Abstract
Study Design
Case report
Objective
Syndromic multi-suture craniosynostosis can result in complex dysmorphology and increased intracranial pressure. We present a case report of a child with craniometaphyseal dysplasia and syndromic multi-suture craniosynostosis who presented with increased intracranial pressure, ventriculomegaly and Chiari deformity Type 1.
Methods
The child underwent a posterior vault distraction to increase the intracranial volume.
Results
The posterior cranial expansion was successful in correcting the craniocerebral disproportion caused by multi-suture synostosis, and resolved the high intracranial pressure and papilloedema. There were no post-operative complications.
Conclusions
Posterior cranial vault distraction was an effective method of addressing increased intracranial pressure by correcting craniocerebral disproportion by increasing intracranial volume and also addressing the Chiari Type I deformity that resulted from syndromic multi-suture craniosynostosis in a child with craniometaphyseal dysplasia.
Keywords
Introduction
Patients with syndromic craniosynostosis can present a unique set of challenges with respect to their diagnosis and management of the associated pathological manifestations. Surgical management of craniofacial dysmorphism and elevated intracranial pressure in these patients includes a multitude of procedures. Posterior cranial vault distraction has emerged as an effective technique to expand the intracranial volume, reduce turribrachycephaly and correct craniofacial dysmorphism in patients with syndromic multi-suture craniosynostosis.1,2 While advancement of the fronto-orbital complex increases intracranial volume, posterior vault expansion proportionally generates a greater volumetric increase.3,4 Distraction osteogenesis has increased the potential for bony advancement in craniofacial surgery, with reduction of overall morbidity and less likelihood of relapse 5 as well as reduction in operative times, blood loss and length of hospital stay.3-5 However, complications related to distraction techniques include device failure, infection, skin necrosis, as well as the complications related to osteotomies and device exposures. 6
Craniometaphyseal dysplasia is a rare genetic condition that is characterised by craniofacial hyperostosis which results in physical dysmorphology as well as symptomatology due to compression of anatomical structures by the hypersclerotic calvarium, including cranial nerve neuropathies and raised intracranial pressure.7,8 We present a rare case of multi-suture craniosynostosis with increased intracranial pressure in a child with craniometaphyseal dysplasia who underwent surgical management and the technical challenges navigated in performing a posterior cranial vault distraction.
Case Report
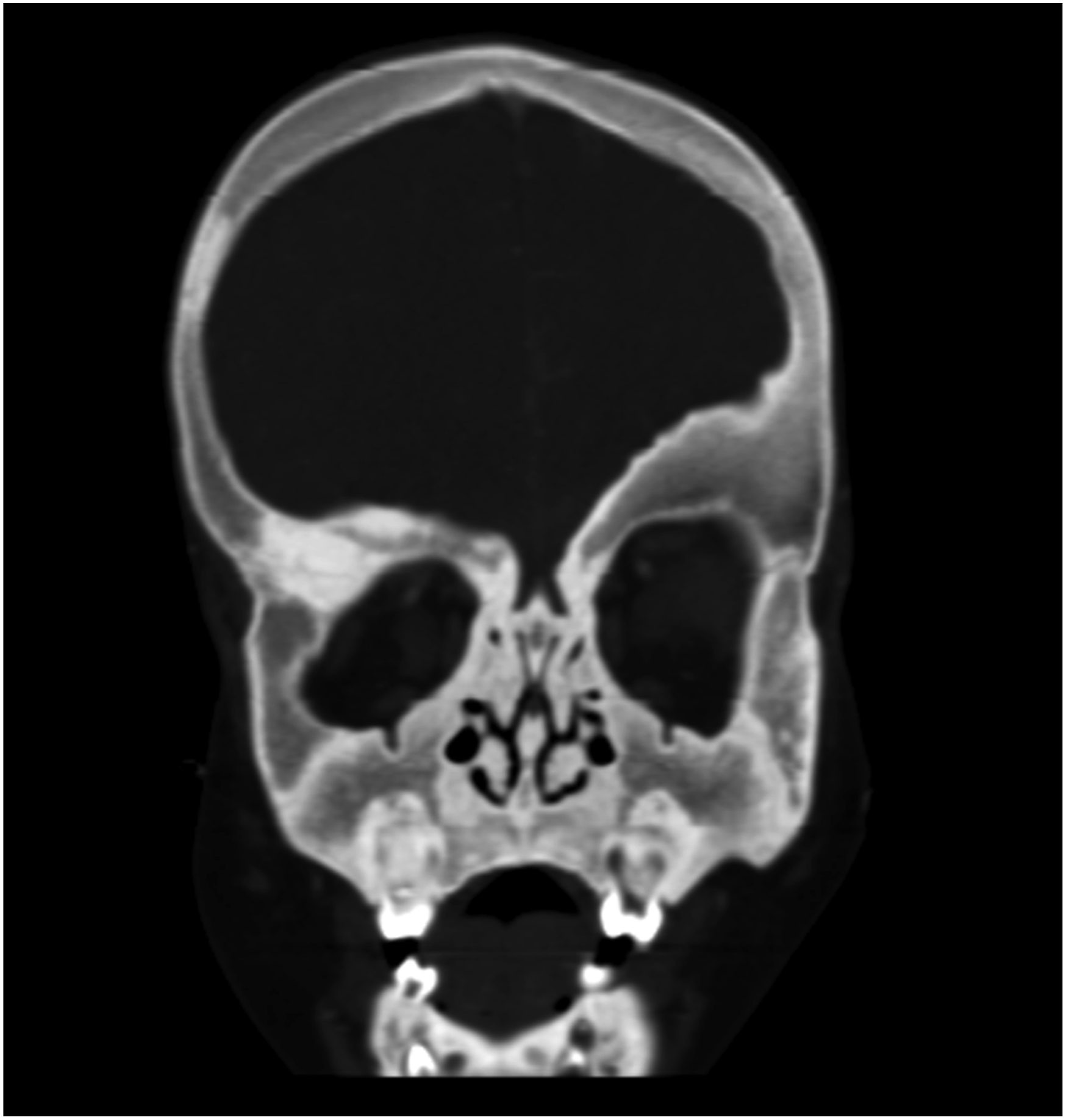
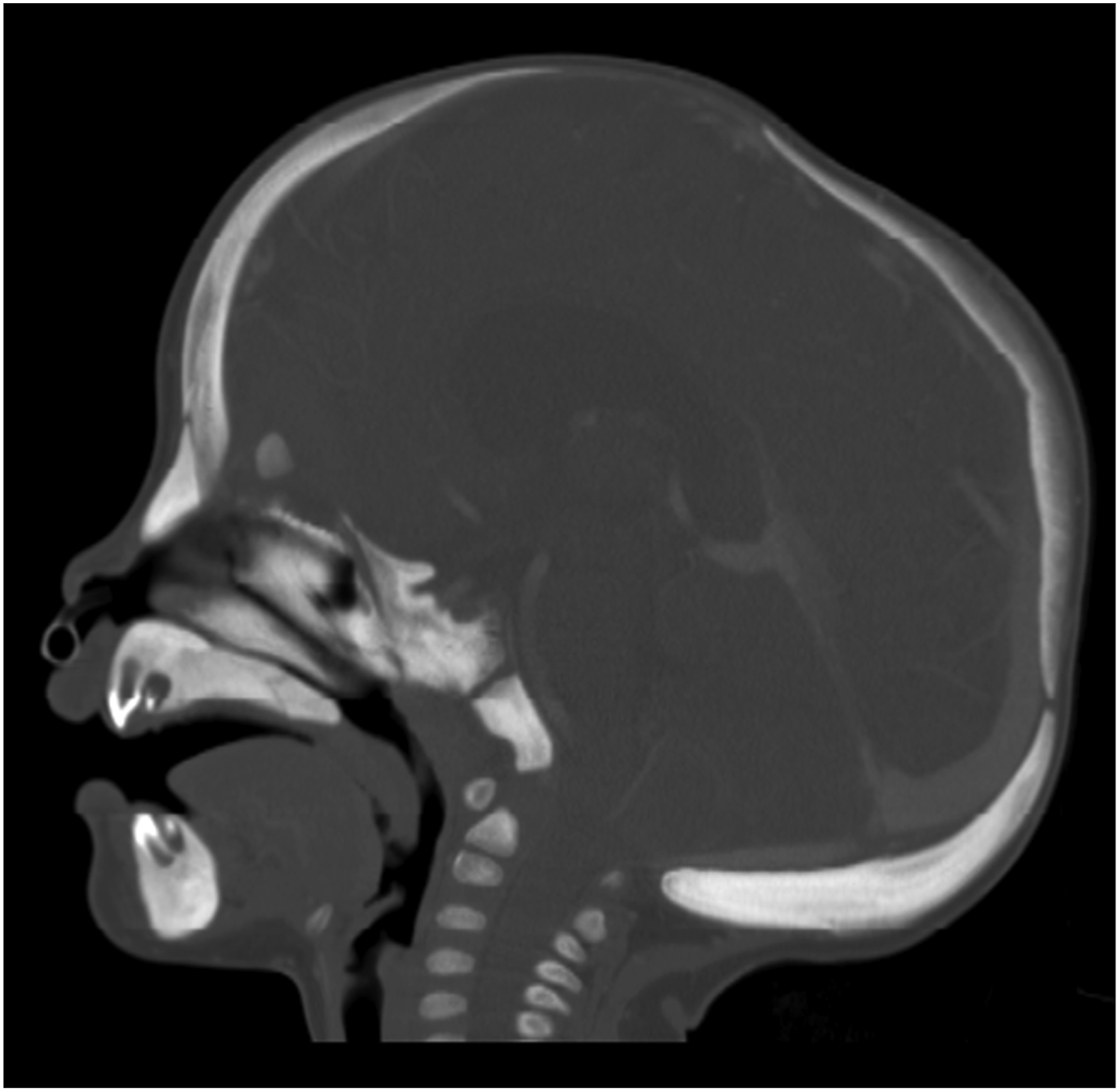
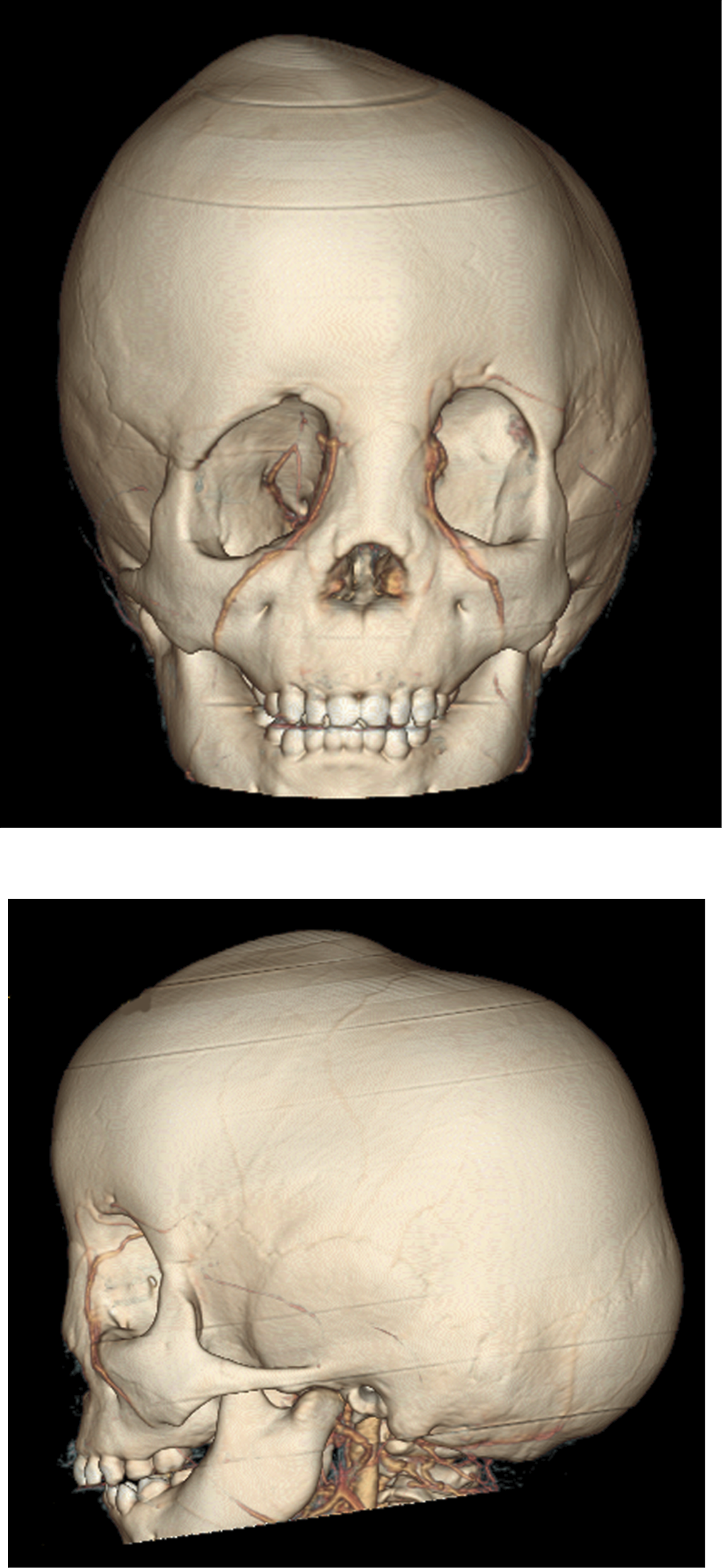
