Abstract
Background:
Delayed gastric emptying (DGE) is the most common postoperative complication following any pancreatic resection. The incidence and risk factors of DGE in patients undergoing distal pancreatic resection (DPR) is not well defined. We aimed to determine the incidence of DGE not associated with postoperative pancreatic fistula (POPF) in patients undergoing DPR and to identify predictors of DGE.
Methods:
ACS-NSQIP pancreatectomy database (2014-2017) was queried for patients with pancreatic adenocarcinoma undergoing DPR, excluding patients with POPF. A classification and regression tree (CART) analysis was performed to identify risk for DGE, defined by nasogastric/gastrostomy tube placed after postoperative day (POD) 7 or no oral intake by POD 14.
Results:
A total of 1626 patients underwent DPR without POPF; 59 had DGE (3.6%). Patients with DGE had a longer length of stay vs patients without DGE (median 15 vs 6 days, P < .001). CART analysis showed vascular resection and open surgery were predictors of DGE with a specificity of 98.3%. Patients requiring vascular resection had a 7.8% rate of DGE. Patients who did not undergo open surgery or vascular resection had a 1.8% rate of DGE.
Conclusions:
The rate of DGE in patients undergoing DPR without postoperative pancreatic fistula is low. Predictors of DGE include open surgical approach and vascular resection. These findings may be utilized to counsel patients and take precautions in those at greater risk of developing DGE. Further research can involve implementation of a scoring tool to help stratify patients at risk for DGE after DPR.
This is a visual representation of the abstract.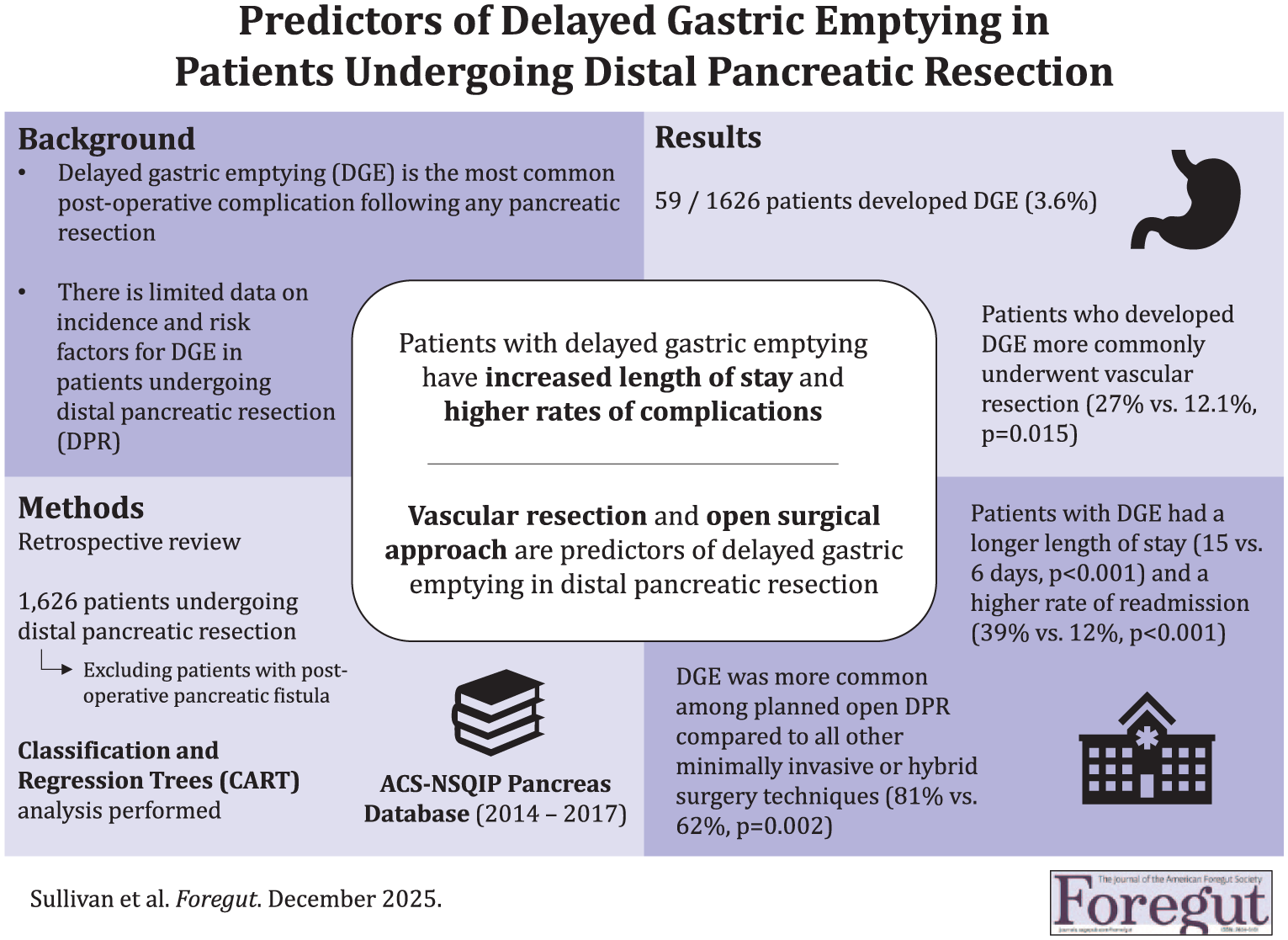
Key Learning Points
Delayed gastric emptying can result in increased length of stay and mortality.
Patients with delayed gastric emptying have higher rates of complications.
Vascular resection and open operations are predictors of delayed gastric emptying.
Identifying risk factors for delayed gastric emptying may minimize complications.
Introduction
