the extent of the disease and its progression without improvement following multiple courses of antibiotics and biopsies negative for fungal pathogens and malignancy, infectious disease was consulted for recommendations. Since the patient did not have a prior history of diabetes mellitus before steroid use, known immunocompromising conditions, or prior chemotherapy for renal cell carcinoma, they recommended surgical intervention with repeat microbiology and pathology on tissue specimens to assist with targeted therapy. Notably, initial immunologic and rheumatologic workups for immunodeficiency and vasculitis were unremarkable.
Surgical Treatment
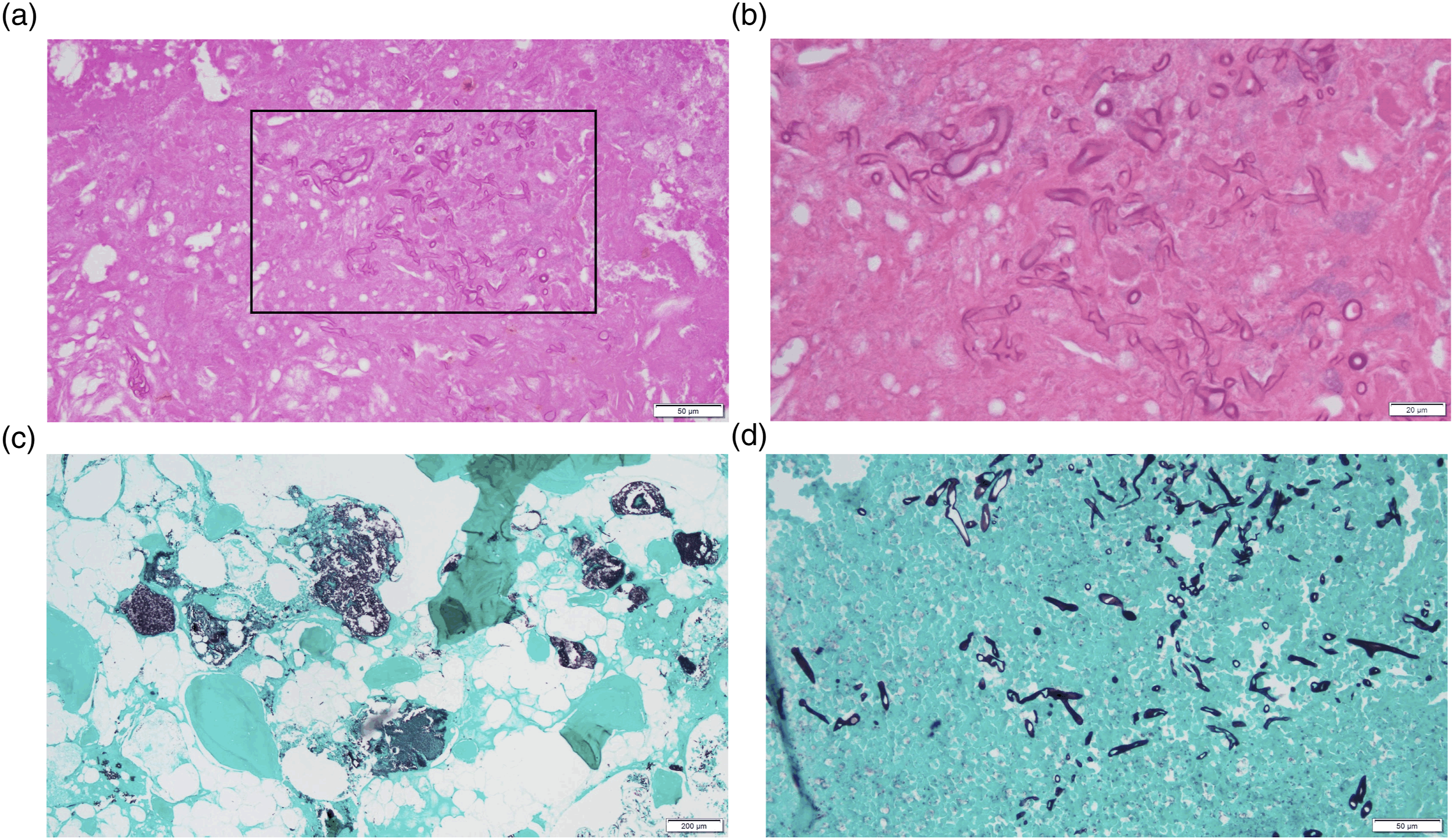
Based on the clinical examination and imaging findings, we proceeded with a right partial maxillectomy and debridement of the surrounding sinus cavity (Figure 2). Intraoperative cultures on the surgical specimen grew Serratia marcescens, Eikenella corrodens, and Aggregatibacter aphrohilus, but no fungal species. The patient was then placed on a 6-week course of piperacillin/tazobactam, 10.125 gm continuous intravenous infusion daily. A completed left maxillectomy with bone debridement was performed 3 weeks following the initial surgery (Figure 2). Again, the tissue specimen was sent for culture and showed mixed