Abstract
Epignathus or Tessier fissure 0-14 is a rare teratoma composed of the three embryonic germ layers. Clinically, it appears as a mass covered with skin and mucosa, originating from pluripotential stem cells. According to the latest classification by the World Health Organization teratoma represents the main benign Germ cell tumors of the sinus region and presents similar histological aspects with its counterparts in the gonads and other extragonadal sites. The purpose of this study is to present a case of epignathus originating from the base of the skull in a Caucasian female patient with a cleft palate after the incisive foramen, not affecting the nasal floor. During physical examination, via intraoral route, in the region below the base of the skull, an extensive solid mass, covered by mucosa and with the presence of hair. Computed tomography confirmed the lesion, in the region corresponding to the base of the patient’s skull. The first surgical approach of resection occurred at the 40th day of the patient’s life, under general anesthesia and subsequent primary closure of the palatal defect. The second surgery was performed 10 months later, when tissue expanders were used on the palate to increase the mucosal surface. At the age of 5, the patient underwent surgery with a tongue flap, from the lingual dorsum, with an anterior pedicle. The patient was kept under sedation and relaxation for a period of 10 days for flap autonomy. After this period, the section of the flap and the reconstruction of the tongue dorsum were performed. The patient had a good evolution and was maintained under outpatient treatment. Pediatricians and pediatric dentists should be aware of the importance of prenatal exams and soon after birth, to identify possible deformities in neonatal patients, which favors the diagnosis. The 17-year postoperative follow-up of complete surgical removal of the teratoma and reconstruction of the cleft palate, combining the use of a tissue expander on the palate and a flap on the dorsum of the tongue, proved to be a viable resource for improving the patient’s quality of life.
Introduction
Germ cell tumors (GCT) can affect pediatric and adult patients. Teratoma is an example of these tumors, 1 formed from multiple tissues, which are not native to their site of origin2,3, derived from the three embryonic follicles (ectoderm, mesoderm and endoderm),3,4,1 due to changes that occur between the 4th and 5th week of intrauterine life. 5 The occurrence is observed in approximately 1:4.000 births, with a predilection for the female gender.4,6 The most common sites of occurrence of this tumor are the sacral-coccygeal region, anterior region of the mediastinum, ovary testis or retroperitoneum. 7
According to the latest World Health Organization (WHO) classification, teratoma represents the main benign GCT of the sinus region and presents histological aspects like their counterparts in the gonads and other extragonadal sites. 2 Teratomas of the oral region are rare, being observed exclusively in pediatric patients, usually in neonates, 4 representing 2-9% of teratomas. 4 These tumors are known as epignathus6-9 usually derived from the palate or base of the skull. 6
Teratomas of the head and neck region represent 6% of all these tumors, and may affect the sinus tract, maxillary sinus, nasopharynx, and cervical region.2,7 In adults, immature teratomas present a risk of developing malignant behavior.1,3
The treatment of teratomas consists of surgical removal,1,2,4,9 with no cases of recurrence being reported. 4 The present work aims to describe a clinical case of an extensive teratoma affecting the skull base region of a neonate patient.