Delayed gastric emptying (DGE) is the most common postoperative complication following any pancreatic resection.1,2 DGE has been shown to prolong hospital length of stay and increase hospital costs.3 -5 Prior to 2007, there was no standardized definition of what constitutes DGE, making it difficult to accurately evaluate the true incidence of this common postoperative complication. To remedy this, the International Study Group of Pancreatic Surgery (ISGPS) proposed a standardized definition of DGE after pancreatic surgery and classified it into three grades. Following the development of this classification system, the incidence of DGE for pancreaticoduodenectomy (PD) has been well established in the literature and ranges from 12% to 60%; however, there is a paucity of data regarding the incidence of DGE for patients undergoing distal pancreatic resection (DPR).
Due to the high rates of DGE after PD, multiple studies have evaluated the risk factors for DGE, which can be categorized as etiologic or complication related. Examples of proposed etiologies for DGE include comorbidities such as obesity and diabetes,6,7 as well as operative technique.8 -10 This includes injury of the vagus nerve causing gastric atony, resection of the duodenum causing changes in gastrointestinal hormones, division of gastric arteries or veins leading to ischemia of the stomach, pylorus preservation versus excision, and different techniques for anatomic reconstructions.11 -13 However, many of these operative related factors are not performed during DPR. In addition, other studies have demonstrated complications such as abscess, hemorrhage, and pancreatic fistula to be associated with DGE. 14 Despite this connection, there is still a substantial incidence of primary DGE, not associated with postoperative pancreatic fistula (POPF) or other post-operative complications.
This study aimed to evaluate the incidence of primary DGE in patients undergoing DPR and identify predictors of DGE in this population.
Methods
This retrospective study utilized the American College of Surgeons-National Surgery Quality Improvement Program (ACS-NSQIP) pancreas targeted database from 2014 to 2017. All patients undergoing DPR for pancreatic adenocarcinoma were identified. Patients with a documented POPF, defined in NSQIP as a drain amylase level three times the normal serum amylase level, were excluded from this study.