A 1 year old boy presented to the emergency department at the Hospital for Sick Children with macrocephaly and facial dysmorphology. (Figures 1(a), (b), (c)) He was admitted by the paediatric medicine team for diagnostic work up. The infant had bilateral facial nerve palsies and multi-suture craniosynostosis in the context of an unknown syndrome. His skeletal survey revealed abnormal morphology of his long bones and the computerized tomography (CT) scan demonstrated a diffuse skeletal hyperostosis of his craniofacial skeleton including obstruction of sinuses and narrowing of multiple cranial nerve foramina. (Figures 2 and 3) Radiographic imaging confirmed sagittal and left unicoronal craniosynostosis (Figures 4(a), (b)). Ocular examination at that time was normal. After comprehensive endocrine and genetic investigations, he was diagnosed with craniometaphyseal dysplasia. Anterior (A) and Lateral (B and C) Photographs showing craniofacial morphology. The patient is brachycephalic, has orbital asymmetry, left frontal recession, nasal root deviation to the left and right frontal bossing. Coronal Bone Window of CT image demonstrating midface hyperosteosis with nasal vault stenosis, sinus obliteration and generalised thickening of facial skeleton. Sagittal view of CT image of head demonstrating craniofacial hyperostosis at time of diagnosis. The bone was 18 mm thick in areas, which presents technical challenges in performing the cranial osteotomies. Anterior (A) and lateral (B) view of 3 dimensional CT image demonstrating craniofacial hyperostosis and craniofacial skeletal dysmorphology. The CT highlights the left unicoronal craniosynostosis and associated with a ipsilateral