Abstract
Arrow injuries in Bhutan present a unique public health challenge, reflecting the cultural significance of archery in this Himalayan kingdom. Despite being a traditional sport and an integral part of Bhutanese identity, the growing incidence of arrow-related injuries raises concerns about safety and highlights the need for targeted preventive measures. In this case series, we present six cases of arrow injuries in the head and neck region offering insights into our experiences and the challenges encountered in their management. Additionally, cultural and regulatory aspects influencing archery practices and safety protocols are considered. The findings underscore the importance of community education, enhanced safety measures, and regulatory interventions to reduce the prevalence of arrow injuries while preserving the cultural heritage of archery in Bhutan. Addressing this issue necessitates a multidisciplinary approach that combines public health initiatives, cultural sensitivity, and policy interventions.
Introduction
Archery holds a revered status in Bhutan’s cultural tapestry, transcending mere sport to become a cherished national tradition. Rooted in the nation’s history, archery has been a ubiquitous feature of Bhutanese life for centuries. Evolving from a martial skill to a symbol of Bhutanese identity, archery became the official national sport in 1971, when Bhutan became a member of the United Nations. 1 Its significance extends beyond competitions, weaving through religious festivals and social gatherings, fostering camaraderie, and preserving Bhutanese heritage. Archery is a frequently enjoyed sport during Bhutanese festivals and as a recreational activity. Initially, traditional bow was the primary equipment used, but more recently, compound bow has also been introduced and embraced.
While advocating for the preservation of culture, it is equally imperative to note that unsafe archery practices in Bhutan have led to a concerning surge in arrow injuries. Neglect of safety protocols and inadequate awareness contribute to a rising incidence of accidents, resulting in severe head and neck injuries. 2
Injuries caused by arrows to the head and neck region pose a significant threat to life, with the potential for devastating consequences. Such injuries can lead to severe complications, including damage to major blood vessels, resulting in massive bleeding, expanding hematoma, or shock. Patients experiencing laryngeal or tracheal injuries may exhibit symptoms such as air-blowing wounds, expanding emphysema, or upper airway obstruction, necessitating urgent surgical intervention. 3
Managing arrow injuries in the head and neck region is exceptionally complex. The extraction of arrows proves challenging due to their proximity to vital structures. Unskilled removal may exacerbate existing injuries or cause inadvertent damage to crucial structures. This report aims to elucidate our experiences and challenges in handling penetrating arrow injuries to the head and neck region, while also taking into account cultural and regulatory factors that impact archery practices and safety protocols.
Case reports
Case 1
A 39-year-old male presented with an arrow injury to the nose causing severe epistaxis and associated symptoms of headache and mild pain with head movement. Despite the absence of loss of consciousness or limb weakness, immediate attention was required. Successful management involved posterior nasal packing to address the epistaxis, with stable vital signs throughout. The arrow’s trajectory, as revealed by computed tomography (CT), showed penetration into the nasal cavity, reaching the floor at the posterior end of the palatine bone and causing a minor fracture at the anterior arch of the Atlas. Consultation with an orthopedic spine surgeon determined no active interventions for the minor fracture. Thorough preparation for arrow removal included blood provision, consent for potential artery ligation, and nasal decongestion. Under general anesthesia, the arrow was carefully extracted under endoscopic guidance, with mild post-removal bleeding controlled by nasal packing. After 48 hours of observation, the patient was discharged, exhibiting good health, and recovery at the 1-month follow-up (Figure 1).

(a) Clinical image of the patient with an arrow injury to the nose. (b) Clinical image of the patient with an arrow injury to the nose at the operating table.
