Abstract
Abstract
Advanced oral surgery such as the treatment of fractures of the mandible is difficult to be performed in rural and remote settings. Within India, the bulk of the population reside in the countryside rather than in urban settings, leading to a lack of provision of secondary care services. Within the Chitrakoot Project, a modern, fully equipped dental surgery has evolved, which with the assistance of Indian specialists from secondary care, and visitors from abroad, has become a rural clinic capable of treating mandibular fractures using maxillomandibular fixation.
The concept of training for remote and rural dental surgeons is explored, and three cases are chronicled. The experience in Chitrakoot is something which could be usefully rolled out to suitable rural surgeons to receive training in teaching hospitals, which would improve the provision of acute oral surgery within the rural population of India, and other countries.
Introduction
While oral trauma care in Indian cities is typically performed by specialist practitioners who have followed a recognized training program, 1 the vast majority of population in India still live in remote and rural areas which are often far from secondary care centers. Indeed, according to United Nations statistics, while in 2017, 83.14% of the population of the UK live in cities, the figure for India is only 33.6%. 2
One such rural area of India surrounds the town of Chitrakoot (population 35,000), which is situated on the Madhya Pradesh–Uttar Pradesh border. Secondary care assistance for the treatment of facial and dental trauma is unavailable locally, the major center being in the King George Medical University (KGMU) in Lucknow, some 8 h away.
In 1990, Chitrakoot became a center for the Deendayal Research Institute 3 , created by Nanaji Deshmukh to look after the development and sustainability of 500 tribal villages in Madhya Pradesh and Uttar Pradesh regions (Deendayal Research Institute, Chitrakoot). In 1998, some UK dentists, inspired by the selfless philosophy of Nanaji, formed the Chitrakoot Project UK, Healthcare Charity, 4 and set up a dental clinic and mobile unit to bring modern dental treatment to the population of this remote area.
While the fledgling dental unit addressed many of the issues such as restorative, pediatric dentistry, and minor oral surgery in the rural setting, the significant issues of oral cancer which are common in the region due to gutka chewing 5 and trauma proved beyond the limits of locally available treatment. The Maxillofacial Department at the KGMU stepped in to assist by receiving oral cancer referrals, and gave one of the Chitrakoot Dentists (Varun Gupta) training in fracture reduction and treatment using maxillomandibular fixation (MMF).
The clinic in Chitrakoot has treated around 140,000 patients since its inception, with around 30,000 being treated free of charge, while others paying fees as per their ability to pay. It also has a successful mobile unit which has performed over 600 visits to remote tribal villages offering screening and basic treatment. The center has installed a fully functioning operating theatre, and in the past 12 years visiting plastic surgeons have treated nearly 500 cases, mainly in cases of burns and cleft palate.
Methods
This study gives an overview of the treatment protocols that have been developed within the dental unit at Chitrakoot and gives a retrospective study history of 3 recent jaw fracture cases. Later, some recommendations are made for setting training standards in education for suitable practitioners who practice in remote and rural areas.
At present, the treatment of choice in Chitrakoot is MMF, although the development of the use of bone plating with open reduction and internal fixation is now available, as the resident dental surgeon has been recently given further training at the KGMU.
The fractures were classified as per Pogrel and Kaban. 6
Results
As an evolutionary process, the protocols used in the Chitrakoot clinic have developed into a standardized procedure with high success rate. In the past 12 years, the clinic in Chitrakoot has treated around 400 mandibular fractures with a wide range of etiology, exhibiting the whole range of sites both in single and multiple locations.