Case Report
Caucasian female patient, 40 days old (2006), with cleft palate post-foramen incisive. 10 The Spina classification uses the incisive foramen as an anatomic reference and provides a division of the congenital malformations of the face into 4 groups (I, II, III, and IV). In this case, the various groups refer to the type of cleft, namely: group I, pre-foramen (complete, incomplete); group II, trans-foramen; group III, post-foramen (complete, incomplete), and group IV associated with rare clefts of the face that are not related to the incisive foramen. 11
Physical examination revealed, intraorally, in the region below the base of the skull, an extensive solid mass, covered by mucosa with no change in color, and with the presence of hair. The patient did not have nasal floor. Due to the extension and location of the lesion, the patient was intubated for airway control (Figure 1A). (A) Teratoma and hair (palate region). (B) First surgical approach. (C) Teratoma exposure. (D) Surgical specimen.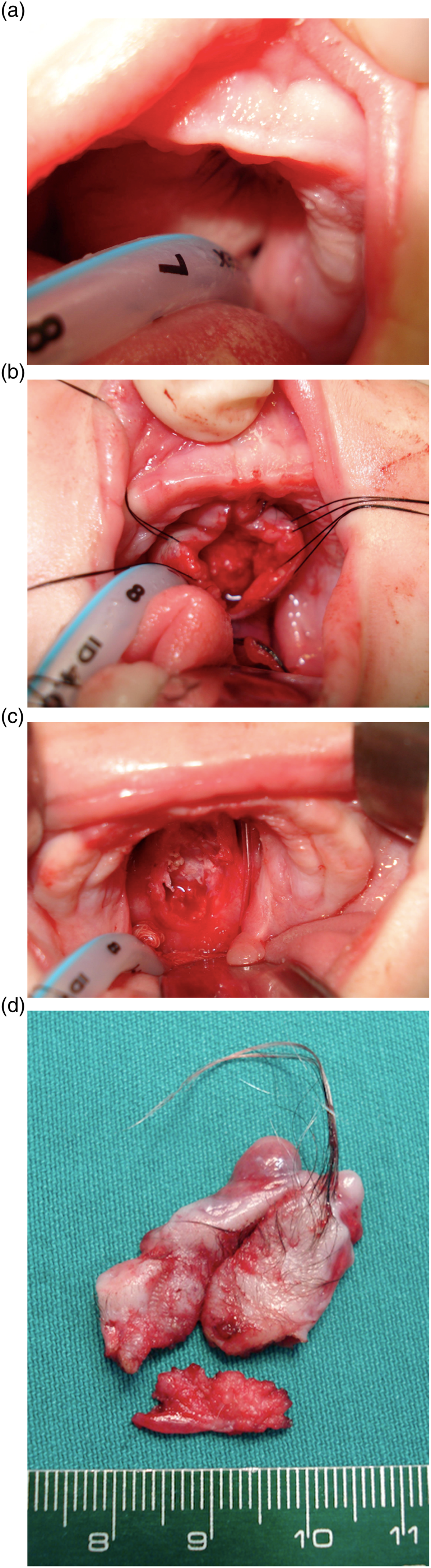
