Abstract
Osteopetrosis is a disorder characterized by an increase in bone density and a reduction in spinal cord spaces. This change results in a defect in osteoclast function and consequent decrease in bone turnover. One of the possible local bone complications is osteomyelitis, which affects up to 10% of patients with this disorder. Platelet concentrates (L-PRF) have been used in cases of bone defects and areas of tissue necrosis, as it has the characteristic of releasing growth factors after activation. The aim of this paper is to present a clinical case of a patient with mandibular osteopetrosis, who underwent dental implantation and subsequent recurrent osteomyelitis and was treated by partial resection associated with L-PRF bone defect coverage. After 1 year of follow-up, the patient presented definitive soft tissue healing, no exposure of bone tissue or phlogistic signs at the site, and good bone repair on computed tomography scan. The present study demonstrated that the association of L-PRF with resection techniques can be a viable method for the management of patients with difficult to treat osteomyelitis, especially in cases of mandibular osteopetrosis.
To the Editor
Osteopetrosis is an uncommon hereditary bone disorder affecting 1 in 250.000 births. Maxillary involvement is rarer than in mandible, and 1 of the possible complications is osteomyelitis, which occurs due to lack of adequate bone vascularization at the site and can be observed in up to 10% of patients. 1 In literature the usage of regeneration techniques is often necessary in case of bone fracture and/or necrosis. Therefore, the application of platelet concentrates, through growth factors may favor the physiological conditions for local bone repair. 2 The aim of this paper is to present a case report of a patient with osteopetrosis mandibular who underwent dental implant installation resulting in chronic jaw osteomyelitis, treated with segmental resection and L-PRF.
A 42-year-old female patient with osteopetrosis attended the Hospital decasecond Clínicas de Teresópolis Costantino Ottaviano-HCTCO, Teresópolis, Rio de Janeiro, Brazil, presenting drainage of purulent intraoral secretion in the mandibular body region, after installation of dental implant, with evolution