frontal recession, orbital and nasal deformity, as well as compensatory contralateral (right) frontal bossing. Left lateral view of three-dimensional CT image demonstrating hyperostosis, left unicoronal and sagittal craniosynostosis.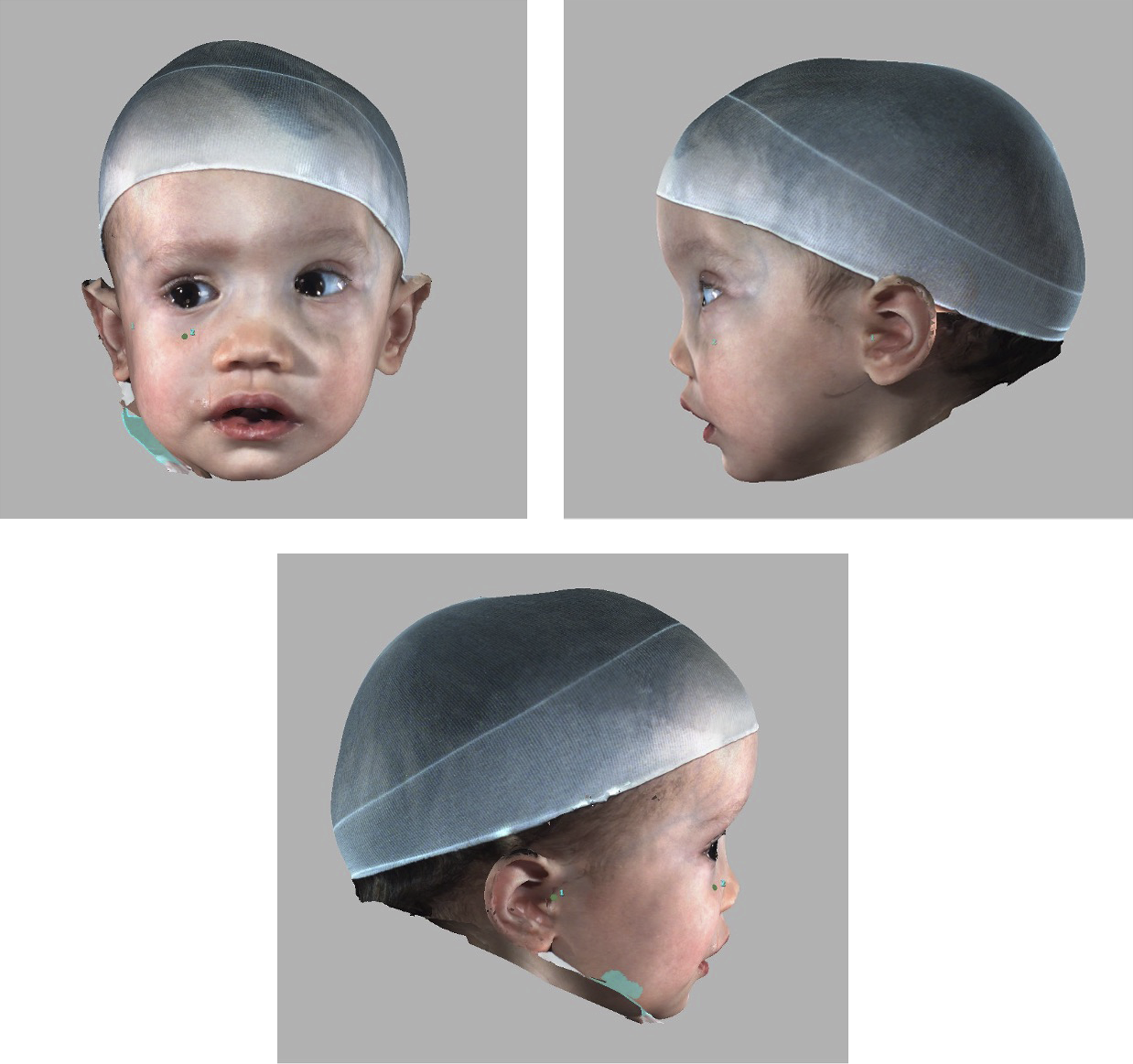
At 18 months of age, an anterior cranial vault remodelling was initially planned but subsequently cancelled because the hyperostosis of the supra-orbital region presented substantial technical challenges to bandeau and frontal reshaping and that the aesthetic concerns of the parents were minimal. Three months later, a magnetic resonance imaging (MRI) scan showed progression, with further thickening and expansion of the occipital bone (basioccipital, supraoccipital, and exoccipital) and severe narrowing of the foramen magnum (Figure 5) in addition to marginal interval progression involving the optic canals. Ophthalmologic examination at this time demonstrated new onset of papilloedema. The cause of papilloedema was considered to be potentially multifactorial, with contributions from the multi-suture craniosynostosis and possibly stenosis of the optic canals. Sagittal view of CT image of head demonstrating hyperostosis at time of surgery, with progression of both frontal and basal sclerosis and further narrowing of foramen magnum.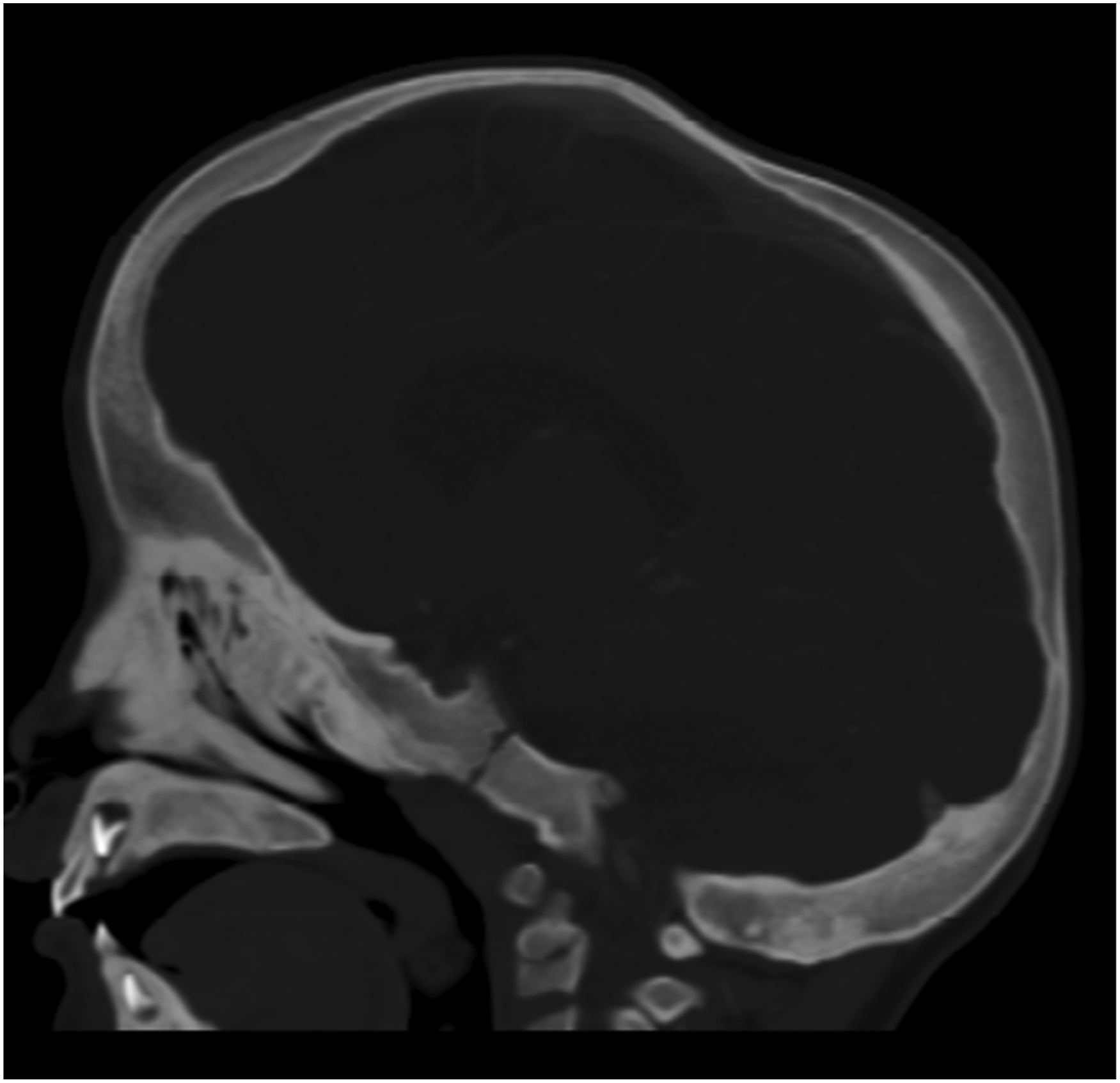