Three recent representative cases are as follows:
Case 1
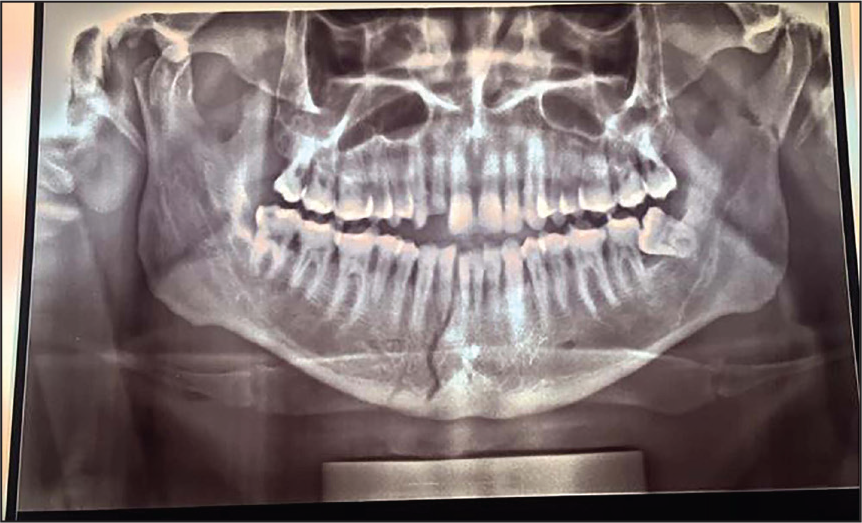
35-year-old male came from a place 35 km away from Chitrakoot. Met with a road accident with a bicycle. The patient was coming back from the farm and because of wet clay stuck on the tire the bike slipped on the road. Other injuries: laceration was present on face. Fractured right side parasymphysis, right side condyle, and left side neck of condyle. Right side Pogrel and Kaban classes 1 and 5 and left side class 1. The patient delayed attending until 7 days after accident. Radiological examination: dental panoramic tomogram (DPT) (Figure 1). MMF was performed (Figure 2). Chlorhexidine mouthwash prescribed and dietary advice given. No postoperative complications existed. MMF was removed after 45 days. The patient was advised to use localized physiotherapy to jaw musculature.
Case 2
A14-year-old male living 40 km from Chitrakoot. Met with a road accident. The patient was riding a bike with his brother when a motor vehicle hit the bike. Soft tissue laceration present on chin. Fractured right side parasymphysis. Right side Pogrel and Kaban class 5. The patient was attended 2 days after trauma. Radiological examination: DPT. MMF was performed. Chlorhexidine mouthwash prescribed and dietary advice given. No postoperative complications existed. MMF was removed after 45 days. Patient advised to use localized physiotherapy to jaw musculature.
Case 3
MG.
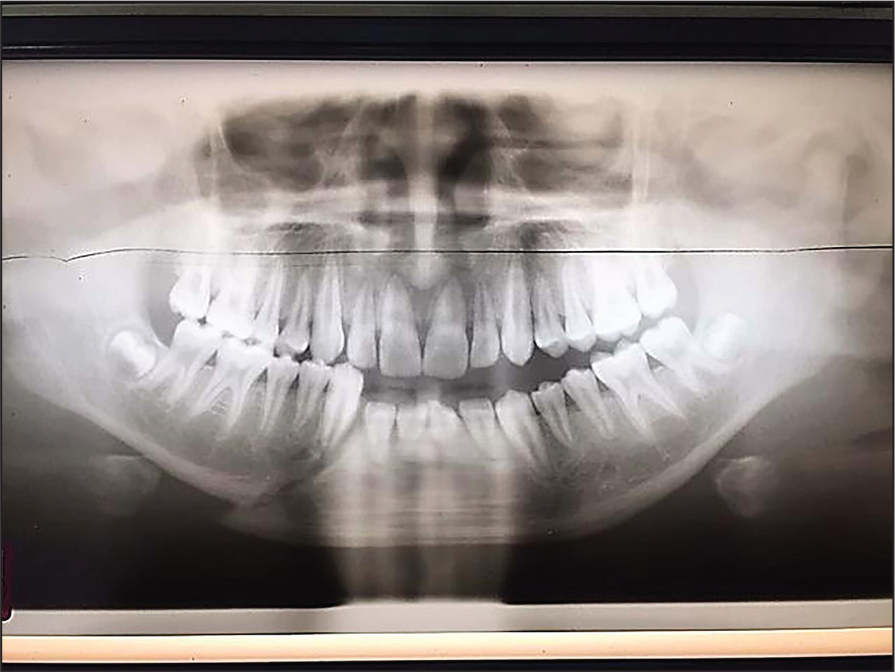
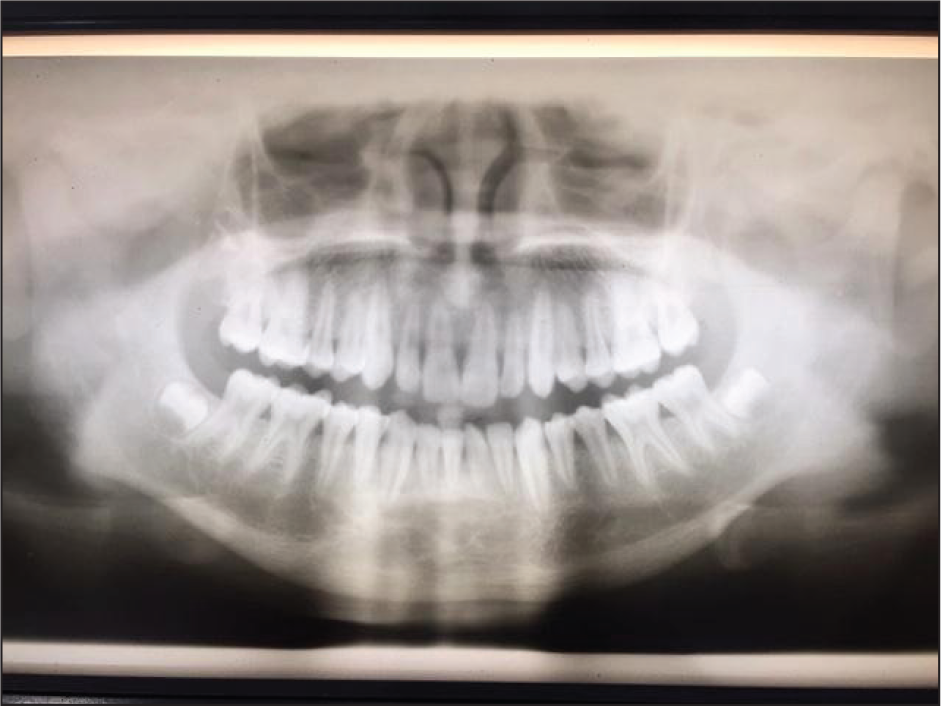
A 30-year-old male living 5 km from Chitrakoot. Met with a road traffic accident. Suffered from no other injuries. Fractured symphysis and left side neck of condyle. Right side Pogrel and Kaban class 5, left side class 1. Atttended 4 hours after the accident. Radiological examination: DPT (Figure 3). Initial emergency treatment performed 4 hours after the injury, with wire splinting of lower incisor teeth. Patient re-evaluated after 14 days, and full MMF placed. Advised chlorhexidine mouthwash and postoperative dietary advice. No postoperative complications were noted. MMF was removed after 45 days (Figure 4). The patient was advised to use localized physiotherapy to jaw musculature.