of 6 months. She reported a history of 2 unsuccessful debridement and local flap procedures under anesthesia local. On cone beam computed tomography (CT), a hypodense area of approximately 10×10 mm in the mandibular body region was observed (Figure 1), confirming the diagnosis of chronic mandible osteomyelitis. Initial computed tomography, panoramic view, with measures of the bone defect.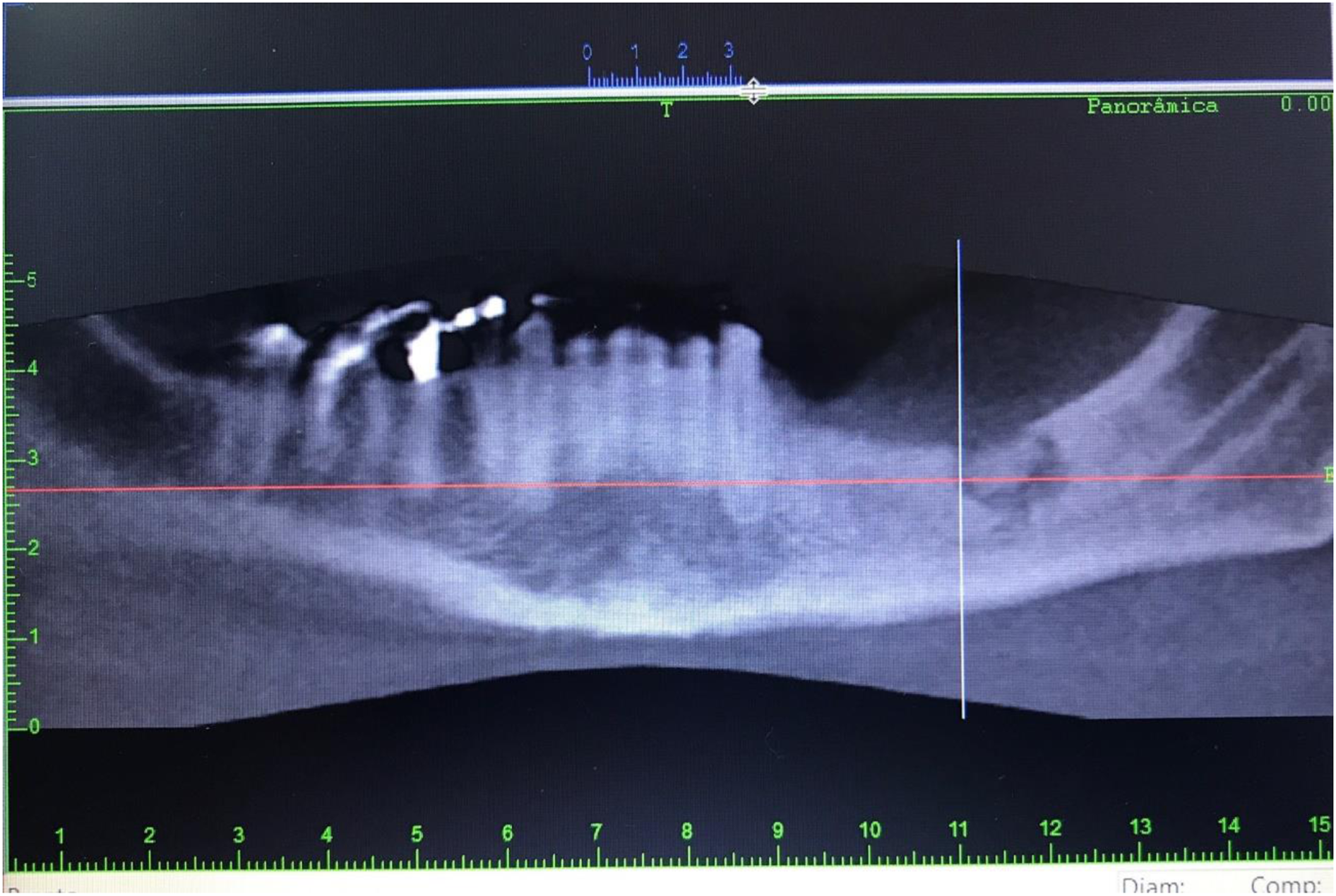
The patient was submitted to surgery under general anesthesia. The intraoral approach was extending from the symphysis region to the mandibular angle, being careful to dissect the mental nerve. A mandibular osteotomy was performed with a piezosonic motor with a 4 × 20 mm osteotomy tip (Traumec®, São Paulo, Brazil) providing a safety margin of 1.5 cm. Healthy bone (Figure 2A). The mandibular body block was removed using elevators, preserving a portion of the cortical base of the mandible, as well as the inferior alveolar neurovascular bundle (Figure 2B). The PRF membranes were prepared as described by Choukroun et al.
3