Imaging assessments were reviewed by the multi-disciplinary team of craniofacial surgeons, neuroradiologists, and neurosurgeons. Considerations for management included anterior cranio-orbital reshaping, posterior cranial vault expansion, total cranial vault reshaping to create additional intracranial volume and cerebral shunt. As per our protocol, venous imaging prior to posterior cranial vault surgery was obtained and demonstrated all dural venous sinuses were patent with some narrowing at the jugular foramina bilaterally on CT venogram. There were no prominent scalp veins identified but a prominent occipital sinus was identified. In reviewing the images, the minor degree of optic canal stenosis was not felt to be the primary cause of elevated ICP and not significant enough to warrant surgical decompression. The pre-operative cephalic index was .79. After discussion with the neurosurgeons, it was decided that posterior vault distraction would be the most efficient approach to increase the intracranial volume with the primary surgical aim being to lower the intracranial pressure in order to alleviate the papilloedema, and secondarily to alleviate the Chiari I deformity.
The patient was taken to the operating room and underwent general endotracheal anaesthetic as nasal intubation was difficult because of nasal stenosis as result of his craniometaphyseal dysplasia. Prophylactic antibiotics and tranexamic acid were given. The scalp was marked out for a coronal incision and in the supine position and the STEALTH navigation system was registered. Navigation was used to aid the neurosurgeons safely approach the intracranial space by identifying the underlying venous sinuses through the thickened calvarium.