Case 2
A 36-year-old male presented with an arrow injury to the medial end of the right supraorbital region, resulting in a brief loss of consciousness and complaints of headache. Despite the absence of epistaxis, visual disturbances, nausea, or vomiting, and with a stable level of consciousness, CT revealed the arrow’s trajectory from the super medial part of the orbit, through the floor of the frontal sinus, and into the left ethmoidal sinus. Pneumocephalus was observed in the left frontal and parietal lobes along the falx. A multidisciplinary discussion involving Otolaryngology, Neurosurgery, and Ophthalmology departments determined the treatment plan. The arrow, lodged 6 cm deep, was removed under general anesthesia, accompanied by repair of a dural tear over the roof of the left ethmoid using adipose tissue, fascia lata, fibrin glue, and gel foam. The patient received intravenous antibiotics for 2 weeks, experiencing an uneventful recovery and discharge after 2 weeks. Follow-up at 1 month revealed parosmia but no cerebrospinal fluid leakage, resolving completely at the 3-month mark (Figure 2).

(a) Image of a patient with arrow lodged at right supraorbital region. (b) Image of a patient with arrow lodged at right supraorbital region at the operating table. (c) X-ray skull lateral view of a patient with arrow tip lodged at right supraorbital region. (d) Image of a patient with subsequent removal of the arrow lodged at right supraorbital region.
Case 3
A 40-year-old male sustained an arrow injury to the anterior neck which he removed himself. He was airlifted, and upon arrival at the emergency room, he complained of neck pain, odynophagia, and mild shortness of breath. There was a 1 cm wide puncture wound just above the suprasternal area with no active bleeding. Fiber-optic laryngoscopy revealed mobile bilateral vocal cords, and CT showed the arrow had traversed the lower part of the thyroid cartilage, entering the subglottis and hypopharynx. Awake tracheostomy was performed due to anticipated intubation challenges, followed by the removal of meticulous dissection of tissue around 4.5 cm deep to trace the path of the arrow under general anesthesia and thorough wound debridement. The patient recovered well, experiencing surgical emphysema which was managed conservatively. Discharged on postoperative day 10, he resumed normal activities without complications (Figure 3).
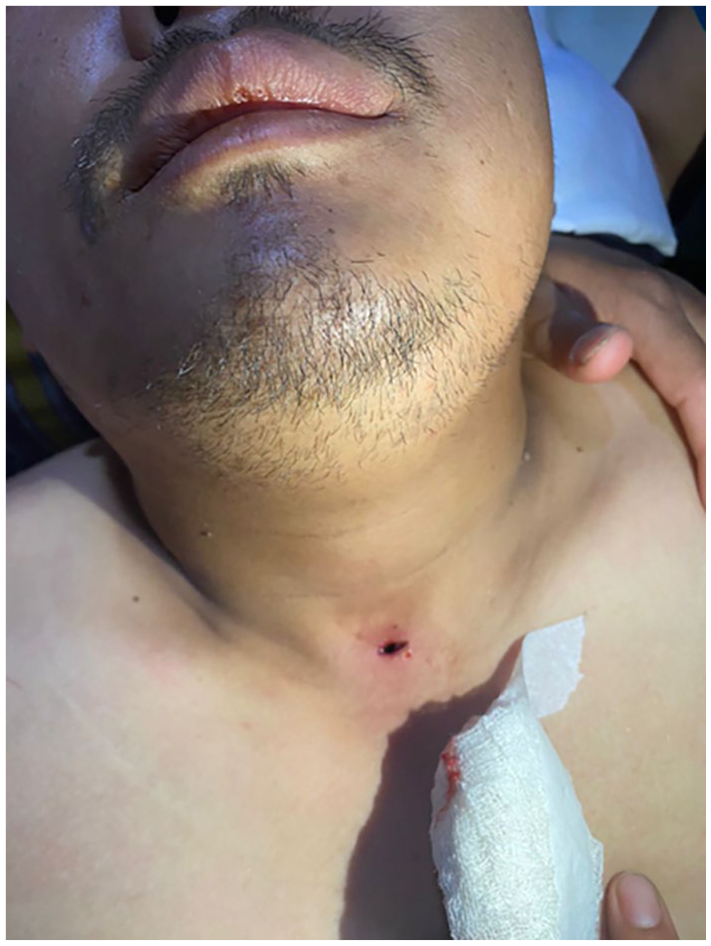
Anterior neck puncture wound of the patient following self-removal of the arrow.