fungal and bacterial organisms including Staphylococcus epidermis, Streptococcus parasanguinis, Pseudomonas aeruginosa, Klebsiella pneumoniae, and a few Candida tropicalis. Based on the new culture results, the patient was then transitioned to oral antibiotics (amoxicillin/clavulanic acid 875 mg/125 mg twice daily and ciprofloxacin 750 mg twice daily) based on culture susceptibility testing. Meanwhile, Candida was determined to likely be representative of the necrotic bone with oral contamination; and thus, was not treated with anti-fungal therapy. Moreover, final histomorphological analysis with fungal staining (hematoxylin and eosin (H&E) and Grocott's methenamine silver (GMS)) on the completion maxillectomy specimen revealed broad aseptate fungal hyphae consistent with the morphology of Mucor (Figure 3). With this new information, the patient was prescribed posaconazole 300 mg daily for 15 weeks. Right partial maxillectomy specimen (a), left partial maxillectomy specimen (b), maxillary defect following right partial maxillectomy and debridement of sinus (c), and maxillary defect following completion infrastructure maxillectomy and debridement (d). Hematoxylin and eosin (H&E) staining of the tissue samples. (a) 20X - H&E. Broad aseptate fungal hyphae consistent with Mucor, marked in black box. (b) 40X - H&E showing presence of Mucor. (c) 10X - GMS staining positive for fungal elements. (d) 20X - GMS staining showing abundant fungal elements consistent with mucor.