Abstract
Study Design
Case report.
Objective
Sotos syndrome is a rare genetic disorder which is characterized by excessive physical growth during the first few years of life. The principal features of this condition include macrocephaly, learning disability and physical overgrowth. The current diagnosis of Sotos Syndrome is based on identification of genetic mutations and deletions in the NSD family (the
Methods
The initial phenotypical presentation was consistent with left coronal craniosynostosis. She underwent strip suturectomy and orthotic helmeting with failure to correct her anterior plagiocephaly and orbital dysmorphology. Additional post-operative investigations revealed a multi-suture craniosynostosis. She subsequently underwent an anterior cranial vault reconstruction and fronto-orbital advancement.
Conclusions
Sotos Syndrome can be associated with single or multi-suture craniosynostosis. This is likely driven by the overgrowth status of this disease. In our case report, the patient presents with unicoronal craniosynostosis which progressed to multi-suture craniosynostosis. Therefore, a multidisciplinary approach and close monitoring by craniofacial surgeons, neurosurgeons, developmental paediatricians and other allied teams is required in the care of such patients.
Keywords
Introduction
Sotos syndrome is a rare genetic disorder characterized by cerebral gigantism and associated with a spectrum of non-progressive neurological symptoms. It was originally described in five children with a constellation of accelerated prenatal and postnatal growth, advanced bone age, variable developmental delay, and characteristic craniofacial features. 1 The genes that have been implicated in reported Sotos Syndrome include the NSD1 gene on Chromosome 5. It is estimated that 95% of cases are of de novo mutation with no predictable hereditary pattern. Very few families have multiple members with this condition and it appeared to be of autosomal dominant in such cases. The incidence of Sotos syndrome is estimated to be 1 in 10,000-14,000 newborns.
Craniosynostosis is the condition in which cranial sutures close prematurely. This leads to a failure of normal bone growth perpendicular to the suture. Compensatory growth occurs at other suture sites and results in a characteristic abnormal head shape. The overall incidence of craniosynostosis is one in 3000 live births. Craniosynostosis occurs as an isolated condition (isolated craniosynostosis) in 80% of cases or as part of a syndrome (syndromic craniosynostosis) in 20% of cases. Isolated craniosynostoses are usually simple, are not associated with other abnormalities and their etiology is non-genetic, the majority probably being caused by intrauterine fetal head constraint.
Since the original case report of Sotos Syndrome cases, there have been descriptions of other abnormalities including craniofacial anomalies, cardiac defects, and increased risk for tumor development. Most reported cases are sporadic, but familial cases have been identified. 2 Accelerated postnatal growth is most remarkable in the first four years of life with a gradual plateau in the growth rate. Although the height and weight of adults with Sotos syndrome may remain in the upper limits of normal range. 3 Single suture craniosynostosis has been associated with Sotos Syndrome in rare cases. 4 However, in our review, we found no reported cases of multi-suture craniosynostosis associated with Sotos syndrome. Our case report presents a complex case of Sotos syndrome with single-suture craniosynostosis that progressed to multi-suture craniosynostosis after strip suturectomy.
Case Report
A 3-week old female presented to the Craniofacial clinic at the Hospital for Sick Children with concerns for an abnormal head shape. She was born at 38 + 1 week’s gestation via elective Caesarian section with a brief hospitalization due to jaundice requiring phototherapy. Her abnormal head shape was noted at birth, specifically a flattening of the left side of the forehead with prominence of the contralateral side. Parents did not report any improvement between birth and presentation to our clinic. The family reported that this child was large for her age in the 95-98 percentile for weight and height without other developmental concerns. There was no family history of consanguinity, congenital anomalies, developmental delays/autism, or stillbirths/recurrent miscarriage.
