Abstract
Reconstruction of post traumatic facial soft tissue defect remains a challenge. The reconstruction of nasal substructures with the locoregional flap is been practiced since the times of Sushruta. But still the quest for ideal reconstructive option is in pipeline. We present a case of posttraumatic nasal alar defect with superiorly based interpolated nasolabial flap. The postoperative outcomes were very encouraging.
Introduction
Soft tissue injuries are among the most common injury reporting to emergency department. Maxillofacial soft tissue injury either isolated or with combined other injuries accounts for 10% of injuries amongst them. Repairing traumatic orofacial injury, especially nasal defect, is a challenging task because of complicated facial anatomy and matching contour and skin of the nose according to tissue defect becomes an even more demanding task. Nasolabial flap (NLF) being a simple and easily available flap with less complication for small intraoral and extraoral tissue defects is now prioritized. NLF is one of the ancient flaps for reconstruction of facial soft tissue defects and was first described in 600 BC by an Indian surgeon Sushruta. 1
NLF utilizes skin reservoir lateral to nasolabial fold and results in a minimal inconspicuous scar. Pectoralis major flap, radial forearm flap, and anterolateral thigh flap need expertise followed by significant morbidity at the donor site and are bulky for the small facial defect. In comparison to these flaps, nasolabial requires less skill, and leads to less morbidity at the donor site with uneventful and even better healing. The need for general anesthesia is another drawback of other facial flap as NLF can be performed under local anesthesia. 2
Anatomical Consideration
The NLF receives vascular supply basically from the angular artery (a branch of a facial artery), the infraorbital artery (a branch of the maxillary artery), and the transverse facial artery (a branch of a superficial temporal artery). Although the main supply of the flap is a facial artery, a dense vascular anastomosis between these branches gives this flap excellent post-operative success and can be used diversely for the reconstruction of lips, anterior floor of the mouth, nose alar rim, and tip.
NLF is a versatile flap and is ideal for small to moderate intraoral and extraoral defect 1 . Defect of size up to 2 × 3 cm can be reconstructed with unilateral NLF, whereas bilateral NLF can cover defect up to 5 × 5 cm2. Because of adequate blood supply to the flap, it allows flap’s length to breadth ratio of 3:1. 2 NLF can be utilized as a random flap although it’s an axial flap. Depending on the requirement, NLF can be medially, laterally, superiorly, or inferiorly based flap. NLF can also be utilized as an interpolated flap that we did in this case.
Case Report
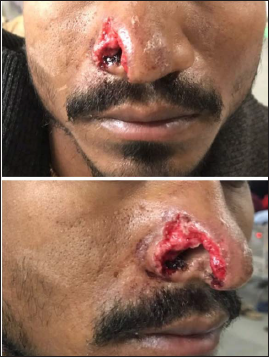
A 17 years male reported at our institute with a chief complaint of being chopped off the right side of his nose due to physical assault. On clinical examination, a raw abraded area was observed on the right lateral nose region with loss of alar of nose and defect of size 2 × 3 cm approximately. The defect does not cross midline (Figure 1).
Right sided Nasal Alar defect in front and lateral view.
Surgical Procedure
The patient was prepared for reconstruction under general anesthesia. The patient was painted and draped and dead skin and debris were scraped off to induce fresh bleeding. The defect was measured and the right side NLF was measured and marked accordingly lateral to the nasolabial fold keeping the distal end rounded to adapt to the defect (Figure 2). The superiorly based subcutaneous NLF was raised taking care of adequate thickness with rich vascular supply on the other hand. NLF was carefully adapted and interpolated to the site of the defect for reconstruction. Double-layered closure was done with vicryl 3.0 and prolene 4.0. With help of blunt dissection and laxity of the skin around the donor site, primary single-layered closure was done with prolene 4.0 after achieving hemostasis (Figure 3).
Marking of Superiorly based Nasolabial Flap for Alar reconstruction.
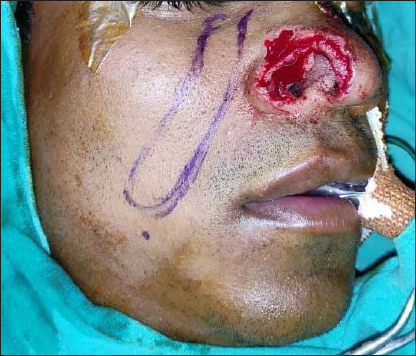
Immediate post-operative photograph showing donor & recipient site closure.
