Abstract
Dissociative shutdown states occur when the individual encounters inescapable stress or trauma – or memories of inescapable stress or trauma. In the therapeutic space – occupational therapy, psychotherapy, or family therapy – working with shutdown states poses a clinical challenge. The individual’s loss of full awareness of what they are doing, or their loss of capacity to feel their body, to think, or to move or act, can bring the therapeutic process to a halt. Over the last half-century, body-oriented therapists working with the felt sense of the body, therapists working with patients presenting with complex trauma, and therapists working with patients with functional/dissociative seizures have introduced the use of grounding strategies to help patients maintain their connection with the body, self, close others, and the environment. This article explores the use of pickle juice (and other pungent foods) as a useful grounding strategy for managing dissociative shutdown states. Clinical examples are provided via vignettes. Also provided are a hypothesis and neurobiological model – the homeostatic sensory-reset hypothesis – as to why pickle juice and other pungent foods, which activate special sensory receptors in the gastrointestinal tract called transient receptor potential channels, help to disrupt and alleviate dissociation shutdown states.
Keywords
In the field of mental health, grounding refers to the feeling of awareness of, and connection to, our bodies, the environment, and the earth itself – being connected to the earth, being present in the here and now, having ‘not only our “feet on the ground” but our “minds on the ground”’ (p. 5) (Fisher, 1999; Koniver, 2023; Shuper Engelhard et al., 2021; Temple, 2018). ‘The sense of belonging, of having roots, [is] directly related to the feeling of intimate contact between the feet and the ground’ (p. 85) (Lowen, 1958). 1 Grounding interventions are activities that help the patient establish ‘an awareness of his legs and the feet on the ground on which he stands’ (p. 88) (Lowen, 1958). Grounding interventions help the individual feel more ‘solid, centred, balanced, contained or connected to the [self]—particularly to [the] body’ (Jackson, 2017; Schielke et al., 2023). Common interventions include the following: bringing ‘awareness to the legs and feet to increase the felt sense of a physical base of support’ (p. 325) (Ogden and Fisher, 2015; Paulsen and Golston, 2014); touching or rubbing parts of the body to stimulate sensation (University of Manchester, 2025); attention to the breath coupled with slowing of the breath (Goldstein, 2025; Kabat-Zinn, 1982); and using a range of taste, smell, auditory, tactile, or kinaesthetic sensations (Fisher, 1999; Frewen and Lanius, 2015; Paulsen and Golston, 2014) to increase sensory input, making the sensations of our bodies within the environment more noticeable (Chessell et al., 2019).
In non-Western traditions, grounding is an element of many ancient healing practices. It is a central, embedded element of the Chinese health-preservation practices known as daoyin, qigong, and tai chi (practiced either as exercises or as movement meditations) (Chen et al., 2019; Chinese Health Qigong Association, 2014; Smith and Carmone, 2022), and it is a core element of Indian yoga practices (Brown and Chevalier, 2015). By contrast, grounding interventions are a recent addition to Western clinical practice. They reflect a shift away from talking therapies – which prioritise language, mentalisation, and the use of cognitive top-down regulation strategies – to body-oriented therapies that work with felt sense of the body and that use a broad range of somatic interventions and bottom-up regulation strategies (Bloch-Atefi and Smith, 2015). The use of intense sensations has been integrated into dialectical behaviour therapy and sensory modulation interventions as an effective way of grounding patients, helping them to manage states of distress and high arousal, and providing an alternative to self-harm (Linehan, 2015; O’Sullivan and Fitzgibbon, 2018). The use of breathing interventions – embedded in meditation – has been integrated into stress-reduction and pain-management programs (e.g., mindfulness-based stress reduction [MBSR] and mindfulness-based pain management [MBPM]) (Kabat-Zinn, 1982; Pérez Fernández, Salaberria and Ocenda, 2022).
In the current article we discuss the use of pickle juice – and other pungent foods – as a grounding strategy for individuals who experience dissociative shutdown states, enabling them to manage these states in a proactive way and to maintain their connection with the body, self, close others, and the environment. We discuss the origins of the authors’ use of pickle juice as a grounding strategy (O’Sullivan and Fitzgibbon, 2018), and we provide vignettes as clinical examples. Finally, we propose a neurobiological model to support our hypothesis as to why pickle juice and other pungent foods help to disrupt and alleviate dissociative shutdown states – what we call the homeostatic sensory-reset hypothesis.
