Abstract
Aim
To discuss the clinical presentation of thyroid rupture following blunt neck trauma and highlight key management principles for the case.
Methods
A 45-year-old female motorcycle passenger with a pre-existing right thyroid nodule hit her right anterior neck against a bottle during sudden stop and developed painful right neck swelling, odynophagia, and hoarseness. She was seen at the emergency room 5 hours post-injury, awake, cooperative, and ambulatory, without stridor or dyspnea at room air. On examination, she had ecchymoses behind her right tonsillar pillars; her neck was grossly swollen and was tender on palpation without subcutaneous emphysema. Laryngoscopy showed good left vocal cord mobility while the right vocal cord had a visible hemorrhage and limited abduction due to the mass effect of the hematoma seen at the right aryepiglottic area extending toward the right piriform fossa and the right parapharyngeal area. Intact bilateral vocal cord adduction was noted upon phonation. Contrast-enhanced computed tomography revealed hematoma formation in the right thyroid lobe area with extension to the right side of the oropharyngeal region, anterior cervical, parapharyngeal, and retropharyngeal space, confirming the aerodigestive tract narrowing and leftward deviation previously noted. Baseline thyroid function tests were normal. Under general anesthesia, the patient underwent neck exploration where the ruptured right thyroid lobe was resected, and the hematoma was evacuated.
Results
Postoperatively noted significant improvement in neck swelling, odynophagia, and hoarseness. Transient subclinical hyperthyroidism remained asymptomatic and resolved upon outpatient follow-up. A year after the surgery, the patient had a well-healed cervical scar, complete hematoma resolution, and regained her pre-morbid phonation.
Conclusion
Thyroid gland rupture should be among the considerations for patients presenting with tender neck swelling, progressive hoarseness, and/or dyspnea following neck trauma. Prompt airway assessment and close monitoring for potential compromise are essential to avoid fatal sequelae of external airway compression. Management varies from close observation to surgical neck exploration and should be personalized depending on the severity of thyroid injury and symptomatology.
Background
Thyroid hemorrhage and its potentially fatal sequelae were earliest emphasized in the 1894 report by Simon as cited by Heizmann in 2006 and have since been known as a rare injury arising from various mechanisms of direct and indirect neck trauma. 1 Upon review of the literature, we encountered a wide age range of affected patients presenting with a combination of painful neck swelling, varying degrees of dysphonia and dysphagia, transient thyrotoxicosis, and worsening airway obstruction. To the best of our knowledge, this thyroid rupture case due to blunt neck trauma is the first in our institution and the Philippines.
Case Report
A 45-year-old female motorcycle passenger was riding with her bag in front which contained a water bottle. A sudden stop caused her to hit her right neck and submandibular area against the said bottle. She then presented with a painful enlarging neck, odynophagia, and hoarseness. She first came to the nearest hospital, where she was advised to transfer to our institution for further evaluation and management. The patient was hypertensive, previously diagnosed case of nodular right thyroid lobe, and was scheduled to undergo elective thyroid surgery before the accident.
The patient was seen at the emergency department 5 hours post-injury awake, cooperative and ambulatory, comfortable, without stridor or dyspnea. She had an elevated blood pressure of 140/70 mmHg, a heart rate of 97 bpm, and a respiratory rate of 18 breaths per minute. Her O2 saturation was 98% at room air. On examination, she had ecchymoses behind her right tonsillar pillars; her neck was grossly swollen and tender on palpation without subcutaneous emphysema.