Case 4
A 42-year-old man presented with an arrow injury to the left side of the face during an archery match. Experiencing a dull, heavy headache and a brief blackout episode, he had no ENT bleeding, neurological deficit, nausea, vomiting, or seizures. CT revealed the arrow’s path from the left maxillary sinus to the base of occiput. Multidisciplinary consultations yielded no active interventions. A 10 cm deep arrow was removed through small incisions, with no active bleeding observed. The patient received antibiotics and was discharged. One month post-operation, he was doing well with minimal scarring on the face (Figure 4).

(a) Clinical image of a patient with left facial arrow injury. (b) Clinical image of a patient with left facial arrow injury at the operating table. (c) The arrow removed from the left side of the patient’s face.
Case 5
A 35-year-old man experienced a compound arrow injury during a friendly archery match, with the arrow piercing the left side of his face. Despite the severity, he remained clinically stable, showing no significant bleeding, and retained full alertness. He was swiftly transported to the nearest hospital and then airlifted to Jigme Dorji Wangchuk National Referral Hospital. A CT scan revealed a complex trajectory: the arrow entered through the anterior aspect of the left infratemporal fossa, causing a comminuted blow-in fracture in the left orbit, traversed the maxillary antrum, penetrated the posterior ethmoid sinuses, crossed the midline through the fractured posterior wall of the right maxillary antrum, pierced the right pterygoid bone, and lodged in the right infratemporal fossa. Fragments from the left orbital fracture were observed affecting the left lateral rectus muscle. In the operating room, under general anesthesia, the arrow was successfully removed, and the entrapped lateral rectus muscle was released without significant bleeding. The patient, observed for 3 days, was discharged, and follow-up visits indicated a satisfactory recovery and overall well-being (Figure 5).

(a) CT image of Case 5 showing the arrow. (b) CT image of Case 5 showing the arrow trajectory marked by a white line.
Case 6
During a friendly archery match, a 46-year-old archery player sustained an arrow injury at the posterior neck. All players were using traditional bows. Fortunately, the victim remained stable with no loss of consciousness or bleeding. A CT scan revealed that the arrow had penetrated the right trapezius muscle and splenius capitis muscles, and the tip was located lateral to the lateral processes of C2 and C3 vertebrae, and medial to the internal carotid artery. Under general anesthesia, the entry site was widened, and meticulous tissue dissection was performed to safely remove the arrow. There was no significant bleeding, and the patient is reported to be doing well after a period of 2 weeks (Figure 6).

Clinical image of the patient with arrow lodged at posterior part of neck.
Discussion
Arrow injuries, though uncommon, pose unique challenges in both diagnosis and management due to the delicate anatomy and vital structures in these regions. One of the primary challenges encountered is the potential for severe, life-threatening injuries, including damage to major blood vessels, the airway, and the brain or spinal cord. In some instances, unreported cases have resulted in fatalities on the spot, underscoring the severity of such injuries. However, our recent experiences with arrow injuries, as discussed above, have demonstrated favorable outcomes, with all patients maintaining stability during their course of treatment.
The majority of reported arrow cases from other countries stem from incidents involving assault, hunting, or self-inflicted injuries as a result of suicidal attempts.4–7 Our case series marks the first reported series of arrow injuries occurring as part of sporting or recreational activities.