Scientific background
Dissociative shutdown states
Dissociative shutdown states occur when the individual encounters inescapable stress or trauma, or memories of inescapable stress or trauma (Kozlowska et al., 2015; Lanius et al., 2018). In the therapeutic space – occupational therapy, psychotherapy, or family therapy – working with shutdown states poses a significant clinical challenge. The individual’s loss of full awareness of what they are doing or the loss of capacity to feel their body, to think, or to move or act, brings the therapeutic process to a halt. The here-and-now connection between the patient and therapist is disrupted, as are the connections between the patient and family members. Sometimes the individual retains a memory of their subjective experience of the dissociative shutdown state, and sometimes they do not. For some, the body feels unreal or may be experienced as floating outside of the physical self (out-of-body experience). For others, the environment is experienced as unreal, dream-like, foggy, slowed down, or alien. For many, the experience of these states amplifies feelings such as the loss of control or connection with the outside world; a sense of powerlessness, helplessness, defectiveness, or defencelessness (accompanying the loss of movement and agency); a pervasive sense of emotional detachment; or paralysing fear. The sense of powerlessness to help or intervene or to connect with the individual when they are caught in that state – and do not seem to be reachable – may also be experienced by the therapist, partners, or other family members.
Tonic immobility, the prototype of the shutdown state, is a phylogenetically old defence response that occurs across many different species, including humans (Kozlowska et al., 2015). It involves a state of immobility (not being able to move), lowering of heart rate and arousal (the individual goes pale and feels cool), changes in sensory processing (loss of pain sensation), and a subjective sense of being numb, spacey, and disconnected from the self and here-and-now. Variations of this shutdown state are noted across different clinical settings. In the animal and human literature, a ‘collapsed’ version of tonic immobility – involving a loss of muscle tone – is described (Bracha, 2004; Kozlowska et al., 2015; Rivers, 1920). In the sexual assault literature, this shutdown state is called rape-induced paralysis (Foa and Rothbaum, 1998). In the trauma literature, the construct of peritraumatic reactions include symptoms of panic, dissociation, and sometimes tonic immobility (Coimbra et al., 2023; Rocha-Rego et al., 2009; Volchan et al., 2017). In the posttraumatic stress literature, a subset of individuals experience dissociative ‘shutdown’ symptoms – compromising consciousness, derealisation, depersonalisation, analgesia/anaesthesia, and tonic immobility – a PTSD subtype referred to as dissociative PTSD (Kearney and Lanius, 2022; Lanius et al., 2010; Nicholson et al., 2017). In the neurology and psychiatry literatures, dissociative shutdown states – presenting as zoning out, collapses, episodes of unresponsiveness – fall under the umbrella of functional/dissociative seizures (Hingray et al., 2025; Savage et al., 2022).
A growing body of work suggests that some dissociative shutdown states – tonic immobility and dissociative PTSD – involve a decrease in sensory information that reaches higher-level, somatosensory-information integration centres, coupled with decreased arousal (a change in the pattern of autonomic-system activation) and blunted processing in the amygdala (Kearney and Lanius, 2022; Kozlowska et al., 2015; Lanius et al., 2014; Schauer and Elbert, 2010). This low-arousal state is accompanied by the subjective absence of bodily sensations, an affective state of disconnection from the body, self, and environment, and the loss of motivation to act. Along similar lines, functional/dissociative seizures appear to involve disconnection (dissociation) between processing regions in the frontal and posterior cortical regions and between cortical and subcortical regions (Kozlowska and Scher, 2024; Lan et al., 2025; Madec et al., 2020). From a whole brain perspective, patients suffering from dissociative PTSD show distinct functional-connectivity patterns, reflecting decreased communication between some brain networks and increased communication between other brain networks (Harricharan et al., 2016; Lebois et al., 2022).