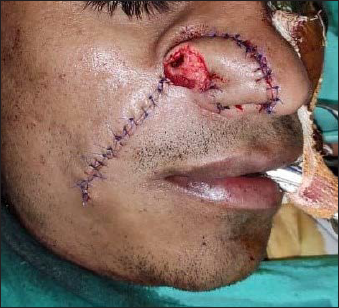
The patient was recalled for follow-up for revision of the flap after 1 week. The patient reported after 3 weeks post NLF reconstruction surgery (Figure 4). Sutures were removed and disjunction of the flap was done followed by mild debulking and primary closure with prolene 4.0. The patient was asked to report after a week for suture removal.
Post operative 3 week photograph showing uptake of NLF.
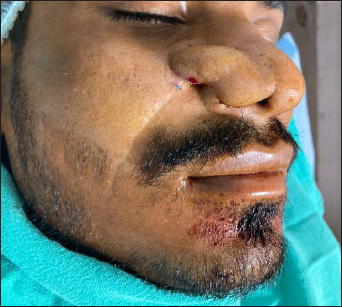
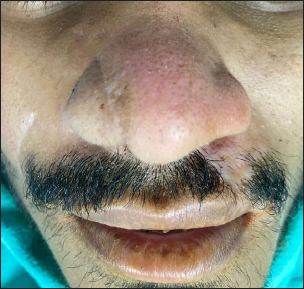
Patient reported after one week with satisfactory healing and contour (Figure 5). Suture removal was done and the patient was further planned for debulking on the nasal cavity aspect.
Satisfactory esthetics and alar contour 4 weeks post operatively.
Discussion
Alar rim defect reconstruction is a tough job due to its minimal mobility and single subunit structure of ala. 3 There are various reasons for nasal defects such as trauma, tumor resection, or infective etiology. There is a plethora of reconstruction options for alar rim defects according to the dimensions of the defect such as primary repair, skin graft, paramedian forehead flap, auricular graft, and septal mucosal flap. However, repairing a full-thickness alar rim defect has limited options. Paramedian forehead flap and septal mucoperichondrial sometimes serve as a good option for reconstruction of alar defects; however, they are technique sensitive. 4 Para median forehead flap has been widely used in nasal defect reconstruction but the main disadvantage of this flap is that it results in donor site scar mainly in the Asian race.
One of the versatile flaps used in the reconstruction of the lateral wall of the nose, ala, the columella is a NLF due to the laxity of the cheek. Spear et al and Kroll et al described the modified application of NLF for the reconstruction of full-thickness nasal defects. 5 Spear et al gave a twist to NLF to repair ala. 5 There are various kinds of NLF used to reconstruct alar defects such as propeller type, subcutaneous pedicled, and transposition type NLF. Durgeon et al advocated and popularized propeller type NLF for full thickness alar region defects.6, 7 Transpositional NLF is mainly advocated in case of alar defects extending to rim and sidewalls. The technique to employ transpositional NLF is simple and quick as we have seen in this case report. Trimming and thinning of raised NLF can be done to allow better incorporation. The distal end of the trimmed NLF can be turned over itself or covered cartilaginous graft to achieve the reconstruction of the full-thickness alar defect. One of the main concerns around transpositional NLF are the scars that reach out sidewalls and disfigurement of the alar region. In the case of transpositional NLF secondary procedures may be required to thin the flap and form the groove between the alar region and sidewalls. In the case of subcutaneous pedicled NLF, it is mainly used in alar defects which do not have lost cartilage. Various factors should be taken into consideration in the planning of subcutaneous pedicled NLF such as the turning point of the flap, the arc of rotation, and the length of the pedicle. 8
In spite of being popular and versatile, NLF has few complications. Trap door deformity, alar distortion, and venous congestion are the main complications associated with NLF. Trapdoor deformity is mainly associated with subcutaneous pedicled NLF used for alar rim defect or tip reconstruction, whereas alar distortion is one of the most common complications associated with transpositional and propeller type NLF. Surgeon inexperience and poor planning often lead to alar distortion. Venous congestion can be associated with all types of NLF. Kinking of pedicle and tight tunnels can be a possible explanation for venous congestion. 8
Conclusion
With our experience, we conclude that NLF serves as a simple, effective, and safe choice for small to medium size alar region defects with minimal donor site morbidity. NLF in spite of having few complications has proven to be a reliable and less technique-sensitive alternative as compared to other flaps.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent and Ethical Approval
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for images and other clinical information to be reported in the journal. The patient understands that his name and/or initials will not be published and due efforts will be made to conceal the identity, but anonymity cannot be guaranteed.