The computed tomography scan confirmed the presence of the mentioned lesion in the region corresponding to the base of the patient’s skull (Figure 2A and B). The proposed treatment was surgical resection of the lesion under general anesthesia and subsequent primary closure of the palatal defect, without success, due to the large defect present. The biopsy (Figure 3) revealed it to be a mature teratoma (bone and dermal tissue). (A) CT scan, axial section showing teratoma. (B) CT scan, sagittal reformation showing teratoma. Biopsy conclusion: mature teratoma (bone and dermal tissue).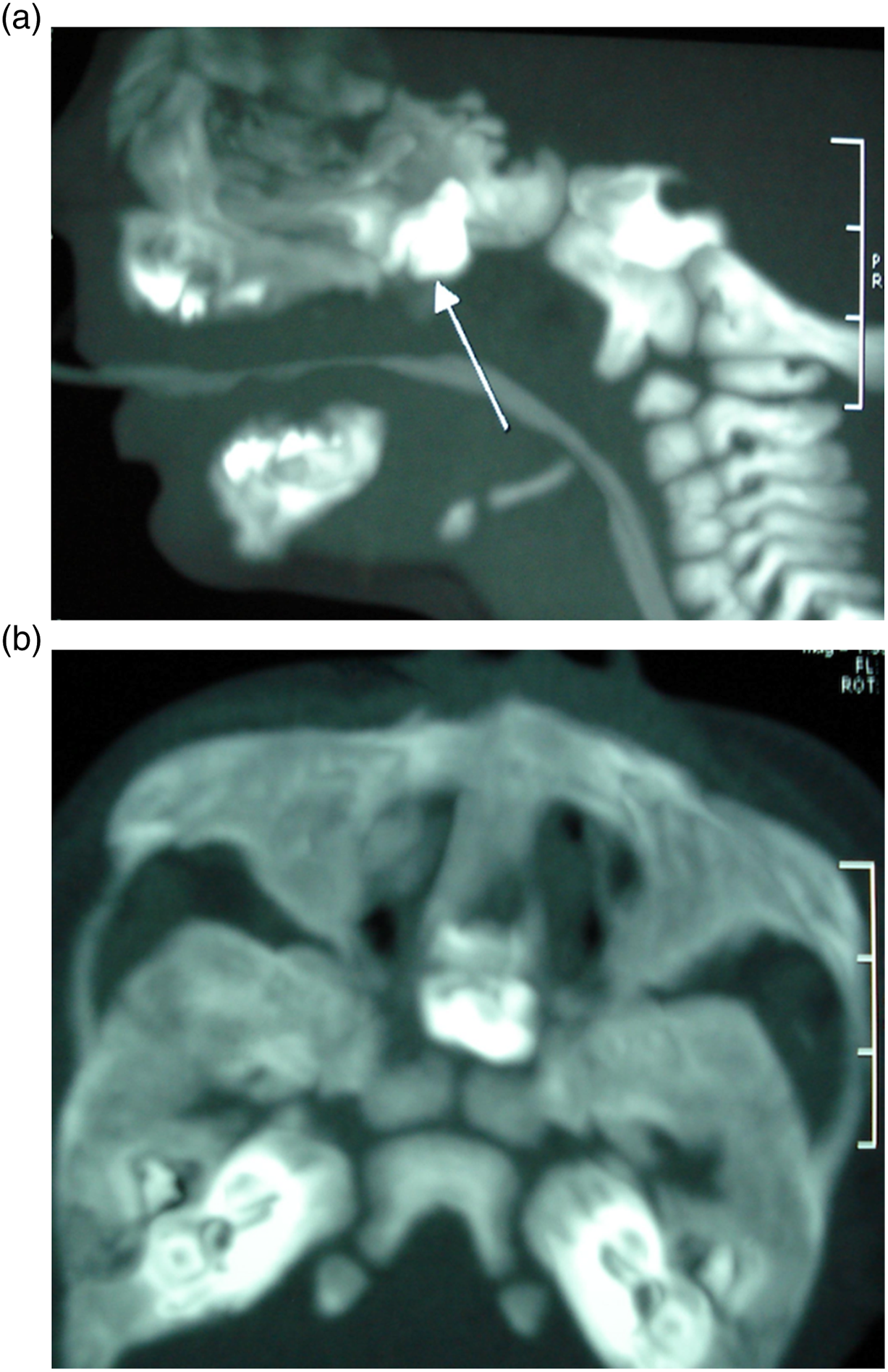

The first surgical approach of resection occurred at the 40th day of the patient’s life, under general anesthesia and subsequent primary closure of the palatal defect (Figures 1B-D).
The second surgical approach was performed 10 months later, when tissue expanders were used on the palate to increase the mucosal surface (Figures 4A and B). (A) Second surgical approach: tissue