Laryngoscopy showed good left vocal cord mobility while the right vocal cord had a visible hemorrhage and limited abduction due to the mass effect of the hematoma seen at the right aryepiglottic area extending toward the right piriform fossa and the right parapharyngeal area. Intact bilateral vocal cord adduction was noted upon phonation (Figure 1). (A) Visualized parapharyngeal hematoma, right upon examination of the oropharynx. (B) Swelling at the right anterior neck prior to surgery. (C-D) Video laryngoscopy prior to surgery on inhalation (C) and phonation (D).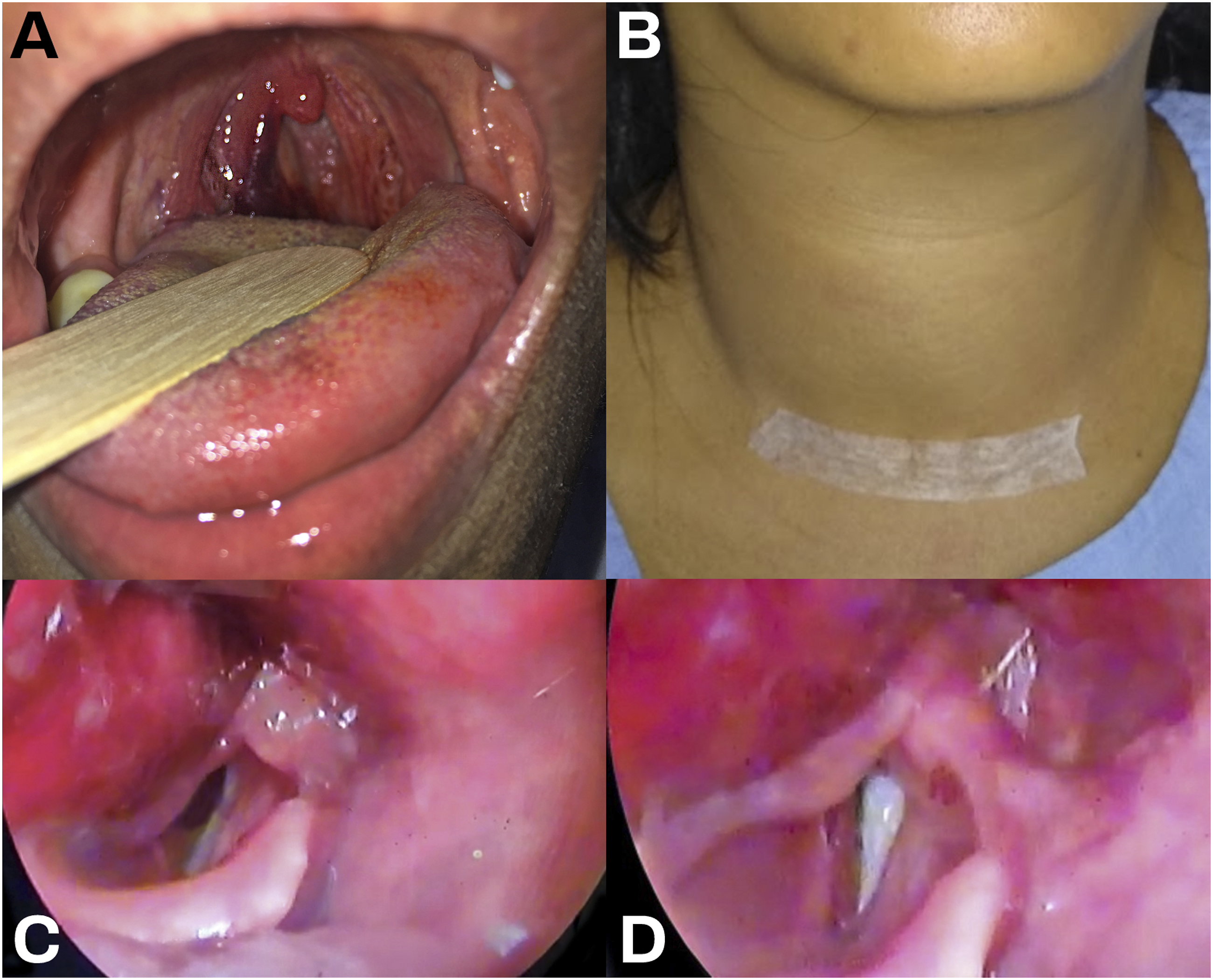