Grounding, and grounding strategies
In the last half-century, therapists using body-oriented therapies and working with felt sense of the body have begun using a range of grounding strategies (Lowen, 1958; Lowen, 1975) – sometimes referred to as ‘grounding and centering’ practices (p. 5) (Fisher, 1999) – in working with patients who experience dissociative shutdown states. In the phased approach to the treatment of dissociation, grounding interventions are embedded in the initial part of the intervention – the stabilisation phase (Herman, 1992; International Society for the Study of Trauma and Dissociation (ISSTD), 2011). Stabilisation work, which aims to contain traumatic symptoms and to stabilise the patient, precedes any attempt to engage in trauma work per se. The goal is to provide the patient with resources that they – together with the therapist – can use to support the patient ‘to be fully connected and aware of the present time and situation in both body and mind’ (p. 15) (Temple, 2018). Later in therapy, when traumatic material arises, the patient can implement the grounding resources to avoid overwhelm and the shift into dissociative shutdown. Clinical examples describing the utility of grounding strategies when working with patients who go into dissociative shutdown states have been described by therapists working from numerous therapy frameworks: somatic experiencing (vignette of Nancy, pp. 20–22 (Levine, 2010)), sensorimotor psychotherapy (vignettes of Victoria, p. 39; Mary, pp. 222–223; Sally, pp. 247 and 281 (Ogden et al., 2006); and Julie, p. 407, Chapter 19 (Ogden and Fisher, 2014)); phase-based therapy for the treatment of dissociative disorders (vignettes of Anna, John, Maria, and James (Goldstein, 2025)); and the treatment of dissociative PTSD (vignettes of ‘the wife’ and Marie, pp. 71–100 (Frewen and Lanius, 2015)).
Here we note that the broad range of grounding and centring interventions used by therapists in the clinic have their roots in ancient healing traditions without yet having the evidence base required by Western medicine. For example, slow-breathing practices come from ancient healing traditions and are utilised across contemporary therapeutic settings (Brown et al., 2013). Slow-breathing interventions work because ‘the neural networks regulating breathing and the neural networks regulating the autonomic nervous system (arousal) are coupled systems. They are located close to each other in the brain stem, and they work together in a synchronised way’ (p. 72) (Benarroch, 2007; Savage et al., 2022). Notwithstanding, the evidence base for breathing interventions as such is only just beginning to emerge (Bentley et al., 2023; Kabat-Zinn, 1982; Luo et al., 2025; Pérez Fernández et al., 2022), and the evidence base for various other grounding interventions is in its infancy (Chevalier et al., 2019; Park et al., 2025). That said, grounding interventions harness healing properties of slow breathing, movement, imagery, foods, spices and herbs, and perfumes and scents that have been part of various cultural traditions for centuries. They also have a low risk profile compared to other pharmacological and technical medical interventions.
Clinical curiosity in pickle juice as a grounding strategy
The first two authors (JO and CF) are mental health occupational therapists who have long used various intense sensory inputs (including pickle juice) to assist with grounding and to help patients manage episodes of dissociative shutdown (O’Sullivan and Fitzgibbon, 2018). It was only recently, in the context of helping a patient to manage persistent muscle cramps, that we took a careful look at the small body of literature on strategies to address muscle cramps (see Text Box 1). We noted that pickle juice, along with a variety of other pungent foods, was being used to help alleviate muscle cramps. The range of strong/intense taste inputs included vinegar flavours (pickle juice, yellow mustard), hot pepper, bitter flavours (e.g., tonic water), hot flavours (e.g., wasabi and horseradish), cinnamon, and ginger. Muscle cramps are an occupational hazard in sport, and it has long been recommended that they be managed with pickle juice. Many theories as to the aetiology of muscle cramping have been proposed: inherited abnormalities of substrate metabolism (‘metabolic theory’); fluid imbalance (‘dehydration theory’); imbalances of serum electrolyte concentrations (‘electrolyte theory’); extreme environmental conditions of heat or cold (‘environmental theory’); and sustained abnormal spinal reflex activity (‘abnormal neuromuscular control theory’) (Schwellnus et al., 1997). A 2009 literature review by Martin Schwellnus found that contemporary evidence did not support the electrolyte depletion and dehydration hypotheses and that evidence for the altered neuromuscular control, though supportive, was not yet compelling (Schwellnus, 2009). In 2009 and 2010, the American exercise physiologist Kevin Miller published two small studies (with 9 and 10 subjects, respectively) relating to the use of pickle juice for muscle cramps (Miller et al., 2010; Miller et al., 2009). In line with Schwellnus’s review, he found that muscle cramp cessation on drinking pickle juice was not due to any changes in plasma electrolyte concentrations, plasma osmolality, or plasma volume. He hypothesised that the response, rather than being the product of some chemical or metabolic change within the muscle, was a ‘neurally mediated reflex’ originating