Abstract
Study Design
Technical Note
Objective
Pharyngoesophageal injury in the setting of previous anterior cervical discectomy and fusion (ACDF) is a devastating complication with no standard corrective treatment protocol. Reconstruction can thus be a complex endeavour often leading to treatment failure, recurrent pharyngoesophageal fistula and need for multiple surgical procedures. The authors present our novel approach to free tissue reconstruction of these injuries.
Methods
We utilized a bulk adipofascial flap to completely obliterate the retropharyngeal space and correct the pharyngoesophageal defect.
Results
An adipofascial flap facilitates complete separation of the injured pharyngeal/oesophageal mucosa form the cervical spine and any retained hardware.
Conclusions
In our hands, this technique has allowed successful repair of complex pharyngoesophageal injuries after previous ACDF procedures which includes resumption of normal oral intake.
Keywords
Technique
Anterior cervical discectomy and fusion (ACDF) is an increasingly common approach for the management of cervical spinal pathology. Although rare, pharyngoesophageal injury is the most feared risk of ACDF procedures and often poses a unique reconstructive challenge.1,2 While a defined treatment algorithm is lacking, primary closure buttressed by locoregional myofascial flap, coupled with removal of contaminated hardware (when present) is advocated for defect repair with reasonable success rates.1,3,4 However, in patients with previous reconstructive failure or particularly complex delayed injury (occasionally occurring many years after original ACDF procedure) free tissue reconstruction may be required to ensure treatment success.