Plain films of the neck revealed prevertebral space thickening with mild leftward and anterior tracheal deviation. No fractures or bony abnormalities were seen (Figure 2). A contrast-enhanced computed tomography (CT) scan was performed to better assess the extent of injury and the mass effect on adjacent structures. Plain films taken at the ER (A) AP view showing mild leftward and (B) soft tissue lateral view showing anterior tracheal deviation with prevertebral thickening.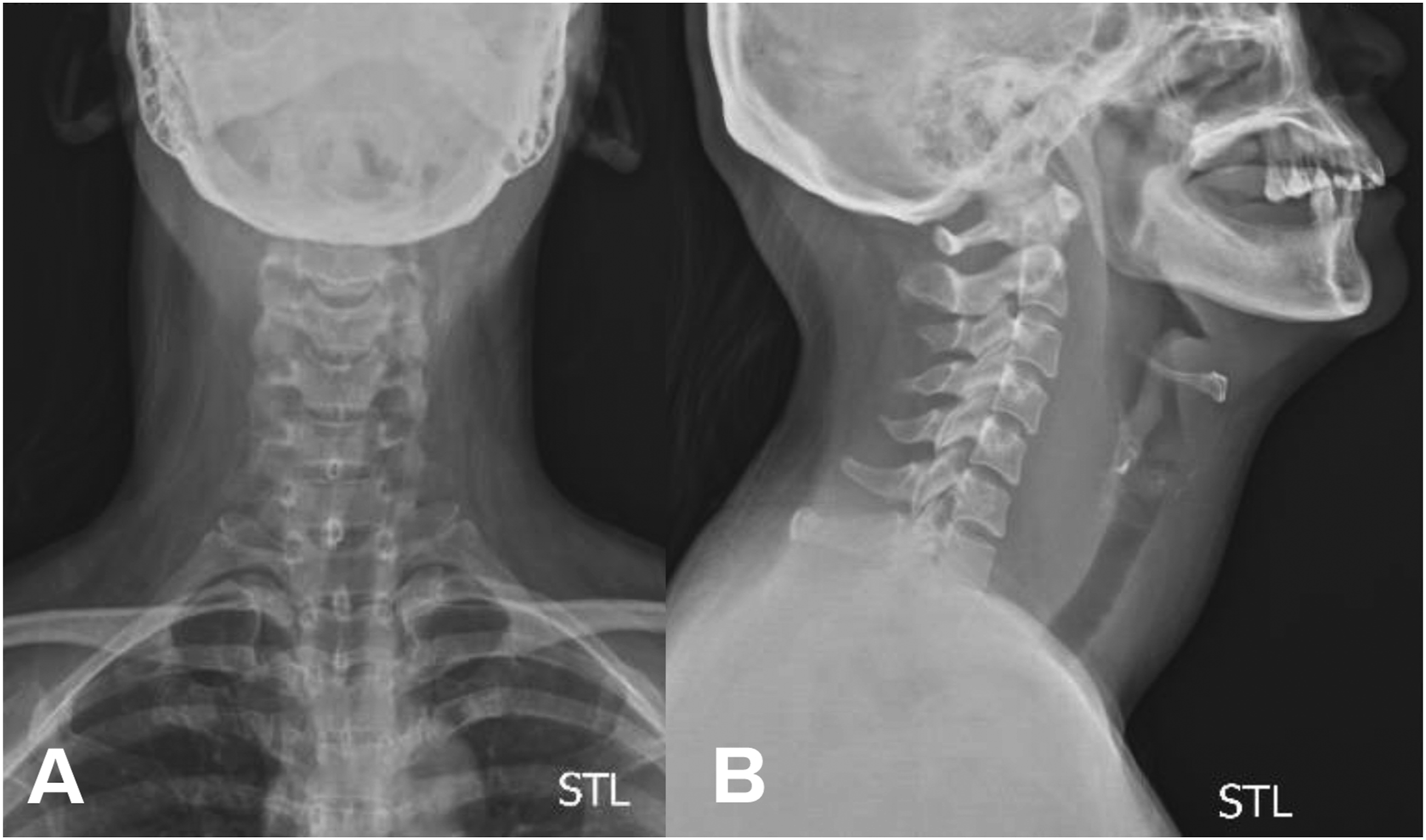
The CT revealed hematoma formation in the right thyroid lobe area, measuring 4.4 × 4.6 × 5.1 cm (APxWxCC). Soft tissue swelling and possible hematoma formation are likewise seen in the right side of the oropharyngeal region, anterior