The primary outcome was incidence of primary DGE after DPR. DGE is defined in NSQIP by patients requiring a nasogastric tube (NGT) past postoperative day 7 or no oral intake past postoperative day 14. The ACS-NSQIP pancreas database does not grade DGE by the International Study Group of Pancreatic Surgery (ISGPS) definition so there was no differentiation made between ISGPS grades (A, B, and C) of DGE. We compared patients with DGE after DPR to those without DGE after DPR. The secondary aim was to define clinical metrics to classify patients as low and high risk for primary DGE after DPR. Other outcomes measured include demographic variables such as age, gender, and co-morbidities. Operative approach variables were obtained which include planned open, laparoscopic, laparoscopic with unplanned conversion to open, robotic, and robotic with unplanned conversion to open. Operative variables included: vascular resection (artery, vein, vein and artery, not performed), drain placement, number of days after surgery for drain removal, pancreatic duct size, and pancreatic gland texture.
Frequency statistics were performed for all available variables. A Student’s t-test or Mann-Whitney-U test was used to compare continuous variables, and chi-square was used to compare categorical variables for bivariate analysis. Continuous data were reported as medians with interquartile range or as means with standard deviation. Categorical data were reported as percentages.
To study the effects of various factors on the incidence of DGE after DPR we performed a Classification and Regression Trees (CART) method analysis. 15 CART analysis was used to compute a decision tree using the Gini splitting function. In short, this allows for an iterative process where the patient population is divided by outcome according to the variables input by the study authors. CART will output intermediate nodes, as well as terminal nodes which will demonstrate how many patients developed DGE and how many did not. In essence, CART analysis provides a set of significant predictors for a given outcome, in this case being DGE. However, in contrast to classic logistic regression analyses, which aim to