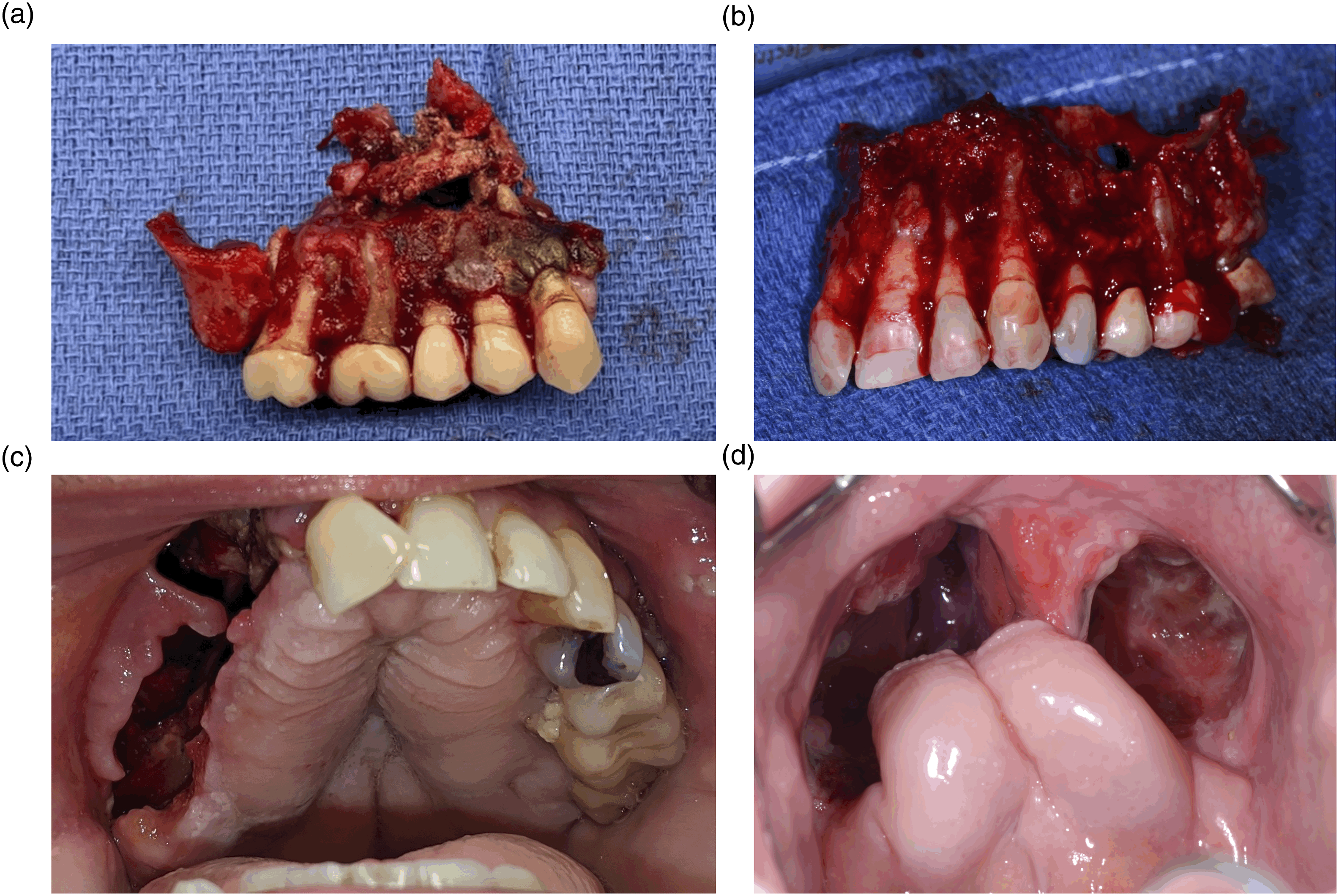
Before definitive reconstructive surgery and prosthetic rehabilitation, the patient was surveilled in the outpatient clinic setting for 4 months on a 2-4 week interval by the otolaryngology, infectious disease, and maxillofacial reconstructive surgery teams to ensure complete disease resolution as well as adequate soft tissue healing. With the aid of computer-assisted virtual surgical planning (VSP), a three-piece vascularized fibular flap with 6 endosseous dental implants, and a custom patient-specific implant were utilized to reconstruct the maxillary defect (Figure 4). The patient had an uncomplicated postoperative hospital course and definitive dental rehabilitation was completed following secondary revision surgery of the fibular flap skin paddle in the outpatient setting. Computer-aided virtual surgical plan with patient-specific implant for vascularized free fibula reconstruction of the maxilla (a) and with 6 endosseous dental implants (b).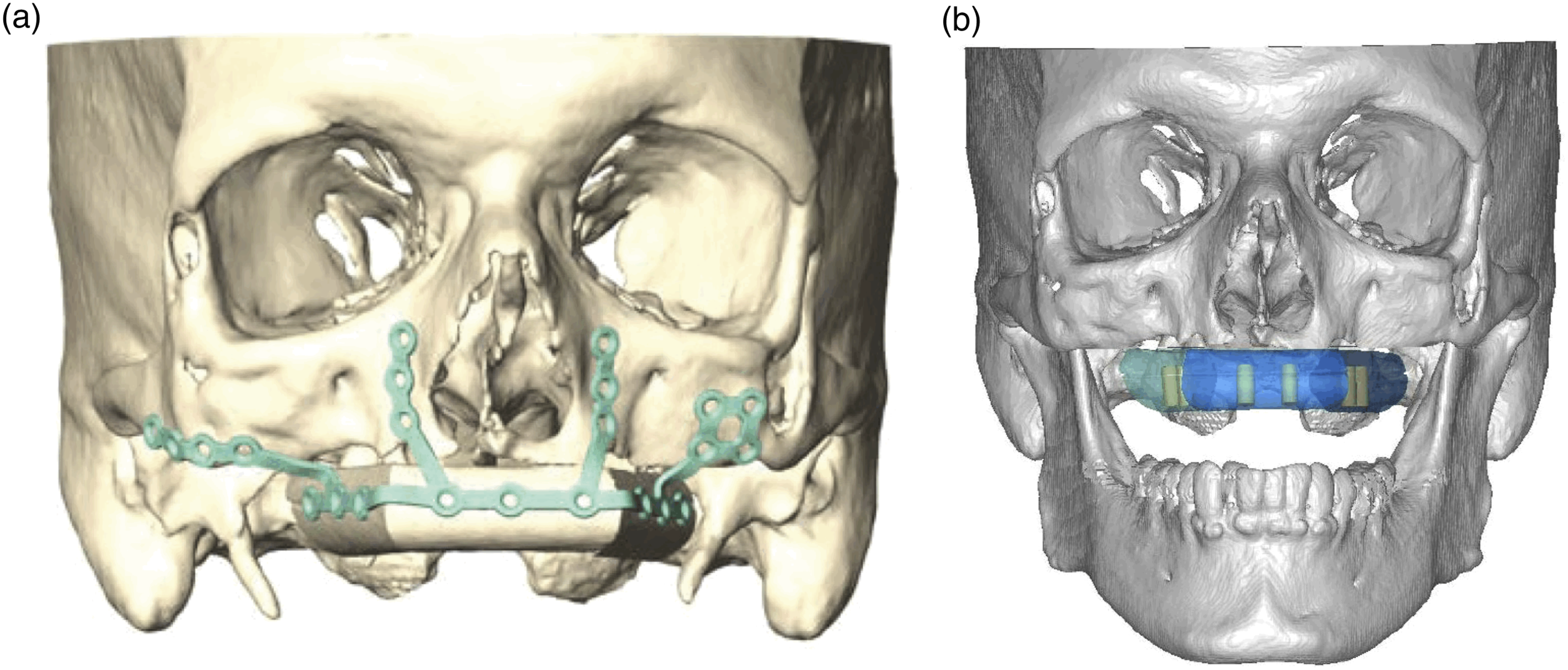
Prosthetic Treatment
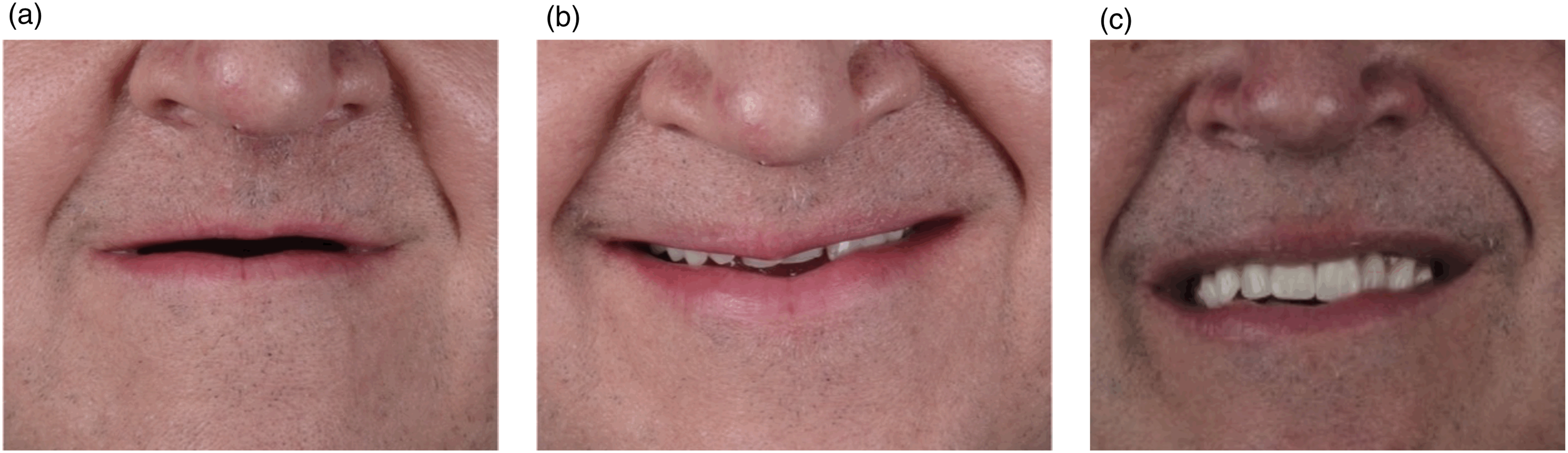