cervical, and parapharyngeal spaces extending to the infrahyoid neck/visceral space and retropharyngeal space with relatively hyperdense foci causing narrowing and deviation of the aerodigestive tract to the left at the infrahyoid level to the supraglottic region (Figure 3). Contrast-enhanced CT scan of the neck done prior to surgery (A) coronal view and (B) axial view.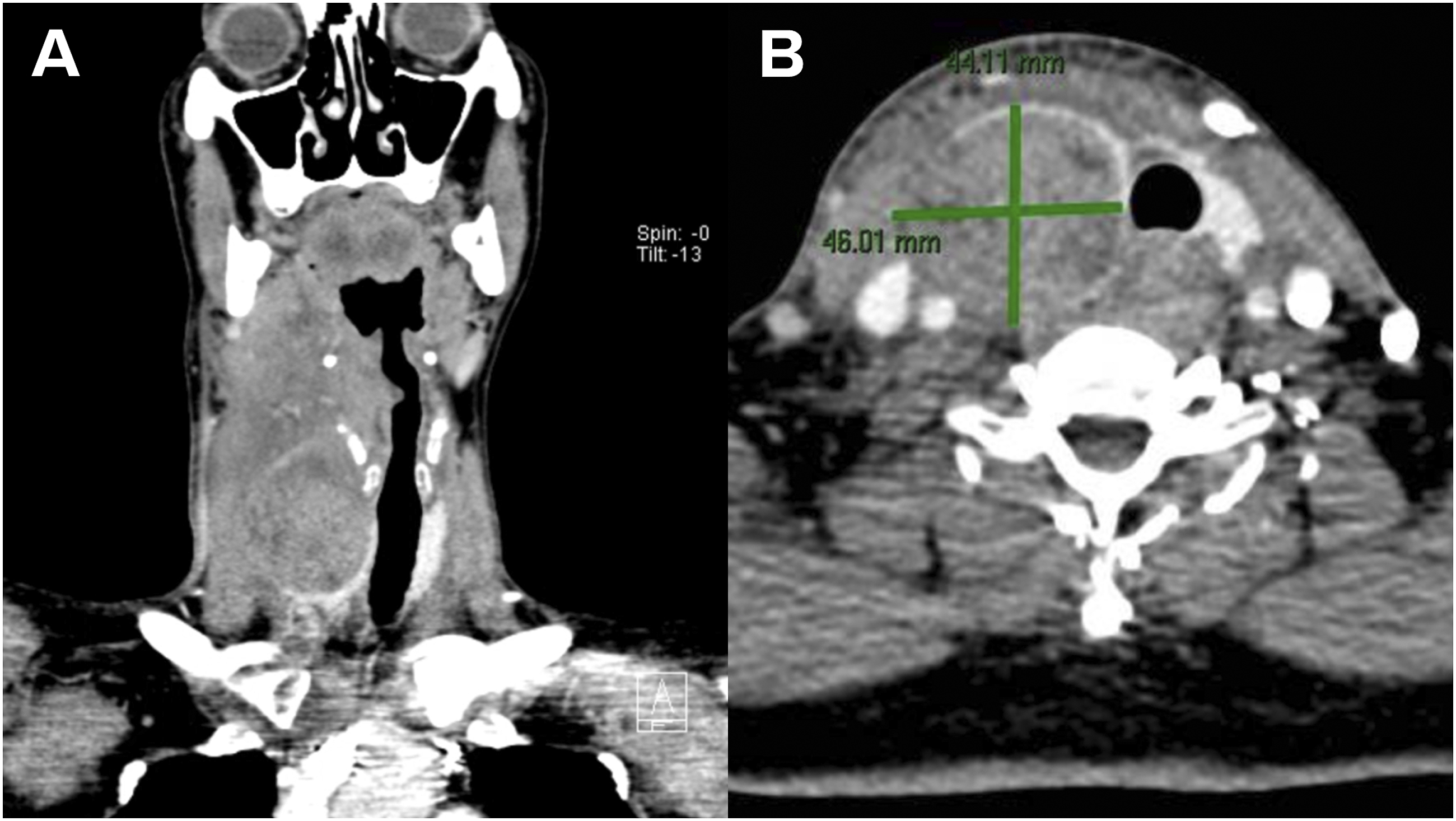
Patient was euthyroid on initial presentation: FT4 1.00 pg/mL (reference range, 0.70–1.48 ng/dL), FT3 2.49 pg/mL (reference range, 1.71–3.71 pg/mL), and TSH 0.5684 uIU/mL (reference range, 0.35–4.94 uIU/mL). WBC was 13.6 K/μL (normal: 4 to 11), with 85% segmenters.