We present our bulk adipofascial flap technique for free tissue reconstruction of pharyngoesophageal injuries after ACDF, which acts both to repair the defect and obliterate the retropharyngeal dead space isolating the pharynx from the cervical spine. A representative case is a 50-year-old female with a past history of anterior cervical diskectomy and fusion of C3–C7. While initially doing well, roughly 10 months after her ACDF she began to develop progressive dysphagia, odynophagia and hoarseness. At this time, a deep neck space infection associated with a pharyngeal tear at the hardware site was identified. Initial management included hardware removal and a combined primary defect repair, buttressed with a sternocleidomastoid muscle rotational flap. This original reconstruction failed with development of a recurrent pharyngocutaneous fistula that was managed three months after the initial reconstruction with a right pectoralis major myofascial flap. However, she again developed a recurrent wound to the right supraclavicular fossa with high output salivary drainage (Figure 1). Interestingly, endoscopy failed to identify an obvious site of intraluminal injury, but the wound failed to heal despite enteral nutrition and NPO status. Preoperative image of chronic fistula with ribbon gauze packing to aid dissection. Note, the fistula site is distinct from the previous ACDF scar, with a poorly vascularized intervening skin bridge that required resection/debridement.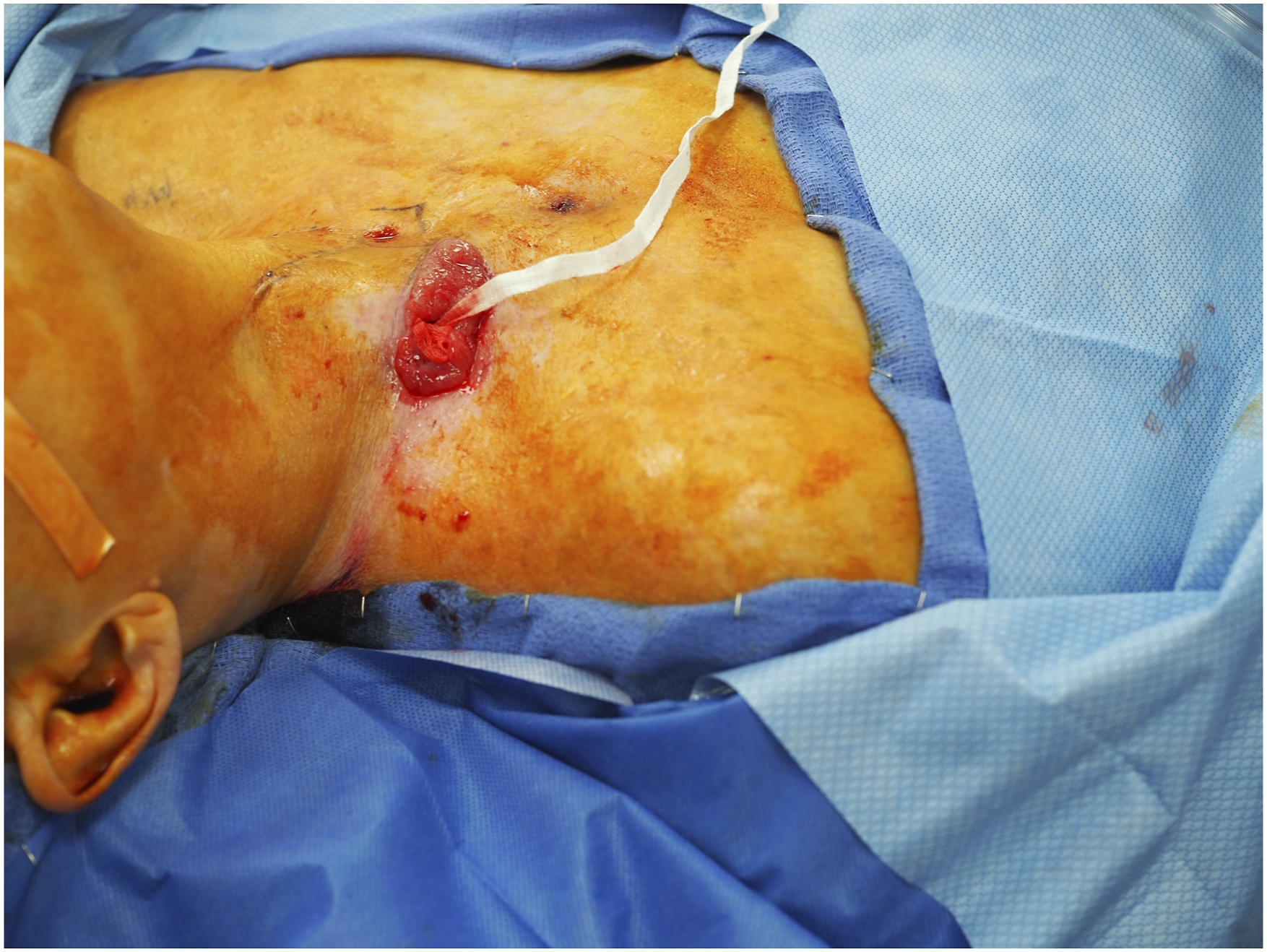
