Abstract
The finding of elevated basal lower esophageal sphincter (LES) pressure but normal integrated relaxation pressure (IRP) on high resolution manometry (HRM) can be due to multiple etiologies. In the absence of a structural cause, esophageal dysmotility should be considered, and functional lumen imaging probe (FLIP) can provide additional information about LES function not captured on HRM. We report the clinical outcomes of three patients from a single center with nonobstructive dysphagia without narcotic use, achalasia or previous foregut surgery who demonstrated a hypertensive LES on HRM with no CCv4.0 diagnosis but had abnormal FLIP findings with LES targeted endoscopic interventions leading to symptomatic improvement. This case series underscores the potential need for additional diagnostic testing in patients presenting with dysphagia who lack a definitive manometric diagnosis on HRM, specifically highlighting the complementary role of FLIP in the evaluation of these patients.
Keywords
Introduction
High resolution esophageal manometry (HRM) is often performed in patients with nonobstructive dysphagia who do not have endoscopic findings to explain their symptoms. 1 The Chicago Classification version 4.0 (CCv4.0) provides a framework for the diagnosis of esophageal motility disorders based on HRM findings. 2 While functional lumen imaging probe (FLIP) is primarily recommended as a confirmatory test for an EGJOO manometric diagnosis, studies have shown that FLIP can be used to further assess esophageal motility in symptomatic patients who do not meet CCv4.0 criteria for a motility disorder.3,4 For example, Ponds et al 4 used FLIP to identify 13 symptomatic patients with clinical and radiographic features of achalasia albeit with normal esophagogastric junction (EGJ) relaxation on HRM; FLIP identified impaired EGJ distensibility which guided lower esophageal sphincter (LES) directed therapy and led to symptomatic improvement. Another study of 164 patients found 20 (12%) of patients with a diagnosis of absent contractility on HRM had achalasia diagnosed on using FLIP and barium esophagography. 5 At our center, we also observed that FLIP can identify esophageal motility dysfunction in patients with hypertensive LES (elevated basal LES pressure but normal IRP) on HRM. In this case series, we describe the FLIP findings in these patients and the outcomes of treatments targeted at these FLIP findings (Table 1).
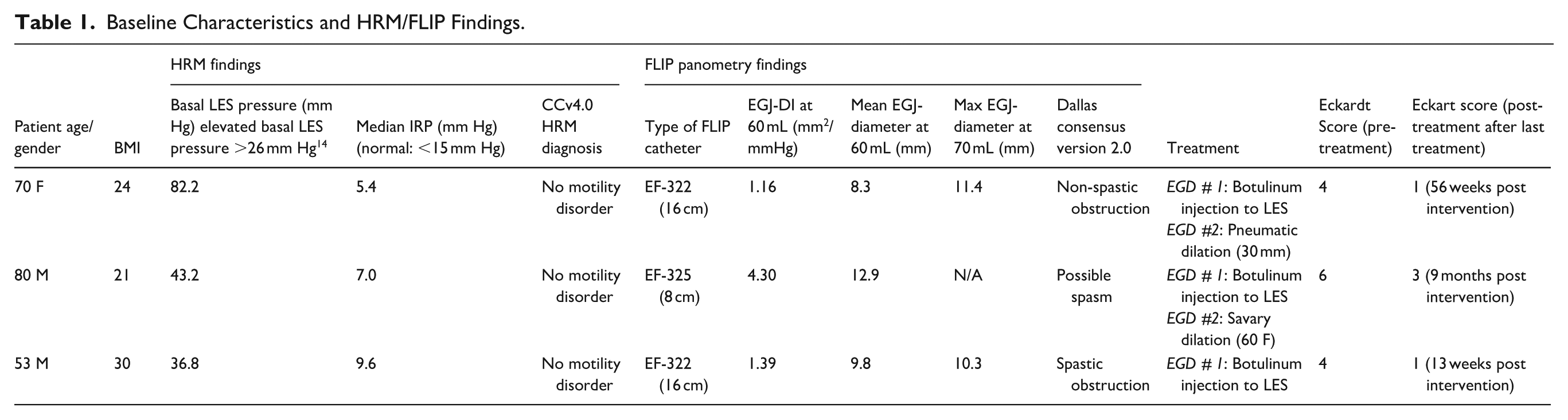
Baseline Characteristics and HRM/FLIP Findings.