Having confirmed the presence of expanding hematoma, the patient underwent neck exploration under general endotracheal anesthesia. Intraoperatively, the right thyroid lobe was noted to have an area of rupture approximately 1.5 cm in the superior aspect. Right thyroid arteries were ligated, and the recurrent laryngeal nerve (RLN) was identified and preserved (Figure 4). Right hemithyroidectomy was done. The hematoma was evacuated from the right parapharyngeal and retropharyngeal spaces. Intraoperative pictures showing (A) the area of rupture on the right thyroid lobe (dashed circle). (B) Photo after right hemithyroidectomy showing the right RLN identified and preserved.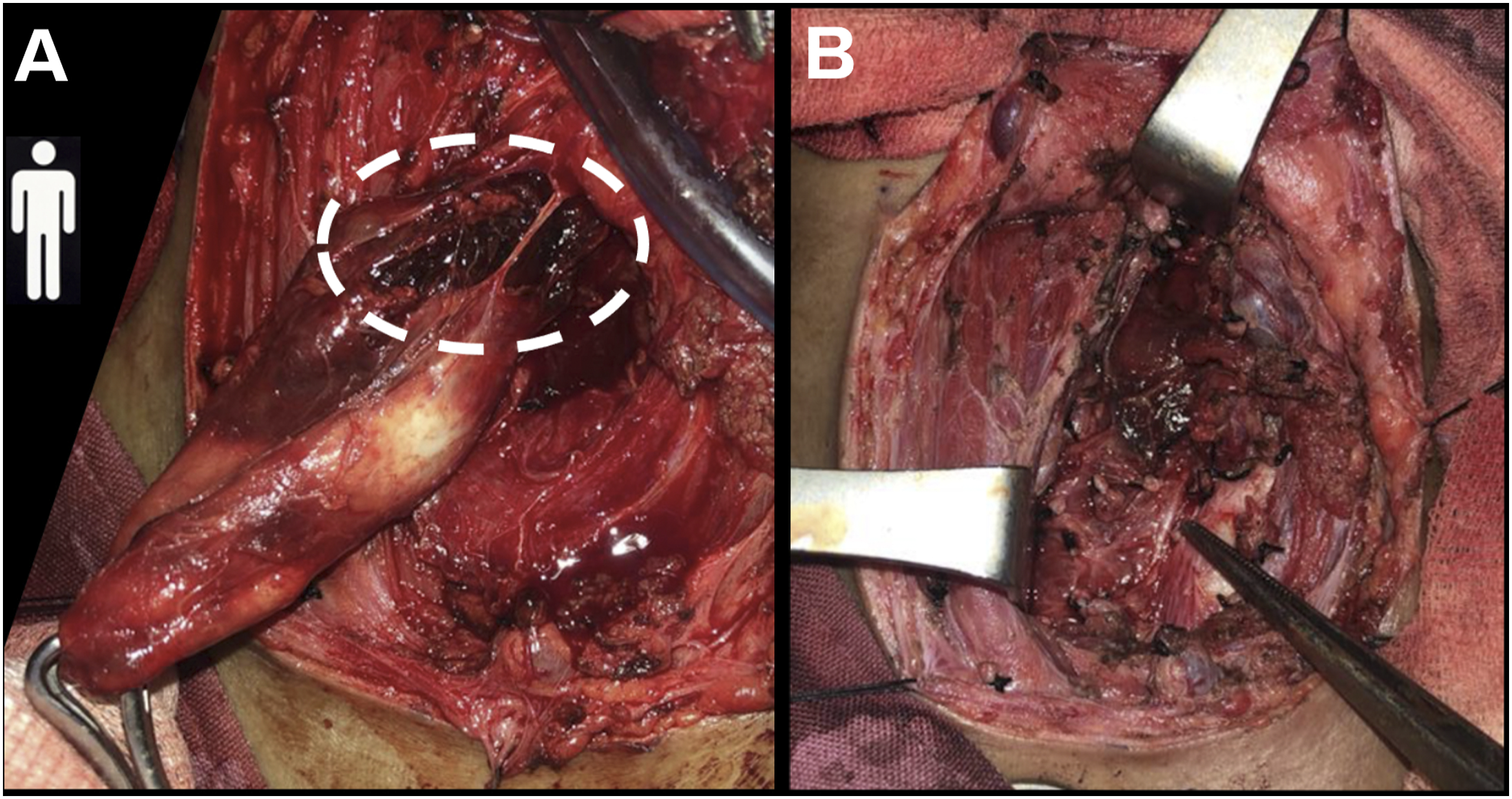
The patient tolerated the procedure well and was extubated immediately postoperatively without complications. A significant decrease in neck swelling was seen after evacuation of hematoma, and the patient’s odynophagia and hoarseness continued to improve. Drain and sutures were removed on the third and seventh day, respectively. Post-operative TSH was noted to be suppressed (.0821 uIU/mL) while FT3 and FT4 remained within normal range, signifying transient subclinical hyperthyroidism. The patient was discharged unremarkable on the seventh postoperative day.