provide a complete list of all significant predictors for a set outcome, CART provides the most clinically important variables.16,17 In order to reduce overfitting while building the tree, pruning in the training data was performed using minimum Cook’s D parameter. The minimum number of parent node cases was 40 while the minimum number of cases for the child nodes was set at 10. The maximum tree depth was set at 4. All analyses were performed with IBM SPSS Statistics for Windows (Version 24, IBM Corp., Armonk, NY).
Results
Demographics, Comorbidities, and Functional Status
A total of 1626 patients who underwent a DPR for pancreatic adenocarcinoma were identified. From this, 59 patients (3.6%) had DGE. Compared to patients without DGE, patients with DGE were of similar age (median, 69 vs 68-years-old, P = .56). When compared to patients without DGE, patients with DGE less commonly had diabetes mellitus (19% vs 31%, P = .042); however, the cohorts were similar in terms of all other comorbidities (all P > .05). In addition, both cohorts were similar in terms of functional status (Table 1).
Demographics of Patients Undergoing Distal Pancreatectomy With and Without Delayed Gastric Emptying.
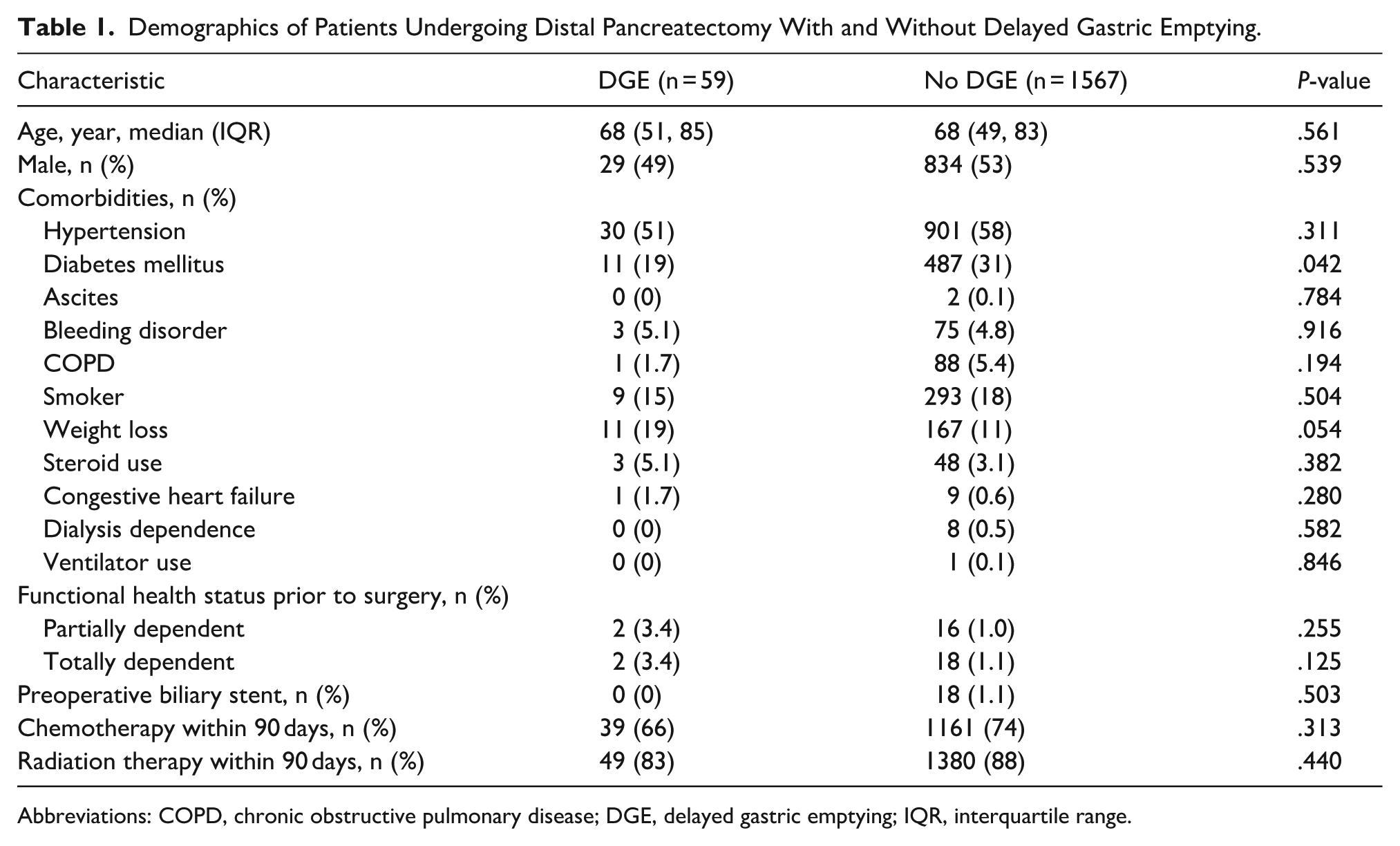
Abbreviations: COPD, chronic obstructive pulmonary disease; DGE, delayed gastric emptying; IQR, interquartile range.
Operative Characteristics and Outcomes
Patients who developed DGE after DPR more commonly had a pancreatic duct size <6 mm (17% vs 8%, P = .035) and had a vascular resection during their surgery (27% vs 12.1%, P = .015). Of the patients who developed DGE after DPR, 7% underwent arterial resection, 15% underwent venous resection, 5% had combined artery/vein resection, and 73% had no vascular resection performed (Table 2). Both cohorts had similar rates of hard, intermediate and soft pancreatic gland texture as well as use of a wound protector. Patients undergoing planned open DPR more commonly developed DGE compared to all other minimally invasive or hybrid surgery techniques (81% vs 62%, P = .002) (Table 2).
Operative Characteristics of Patients Undergoing Distal Pancreatectomy With and Without Delayed Gastric Emptying.