She was now referred to our clinic for definitive management. The first aspect of the surgical approach required complete resection of the fistula with exposure of the retropharyngeal space. In our hands this is addressed similarly to a brachial anomaly. The patient’s previous neck incision is opened, and the cutaneous aspect of the cyst is incorporated into the resection specimen. In this case, there was exuberant scar formation, but the tract was able to be carefully dissected free from the carotid sheath and strap musculature allowing it to be isolated to the retroesophageal space (Figure 2A). At this point, the tract is opened and an oesophagoscope placed transorally to help identify an area of injury/defect if present. While an obvious mucosal injury was not present, there was extensive mucosalization of the retropharyngeal space which is completely resected and debrided to healthy tissue at the time of fistula resection. This now creates a sizable pocket between the pharyngoesophageal wall and underlying spine (Figure 2B). An anterolateral thigh free tissue transplant was than harvested on a single perforator. In this case previous scar placement and infection had caused a significant skin defect and thus a skin paddle was maintained. We than created a generous adipofascial flap which would be used to fill the entire retroesophageal space completely isolating the spine from the oesophagus (Figure 3A). This is inset carefully with multiple tacking sutures to the oesophageal lining. Inset of these flaps is often challenging given poor tissue quality. This is aided by flap bulk which can obliterate the entire dead space despite relatively minimal anchoring. With the inset complete the flap is than vascularized and all sites closed. (a) Dissection of the fistula tract off the carotid sheath now isolated along the tracheoesophageal groove region. (b) Completed fistula resection with retractor showing sizable retropharyngeal pocket between the oesophagus and cervical spine. (a) Flap design with large adipofascial component to obliterate the retropharyngeal space. Note the sizable and bulky cutaneous segment in this particular case given the need for extensive resection. (b) Final healed appearance 3 months postoperatively without evidence of recurring fistula despite resumption of oral intake. Patient currently in process of aesthetic debulking and recontouring.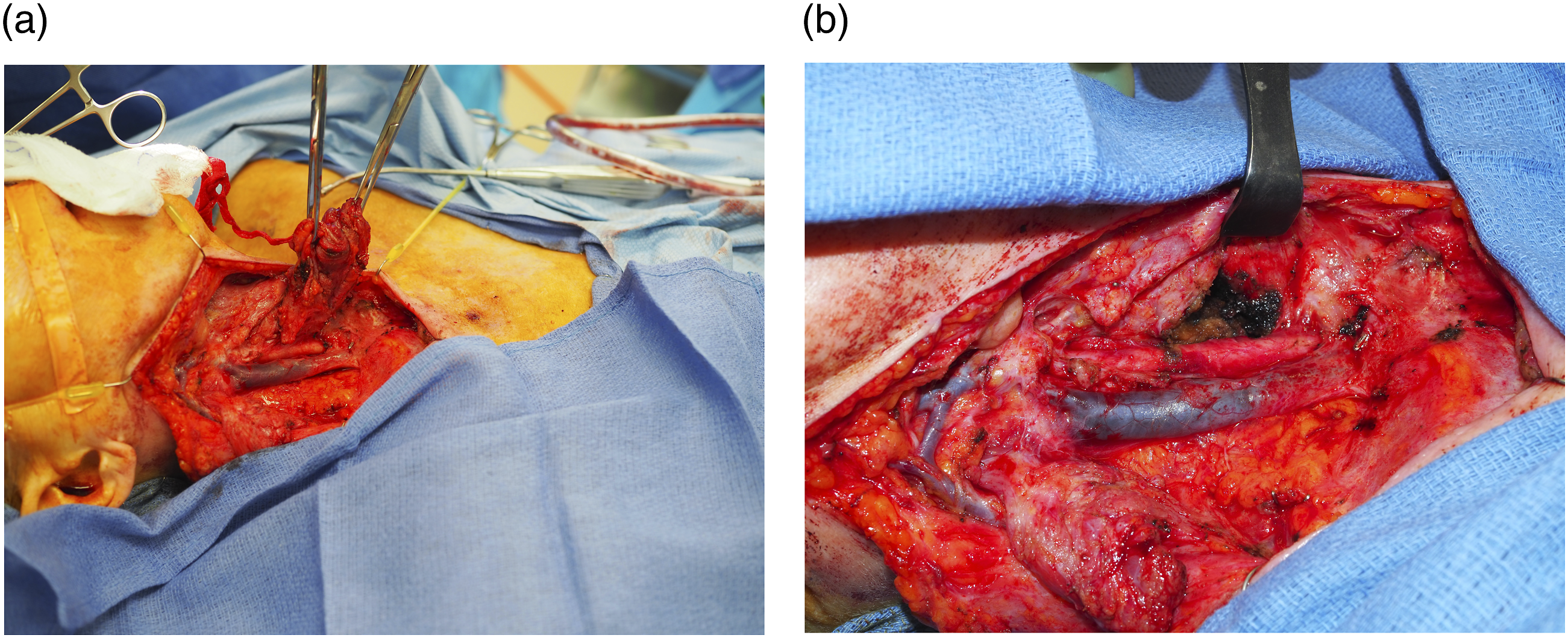
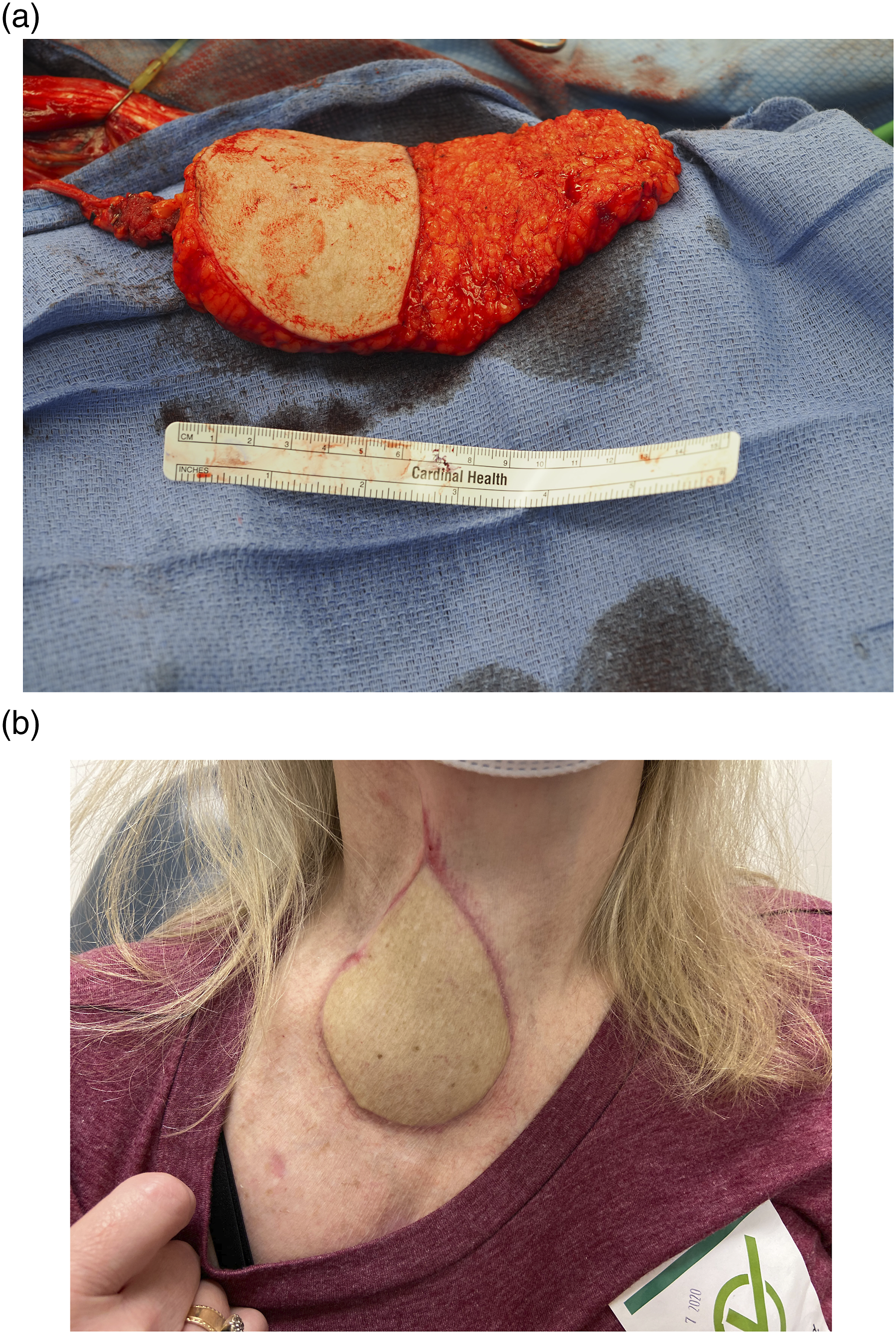
The hallmarks of recovery from pharyngoesophageal injury are resumption of normal oral intake, resolution of infection, and a stable cervical spine. Our patient remained NPO for two months initially resuming liquid diet with full return to oral intake three months after her procedure. She has not suffered any further infectious complications and her cervical spine stability has been successfully maintained. She is currently > 1-year post-surgery and undergoing aesthetic debulking of the cutaneous skin paddle to improve cosmesis (Figure 3B).