Histopathology of the submitted specimen later revealed acute hemorrhage and congestion with reparative atypia of some foci of follicular cells. Thyroid hormones returned to normal levels on outpatient follow-up. The patient was seen a year later with normal phonation and a well-healed cervical scar (Figure 5). Post-operative evaluation. (A-B) Post-operative laryngoscopy and (C) noted resolution of neck swelling 1 day after the procedure. (D-E) Laryngoscopy and (F) well-healed neck scar 1 year after the procedure.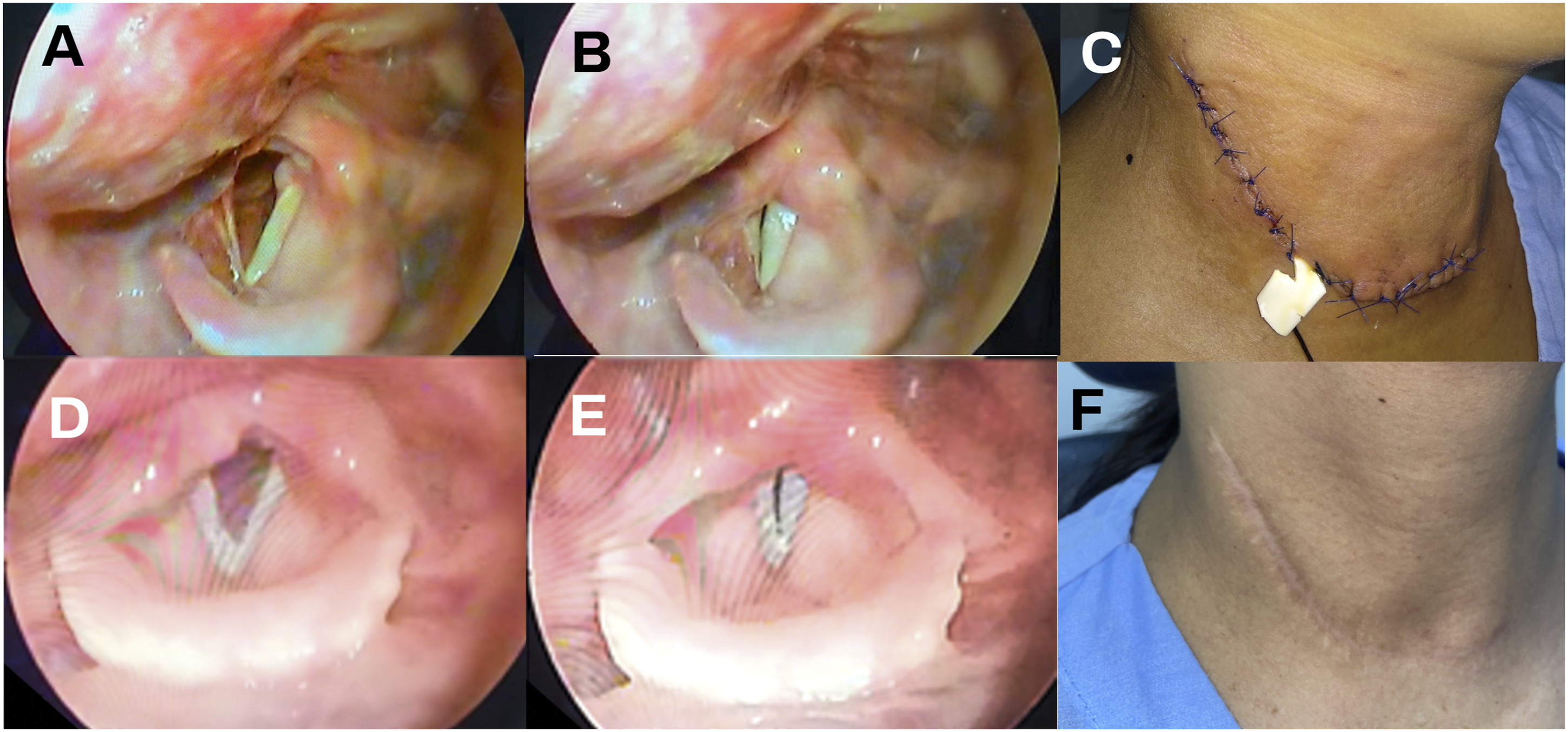
Discussion
The thyroid is the largest endocrine gland of the body and is richly supplied by blood with a normal flow rate of about 5 mg/mL/min, increasing 100-fold in disease states. 2 The thyroid gland is contained within the visceral space and the pharynx, esophagus, larynx, and trachea. Hemorrhage within this space can cause extrinsic compression of these adjacent structures explaining the most common presenting symptoms of neck swelling, dysphagia, dyspnea, and hoarseness. Neck pressure may tamponade the bleeding; however, uncontrolled hemorrhage may spread through communications to the submandibular, parapharyngeal, and retropharyngeal spaces showing the potential involvement of other deep neck spaces and even the mediastinum. 3
Our patient suffered from direct, blunt trauma to the neck, but other similar injuries noted were penetrating neck injuries, vehicular accidents, assaults, sports-related injuries, and fine-needle aspiration.1-5,7-23 Occurring less commonly are those arising from indirect mechanisms such as straining from heavy physical activities, Valsalva from coughing or defecating, and deceleration injuries.1,3,4 There have also been rare instances of spontaneous thyroid bleeding, but most were associated with preexisting thyroid pathology and chronic anticoagulation. 3 In a literature review done by Lemke et al 5 (2017), more cases were female (58%), the median age was 44 years, and about half of them had an established preexisting thyroid disease. The increased size, fragility, and vascularity of goitrous glands increase its risk for concomitant injury and bleeding, but rupture has likewise been reported in normal thyroid glands.
Following the Advanced Trauma Life Support (ATLS) protocol, the initial approach to any trauma prioritizes airway evaluation and management. Initial diagnostic airway evaluation via laryngoscopy may help document post-injury changes and endolaryngeal findings. 6 Even in the absence of hematoma, significant laryngeal edema may still occur in patients suffering from blunt neck trauma during the first 24 hours of injury. Respiratory distress may be immediate, but delayed presentations as late as 33 hours post-injury have been reported.1,7,8 Emergency airway management was needed in 24% of patients in the review by Lemke et al 5 and was determined on a case-to-case basis ranging from endotracheal intubation to tracheostomy.