Examination was notable for her weight in the 98th percentile based on WHO Growth Chart for Canada and height in the 99th percentile based on WHO Growth Chart for Canada. Her head circumference measured 48.5 cm which placed her in the 96th percentile for her age and gender. She displayed an inverted triangular shape to her face with a prominent right side of her forehead with flattening of the left side. This was associated with left sided temporal bulging and asymmetric eyebrow position (left side higher than the right). She had nasal root deviation to the left side and orbital dysmorphology with the orbital aperture of the left side larger and rounder than the right with evidence of bilateral lateral canthal dystopia. Her anterior and posterior fontanelles were open, soft, and flat and open right coronal, sagittal, metopic and bilateral lambdoid. She had a high arched palate and a narrow, prominent and pointed chin point. Examination of her upper extremities showed mild bilateral second and third cutaneous web space syndactyly. A detailed ophthalmological examination by a board-certified paediatric ophthalmologist showed normal eye examination and no evidence of papilledema.
The initial investigations included a bone-window computerized tomography (CT) scan of her head with three-dimension (3D) reconstruction. This showed partial fusion of the left coronal suture consistent with a left unicoronal craniosynostosis. This was associated with flattening of the frontal bones bilaterally (left > right) and bulging of the right frontal bone inferiorly and flattening and recession of the left supraorbital ridge. The metopic suture, sagittal suture, right coronal suture, bilateral lambdoid sutures and bilateral squamosal sutures were patent as shown in Figure 1. Pre operative 3D reconstruction CT scan showing left unicoronal craniosynostosis. (A): Frontal view, (B): Birds eye view, (C): Top view.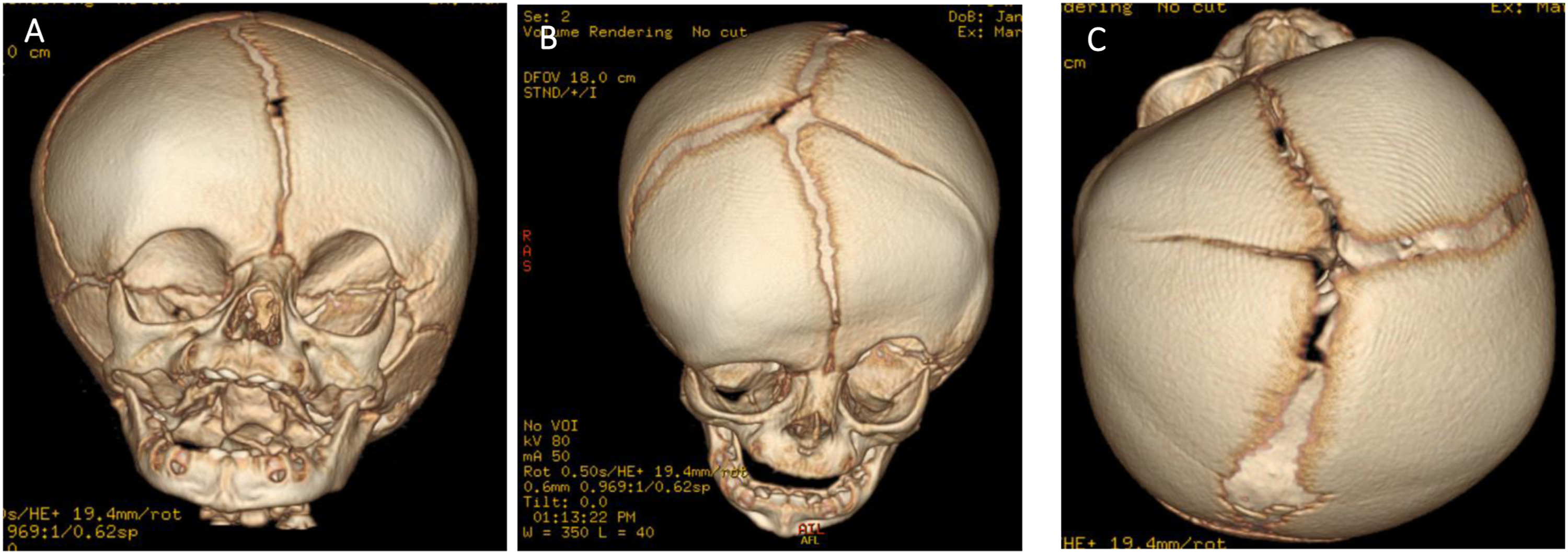
At three months of age, she underwent a strip suturectomy. She was discharged home on postoperative day one in stable clinical condition. The post-operative CT scan showed adequate release of left coronal suture (Figure 2). She was seen for follow up by the craniofacial team and a molding helmet was initiated on post-operative day 14. As part of our standard craniosynostosis management protocol, she was referred to medical genetics for assessment. immediate post-operative 3D CT reconstruction showing adequate suturectomy of left coronal suture. (A): Birds eye view, (B): left lateral view, (C): top view.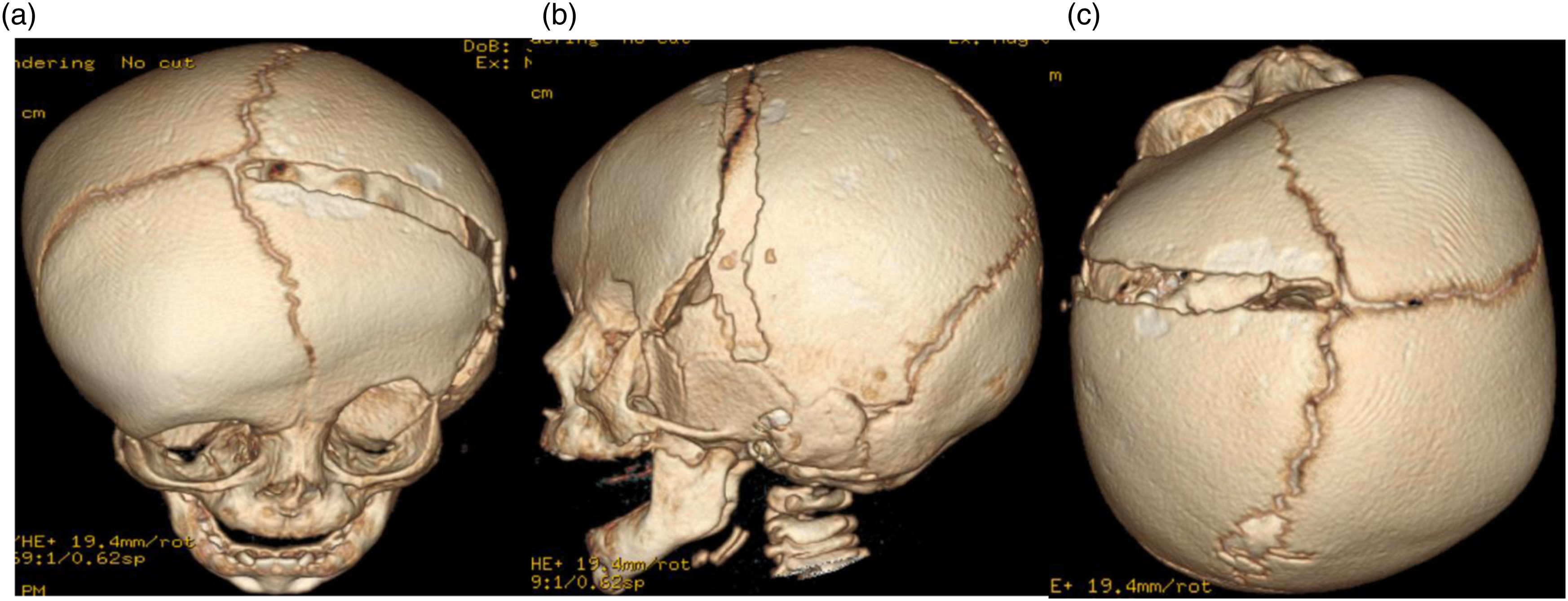
Three weeks post-operatively, the mother reported that the child was becoming very fussy with the helmeting and had inconsolable crying spells. She was reviewed by the general paediatric team and gastro-esophageal reflux was thought to be the reason for the irritability and was started on anti-reflux medications. At 6 months of age, she developed a seizure-like episode at home and was admitted to hospital where further work-up by Neurology was unremarkable. In the interim, genetic testing identified a pathological NSD1 variant, consistent with Sotos Syndrome.