Before the right partial maxillectomy, an immediate surgical maxillary obturator without teeth was fabricated by the maxillofacial prosthodontist using a conventional alginate impression and clear denture base. This was relined with a soft tissue conditioner for immediate use postoperatively. Following the completion of the left maxillectomy and the appropriate healing time of 3 months, a two-piece maxillary interim obturator with teeth was then fabricated using heat-cured denture acrylic resin. The cameo surface of the obturator portion of this prosthesis was embedded with 2 multi-purpose magnets. (Figure 5). Three months following the definitive reconstruction of the vascularized fibula flap with dental implants, definitive prosthetic rehabilitation was initiated. This included the fabrication of an implant-supported removable bar-overdenture by using conventional prosthodontic methods. The final prosthesis provided improved esthetics with increased teeth show by establishing increased vertical dimension of occlusion. It also provided more stability with the use of the implant-supported connector bar (Figure 6). Two-component interim maxillary obturator shown in multiple different views as separate (a and b) and combined unit (c and d). Clinical photos of oral aperture without a prosthesis (a), interim prosthesis (b), and final prothesis (c).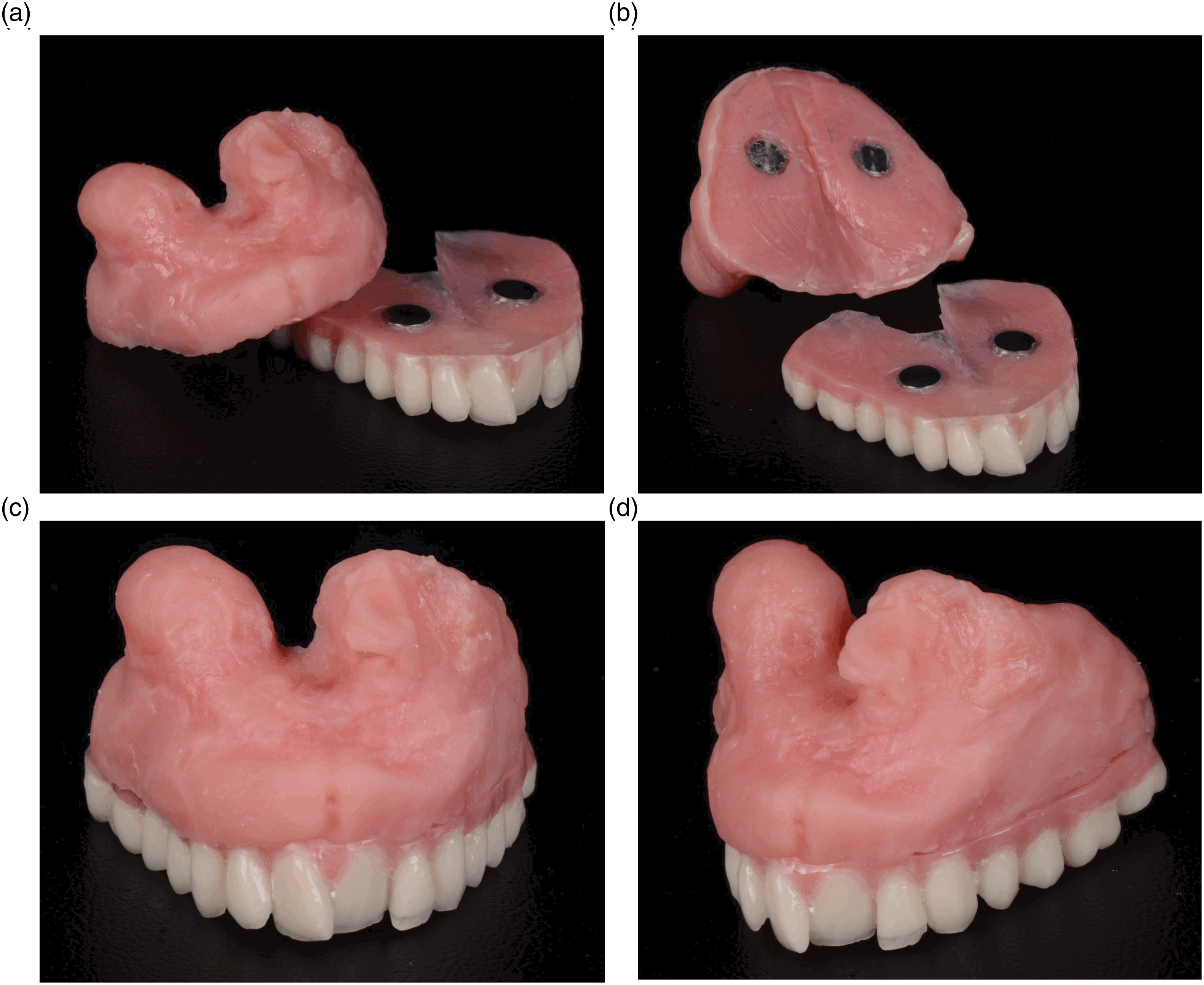
