Abstract
Fusarium species, a soil-borne fungi, causes disease in animals and humans, particularly in immunocompromized patients. A 62-year-old male presented with type II diabetes mellitus, diagnosed 4 years ago. He had a motorcycle accident-caused open tibiofibular fracture of the left lower extremity (Gustilo grade IIIb). With open reduction and internal fixation, an anterolateral thigh musculocutaneous flap was harvested for coverage of exposed bone and defect reconstruction. Partial failure of the flap occurred 9 days following reconstruction, and histological examination revealed Fusarium spp. After treatment with antifungal drugs and debridement, we performed a split-thickness skin graft. At 2-year follow-up, the flap was viable with adequate bone union. This is the first reported case of partial flap failure due to a Fusarium spp. infection. Possibility of fungal infections in patients with late-onset flap failure should be noted. Prompt diagnosis and treatment are needed to prevent repeated free-tissue transfer and/or devastating outcomes.
Introduction
Fusarium species, a soil-borne fungi and plant pathogen, can cause diseases in animals and humans, ranging from a localized infection of a target organ to disseminated infections.1–6 In particular, immunocompromized patients are at elevated risk.1–3
Case
This report is about a 62-year-old male with uncontrolled type II diabetes mellitus diagnosed 4 years ago and an open tibiofibular fracture of the left lower extremity caused by a traumatic motorcycle accident (Gustilo grade IIIb) (Figure 1(a) and (b)). After open reduction and internal fixation, an anterolateral thigh (ALT) myocutaneous flap was harvested to cover the exposed bone and for defect reconstruction (Figure 1(c) and (d)). Recipient vessels were the anterior tibial artery and its concomitant veins. Postoperatively, his pre-meal blood sugar levels were 150–170 mg/dL with oral anti-diabetic medications.
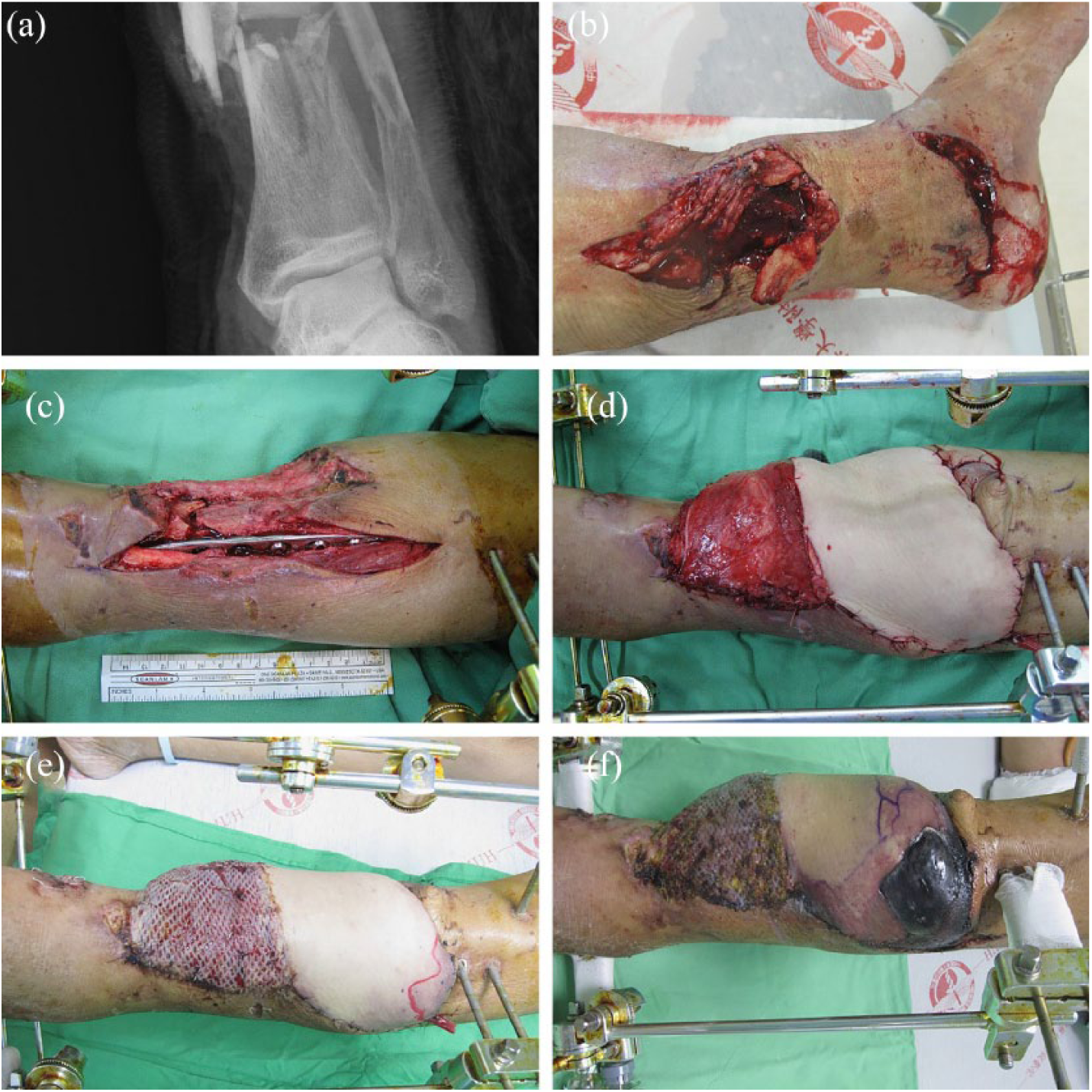