Patient 1
70-year-old female presented with a 2-year history of progressive dysphagia to solids and liquids (Eckardt score 4). The esophagram demonstrated rapid liquid barium transit, with barium tablet retention at the LES and no clear stricture/ring. A small epiphrenic diverticulum was also noted, suggestive of LES dysfunction. HRM demonstrated a small hiatal hernia and basal LES pressure of 82.2 mm Hg with a median IRP of 5.4 mmHg. Endoscopy with FLIP was notable for a small epiphrenic diverticulum and reduced-EGJ opening (REO) with absent contractile response (ACR) pattern (Figure 1a). Botulinum injection to the LES was performed with incomplete relief of symptoms. Repeat EGD with 30 mm hydrostatic balloon dilation resulted in clinical remission (Eckardt score 1) and continued to have symptom improvement at 56 weeks post intervention (Table 1).
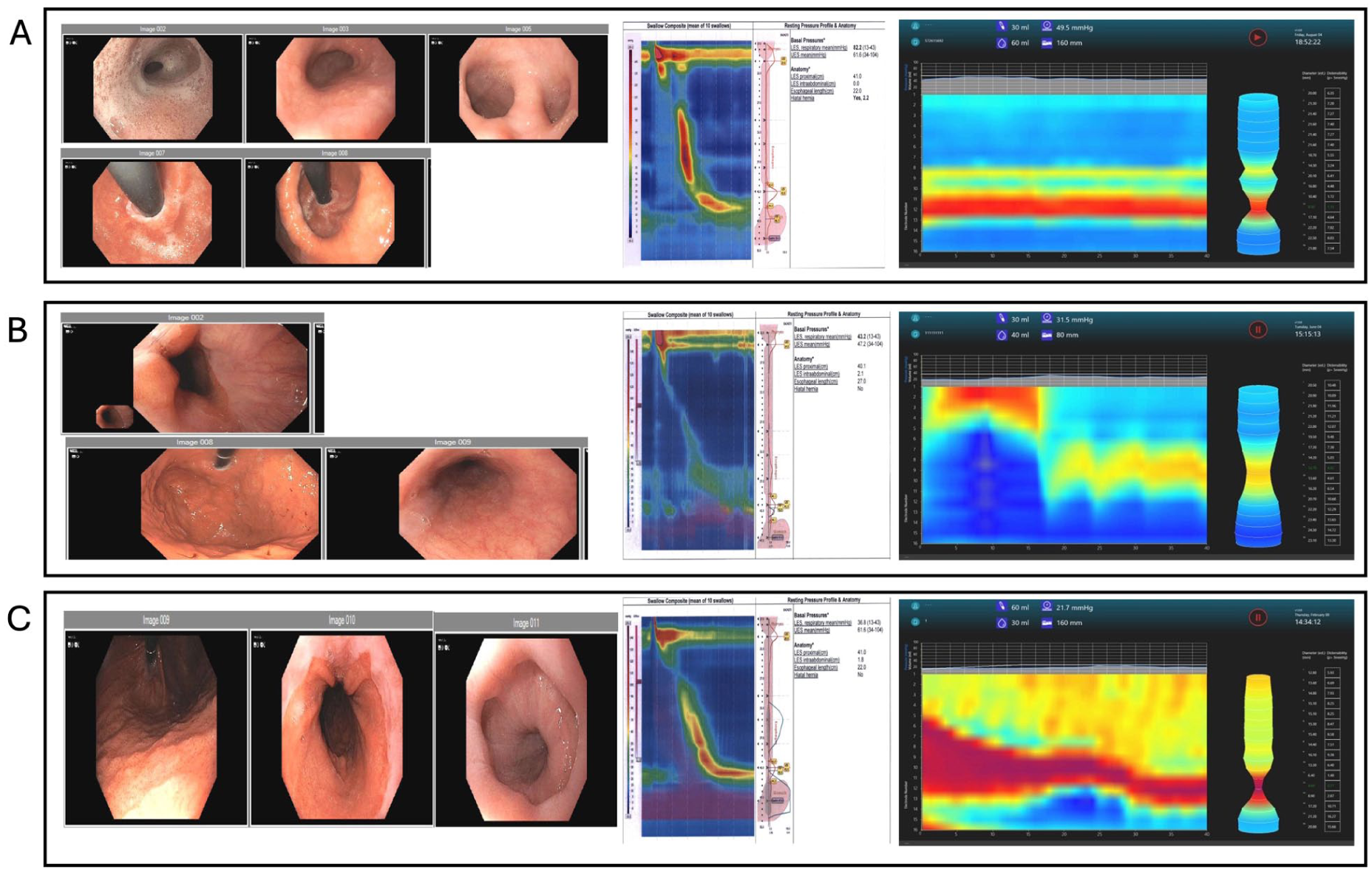
Endoscopy images, HRM findings, and FLIP patterns in study patients. (a) Patient 1: Endoscopy confirmed no stricture or Schatzki’s ring at gastroesophageal junction. Retroflexed views with AFS Grade III flap valve with small hernia. Esophageal body was notable for frothy secretions and a small ephiphrenic diverticulum. Manometry composite image displayed with no motility disorder per CC4.0. Using EF-322 catheter at 60 mL fill volume, mean EGJ-DI was 1.16 mm2/mm Hg and mean EGJ diameter was 8.3 mm with a maximum diameter of 11.4 mm at 70 mL with absent contractile response pattern. Persistent narrowing above the GE junction corresponded with location of epiphrenic diverticulum. (b) Patient 2: Endoscopy confirmed no stricture or Schatzki’s ring at gastroesophageal junction. Retroflexed views with AFS Grade I flap valve. Esophageal body was normal. Manometry composite image displayed with no major motility disorder per CC4.0. Using EF-325 catheter at 50 mL fill volume, mean EGJ-DI was 4.3 mm2/mm Hg, mean EGJ diameter was 12.9 mm with sustained occluding contraction pattern. (c) Patient 3: Endoscopy confirmed no stricture or Schatzki’s