Contrast-enhanced CT scan is the diagnostic method of choice for examination due to its ability to show the extent of hematoma, extravasation in the event of vascular injury, thyroid injury, and the upper aerodigestive tract assessment, making it useful for surgical planning.1,3,6,7 Other diagnostics that may be considered are ultrasonography and angiography. High-resolution ultrasound may be done as a fast and excellent method for first-line evaluation of suspected thyroid gland hematoma.1,3,7 CT Angiography may be indicated if significant vessel injuries are suspected.1,3
Although our patient did not present with overt hyperthyroid symptoms, there have been reported cases of life-threatening thyroid storm after blunt neck injury due to sudden thyroxine release in the blood stream from traumatic rupture of thyroid gland acini.3-5,9 Baseline thyroid hormone levels upon presentation and daily monitoring are recommended regardless if the patient is to be treated surgically or conservatively.9-12 In low resource settings where thyroid hormone assays may not be readily available, the main features for a thyroid storm must be included in clinical status monitoring and must be managed accordingly to avoid its potentially fatal sequelae: fever, tachycardia or supraventricular arrhythmias, central nervous system symptoms, and gastrointestinal symptoms.9,10
While approaches to diagnosis and management have been proposed, a consensus is yet to be made. Like Moore’s classification system for injury to parenchymatous organs like the liver and spleen, Heizmann and colleagues (2006) proposed a classification and treatment algorithm for blunt thyroid gland injuries based on radiological findings. Lemke and colleagues (2017) adapted the same grading system. They offered to include clinical monitoring for dyspnea and increasing hoarseness as part of an expanded management algorithm, as detailed in the succeeding paragraphs.
Conservative management with close monitoring and daily ultrasound follow-up is suggested among patients with Grade I–II lesions but with an otherwise normal thyroid gland, stable circulation, and airway. Patient observation in an intensive care unit should be no less than 24 hours to account for cases of delayed onset.1,7,8 For subjects seen a few hours after injury, some have attempted aspiration of the hematoma with success.2,13 Still, late diagnosis may fail aspiration once the blood starts to coagulate. 14 Other suggested monitoring and safety precautions include frequent clinical assessment of respiratory status, raising the head of bed 30–45° (reverse Trendelenburg position), and keeping an emergency tracheostomy set at the bedside.2,15 Some argue the utility of serial neck circumference measurements due to the compressive nature of soft tissue masses that may preclude early detection and prevention of airway compromise.2,8 Among the pediatric group (ages 8–15), only 1 had preexisting thyroid pathology 16 and none required surgical intervention12,15,16 making conservative management a reasonable option in children with thyroid hemorrhage without worsening symptoms.
Patients with Grades III and IV lesions, dyspnea, and increasing hoarseness require endotracheal intubation and neck exploration to evacuate the hematoma and control the bleeding. The review found that surgery was needed in up to 48% of cases. 5 Surgical management is likewise determined on a case-to-case basis. It may range from ligation of an artery to extensive neck exploration for hematoma evacuation, hemithyroidectomy, total thyroidectomy, and tracheostomy. However, most cases involve hemithyroidectomy. Whenever possible, total thyroidectomy is avoided to minimize the risk of bilateral recurrent laryngeal nerve palsy and postoperative hypoparathyroidism. 5 Aside from clinical presentation, another factor to consider is whether the patient has concomitant thyroid pathology (adenoma, cyst, multinodular goiter, and carcinoma) as resecting the diseased thyroid would remove the risk of continued, delayed bleeding from the fragile goitrous tissue and future operation or reoperation from nonresolution or persistent compressive symptoms.14,17,18
Conclusion
Although rare, thyroid gland rupture should be among the considerations for patients presenting with tender neck swelling, progressive hoarseness, or dyspnea following direct or indirect neck trauma. Prompt airway assessment and close monitoring for potential compromise are essential to avoid fatal sequelae of external airway compression. Management should be personalized depending on the severity of thyroid injury and symptomatology, watching out for progressive hoarseness and dyspnea.
Footnotes
Ethical Statement
Written informed consent was obtained from the patient to publish this case report and accompanying images. This case has undergone ethical review and was approved by Ospital ng Makati Research Ethics Board. This case has not been previously reported in part or whole in any publication. The case was presented virtually as a free paper in the 19th ASEAN ORL-HNS Congress held in Medan, Indonesia last October 21–23, 2021.
Acknowledgments
The authors would like to acknowledge Dr. H.M. Enriquez, our department chairman who provided general support, as well as Dr. A.V. Santos, Dr. J.B. Bombay, and Dr. C.J. Batan who were the surgeons of this case.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