(a) Left tibiofibular shaft open fracture (Gustilo grade IIIb). (b) Left lower leg open fracture contaminated by roadside soil. (c) The orthopedic surgeon performed open reduction and internal fixation of the tibiofibular fracture. (d) We performed an ALT musculocutaneous flap, harvested from the ipsilateral leg, for defect reconstruction. Recipient vessels were the anterior tibial artery and its concomitant veins. (e) The patient’s postoperative course was uneventful. However, the proximal part of the flap started to show mild bluish changes 9 days following reconstruction. (f) The size of the affected area gradually increased day by day, and dry gangrenous changes ultimately developed over the proximal one-third of the by 35 days following reconstruction.
The proximal part of the flap began showing a mild bluish change 9 days following reconstruction (Figure 1(e)). Capillary refill and the pinprick test on the bluish area were brisk and produced dark blood. The size of the affected area gradually increased, and dry gangrenous changes ultimately developed over the proximal one-third of the flap 35 days following reconstruction (Figure 1(f)). We performed a wound culture that revealed no bacterial growth.
An infectious disease specialist used standard mycological procedures and grew Fusarium species from two separate cultures at different intervals (Figure 2(a) and (b)). A light microscope examination with lactophenol cotton blue stain revealing septated and acute branching hyphae with microconidia spores (Figure 2(c) and (d)).

(a) Orange cottony colonies grew on the Sabouraud dextrose agar. (b) White-cottony colonies grew on the brain heart infusion agar. (c) Cover slide under a light microscope showed septated hyphae with acute branching (lactophenol cotton blue stain, ×1000). (d) Cone-shaped microconidia, the characteristic of Fusarium (lactophenol cotton blue stain, ×1000). (e) Debridement of the gangrenous flap was performed on 35 days following reconstruction. (f) The periodic acid Schiff stain demonstrates septated, acute angled fungal hyphae, and spores in the tissues from the left lower leg (×1000).
There were no other Fusarium infection-related symptoms; the patient was afebrile and without any regional lymphadenopathy. A complete blood count revealed mild leukocytosis (10.5 × 103/µL). Chest X-ray, fungal blood cultures and serologic tests were all negative, and tissue examination was recommended to eliminate fungus culture contamination.