She was followed regularly by the craniofacial and orthotics teams for head-shape correction. The follow up consisted of serial head-shape measurements and 3D photography and scanning analysis. After eight months of molding helmet, she had minimal head shape improvement. Therefore, a repeat CT scan demonstrated premature fusion of bilateral lambdoid sutures, sagittal suture, right coronal suture and bilateral squamosal sutures (Figure 3) with evidence of scalloping of the inner table of the cranium. These findings were consistent with new onset and progressive multi-suture craniosynostosis. An urgent ophthalmological examination did not identify any signs of papilledema or optic disc swelling. 3D reconstruction CT scans showing multi-suture craniosynostosis that was not evident in earlier scans. (A): frontal view, (B): Top view, (C): posterior view.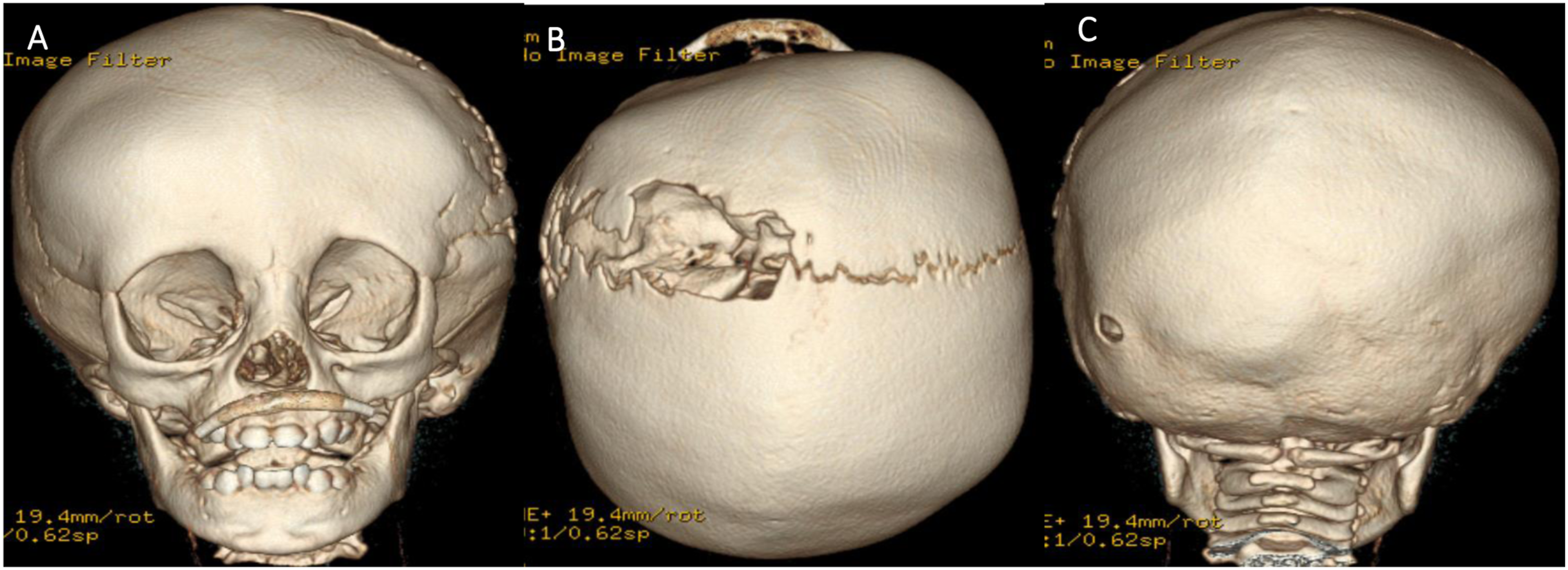
A multidisciplinary team discussed the surgical approach and due to residual head shape abnormality and radiological evidence of new onset multi-suture craniosynostosis, an anterior cranial vault reconstruction with fronto-orbital advancement was recommended. At age 17 months, this patient underwent this procedure with no complications. She was discharged home on post-operative day 3. Her post-operative CT scan showed good correction (Figure 3).