Archery, an integral part of Bhutanese culture, is not only featured in numerous festivals and occasions but also embraced as a recreational activity.1,2 However, there exists an open secret regarding the consumption of alcohol during these matches, coupled with a lack of proper safety precautions. While there is supposed to be a concrete wall near the target to provide protection for nearby players, there is a widespread habit of individuals peering over it to witness the trajectory of incoming arrows. Additionally, there are novice players who participate for enjoyment, sometimes struggling to control the arrows, leading to deviations in trajectory and resulting in injuries. 2
The challenges in treating penetrating injuries to the head and neck, such as potential damage to vital structures, demand a meticulous approach. 8 Immediate assessment and stabilization are crucial to prevent further harm and ensure the patient’s survival. Additionally, the extraction of the arrow must be approached with extreme caution to avoid exacerbating tissue damage or causing hemorrhage. There have been instances where attempting self-arrow removal has led to bleeding or, in some cases, even death. 3 It is crucial to resist the temptation to remove the arrow oneself. Imaging, particularly CT, plays a pivotal role in assessing the extent and trajectory of the arrow, aiding in meticulous surgical planning.3,8
In our case series reported above, almost all individuals were brought to the hospital with arrows still intact. Following a thorough evaluation and planning process involving a multidisciplinary team, the arrows were successfully removed. Our cases highlight the significance of careful planning, collaboration between specialties, and readiness for unforeseen complications.
Bhutan’s referral system has been crucial in ensuring that patients receive timely and appropriate care. Multidisciplinary discussions between departments such as ENT, Neurosurgery, and Ophthalmology are essential for comprehensive management strategies. The successful airlifting of patients from remote areas to specialized medical facilities further emphasizes the importance of efficient emergency services and transport infrastructure.
Valuable lessons learned from handling these cases emphasize the importance of rapid and coordinated emergency response, including on-site medical teams trained in trauma management. Early recognition of the severity of the injury and prompt initiation of appropriate interventions, such as airway management and hemorrhage control, are critical for optimizing outcomes. Furthermore, comprehensive imaging studies, such as CT scans, are essential for assessing the extent of internal damage and guiding surgical intervention if necessary. Collaborative efforts between trauma surgeons, neurosurgeons, otolaryngologists, and other specialists are vital for providing comprehensive care and addressing the complex nature of these injuries.
Moreover, the psychological impact on both patients and healthcare providers cannot be overlooked. Arrow injuries to the head and neck can result in long-term physical disabilities and emotional trauma. Therefore, holistic support services, including psychological counseling and rehabilitation programs, are essential components of the management process.
While arrow injuries remain rare, these cases underscore the need for ongoing research, standardized protocols, and enhanced awareness to optimize outcomes for patients facing such unique and challenging incidents. To address the prevalent issue of arrow-related injuries in Bhutan, particularly stemming from unsafe practices during archery events, several preventive measures can be proposed. Firstly, implementing strict regulations mandating designated spectator areas, separated from the shooting range, could significantly mitigate the risk of injuries caused by individuals peeping for incoming arrows. These areas should be clearly demarcated and enforced by trained personnel to ensure compliance. Secondly, organizing educational campaigns and workshops within communities to raise awareness about the dangers of irresponsible behavior during archery events, especially under the influence of alcohol, can foster a culture of safety and responsibility.
Conclusion
In the unique realm of Bhutanese archery, this case series sheds light on the perilous landscape marked by an unsafe environment during archery matches, subsequently leading to a surge in associated arrow injuries targeting the head and neck region. The study meticulously examines instances where the traditional sport transforms into a potential hazard due to inadequate safety measures and lapses in regulatory practices. Through a comprehensive analysis of documented cases, this series aims to identify the patterns, contributing factors, and consequences of arrow-related injuries. Beyond highlighting the immediate physical implications, the research delves into the broader implications for both archers and spectators within the Bhutanese archery culture. The findings not only underscore the urgency for enhanced safety protocols but also advocate for a heightened awareness of the inherent risks, fostering a safer environment for participants and enthusiasts alike in the pursuit of this revered national sport.
Footnotes
Acknowledgements
We want to convey our heartfelt gratitude to the dedicated staff of the local hospital, Emergency Room, Operating Theater, Otolaryngology/Head Neck Surgery, and Maxillofacial Surgery departments, for their unwavering commitment and exceptional expertise in managing the cases.
Author contributions
UP contributed to concept and design of case report, literature review, and final manuscript writing. SJ contributed to concept and design of case report, literature review and supervised the final version of the manuscript writing to be published.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
The authors certify that written informed consent was obtained from the patient(s) for their anonymized information to be published in this article. In the form, the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity.