Debridement of gangrenous flap (Figure 2(e)) was performed at 35 days following reconstruction. Specimen pathology revealed a deep fungal infection with clustered fungal spores and septated, acute angled hyphae with extensive necrosis of adjacent tissues (Figure 2(f)).
The patient immediately began amphotericin B, 75 mg intravenously per day. Twelve days later, we shifted to liposomal amphotericin B to 200 mg due to elevated serum creatinine levels (from 1.07 to 3.17 mg/dL). After the 7 day course of liposomal amphotericin B, voriconazole was prescribed. The patient took 200 mg orally every 12 h for the first two doses and then 100 mg orally every 12 h for 19 days. After 15-day treatment, repeat fungus cultures were negative.
A second debridement was performed 51 days following reconstruction, and the subcutaneous fat layer was still viable. We arranged for a split-thickness skin graft from the ipsilateral leg, and at 2-year follow-up, the flap was viable with adequate bone union (Figure 3).

At 2-year follow-up, the flap was viable with adequate bone union.
Written informed consent was obtained from the patients for their anonymized information to be published in this article. Our institution does not require ethical approval for reporting individual cases or case series.
Discussion
Free flap fungal infections appear particularly rare. Lai et al. 7 reported a case of a patient with a diabetic foot ulcer and Aspergillus flavus infection after reconstruction of a free muscle flap with a skin graft. Mahajan et al. 8 also reported a case of free gracilis muscle flap with an overlying skin graft due to an Aspergillus fumigatus infection in an immunocompetent 23-year-old female with a severe automobile-related right leg crush injury (Gustilo grade IIIc). Fusarium infection-induced flap partial failure has not been reported thus far.
Fusarium species cause superficial to disseminated infections in humans. The clinical manifestations relate to host immune status and the portal of infection entry. The main risk factors are cutaneous tissue breakdown and presence of foreign bodies, as with our case. 3 Additional risk factors are profound neutropenia and/or severe T-cell immunodeficiency. 4 Although aspergillosis remains the most common infection in patients with hematologic cancers (aspergillosis to fusariosis, 90% to 4%), the mortality rate of fusariosis can be as high as 53% (aspergillosis: 42%). 9 Keratitis and onychomycosis are the most common Fusarium infections. Marcio et al. described other infections, including peritonitis, that were associated with continuous ambulatory peritoneal dialysis, sinusitis, pneumonia, thrombophlebitis, fungemia with or without organ involvement, endophthalmitis, septic arthritis, and osteomyelitis. Although our case’s infection was localized, disseminated infections present as prolonged and profound neutropenia, with persistent fever and disseminated and characteristic skin lesions. 6
Definite diagnosis for infection with Fusarium spp. requires histopathology. Although the hyaline and septate hyphae with acute and right angled branches are similar to those of Aspergillus species, adventitious sporulation and the finding of hyphae and yeast-like structures can be helpful for diagnosis. Cultures and biopsies on different sites and at different intervals are recommended. 6
The slow and progressive flap change suggested the formation of microemboli and regional vessel occlusion, consistent with Fusarium spp. Fusarium infections are characterized by endovascular invasion and thromboses, 10 particularly in immunocompromized patients. 3 There are cases of Fusarium-caused ophthalmitis that cause infarction and necrosis of ocular tissue (as demonstrated by histopathological examination)11,12 and thrombophlebitis. 13
Although our case’s Fusarium infection was localized, we did not use topical antifungal agents because of the vascular invasion and microemboli formation that characterizes these infections. Antifungal susceptibility must be considered before initiating any therapy because Fusarium species are resistant to many antifungal agents in vitro. Amphotericin B and its lipid complex have been successfully used to treat these patients. Voriconazole and posaconazole could be used with patients intolerant or refractory to primary therapy.14–16 In addition, debridement of the entire gangrenous area was necessary.
Conclusion
To the best of our knowledge, this is the first documented case of Fusarium infection that induced partial failure of a free ALT musculocutaneous flap in a patient with diabetes status-post traumatic injury. We are hopeful that this case serves to remind of the possibility of fungal infections accompanying late-onset flap failure.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