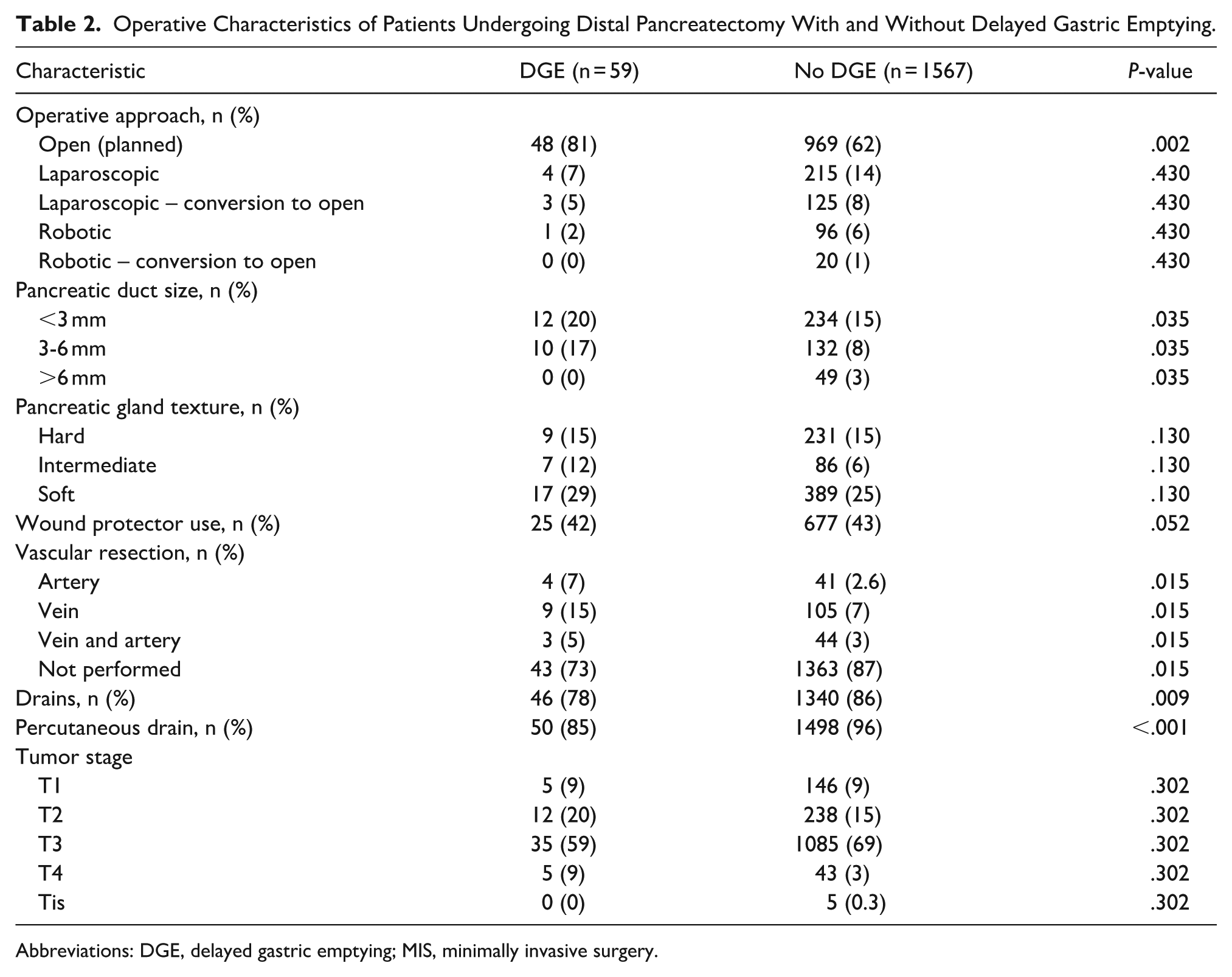
Abbreviations: DGE, delayed gastric emptying; MIS, minimally invasive surgery.
When compared to patients without DGE, patients with DGE after DPR had a longer length of stay (median, 15 vs 6 days, P < .001) and a higher rate of readmission (39% vs 12%, P < .001). Patients that developed DGE also had higher rates of 30-day complications including increased transfusions, organ surgical site infections, sepsis, unplanned intubation, ventilator past 48 hours, shock, pneumonia, and myocardial infarction (all P < .001). Patients with DGE after DPR also had increased risk of cardiac arrest with CPR (3% vs 0.5%, P = .005) and increased mortality (3% vs 0.7%, P = .023) when compared to patients without DGE (Table 3). It is also important to note that patients who underwent planned open surgery had an increased mortality rate when compared with patients undergoing a planned minimally invasive approach (1.3% vs 0.3%, P = .025).