In the prone position with appropriate padding on the face, the scalp was infiltrated with tumescent solution containing bupivacaine (Marcaine) .25%, xylocaine 1% with 1:200 000 epinephrine, adrenalin and kenalog. Via the coronal incision, the scalp was elevated to the superior nuchal line at the subgaleal level. The craniectomy was marked and the periosteum minimally reflected and the bone exposed over a minimal area at the craniotomy site. In some locations, the bone thickness was 18 mm which presented technical challenges. Our usual approach of burr holes and craniotome could not be used in this case as the craniotome footplate was unable to safely engage the full thickness of the hyperostotic calvarium. To approach the intracranial cavity, the neurosurgeons used a combination of burrs and rongeurs to create osseus gutters around the intended craniotomy site and a Kerrison Punch to complete the osteotomy, creating the posterior vault cranial bone flap. This was performed without any dural tears or significant bleeding. Once the posterior vault segment was mobile, the bone distractors (KLS Martin) were placed in a collinear and parallel fashion and secured with a series of 5 mm screws. Small grooves were made to allow the pre-fabricated footplates to engage on the bony edge of the cranial bone flap because of the excess bony thickness it was not possible to secure it beneath the flap in the usual fashion. The vector was checked and found to be appropriate. The skin was then closed using 4-0 Monocryl and 4-0 Caprosyn monofilament dissolving sutures. The patient was placed in the supine position and the distractor arms were applied. Intraoperatively, the patient was transfused 100 cc of packed red blood cells. Total operative time was 103 minutes. At the end of the procedure, the patient was extubated and transferred to the paediatric intensive care unit for monitoring overnight, before being admitted to the plastic surgery ward the following morning.