With the obvious gaps in the provision of appropriate care for jaw fractures in rural Indian locations, it should be a priority for teaching hospitals to identify competent rural practitioners and to offer a postgraduate training to them for this purpose. A proposed teaching program for rural practitioners providing treatment for mandibular fractures in a rural setting might include the following:
Surgical Anatomy. A course on the soft and hard tissues relating to the mid and lower third of the facial skeleton. Along with the relevant osteology, this should also include details of the relevant neurological, muscular, and vascular structures. Physiology. A course on the physiology of bone and soft tissue healing. Assessment. The candidate should be skilled in the ability to make a holistic assessment of the patient, who may have other injuries related to the trauma which may be life-threatening. An understanding of maintenance of the airway is essential. The practitioner should have a full understanding of the physical and radiological principles of assessment of mandibular fractures. An understanding of surgical limitations of the practitioner for complex cases, and an awareness of Le Fort middle third facial fractures and their emergency treatment implications should be given. Treatment strategies. The candidate should be trained in the principles of aseptic surgery and be capable of assessing and reducing mandibular fractures using interdental wiring. They should be competent in pain management, and effective wound debridement. Initial training for interdental wiring could be done using a phantom head course before exposure to a patient. They should be competent in suturing technique and in understanding the principles of wound closure. The candidate should have an understanding of restoring the occlusion with the wiring strategy. Postoperative care. The candidate should be conversant with all necessary instructions for the patient in terms of hygiene, pain relief, and nutritional issues. They should apply their understanding of tissue healing times to the timing of removal of sutures and of fixation wiring. They should understand the need for postremoval assessment of the occlusion. Appropriate treatment of bacterial infection and sepsis should be understood.