Clinical Outcomes in Patients Undergoing Distal Pancreatic Resection With and Without Delayed Gastric Emptying.
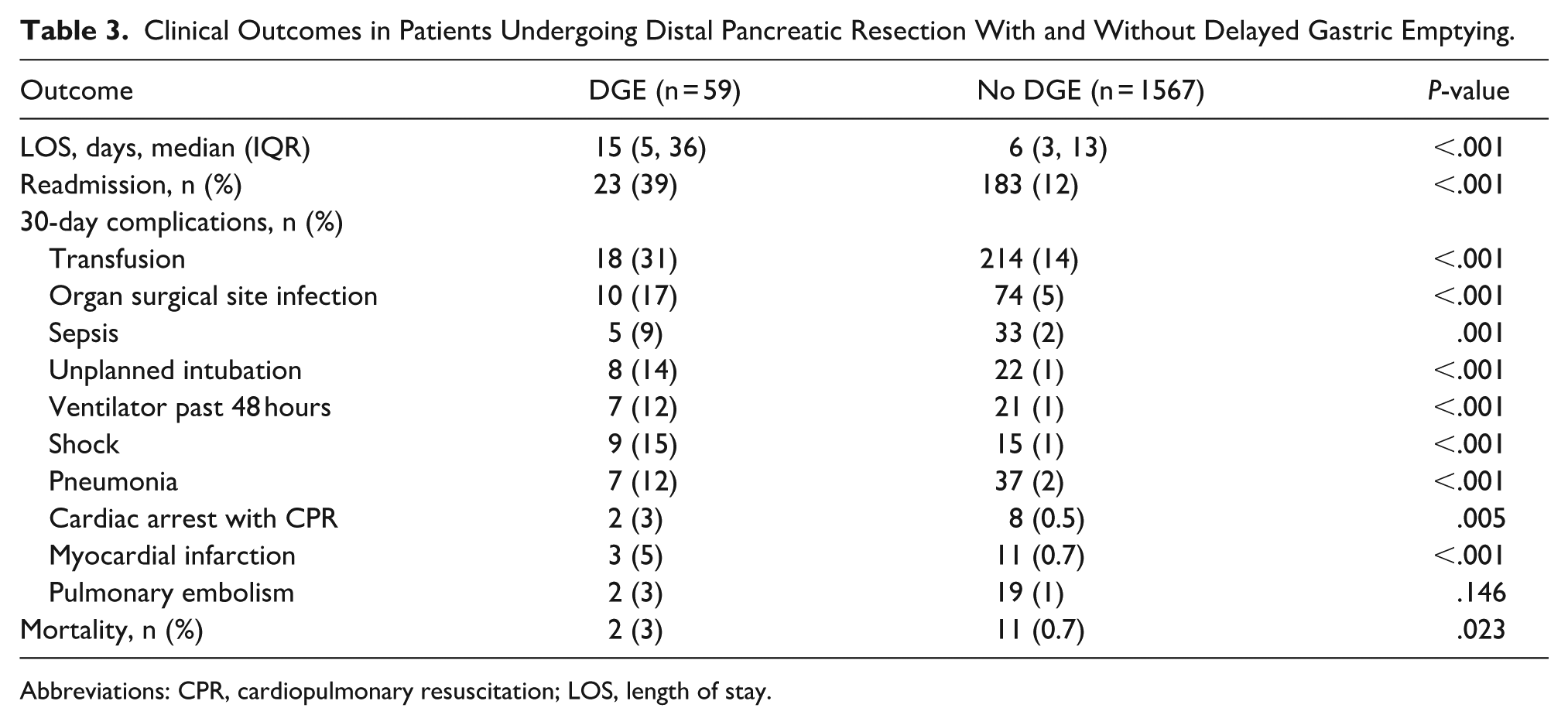
Abbreviations: CPR, cardiopulmonary resuscitation; LOS, length of stay.