from the oropharyngeal region that inhibited the firing of alpha motor neurons (Miller et al., 2010). Bruce Bean and Rodderick MacKinnon – two American neuroscientists – commenced research into muscle cramps after their severe muscle cramps while kayaking had incapacitated them (leaving them unable to row) and put them into serious danger. Because specialised sensory receptors in cell membranes had been the focus of MacKinnon’s research (MacKinnon, 2003), the two researchers looked at the problem through that particular lens. In line with Miller et al. (2010), they hypothesised that muscle cramps have less to do with the muscle itself and more to do with hyperexcitability of the motor neurons (present in the spinal cord) that control the muscles. They hypothesised that the acetic acid in the pickle juice – and the chemical compounds in other pungent foods – stimulates discrete sensory receptors in the mouth, oesophagus, and stomach, known as transient receptor potential (TRP) channels or TRP receptors (Murray, 2016; The People’s Pharmacy, 2017). They further hypothesised that chemical stimulation of TRP channels by these pungent compounds activates sensory (or afferent) vagal fibres (fibres that carry information about viscera and homeostatic state to the brain), which, in turn, activate second-order neurones in the brain stem. The central action of these neurons changes the balance of descending transmitter input to the spinal cord (such as serotonin and norepinephrine), reducing the hyperexcitability of alpha motor neurons that causes cramping (Bruce Bean, Personal Communication, 7 January 2025). They applied this hypothesis to develop a palatable beverage containing ingredients that activate TRP channels, to be used for alleviating cramp pain (Futterman, 2016; Murray, 2016). Unfortunately, they did not publish their experiments, not realising that their hypothesis and discoveries could have implications beyond that of muscle cramps.Text Box 1: The Muscle Cramp Literature Pertaining to the Use of Pickle Juice and Other Pungent Foods
Because of pickle juice’s intense/pungent flavour profile and its reported clinical benefit in relieving muscle cramps, we (JO and CF) started to wonder whether the hypothesised mechanism by which pickle juice – and other pungent foods – resolved muscle cramps (see Text Box 1) could also help to stop episodes of dissociative shutdown. We and our patients began to experiment using pickle juice as a grounding strategy for dissociative shutdown states, with significant clinical success. In time, we contacted our co-authors (PC and KK) to discuss these clinical findings – which marked the beginning of our collaboration.
Vignettes demonstrating the use of pickle juice and other pungent foods when working with patients with dissociative shutdown states
In this section we offer vignettes to describe the use of pickle juice – and other pungent foods – as part of the clinical intervention for dissociative shutdown states.
Vignette 1
A 14-year-old girl developed PTSD following a serious car accident. At the first anniversary of the accident, she began to experience an increase in dissociative shutdown symptoms in response to trauma triggers. After discussing with her therapist the role of intense sensations as a grounding strategy for dissociative symptoms, she decided to trial using pickle juice. She found that pickle juice worked immediately – as long as she used it quickly on noticing her warning signs (a feeling of zoning out coupled with a band of pain across her forehead). Following ingestion, she experienced a ceasing of the dissociation process and a feeling of connection to her body in the present moment. She then used additional grounding interventions (pushing her feet into the ground) and slow breathing to deepen her sense of being grounded and calm. She took some pickles in her lunch box to school, and when going out, carried a tiny bottle filled with pickle juice to use in other settings. She continued to use the pickles (and pickle juice) as an effective strategy for stopping the dissociation. The success in managing the dissociative episodes gave her a new sense of control and mastery, increasing her motivation to attend school and engage in further therapy to address other aspects of her PTSD.
Vignette 2
A 55-year-old man with a diagnosis of complex PTSD presented with recurrent episodes of dissociation that lasted several hours, during which he experienced a significant loss of time. These episodes involved feelings of coldness and detachment, and were often accompanied by intense rumination of traumatic memories. The patient found that slowly eating a single pickled onion helped him regain a sense of grounding and reorient to the present moment, effectively interrupting the ruminative thoughts. To manage his dissociative episodes, he used a timer on his watch, reminding him to consume pickled onions at regular intervals, sometimes as frequently as every hour, to maintain his sense of presence and keep the dissociative episodes at bay. The intervention helped the man regain a sense of control, resulting in a noticeable decrease in other PTSD-related symptoms, including anxiety and difficulty concentrating. It also increased his confidence and ability to engage more in meaningful activities outside of his home environment (including going for walks to his local park) and helped him slowly attempt to interact more with people in the community, including one of his neighbours.