Discussion
Invasive fungal sinusitis is a rare infection that can often become fatal. The annual incidence of IFS associated with Mucor in the United States (US) was estimated to be 1.7 infections per million with approximately 500 cases diagnosed annually. 3 The main risk factors associated with the aggressive form of IFS include hematologic malignancy, poorly controlled diabetes mellitus, organ transplantation, chronic use of iron-chelating agents, and renal insufficiency. 4 McNulty et al reported as many as 70% of patients with rhinocerebral mucormycosis have diabetes mellitus. 5 Furthermore, individuals with diabetes are more susceptible to severe complications related to Mucormycosis compared to healthy individuals. This is because diabetes can impair both innate and adaptive immunity and lead to decreased T lymphocytes, decreased free iron in circulation, and improper neutrophil function. 6 In many cases, the infection is initiated via inhalation of the spores through the respiratory system. Colonization is frequently found in the oral cavity, pharynx, nasal and paranasal cavities. Therefore, the most common clinical form of IFS is rhino-orbito-cerebral (44%–49%), followed by cutaneous (10%–16%), pulmonary (11%), disseminated (6%–12%), and gastrointestinal (2%–11%). 7
Delayed diagnosis of chronic IFS is the most important prognostic indicator for morbidity and mortality in immunocompromised patients. Furthermore, delayed diagnosis of CIFS is commonly attributed to its generalized symptoms and gradual progression that does not warrant surgical intervention or tissue sampling. The most common presenting symptoms include nasal congestion, rhinorrhea, facial swelling, epistaxis, proptosis, and visual deficit.1,8 These non-specific symptoms tend to obscure the index of suspicion for CIFS leading to a delay in appropriate treatment and disease eradication. In the immunocompetent individual, these symptoms can be consistent with acute allergic sinusitis, bacterial sinusitis, or odontogenic infection associated with maxillary dentition. As a result, insufficient conservative medical treatment with antibiotics, decongestants, non-steroidal anti-inflammatory drugs (NSAIDs), and steroids are used as first-line treatment for the symptoms. In some cases, such as the one presented, multiple failed rounds of antibiotic and steroid therapy led to the progression of CIFS. Furthermore, tissue biopsies that were negative for fungal organisms, but positive for bacterial organisms also obscured the definitive diagnosis and treatment regimen.