ring at gastroesophageal junction and LA Grade A esophagitis. Retroflexed views with AFS Grade II flap valve. Esophageal body notable for spastic contractions. Manometry composite image with no motility disorder per CC4.0. Using EF-322 catheter at 60 mL fill volume, mean EGJ-DI was 1.39 mm2/mm Hg and mean EGJ diameter was 9.8 mm with a maximum diameter of 10.3 mm at 70 mL with repetitive retrograde contractions.
Patient 2
80-year-old male presented with a 5-year history of progressive dysphagia to solids (Eckardt score 6). Patient reported longstanding reflux symptoms that persisted despite being on proton pump inhibitor. Esophagram was unremarkable with prompt passage of liquid barium and barium tablet. HRM demonstrated basal LES pressure of 43.2 mm Hg but normal IRP 7.0 mmHg. Endoscopy with FLIP was notable for normal EGJ distensibility but sustained occluding contraction (SOC) suggestive of spastic contractile response (Figure 1b). Botulinum injection to the LES was performed with incomplete relief of symptoms. Repeat EGD with 60 Fr Savary dilation performed showed no mucosal disruption but resulted in clinical remission (Eckardt score 3) at 9 months follow up.
Patient 3
53-year-old male presented with a 10-year history progressive dysphagia and odynophagia that worsened over the past several months (Eckardt score 4). Patient reported longstanding reflux symptoms that persisted despite being on proton pump inhibitor. Esophagram demonstrated rapid transit of contrast, but mild retention of the barium tablet at the LES with no clear stricture or ring seen. HRM was notable for basal LES pressure of 36.8 mmHg with intrabolus pressurization noted but did not meet criteria for a CCv4.0 motility diagnosis. Subsequent endoscopy with FLIP was notable for reduced-EGJ opening (REO) with repetitive retrograde contractions (RRCs) suggestive of spastic obstruction, albeit at lower fill volumes of 30 to 40 mL (Figure 1c). LES-botulinum injection was performed which resulted in clinical remission (Eckardt 1) at 13-week follow-up.