Vignette 3
A 29-year-old woman immigrant from Iraq, with a long-standing history of chronic pain, began experiencing functional/dissociative seizures – episodes of sudden collapse – which she found distressing and socially embarrassing. These episodes often occurred in public spaces: the patient would regain consciousness to find herself surrounded by concerned bystanders, with emergency services having been called.
Through self-monitoring, the woman identified that her functional/dissociative seizures were more frequent when she was exposed to bright lights and experiencing stress brought on by the anticipation of leaving the house. This led to increased avoidance behaviours, which limited her ability to engage in daily activities outside her home.
The woman sought therapy. Her therapist introduced a multifaceted intervention approach with strategies incorporating the following. – Wearing dark sunglasses in bright environments to minimise sensory overstimulation – Using grounding strategies – intense sensory input – to interrupt the functional/dissociative-seizure process
For the grounding strategy to be effective, the chosen stimuli needed to be intense enough to disrupt the functional/dissociative seizures but not aversive to the point of distress. The woman expressed a preference for using intense sensory experiences that were culturally relevant and familiar. She trialled the following. – Consuming mustard before leaving the house to increase grounding and alertness, and to prevent dissociation and a functional/dissociative seizure – Taking vinegar in a little bottle that fit into her handbag as a portable sensory input for when she was outside the home – Maintaining access to pickled onions as an emergency intervention, to be consumed as soon as she noticed the warning signs of a functional/dissociative seizure
Over time, consistent use of these strategies resulted in the complete cessation of functional/dissociative seizures, allowing the woman to regain confidence in leaving her home and engaging in daily life.
Vignette 4
A 25-year-old woman presented with a complex mental health history characterised by depression and dissociation that had worsened over the past year. She had a history of childhood sexual abuse and a sexual assault at age 19. Eye-movement desensitisation and reprocessing (EMDR) therapy with a previous therapist had successfully helped her process many trauma-related memories, but she continued to experience dissociation during sexual intimacy.
The young woman had recently begun a relationship with a supportive and gentle partner but found that during sexual activity, she would disconnect from her body and experience time loss. She expressed a desire to remain present and fully engage in intimacy without dissociation.
The woman sought support from her therapist, who introduced several strategies to enhance bodily awareness and communication during intimacy. These included the use of a nonverbal cue (a predetermined gesture) to signal when to pause or slow down, as well as structured discussions with her partner to establish a sense of safety and mutual understanding. Additionally, the patient was interested in incorporating a sensory-modulation strategy to help her remain grounded and present during intimate experiences. With the guidance of the therapist, the patient and her partner explored potential options: lemon juice, chili, and mint mouthwash. The patient ultimately found that using mint mouthwash before and during intimacy effectively helped her remain present and grounded and fully engage in the experience.
Clinical recommendations
When patients are interested in trying pickle juice – and other pungent foods – as a grounding strategy, we recommend the following. – Medical clearance by a medical practitioner. In the case of functional/dissociative seizures, a formal neurology workup and formal diagnosis of functional/dissociative seizures by a neurologist is essential. In patients with potential medical contraindications such as allergies or fluid or salt restrictions, clearance by a medical practitioner is strongly advised. – Patient-therapist collaboration and use of a trauma informed approach. All sensory-modulation strategies – including grounding strategies for dissociative shutdown states – are trialled in the context of a positive therapeutic relationship and trauma-informed principles of safety, trust, collaboration, empowerment, choice, and cultural responsiveness. This foundation allows the patient to explore a variety of grounding options in a safe context and in a curious or playful manner. For some patients – particularly for children – involvement of family or other significant persons or pets can also be valuable. As part of this trial-and-error process, it may be important to explain to the patient that liking the intense sensation is not necessary for the strategy to be effective. If the sensation becomes aversive or triggers reminders of trauma, however, alternative strategies need to be considered. In sum, collaboration, supported exploration, and provision of choice help ensure that the approaches selected are safe, appropriate, individualised, and meaningful (SAIM) for the person (O’Sullivan and Fitzgibbon, 2018) – yielding a toolkit of effective approaches. – Implementation and reminders. If patients find benefit in using a strategy, it is important to determine how they will remember to use it (e.g., by establishing prompts). Additionally, practical considerations should be discussed, such as how the strategy can be implemented in different settings (e.g., at home vs. in the community). – Holistic (biopsychosocial) approach. The use of pickle juice – or other pungent foods – for managing dissociative symptoms is not a stand-alone intervention. The strategy provides a rapid form of grounding when patients find themselves destabilised and prone to entering a dissociative shutdown state. It is embedded in the broader holistic (biopsychosocial) treatment intervention that enables the patient to attain improvement or recovery from PTSD, functional/dissociative seizures, or other dissociative presentations (International Society for the Study of Trauma and Dissociation (ISSTD), 2011; Norman et al., 2023; Paulsen and Golston, 2014; Savage et al., 2022).