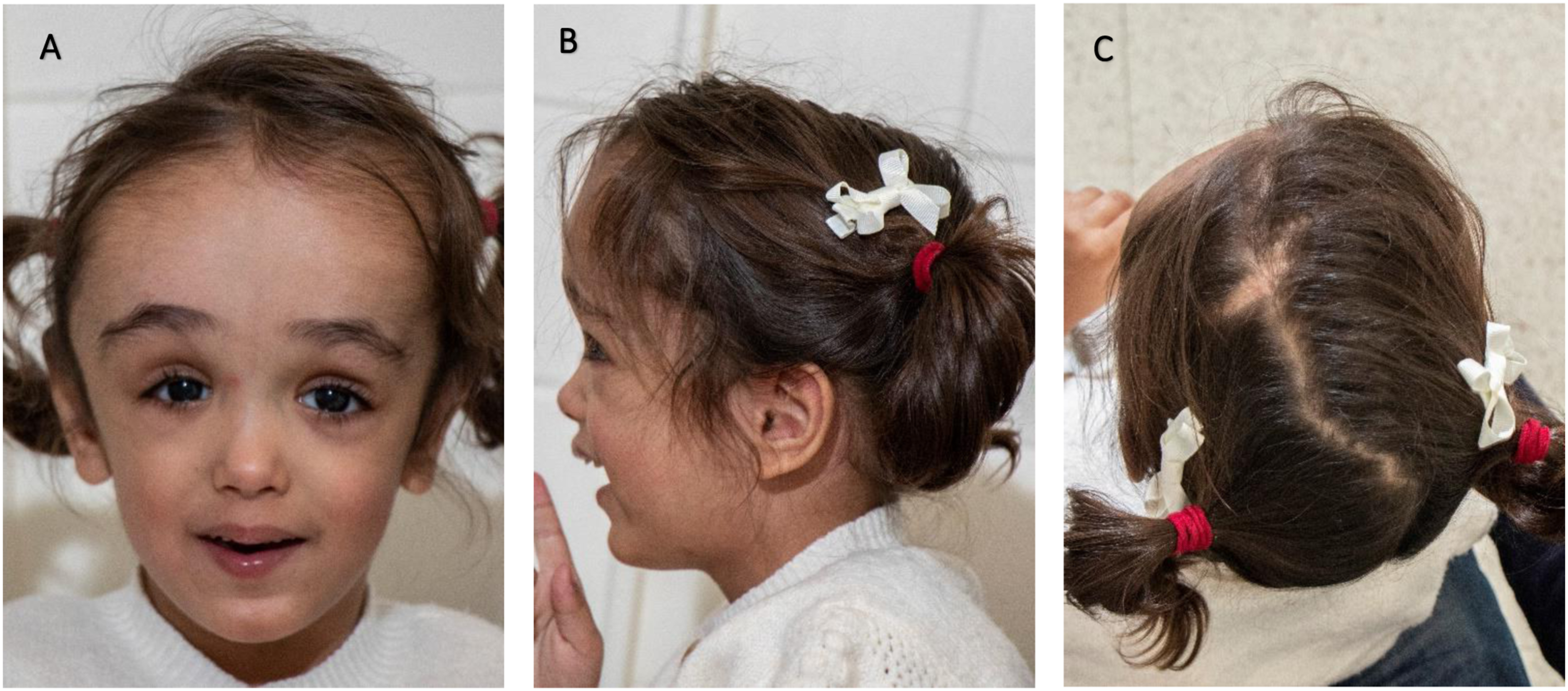
This patient was assessed regularly by the Craniofacial, Neurosurgery, Ophthalmology, and developmental paediatric teams (Figure 4). She continues to grow and her height and weight exceed the age normative values. Overall, the family is pleased with her head shape correction. She has a balanced cranial head shape with minor residual soft spots anteriorly. The family reported that her developmental milestones continue to improve, and she seems to be happier and less fussy as a child after the cranial surgery. Her ophthalmological examination did not show any evidence of papilledema or optic disc swelling. Figure 5 shows clinical photos of this patient at age 2 years old. Post operative CT scan after anterior cranial vault reconstruction and fronto-orbital advancement. (A): Frontal view, (B): Top view. Clinical photo of this patient at 2 years of age. (A): frontal view, (B): Left lateral view, (C): Top view.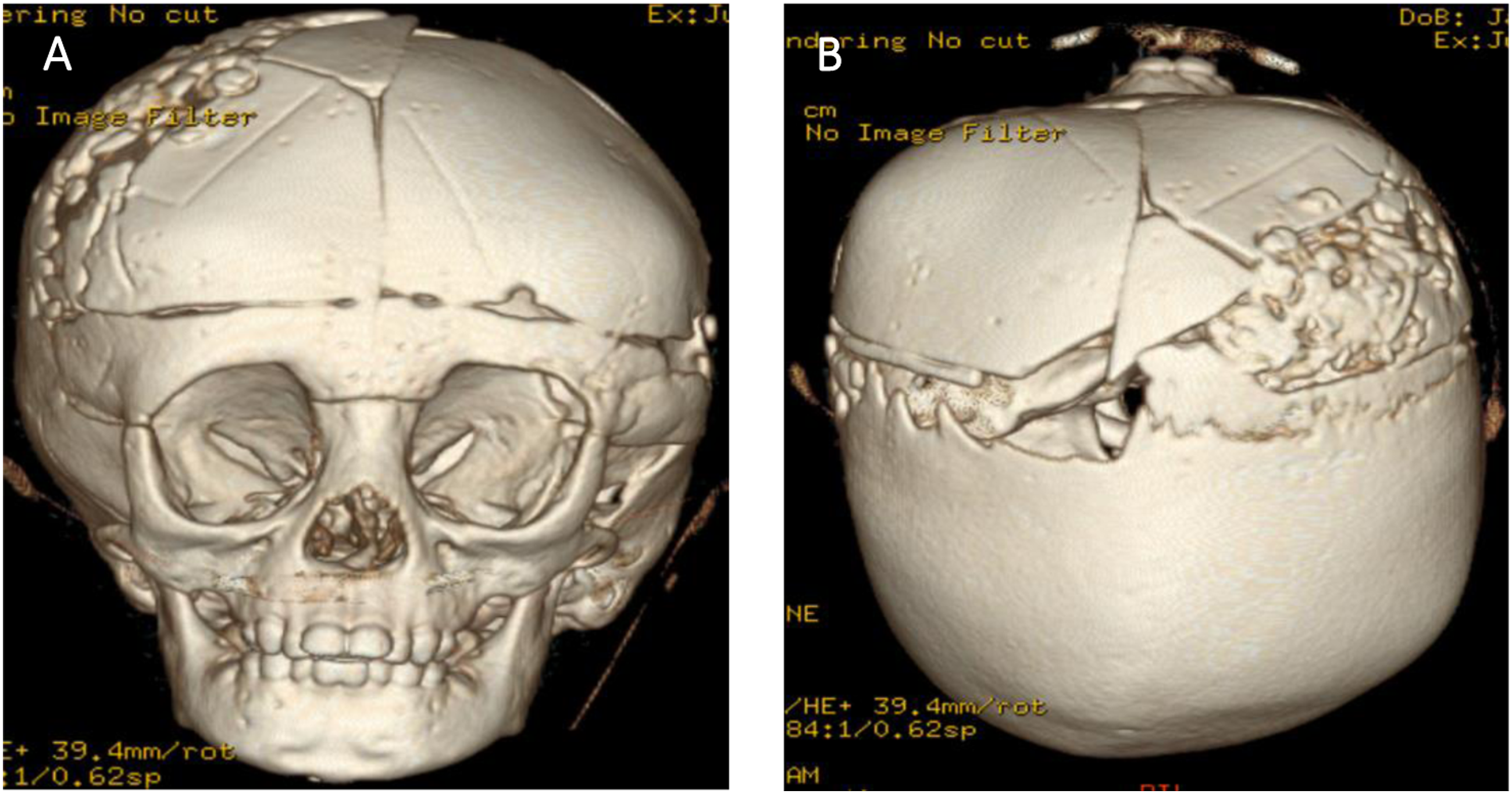
Discussion
We present a case of multi-suture craniosynostosis in a child with Sotos Syndrome that initially presented phenotypically as a single-suture coronal craniosynostosis. This case highlights pertinent craniofacial principles when managing children with syndromic craniosynostosis.