High morbidity associated with IFS is attributed to the tendency for rapid invasion of vascular structures resulting in soft and hard tissue infarction and necrosis. 9 The mortality rate of IFS remains high with the rhinocerebral form being 62.5% and the disseminated form nearing 100%.3,10 This is attributed to the rhinocerebral form generally being diagnosed sooner than the disseminated form. On the other hand, when the disease is localized to the sinonasal cavity without bony extension, the prognosis is better, and mortality is reportedly lower (10%). 3
While the characteristic necrotic ulcer with black eschar is the hallmark feature of CIFS, this is not always present in immunocompetent patients, such as the one presented in this case report. Furthermore, in the immunocompetent patient, the more common clinical form of IFS is cutaneous rather than rhinocerebral and follows physical injury from a burn or trauma that is contaminated with fungal spores. 9 The perception is that the risk for IFS of the upper respiratory is lower when the immune system is intact. Like the immunocompromised patient, when IFS is localized, diagnosed early, and aggressively treated with systemic therapy, the mortality rate is low. However, when the diagnosis is delayed, the infection rapidly spreads into the orbit and the retro-orbital area; thus, extending into the brain and resulting in the rhino-orbito-cerebral form. According to the reviews of Mucormycosis by Roden et al and Mignonga et al, the rhino-orbito-cerebral form remains the second most common presentation seen in immunocompetent individuals following the cutaneous form with a rate of 25%–38%.11,12 Mignonga et al speculated that in an immunocompetent individual, the presence of chronic localized sinusitis can be a predisposing factor for the development of IFS. 11 This is supported by the notion that chronic sinusitis alters mucociliary clearance in the upper respiratory tract resulting in colonization of Mucor. 13
In this case presentation, an immunocompetent patient had delayed diagnosis following inadequate antimicrobial and steroid treatment with multiple tissue biopsies negative for fungal organisms. In addition, the presenting signs and symptoms were nasal congestion and regurgitation, velopharyngeal insufficiency, mucopurulent discharge, and maxillary pain which were consistent with bacterial sinusitis as opposed to IFS. Unfortunately, the patient also developed steroid-induced diabetes mellitus during treatment, which may have led to disease exacerbation. Based on the presence of chronic sinusitis on presentation and new onset untreated diabetes mellitus, the patient had 2 major predisposing risk factors for IFS.11,14 The definitive diagnosis of IFS was made nearly 1 year after the onset of symptoms. This delay led to extensive necrosis of hard and soft tissue of the maxilla and paranasal sinuses which required a bilateral substructure maxillectomy and a 15-week course of posaconazole before definitive reconstructive surgery with a vascularized fibula flap and dental implants.
While rare, the incidence of IFS in immunocompetent individuals has been reported in 35 countries worldwide with the US being the second most common country following India. 11 This may be attributed to a large and diverse multiethnic population with unequal access to health care and medical services due to socioeconomic factors. 15 The significance of presenting this case was to highlight the importance of early and accurate diagnosis of IFS to prevent the devastating sequelae of CIFS that necessitated extensive surgical resection and reconstruction, long-term antimicrobial therapy, and increased mortality.
Conclusion
Invasive fungal sinusitis in the immunocompetent individual remains a relatively rare phenomenon with a high mortality rate. Furthermore, with delayed diagnosis, the disease process can rapidly progress with extensive soft and hard tissue necrosis requiring major ablative and reconstructive surgery. Therefore, it is important to obtain sufficient tissue sampling, often multiple times when warranted, for an accurate diagnosis to initiate early and aggressive antimicrobial therapy.
Footnotes
Acknowledgements
We would like to acknowledge Dr Alison E. Burkett, MD for the histology images.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Written consent has been obtained from the patient regarding the use of identifiable images.