The homeostatic sensory-reset hypothesis: Pickle juice and other pungent flavours for the treatment of dissociation
In this section, we present our hypothesis that pickle juice and other pungent flavours may interrupt episodes of dissociative shutdown by resetting brain interoceptive/homeostatic systems and brain networks that mediate dissociative shutdown states. Our homeostatic sensory-reset hypothesis builds upon the work of Bruce Bean and Roderick MacKinnon, who hypothesised that pickle juice – and other chemical compounds found in pungent foods – stimulates discrete sensory receptors in the mouth, oesophagus, and stomach, known as transient receptor potential (TRP) channels or TRP receptors (see Text Box 1). It also builds upon our previous analysis of tonic and collapsed immobility as part of the defence cascade (Kozlowska et al., 2015). Co-author (and neuroscientist/anatomist) PC has played a central role in moving beyond the hypothesis itself to identify potential neural pathways and mechanisms by which the reset may occur. This hypothesis and its neurobiological support are included here as a first step in developing the evidence base regarding an observed but yet-to-be-understood clinical phenomenon – the capacity of pickle juice and other pungent flavours to counter dissociative shutdown.
What is known about transient receptor potential channels
TRP channels are transmembrane ion channels that act as sensors for a wide variety of stimuli in the environment. When activated by a specific stimulus, these specialised proteins lead to the activation of sensory nerves of the somatic nervous system (which carries information from muscles and skin to the brain) and the autonomic nervous system (which carries information from visceral organs inside the body, including the gastrointestinal tract, to the brain). In the current article, we narrow our focus to TRP channels in the gastrointestinal tract because these are the ones that are activated in response to pickle juice and other pungent foods.
Within the gastrointestinal system, TRP channels are found in the mouth, oesophagus, stomach, intestine, and colon (Houghton et al., 2020; Yu et al., 2016). They are activated by sensory stimuli such as pain, temperature, noxious stimuli, acid, inflammation, and natural food products such as acetic acid (in pickle juice and many other fermented food products), citric acid (in lemons and limes), capsaicin (in hot peppers), gingerols (in ginger), allicin (in garlic), menthol (in mint leaves and candies), cinnamaldehyde (in cinnamon), quinine (in tonic water), and isothiocyanate compounds (in wasabi, horseradish, and mustard oil) (Tominaga, 2007; Vriens et al., 2008). When activated, TRP channels open up to let ions go through the membrane, which induces a change in the cell membrane potential (the difference of electrical charge between the inside and the outside of the cell). These changes, in turn, trigger action potentials that propagate along sensory nerves (e.g., spinal nerves or the vagal nerve). These sensory nerves (called first-order sensory nerves) are typically slow-conducting fibres, and usually unmyelinated. There are two sets of first-order sensory nerves.
One set of first-order sensory nerves terminates in the dorsal horn of the spinal cord (Craig, 2016; Yu et al., 2016), where local reflexes (e.g., withdrawal reflex) may be activated. The sensory information is also relayed to second-order sensory neurons located in lamina I. Their axons, in turn, ascend to the brain, forming the spinothalamic tract (a track running in the spinal cord toward the brain). These ascending axons send branches that terminate in relay centres located in the brain stem (reticular formation, parabrachial nucleus, periaqueductal grey) and thalamus, where they can be integrated with other input to modulate gradually more complex behavioural and autonomic responses. The sensory information can finally reach the sensory cortex as well as other regions such as the hypothalamus, insular cortex, and limbic system, which are high level integration centres regulating homeostatic functions and more (Craig, 2016). In this way TRP channels can feed into multiple neural circuits within the central nervous system.