The classic facial shape of Sotos syndrome has been described as an “inverted pear”. The most prominent craniofacial feature is macrocrania and dolichocephaly which are usually present at birth and persist throughout life. The forehead is notably prominent with variable degrees of frontal bossing. These cranial features are more prominent due to the presence of bitemporal narrowing and frontoparietal balding. The palpebral fissures are downward slanting with strong supraorbital rims which may exhibit the appearance of hypertelorism due to narrow temples. However, true hypertelorism in Sotos children is rare. Craniofacial features also include a flat nasal bridge, high arched palate, and a pointed and prominent chin. Analysis of the progression of such craniofacial features show that individuals with Sotos Syndrome has these typical facies early in life and persist into adulthood. This is in contrast to some other syndromes in which the facial phenotype becomes less characteristic with growth and there may be few residual abnormalities by adulthood. 3 Anthropometric assessment reveals that the measurements in the craniofacial region for different age groups are at or above the 95th percentile of the normal range for children and adults.1-3 In childhood, it is the prominence of the forehead that is most striking. With age, it is the mandibular growth that is dominant, resulting in a long chin that may be pointed or square; however, mandibular prognathism is unusual. Maxillary overcrowding and malocclusion have been reported.
Sotos syndrome is a juvenile overgrowth disorder which has been reported across all ethnic groups. It has an autosomal dominant inheritance pattern. The incidence of this syndrome has been estimated to be 1:14 000 live births.
3
The diagnosis of this syndrome is based on clinical feature identification and genetic testing. Cole and Hughes
4
established a diagnostic criteria for the diagnosis of Sotos Syndrome based on forty-one classic cases. The four major criteria’s included macrocephaly, learning difficulties, characteristic facial appearance and overgrowth with advanced bone age. These clinical criteria’s were the cornerstone for Sotos Syndrome diagnosis until 2002 in which genetic testing became the diagnostic criteria.
3
The current diagnosis of Sotos Syndrome is based on identification of genetic mutations and deletions in the NSD family (the
The focus of therapy in Sotos syndrome aimed to improve speech and cognitive skills by early paediatric developmental interventions. Surgical interventions in Sotos Syndrome aims to provide children with Sotos Syndrome harmonious and balanced craniofacial features. Surgeries such as cranial vault reconstruction, canthoplasties and orthognathic surgeries have been described in the management of Sotos Syndrome.