expanders were used on the palate to increase the mucosal surface – unilateral view. (B) Second surgical approach: tissue expanders were used on the palate to increase the mucosal surface – panoramic view.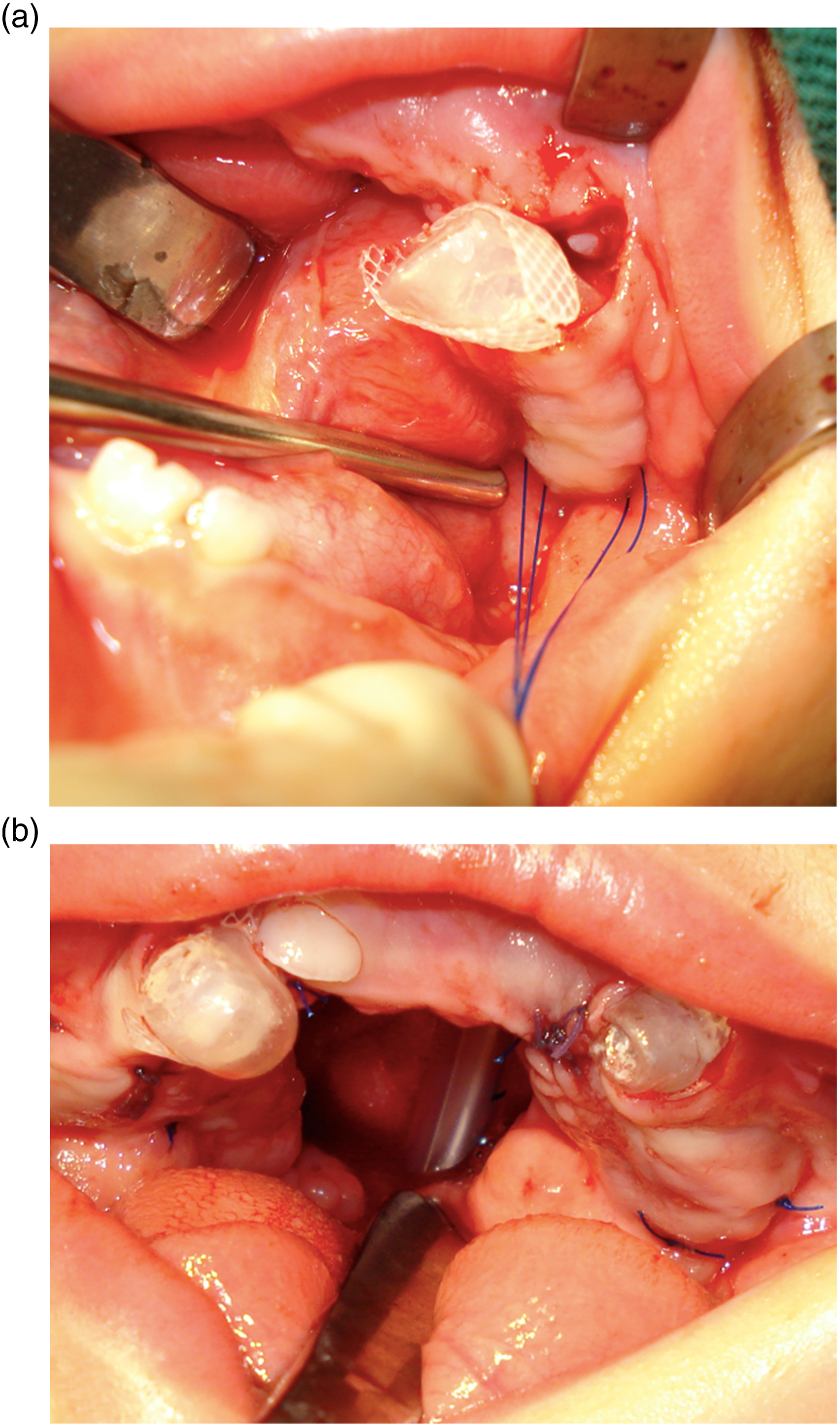
At the age of 5, the patient underwent surgery with a palatoplasty to close the nasal floor (Figures 5A and B) after inverting the expanded palatal mucosa and then a tongue flap (Figures 5C-E), from the lingual dorsum, with an anterior pedicle, an anterior-based dorsal tongue flap.
12
Three millimeters of muscle were included in the tongue flap to allow for adequate vascularization.
13
The tongue flap was then rotated forward and sutured to the raw edges of the palatal defect anteriorly and laterally (Figures 5F and G). After mobilization of the lingual flap, the donor site was sutured with 3-0 nylon interrupted sutures as guide sutures and then with resorbable continuous suture resorbable (Figure 5E). (A) Before palatoplasty. (B) Nasal floor closed after inverting the expanded