The other set of first-order sensory nerves activated by TRP channels enters the central nervous system at brain stem level via cranial nerves (Craig, 2005; Craig, 2016). They are the trigeminal nerve for somatic sensory inputs (including the oral cavity) and the facial, glossopharyngeal, and vagal nerves for autonomic sensory inputs (including the pharynx, oesophagus, stomach, and intestinal tract). They relay in the brain stem on second-order neurons located in the spinal trigeminal nucleus (somatic sensory) and nucleus of the tractus solitarius (autonomic sensory), which are the equivalent of the dorsal horn of the spinal cord at the level of the brain stem. The axons of these second-order neurons join those coming from the spinal cord via the spinothalamic tract to target the same relay and integrating centres described above: brain stem, hypothalamus, insular cortex, and limbic system.
Hypothesised modulation of somatosensory integration centres in the brain
Sensory integration in the relay centres mentioned above occurs in a hierarchical fashion. The higher they are, the more information they integrate. Importantly, both somatic and autonomic stimuli from TRP channels or others can converge on these centres to modulate both somatic and autonomic motor output, starting from brain stem levels. It is because of this anatomical organisation that Bruce Bean and Rodderick MacKinnon hypothesised that pickle juice in the gastrointestinal tract activated TRP channels, causing sensory information to reach control centres in the spinal cord, brain stem, and forebrain, presumably resulting in top-down modulation, which dampened the excitability of motor neurons innervating the muscles, thereby reducing the experience of cramping (see Figure 1) (see Text Box 1). Schematic representation of the central pathways involved in the homeostatic sensory-reset system. The upper panel (A) shows these pathways on a side view of a stylised mammalian brain. In black are the descending pathways connecting brain, brain stem, and spinal cord structures to some of the peripheral organs involved in interoception and homeostatic regulation. In blue are the ascending sensory pathways that are activated by transient receptor potential channels (TRPs) in the gastrointestinal tract and the skin. They target and modulate all structures of the descending pathways from the medulla to the hypothalamus, limbic system, and insular cortex. The bottom panel (B) is a block diagram showing the same descending and ascending pathways.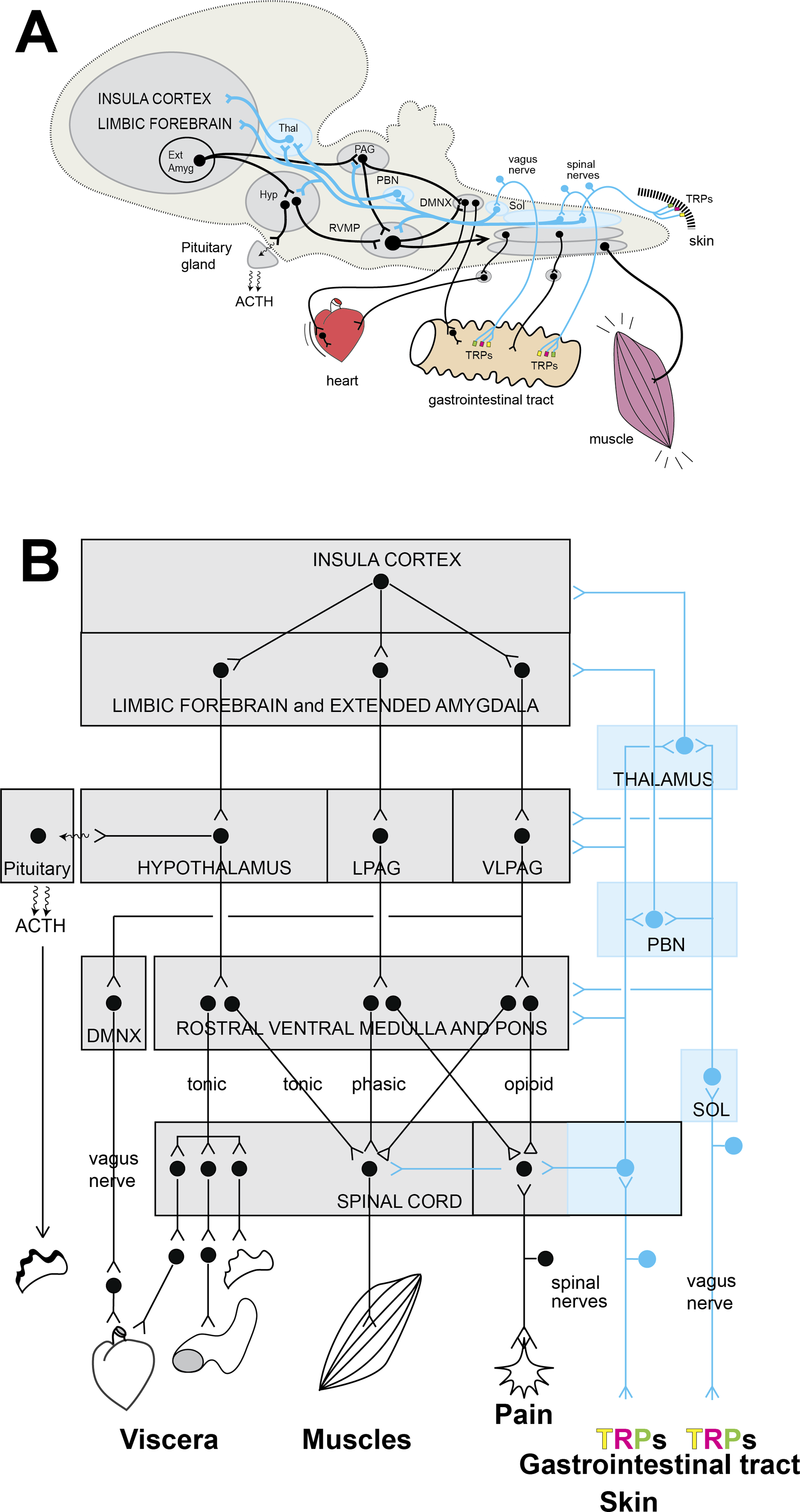
Given the above, we propose the homeostatic sensory-reset hypothesis to explain how the use of pickle juice can induce grounding. We propose that pickle juice and other natural substances with specific intense flavours activate certain types of TRP channels in the mouth, oesophagus, and stomach that carry sensory information – information that is then processed via the brain’s interoceptive/homeostatic system described by Bud Craig (see Figure 1) (Craig, 2005; Craig, 2016). This sensory input from gastrointestinal TRP channels functions to override the decrease in sensory information that reaches higher-level somatosensory information integration centres in dissociative shutdown states (see introduction), resetting the central circuitry that modulates processing within the homeostatic system. In brief, this input feeds into the brain’s interoceptive/homeostatic system, activates it, and resets the system and associated neural networks in a way that supports, once again, the individual’s subjective sense of connection to the body, emotional self, and environment.