An x-ray was performed on post-operative day 1 to confirm distractor position and alignment (Figure 6). Distraction commenced on post-operative day 1 at a rate of .5 mm twice per day. The patient was discharged home on post-operative day 3 and seen in the outpatient department 1 week following discharge. The wounds were clean with no clinical signs of infection or subcutaneous fluid collection. An interval cephalogram was taken and distraction progress was assessed. The distraction continued for the next 3 weeks until the device was out to length (35 mm) and plain lateral x-ray imaging was performed twice to monitor the progress of distraction (Figure 7). At the end of the distraction period, the distractor arms were disengaged in the outpatient clinic. Two months were allowed for bony consolidation. Three months after the initial procedure, the patient returned to the operating room to have the distractors removed and was discharged from hospital the next day. Lateral x-ray pre-distraction of posterior cranial vault, with KLS-Martin distractors in situ. Lateral x-ray post 35 mm of posterior cranial vault distraction.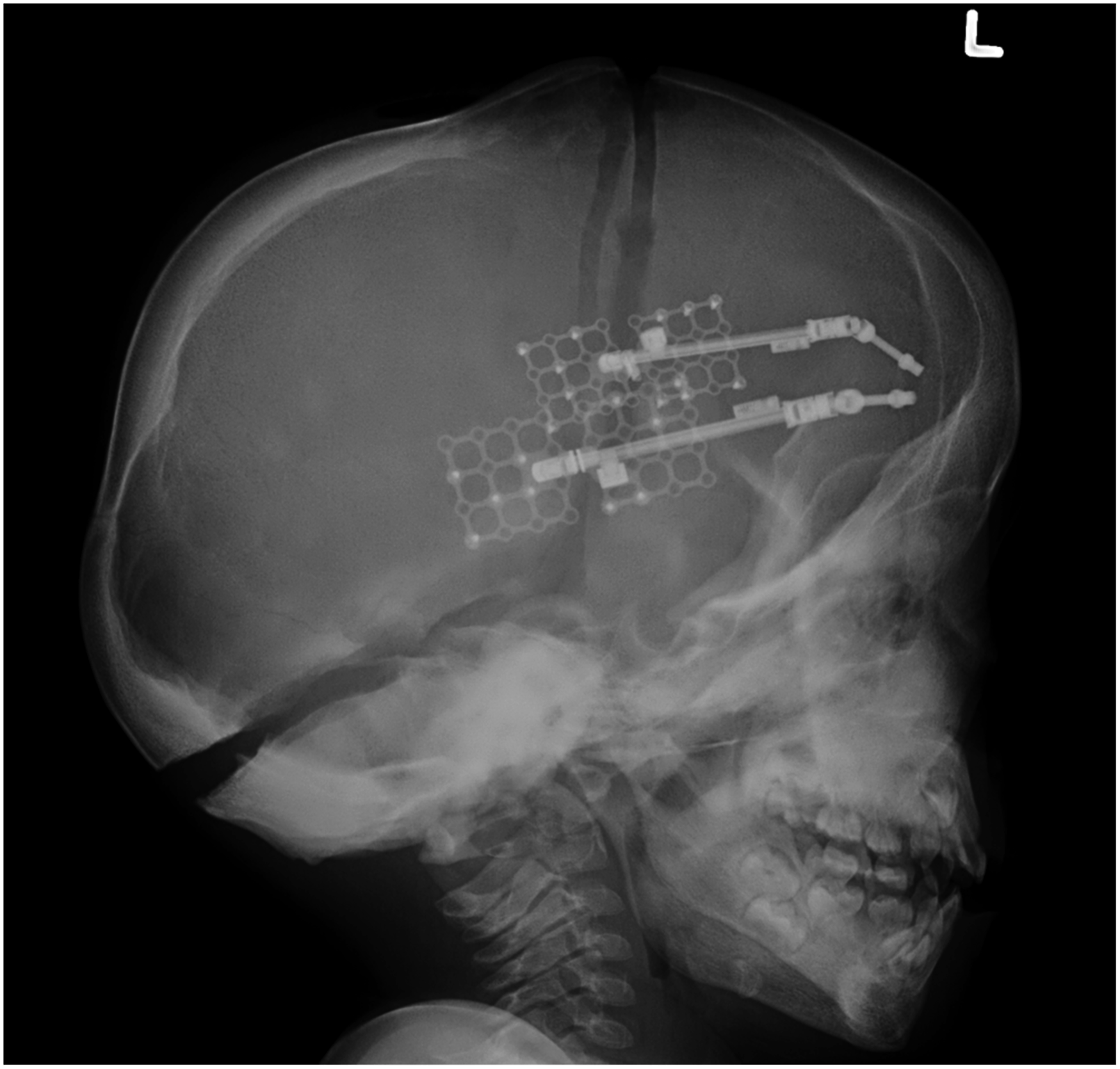
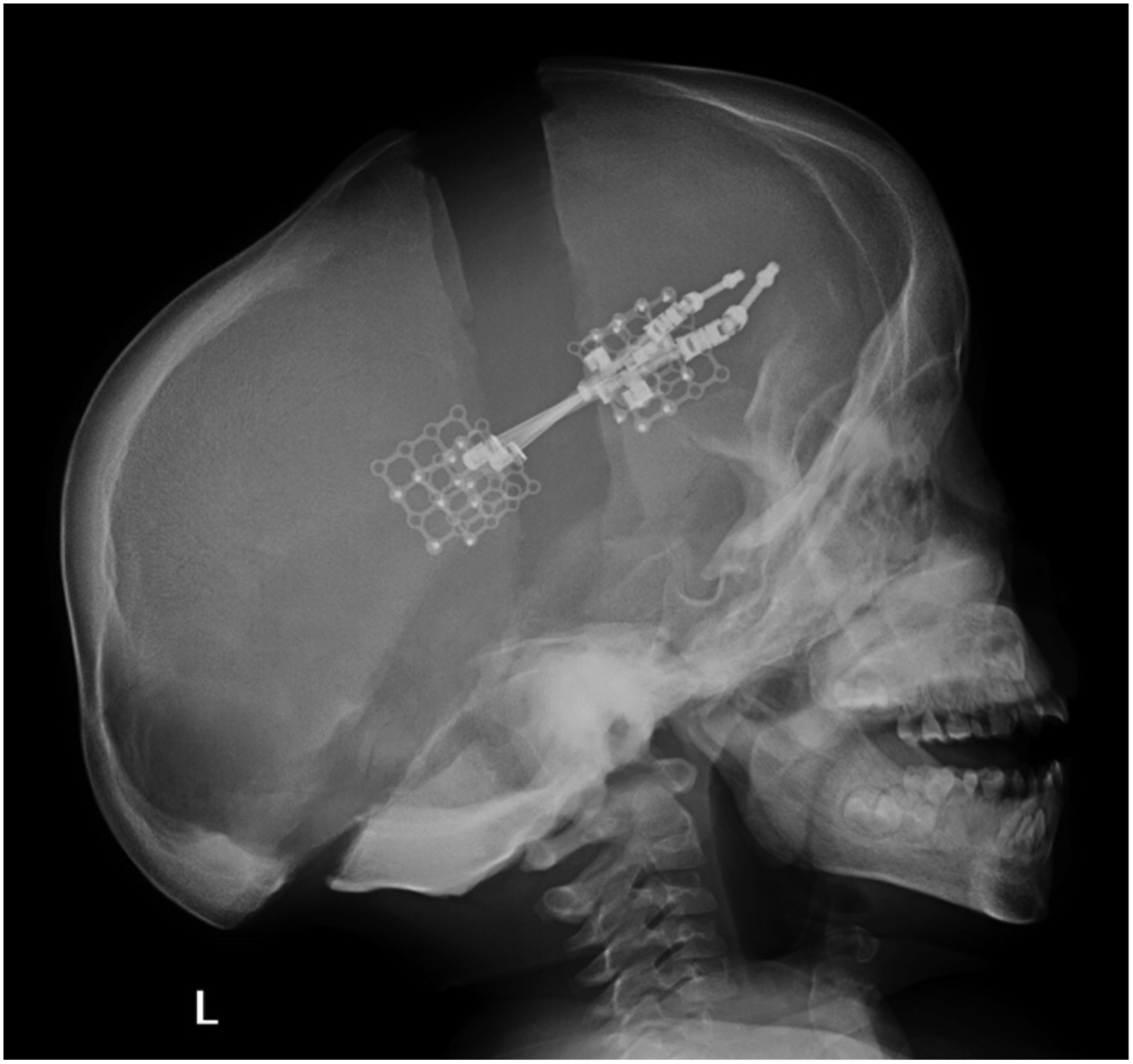
There were no post-operative complications and the patient progressed as anticipated. Follow-up imaging and ophthalmological examination at 6 and 9 months post-operatively revealed the papilloedema had resolved. The cephalic index improved post-operatively to .56 (from .79 pre-operatively). Clinically he continues to do well with satisfactory craniofacial form.