Exploratory CART Analysis in Patients Undergoing DPR
On exploratory CART analysis, vascular resection and open surgery were predictors of DGE with a specificity of 98.3%. Patients requiring vascular resection had a 7.8% rate of DGE while patients without open surgery or vascular resection had a 1.8% rate of DGE. Comorbidities, preoperative chemotherapy/radiation, tumor staging, intraoperative drain placement, hypoalbuminemia or wound protector use were not found to be predictors of DGE (Figure 1).
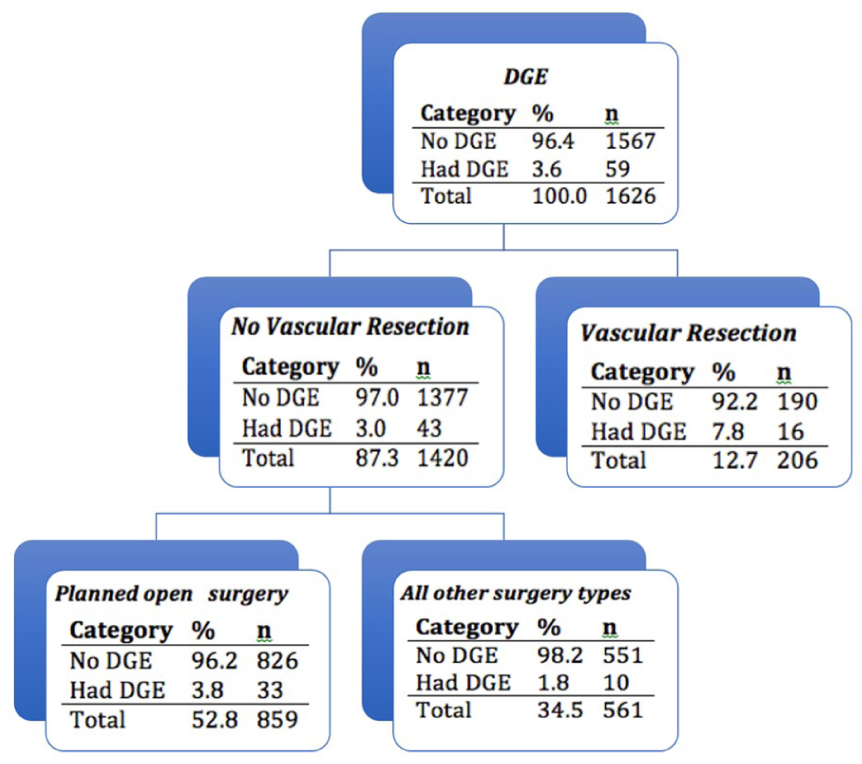
Classification and Regression Tree (CART) analysis showing predictors of delayed gastric emptying after distal pancreatectomy.
Discussion
Delayed gastric emptying is associated with significant morbidity and financial cost, with the majority of existing data focusing on outcomes related to pancreaticoduodenectomy. We found the incidence of DGE after DPR for patients not experiencing a POPF to be low, under 4%. In addition, the patients with DGE after DPR had a significantly longer hospital length of stay and an increased rate of mortality. Utilizing a CART analysis, planned open surgery and vascular resection were found to be predictors of DGE with a specificity of over 98%.