Discussion
Our case series highlights that FLIP can serve as a valuable tool for detecting esophageal motility abnormalities in symptomatic patients when HRM does not demonstrate a CCv4.0 motility disorder.
The hypertensive LES was first described by Code et al 6 and is defined as a LES pressure above 40 mm Hg with normal LES relaxation on conventional manometry. Waterman et al 7 reported that a majority of patients with hypertensive LES may express anxiety and somatization with chest pain and dysphagia being common symptoms. Treatments that have been described in the literature include medication, 8 endoscopic dilation, 9 or surgery. 10 While the development of high resolution manometry has led to advances in the diagnosis of esophageal motility disorder, the finding of elevated basal LES pressure in the presence of normal LES relaxation and absence of a structural cause still occurs and warrants further evaluation in patients when there is a high clinical suspicion for esophageal dysmotility.
Unlike HRM which evaluates LES relaxation and primary peristalsis triggered by swallowing, FLIP panometry measures EGJ distensibility and secondary peristalsis as a mechanical response to distention. Thus, FLIP panometry can provide additional information in the diagnostic workup of patients with esophageal symptoms who do not meet CC4.0 criteria for a motility disorder. FLIP provides unique insight into whether the observed physiology reflects primarily a biomechanical abnormality versus and neuro-sensory or spastic reactive process; reduced EGJ distensibility represents the structural or functional abnormality of LES, while SOC or repetitive retrograde contractions suggest heightened neuromuscular or spastic reactivity. Our cases highlight the overlap of both findings, as patients demonstrated both impaired EGJ opening and spastic contractile responses. Recognizing this overlap may help tailor therapy. One study found spastic secondary contractions on FLIP in 10 symptomatic patients with no CCv4.0 motility disorder or ineffective esophageal motility which guided different treatment modalities and led to symptomatic improvement in eight out of ten patients. 11 In our case series, FLIP uncovered abnormal EGJ opening and/or spastic contractile response in symptomatic patients which helped guide treatment. FLIP panometry interpreted with the Dallas Consensus provides complementary information to phenotype symptomatic patients and enhance patient-centered decision making in clinical management. 12 Furthermore, it may allow for objective monitoring after therapeutic interventions. In our case series, patients 2 and 3 had chronic reflux symptoms refractory to medical therapy, raising the possibility that reflux-related reactive physiology may have contributed to the abnormal FLIP findings. This highlights the overlap between reflux-related dysfunction and spastic contractility, and the potential role of empiric dilation as a therapeutic option in this group, especially given the cost of performing FLIP.
The initial treatment performed in this case series was LES directed botulinum injection with a dilation offered to patients who had a poor symptom response or recurrence of their symptoms. Botulinum injection was selected as an initial, less invasive therapy to assess for symptom responsiveness for both spastic and biomechanical physiology, while dilation was reserved for those with incomplete or recurrent symptoms to provide a more durable mechanical effect. Based on the literature, durable LES directed therapy such as pneumatic dilation or myotomy can be considered, especially if additional testing shows reduced EGJ opening on FLIP or radiologic evidence of outflow obstruction as discrepancies between esophageal physiology testing can commonly occur. 13 As some patients can have spontaneous improvement in esophageal motility over time, we recommend a stepwise approach based on clinical symptoms and objective testing results. 14
In conclusion, symptomatic patients with elevated basal LES pressure on HRM without a CCv4.0 diagnosis can be due to obstructive physiology which can be further elucidated with FLIP. LES directed interventions performed due to FLIP findings resulted in clinical improvement in our patient cohort. Based on these findings, we recommend performing FLIP in patients where there is a high clinical suspicion for a motility disorder and for those who have FLIP abnormalities, we suggest a stepwise, targeted approach to treatment.
Footnotes
Ethical Considerations
Informed consent was obtained from all participants.
Author Contributions
Pooja Prasad: data collection, drafting of the manuscript; Wasseem Skef: interpretation of data, manuscript writing and editing, revision of final manuscript; Anh D. Nguyen: interpretation of data, manuscript writing and editing, revision of final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Use of Artificial Intelligence
No artificial intelligence (AI) was used in the preparation of this manuscript.