During surgery, 80 mL whole blood was drawn in 8 glass-coated plastic tubes (Becton Dickinson Vacutainer, 10 mL), without anticoagulant, and was immediately centrifuged at 3000 r/min for 10 min. The resulted fibrin-rich plasma (L-PRF) was compressed to obtain an autologous fibrin membrane, that was accommodated in the bone cavity to assist in local bone repair and better soft tissue coverage. Synthesis was performed with Vicryl 4.0 (Ethicon®, New Jersey, USA) by simple two-layer suture technique
4
(See Figure 3). (A) Osteotomy marking with safety margin, performed with a piezosonic motor with a 4×20 mm osteotomy tip, (B) surgical cavity after osteotomy, with health bone margins. (A) L-PRF membrane according to the Choukroun technique, (B) placement of L-PRF membranes in the bone cavity.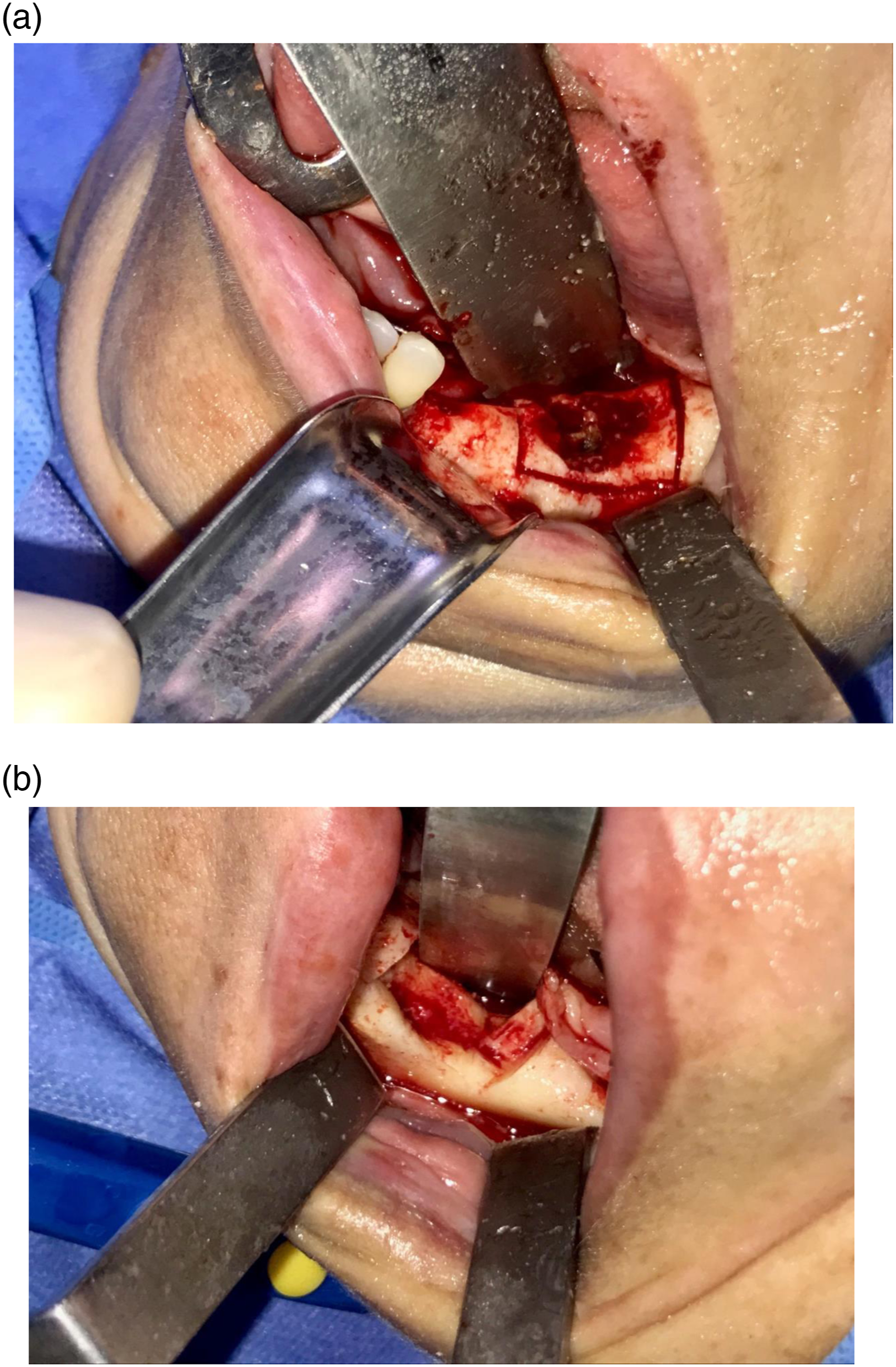
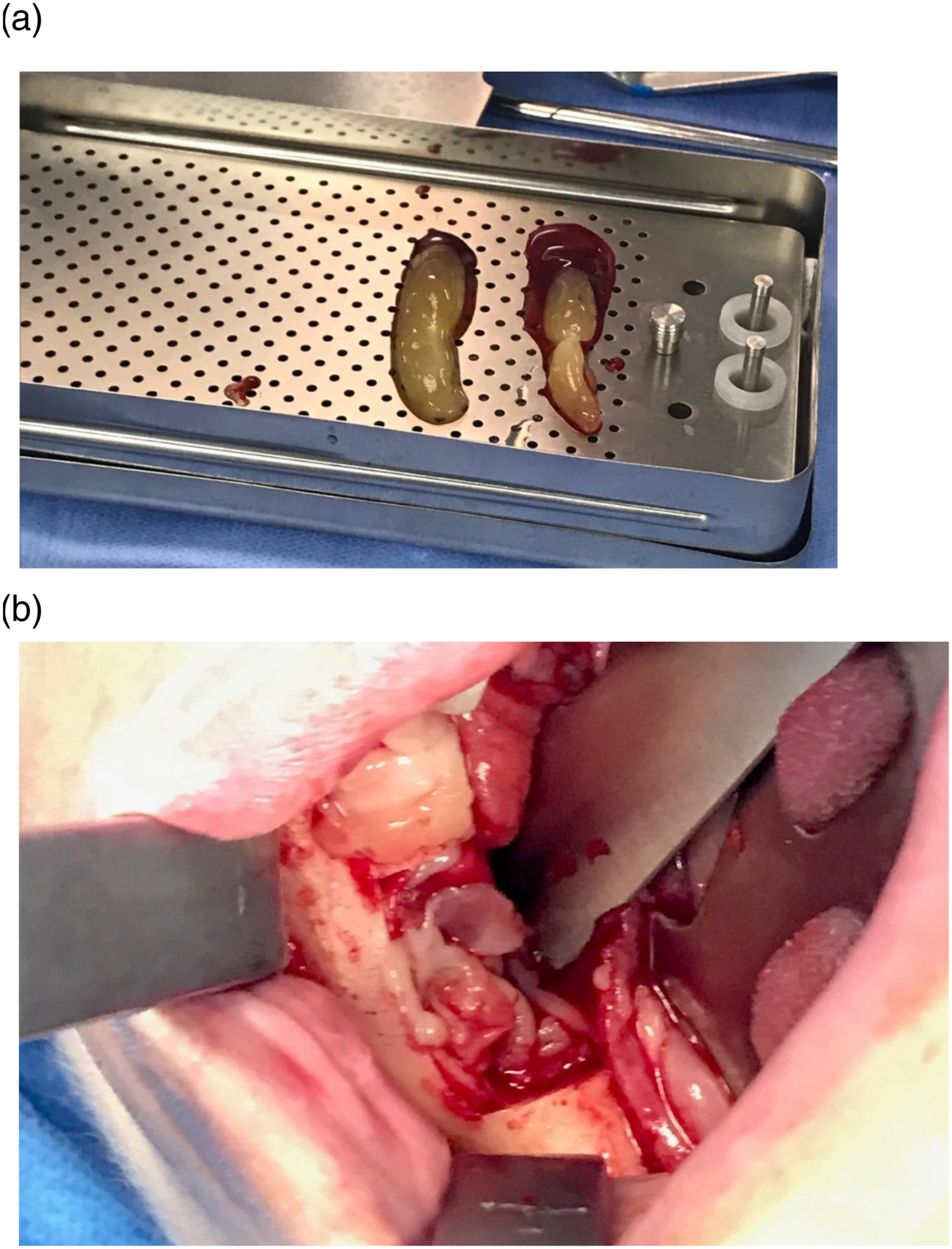
In the immediate postoperative period, the patient presented moderate swelling and good wound healing aspect. Intravenous antibiotic therapy with Clindamycin 600 mg was prescribed, with hospitalization maintained for 5 days. In the 30-day postoperative follow-up, presented good healing of the local soft tissues and the absence of