There have been very few case reports of craniosynostosis in Sotos Syndrome. Brown reported two cases of sagittal craniosynostosis among 226 children with Sotos Syndrome. 3 As such, to the best of our knowledge, this case report is the first of progressive multi-suture craniosynostosis. Details about the other two reported sagittal craniosynostosis is limited and it is conceivable that their cranial suture status is not fully delineated depending on the follow up. Therefore, our case highlights that extra clinical vigilance about progressive nature of craniosynostosis in Sotos Syndrome is critical. Pre-operative and post-operative serial head-shape measurements and 3D photography and head-shape analysis is recommended. Further imaging in the form of bone-window CT scanning is warranted if there is clinical suspension for progressive craniosynostosis despite surgical intervention and helmeting.
We believe that our case developed multi-suture craniosynostosis due to their underlying condition (ie Sotos Syndrome) rather than consequential from the endoscopic suturectomy or helmeting therapy. However, there is some literature to suggest that cranial intervention and external pressure on the skull could induce craniosynostosis in sutures which are prone to premature fusion. 5 There have been a number of animal studies suggesting suture activity and fusion rates respond proportionately to external forces. This process is termed mechanotransduction. 5 Southard and Forbes 5 showed that the application of mechanical force to murine cranial sutures yielded significant histological changes, including increased suture width, vascularity, size, and the number of cells, amount of osseous production, and even alterations in suture morphology. These changes are associated with alterations in molecular signaling in the peri-sutural environment and arise as early as the first day of force. Proponents of this process feel that external forces from cranial helmeting could potentially induce premature fusion of previously patent but prone sutures. It is, however, equally possible that in our case the underlying genetic and epigenetic influences from Sotos Syndrome were already acting on the suture and the final endpoint (multi-suture fusion) is not related to helmeting.
Another concept that is highlighted in this case is whether the patent sutures identified in earlier CT scans were abnormal. Patency on radiological assessment alone is insufficient to infer about the status of the suture. There is a phenomenon of “sticky” suture which is abnormal hyperactivity of the suture material that is not osseous and therefore not identifiable on current CT scan imaging. This phenomenon has also been reported rarely in patient’s phenotypic features of craniosynostosis but no radiological evidence of premature fusion. Losee and others reported on a case of frontosphenoidal craniosynostosis that predates a radiological evidence of fusion on CT scan. 6 Furthermore, Baumgartner et al 7 reported a series of patients with deformational scaphocephaly and patent sagittal sutures. In his series, one patient presented with a persistent scaphocephalic phenotype after completing the helmet molding therapy. This prompted performing a CT scan, whose findings revealed a radiographic fusion of the sagittal suture that was treated surgically. Similar to what occurred in our patient, the latent suture fusion was only identified because there was a persistent phenotypic abnormality despite months of helmet therapy and endoscopic release.
In our case, the head shape was phenotypical for left coronal craniosynostosis and therefore we believe that left coronal craniosynostosis occurred before other sutures fused. Therefore, timing of which suture fuses first determines which phenotype predominates in multisuture craniosynostosis.
Finally, in our case, failure to correct the original cranial deformity despite strip suturectomy led to further imaging sooner than indicated by our established treatment protocol. It is feasible that if this child had a good correction after the endoscopic release, then the multi-suture craniosynostosis will be identified later on routine post-operative imaging. The early identification in our case initiated a closer monitoring and assessment for signs of papilledema and symptoms of raised intra-cranial pressure. Therefore, it is essential to establish close monitoring and follow up for syndromic craniosynostosis cases even for single suture fusion.
Sotos Syndrome can be associated with single or multi-suture craniosynostosis. Close follow up and monitoring in such patients is recommended in order to detect and manage the form and functional sequelae of such condition.
Supplemental Material
Supplemental Material - Multi-suture craniosynostosis in Sotos Syndrome: a case report
Supplemental Material for Multi-suture craniosynostosis in Sotos Syndrome: a case report by Sultan Al-Shaqsi and Christopher R. Forrest in Craniomaxillofacial Research & Innovation
Footnotes
Acknowledgments
The authors acknowledge support from the AO Trauma Fellowship.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