Discussion
Craniometaphyseal dysplasia is a rare genetic disorder due to a mutation in the ANKH or GJA1 genes characterized by hyperostosis and sclerosis of the craniofacial bones and metaphyseal widening of the long bones.7,8 It may be classified into the mild, more common autosomal dominant form and rare, severe autosomal recessive form. 9 It is associated with ANKH gene mutation which encodes the transmembrane protein that transports pyrophosphate ions toward the extracellular environment. Pyrophosphate ion concentration in bone extracellular matrix plays an important role in mineralisation. 9 With ANKH gene mutation, there is dysregulation of bony mineralisation resulting in hyperostosis and sclerosis. Craniometaphyseal dysplasia usually presents in infancy, with progressive facial weakness, visual disturbance and hearing loss secondary to stenosis of skull base foramina due to calvarial hyperostosis. Associated features of the syndrome can include craniofacial dysmorphology with nasal bridge widening, ocular hypertelorism, bossed forehead and a prominent mandible. Bulging fontanelles, cranial nerve palsies, macrocephaly, Chiari I deformity, craniosynostosis and long bone dysplasia have been described in this condition. 6 Due to the rare nature of the syndrome, it is difficult to estimate the true incidence of craniosynostosis. In the autosomal recessive form, where hyperostosis is more severe, the rise in intracranial pressure due to foramen magnum stenosis may be lethal.
Craniofacial hyperostosis with or without appendicular skeletal involvement in children is not unique to craniometaphyseal dysplasia. A number of conditions should be considered in the differential diagnosis, including frontometaphyseal dysplasia, craniometaphyseal dysplasia, craniodiaphyseal dysplasia,7,10 Van Buchem Disease, Craniofacial fibrous dysplasia, Maroteaux-Lamy disease and Camurati-Engelmann disease11-13
In the management of syndromic craniosynostosis, surgical options, timing of treatment, resolution of craniofacial dysmorphology, ocular and respiratory symptomatology must be carefully considered in context of the underlying genetic status of the condition. Rare and unusual cases such as craniometaphyseal dysplasia present additional problems due to the hyperostotic nature of the bone. Access to the dura-endocranial surface, ability to safely osteotomize the calvarium, application of cranial distractors, and bleeding are some of the technical challenges associated with this case. Pre-operative imaging combined with intra-operative navigation allowed site-specific information about bone thickness and underlying venous anatomy. Careful use of a high-speed burr (match-stick) was associated with no dural breaches. Distractor footplate modification was required as the depth of the pre-fabricated devices will not engage as they typically would to the cranial surface of the flap. Small osseous grooves were created in the bony flap and calvarium to fixate the modified footplate and provide bony stability. Bone quality for screw fixation was not an issue in this condition. Bone healing did not appear to be affected by craniometaphyseal dysplasia. In the future, we plan for the anterior plagiocephaly associated with the unicoronal craniosynostosis to be managed expectantly as he gets older and there is not an immediate plan to perform an intra-cranial procedure given technical challenges of the intraorbital osteotomies. His anterior plagiocephaly has remained stable. In the future should the patient need frontal contouring, an extracranial camouflage procedure will be arranged.
There are a variety of surgical options to correct cranio-cerebral disproportion that include posterior vault reshaping, anterior cranio-orbital advancement and reshaping, total cranial vault reshaping and posterior cranial vault distraction. In this case, given the increased bone thickness and the technical challenges in performing a frontal-orbital osteotomy with bandeau reshaping due to the bone thickness, a posterior cranial vault distraction is advantageous because it is less invasive and having the biggest impact on increasing cranial volume. However, this comes at the expense of creating cranial dysmorphology (scaphocephaly). In this case, posterior cranial expansion was successful in correcting craniocerebral disproportion caused by multi-suture synostosis with resolution of papilloedema and intracranial pressure.
Conclusion
Posterior cranial vault distraction has emerged as an effective technique to expand the intracranial volume and correct craniofacial dysmorphology in patients with multi-suture craniosynostosis and proportionally generates a greater volumetric increase compared with anterior cranial vault remodelling. Posterior cranial vault distraction was an effective method of addressing increased intracranial pressure by correcting craniocerebral disproportion by increasing intracranial volume and also addressing the Chiari Type I deformity that resulted from syndromic multi-suture craniosynostosis in a child with craniometaphyseal dysplasia.
Footnotes
Acknowledgments
The authors acknowledge support from the AO Trauma Fellowship.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