palatal mucosa. (C) Anterior-based dorsal tongue flap (Guerrero-Santos et al, 1966). (D) Anterior-based dorsal tongue flap 6.7 cm long. (E) Tongue flap before being positioned on the nasal floor reconstruction. (F) Tongue flap before being positioned backwards. (G) Tongue flap positioned.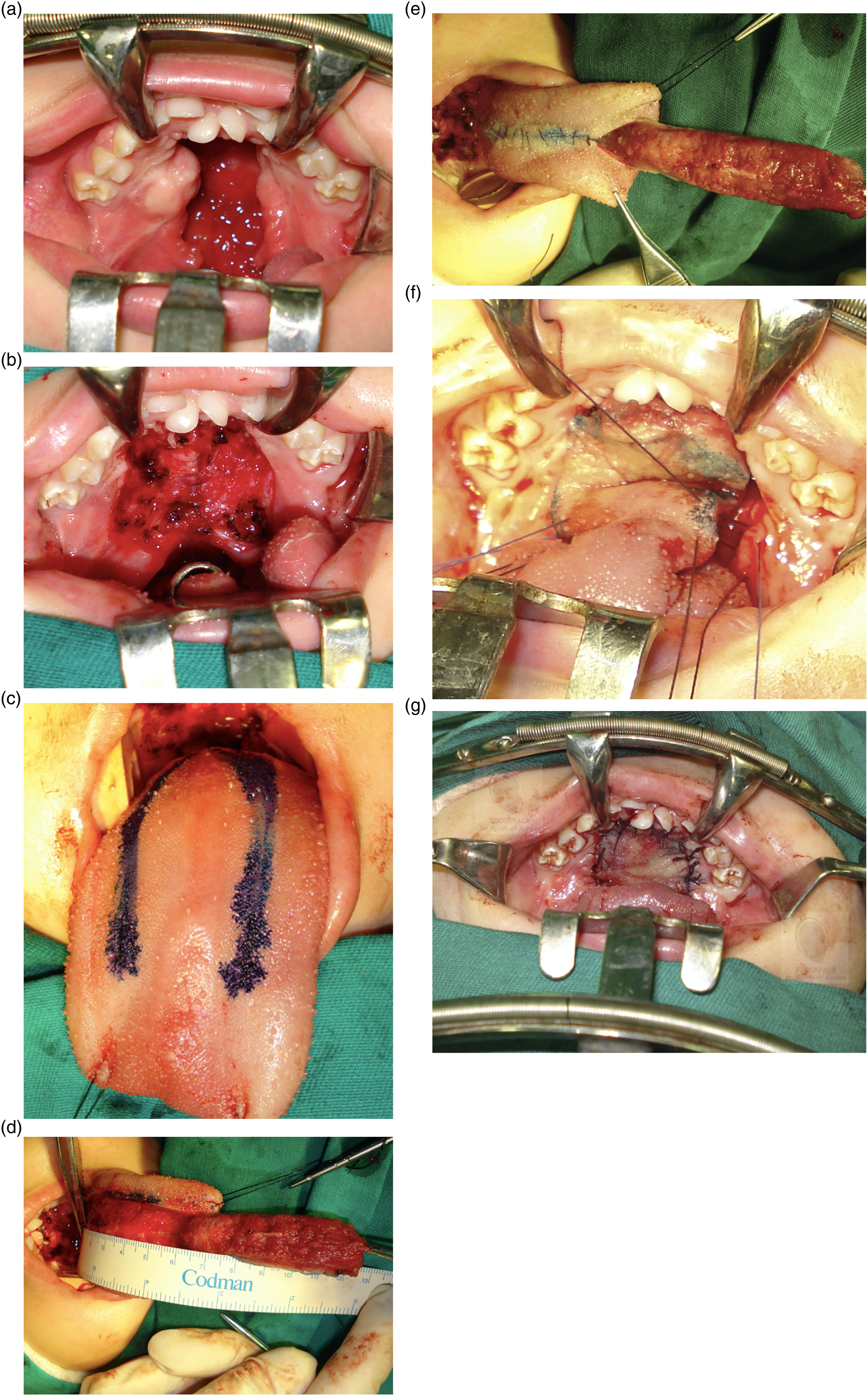
These 2 steps, closure of the nasal floor and tongue flap, allow the adequate palatal closure. The patient was kept under sedation and relaxation for 10 days for flap autonomy. After this period, the section of the flap, and the reconstruction of the tongue dorsum were performed (Figures 6A and B). (A) Section of the flap. (B) Tongue apex reconstruction. (C) 17-year follow-up (donor site). (D) 17-year follow-up. Palatal reconstruction. Aligned and level teeth.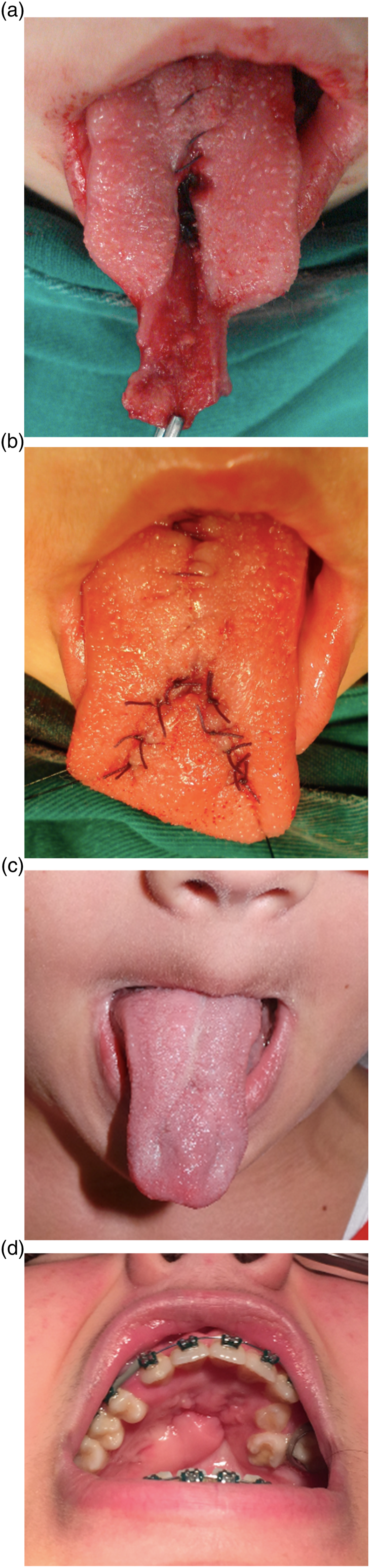
In a 17-year postoperative follow-up of the complete surgical removal of the teratoma, the patient does not show signs of recurrence and shows improvement of the palatal defect (Figures 6C and D).