The majority of DPR are performed with minimally invasive techniques.18,19 This national analysis identified planned open DPR to be a predictor of DGE, which in turn is associated with increased length of stay. This is supported by previous prospective, multicenter studies on laparoscopic versus open distal pancreatectomy – for both benign and malignant lesions – which demonstrated prolonged hospital stays for patients with DGE after open DPR. 20 In further support, Zhou et al 21 demonstrated that there was significantly less DGE in the laparoscopic DPR cohort (1.3%) compared to open (28.7%). The underlying mechanism of DGE is poorly understood. Most hypotheses pertain to devascularization or denervation of the pylorus or duodenal resection causing decreased levels of plasma motilin after PD as possible triggers of DGE. 22 However, this would not explain the rates of DGE after DPR. Other hypotheses that may pertain to DPR include increased operative time, hormonal changes caused by surgical stress, and postoperative fluid volume status.23 -25 Minimally invasive technique for DPR may help minimize these risks via less surgical trauma and less perioperative fluid resuscitation.26 -28
Pancreatic surgery in general has a relatively high rate of requiring major vascular resection. In fact, locally advanced pancreatic cancer with vascular involvement accounts for 30% to 40% of all pancreatic cancer cases. 29 Pancreatic body tumors that involved the hepatic or celiac axis were once considered unresectable; however, resections are now being performed with increasing regularity. 30 Vascular resection in DPR was found to be a predictor of DGE. This may be related to extensive resections that could affect gastric blood supply and induce DGE.31 -33 Okada et al 32 found that in patients undergoing distal pancreatectomy with celiac axis resection (DP-CAR), resection of the left gastric artery was an independent risk factor for DGE. However, when the left gastric artery was preserved or reconstructed in DP-CAR, there was decreased incidence of DGE. 34
Prior to the ISPGS definition, reports on the incidence of DGE after DPR ranged from 0% to 18%. 35 More recent reports have stated an incidence of DGE after DPR between 9% and 56.5%, with a high rate of DGE grade A. 35 In these studies, the high incidence of DGE after DPR was often associated with a POPF, a known independent risk factor for secondary DGE. Furthermore, there is a lack of large multicenter studies evaluating primary DGE after DPR. However, single center studies by Glowka et al 35 and Noorani et al 36 identified the rate of DGE in DPR when controlling for pancreatic fistula to be 10% and 12.5% respectively. This current study, which is the largest and only multicenter study looking at primary DGE after DPR, demonstrated a much lower incidence of 3.6%. This may be related to varying definitions of DGE or low sample size in prior studies.
Limitations to this study include those inherent to a retrospective database analysis including misclassification and missing data, documentation of appropriate diagnosis and procedural codes, and reliance on the accuracy of the input of data. Furthermore, the ACS-NSQIP database is limited to data within 30 days of operation and thus does not have long-term outcomes. This database also lacks pertinent clinical information including specific treatments for DGE, the presence and impact of other intra-abdominal processes, multi-visceral resection during index surgery, hospital procedure volume, and surgeon procedure volume, some of which have been demonstrated to be associated with DGE. 37 Our study design utilized bivariate comparisons and a CART analysis rather than multivariable regression; therefore, statistical adjustment for covariates is limited, and potential confounding variables cannot be fully excluded – most importantly of which is the impact of planned open surgery versus laparoscopic surgery on outcomes. Despite these limitations, this is the largest, multicenter study looking at the incidence and risk factors for primary DGE in patients undergoing DPR without postoperative pancreatic fistula.
Conclusion
This large, nationwide, multicenter, retrospective database study found the rate of primary DGE in patients undergoing DPR without POPF to be much lower than previously reported. Patients who had DGE after DPR did have increased length of stay and mortality compared to patients without DGE. On CART analysis, vascular resection and open surgery were predictors of DGE after DPR with a specificity of over 98%. These findings may be utilized to counsel patients and take precautions in those at greater risk of developing DGE. Future research utilizing these and other known and novel predictors of DGE may help to develop a clinical scoring tool to stratify patients at risk for DGE after DPR.
Footnotes
Ethical Considerations
Ethical approval is not required for this manuscript.
Author Contributions
All authors made a substantial contribution to this work. AG, RW, ZJ, DI, JN, CV, SM, and BS were involved in idea conceptualization, data curation, formal analysis, and writing/review. SM, BS, JN, AG, and ZJ were involved in reviewing and editing of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Use of Artificial Intelligence
No artificial intelligence (AI) was used in the preparation of this manuscript.