Testing the homeostatic sensory-reset hypothesis
The homeostatic sensory-reset hypothesis is a hypothesis that, as such, needs to be tested both at the clinical level (in clinical trials) and at the neuroscience level (with regard to the hypothesised mechanisms). Notwithstanding, based on our knowledge of neuroanatomy – and the broader neuroscience research pertaining to dissociation – we have presented proposed pathways via which pickle juice and other pungent foods may activate and reset the interoceptive/homeostatic system. However, the question as to ‘what exactly is reset’ and ‘at what level of the nervous system’ has yet to unpacked. Does the reset occur at the level of first-order neurons and second-order neurons – thereby overriding the decrease of sensory information reaching integration centres in shutdown dissociative states? Or does the reset occur at higher integrating centres, such as the brain stem or the thalamus, or at the level of brain networks (Harricharan et al., 2016; Lebois et al., 2022), resetting them to a more normative pattern? Or does the reset work at multiple levels of the interoceptive/homeostatic hierarchy? All these questions are yet to be answered and require further consideration in future research.
Conclusion
In this article, we have discussed the use of pickle juice – and other pungent foods – as a clinically useful grounding strategy when working with patients who experience dissociative shutdown states. Once the effectiveness of pickle juice – or another pungent food – has been established by the patient, the therapist can then continue to cultivate confidence in the strategy to foster the patient’s growing sense of control and mastery in managing dissociative symptoms. While further clinical trials to explore this new intervention are warranted, it offers even now a safe and cost-effective option to address a common, distressing clinical phenomenon. Pungent flavours provide the patient with an additional grounding strategy for inclusion in their toolbox of useful grounding strategies (Schielke et al., 2023).
This article has also examined the hypothesised neurobiological mechanisms underlying the use of pickle juice and other pungent flavours to effectively manage dissociative shutdown states. While the underlying neurobiology may not be of interest to everyone, it is of substantive relevance and importance in the broader arenas of evidenced-based medicine and neuroscience.
Footnotes
Acknowledgements
We thank our patients for the opportunity to work together to trial the clinical effectiveness of pickle juice and other TRP channel activators to manage episodes of dissociation. Of the vignettes in the article, the majority are amalgams from the authors’ clinical practices (vignettes 1, 3, and 4). Vignettes 2 is from a patient who kindly gave consent to be included in this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