Discussion
The etiology of epignathus is unknown, with the most accepted theory being that this tumor originates from the disorganized growth of pluripotent cells in the region of Rathke’s pouch.4,7 Its occurrence is rare, being observed exclusively in children, usually in neonates, with an incidence that varies between 1:35 000 to 1:200 000 of live births, with a prevalence observed in female patients. 4
According to the literature, most oral teratomas present with a pedicle at the base of the skull, 14 the same fact being observed in the present clinical case. Diagnosis of this lesion is extremely important, as the presence of this tumor may require maintaining the airway of patients, due to the risks of airway obstruction and death from asphyxia.3,6,7,15
Microscopically, teratoma presents variable mixtures of mature skin, skin appendages, fat, glial tissue, smooth muscle, cartilage, bone, minor salivary glands, respiratory epithelium, and gastrointestinal epithelium2,7 being classified as mature or immature depending on the degree of differentiation of its components. Macroscopically, teeth, hair and fur can be observed 8 In the present study, it was possible to observe the presence of hair in the lesion.
The presence of teratoma may be related to congenital malformations, such as cleft palate, bifid tongue, oronasal fistula, nasal dermoid cyst, and supernumerary teeth in the region between incisor teeth.4,8 In the present study, the presence of the tumor was responsible for the cleft in the region of the palate connecting the base of the skull with the oral cavity, which required secondary reconstruction of this region.
The differential diagnosis: hamartomas, dermoid cyst and heterotropic gastrointestinal cyst, and the presence of tooth(s) inside the lesion confirms the diagnosis of teratoma ³. In adult patients, the presence of teratoma is associated with high rates of malignancy3,15 and with a suggestive nature of benignity in pediatric patients. 15
The treatment means the complete surgical removal of the lesion,2-4,7,15 without recurrence or malignant transformation reported. 4 In the present study, the option consisted of surgical removal of the lesion under general anesthesia, with no recurrence observed in the 17-year postoperative control.
The tongue is an excellent donor area for the reconstruction of soft tissue defects, due to its vascularity16,17 and can be used for the reconstruction of numerous defects in the oral cavity such as defects in the palatal region resulting from tumors and cleft palate. 17 The lingual flap is versatile and safe for use in children. 16 In the present study, the option of reconstructing the palatal defect resulting from the presence of the epignathus was performed with a flap from the lingual dorsum. In the 17-year of follow-up was observed the complete closure of the defect.
Anterior-based dorsal tongue flaps are excellent for reconstruction of the anterior hard palate, anterior buccal mucosa, floor of mouth, lip, vermillion, and commissure defects and are commonly favored for their increased mobility. 17
Conclusion
The present paper aims to alert pediatricians and pediatric dentists about the importance of exams in the prenatal phase and immediately after birth, to identify possible deformities in neonatal patients, which favors the diagnosis. Depending on the case, epignathus can be related to dramatic consequences for newborns. The 17-year postoperative follow-up of complete surgical removal of the teratoma and reconstruction of the cleft palate, combining the use of a tissue expander on the palate and a flap on the dorsum of the tongue, proved to be a viable resource for improving the patient’s quality of life.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