infectious process. After 1 year of follow-up, the condition showed complete soft tissue healing, no exposure of bone tissue or phlogistic signs at the site, and good bone repair on CT scan (Figures 4A-4B). (A) 1-year postoperative panoramic view showing satisfactory bone repair, (B) axial view.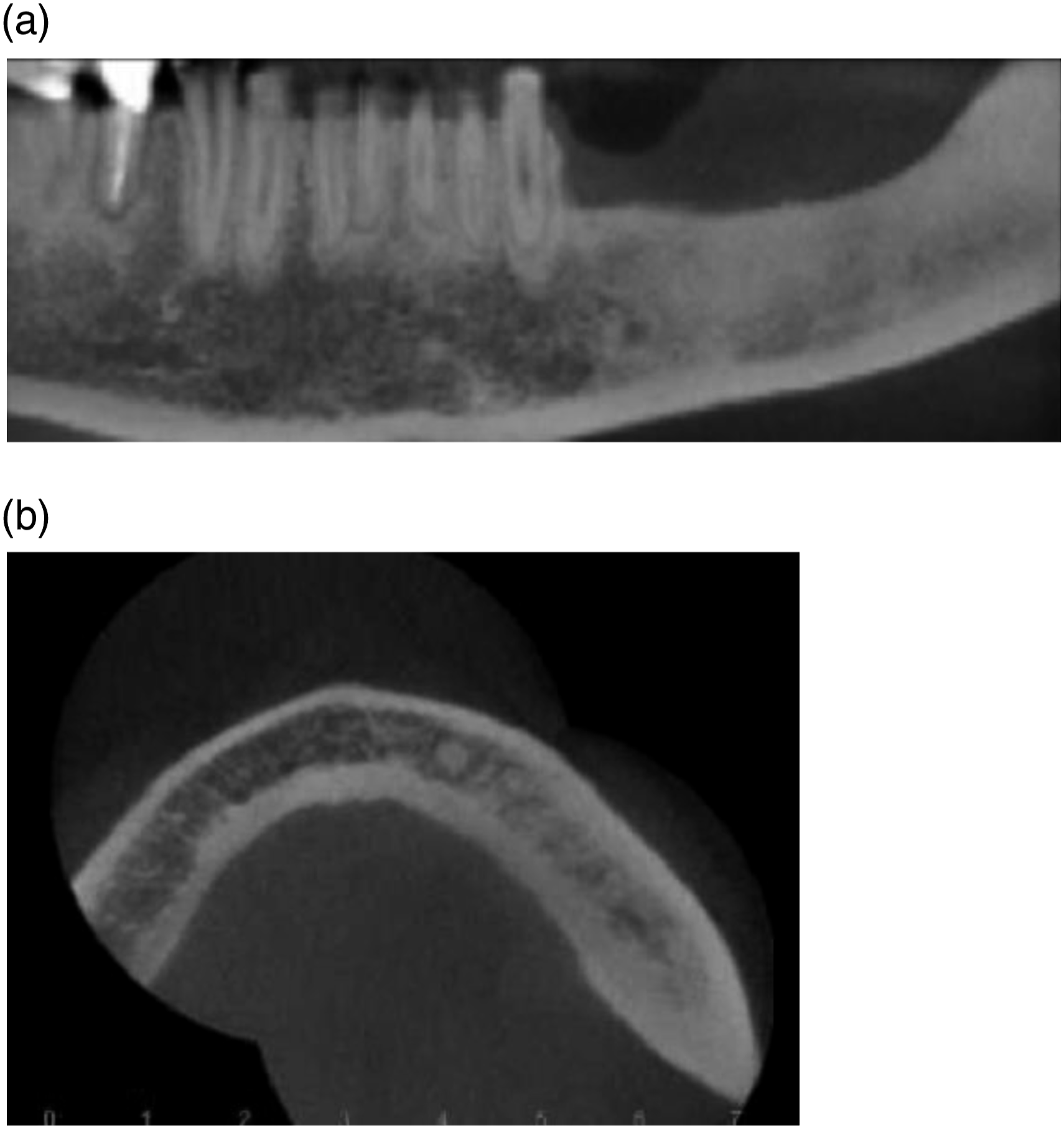
Due to the difficulty in osteomyelitis treatment in patients with osteopetrosis, additional therapies may be indicated to decrease the failure rate such as hyperbaric oxygen therapy and use of local growth factors. 5 The L-PRF allows the release of vascular endothelial growth factor (VEGF), increasing angiogenesis and local cellular recruitment, favoring revascularization and bone repair, as well as reducing the possibility of surgical access dehiscence.
This is the first case where the L-PRF membrane was used as an adjuvant method in the treatment of mandibular osteomyelitis in a patient with osteopetrosis, and despite the good result, more studies are needed to establish a protocol and incorporate this technique into the surgeon’s arsenal.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