Discussion
Although not a common complication of ACDF, pharyngoesophageal injuries can be devastating and have a lasting impact on quality of life. Delayed injuries, often occurring years after the initial ACDF surgery, can be particularly challenging. The pathophysiologic mechanism for these is likely repetitive tissue microtrauma, leading to extensive inflammation, chronic tissue damage, and bacterial colonization of the involved hardware. Treating these delayed injuries are thus more likely to require complex management with hardware removal, defect closure and at minimum reinforcement with a vascularized flap to promote healing.1,2 Vascularized tissue assists antibiotic delivery, obliterates dead space, and facilitates a water-tight pharyngoesophageal closure – particularly in the setting of a hostile wound. 2 A variety of regional muscle flaps are available to serve this purpose, with the sternocleidomastoid rotational flap most commonly described in the available literature. 4 Regional flaps such as pectoralis major muscle flaps may also have a role in cases of recurring fistula, however, are often bulky and difficult to lay down toward the inferior aspect of the wound site as they must be brought over the clavicle. 4
In comparison to local or regional flaps, free flaps are far more customizable to fit various complex defects. This is essential in the setting of pharyngeal injuries after ACDF given the large dead space created by previous dissection as well as the active fistula/infection which must be completely obliterated to prevent disease recurrence. There is limited literature to guide microvascular free flap selection in such cases; however, use of both omental and anterolateral thigh flaps have been demonstrated in case studies.2,5 Omental tissue is known to have both angiogenic and immunogenic properties, making it a good choice in contaminated wound beds. Another potential benefit of omentum is the fact that it is thin and readily pliable.2,5-7 However, omental flaps suffer from increased complexity and potential donor site morbidity, given the need for intra-abdominal harvest. In our practice, we have thus preferred adipofascial free flaps for most cases of pharyngeal reconstruction.
Adipofascial flap are advantageous in our opinion given their inherent flexibility. They can be fashioned into any template and even aggressively thinned as necessary providing the ability to not only fill the retropharyngeal dead space but also prevent excess mass effect on the pharyngoesophageal complex, supporting resumption of normal swallowing.2,8 Selection of an appropriate adipofascial flap must be individualized taken into account features such as a patient’s body habitus, previous surgical scars, and surgeon preference. In our hands the ALT is generally preferred for all but obese patients, given customizability (including ability to add a vastus lateralis muscle pedicle if required), relative skin pliability, ease of harvest (including ability for two team surgery) and relatively minor donor site morbidity without need for skin grafting.
In our practice, free tissue reconstruction has become the go to for cases of recurrent pharyngeal injury – particularly in the “delayed” setting. Including the representative patient, we have utilized this technique in a total of four patients to date. All four patients were suffering from recurrent pharyngeal injury/neck fistula (after precious ACDF), who had failed previous reconstructive operation. Two patients were males and the other two females, with a mean age of 57 (50–65 years old) at the time of surgery. An ALT flap was utilized in three cases with a radial forearm free flap selected for the fourth because of the patient’s body habitus. We utilized the facial artery as the recipient arterial vessel in all four cases, but the venous vessel varied, including the external jugular venous branch, facial vein, and venae comitantes of the hypoglossal nerve.
In all patients to date, the free tissue reconstructive procedure was the final open operation used to address the pharyngeal injury. We have, however, performed diagnostic esophagoscopy in three of the four patients due to abnormalities on postoperative esophagram. In cases 1 & 2 (including the representative case), esophagoscopy was normal facilitating resumption of oral intake. In case 3 (reconstructed with a radial forearm flap), a small diverticulum was noted along the suture line scarred to the prevertebral fascia. This however did not prevent resumption of normal oral intake and thus an observational approach was undertaken. The fourth patient is our most recent case, she has had inconsistent follow up and to date has only partial resumed oral intake, continuing to require a G-tube four months post op.
The obvious disadvantages of microvascular free tissue transfer when compared to regional pedicled flaps are increased complexity and operative time with some risk of microvascular thrombosis which can lead to flap loss. 4 However, in cases of delayed injury or previous treatment failure, this must be weighed against the relative unreliability of regional pedicled muscle flaps that can be associated with recurring infection/fistula and need for prolonged enteral nutrition with additional surgical salvage. 9 As a consequence, an adipofascial free tissue reconstruction should strongly be considered in these complex cases, and has become our favoured reconstruction in this setting.
Conclusion
We have presented our approach for the application of a bulk adipofascial flap free tissue flap for pharyngoesophageal reconstruction. This technique is a promising and reliable reconstruction option for the management of pharyngoesophageal injuries in the setting of anterior cervical hardware failure.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient Consent
Written informed consent for patient information and images to be published was provided by the patients or a legally authorized representative.