Discussion
While the tenet of “Do No Harm” applies to all patients, dental surgeons operating in remote and rural areas are often faced with the dilemma of “to treat” or “not to treat.” In many cases, rural practitioners are forced to undertake treatment well beyond their comfort zone, as if they do not attempt to give a primary care treatment, the patient’s condition would significantly deteriorate. Ideally, patients should always have access to specialist centers, but in countries such as India this is clearly not always possible, and a surgeon sometimes has to push his/her skill envelope to the limit to provide immediate care.
There are many classifications for fractures of the mandible, 7 but for this study, we opted for the relatively simple method described by Pogrel and Kaban. 6
There are a wide variety of mandibular fracture sites, but in a series of 600 mandibular fractures, Oikarinen and Malmstrom 8 reported single fractures in 49.1% of cases, two fractures in 39.9%, three fractures in 9.4%, four fractures in 1.2%, and more than four fractures corresponding to 0.2% of cases.
In the experience of the Chitrakoot clinic, the etiology of jaw fractures is variable, ranging from bicycle accidents, farming accidents to the rare causes such as gunshot wounds. Road accidents are the most common cause of mandibular trauma in the area, mainly relating to bicycles. The often variable condition of road surfaces, the unpredictable behavior of roadside animals such as free-roaming cows, poor cycle maintenance, and lack of cycle helmet use 9 all contribute to such accidents.
The use of interdental wiring by MMF is a simple, easily managed option, and the technique can be simply taught and the materials used are relatively inexpensive. MMF can be performed in surgeries without the use of general anesthesia, which is more difficult to achieve when bone plating is being used. There is a case for teaching suitably trained and experienced practitioners bone plating techniques, and lifting their skill sets to a higher level. In a remote and rural setting, bone plating would benefit patients travelling long distances to attend the clinic and would help to circumvent some of the eating and nutritional issues that are difficult after interdental wiring. Also, there is a higher incidence of ankylosis of the temporomandibular joint in condylar fracture cases reduced in by MMF. 10
As well as good visual and tactile assessment skills, palpating the injured sites and looking for acquired occlusal abnormalities, and radiological examination are essential. For radiological examinations of these patients, the DPT is the recommended initial screening tool. 11 The operator should be aware of the possible dimensional distortions in the resulting films, and the need for good patient positioning. 12 A posteroanterior mandible view is also of use for diagnosis. Ideally, further radiographs such as 3-dimensional tomographic views should be taken of the site, 13 but such examinations are rarely available in rural clinics. Before the installation of the DPT in Chitrakoot, most of the fracture evaluations were acquired using a standard medical X-ray machine providing lateral oblique views, but the interpretation of these can be problematical. 14 For surgeons without access to extraoral radiography, careful examination of injured sites using occlusal and periapical intraoral radiographs will in many cases suffice, although acquiring such images may be difficult in fracture cases. It must be remembered that 2-dimensional radiography may lead to missing fractures in the line of the X-ray beam, and supplementary views from differing angles might be needed to clarify the areas of concern. In an ideal situation, the use of cone-beam computed tomography might be indicated, but these machines are largely outwith the remit of most rural and remote surgeries.
The surgeon should also be vigilant to assess other areas such as the zygomatic bones and the maxilla, and if concerned seek advice.
The rural practitioner should be versed in the principles of life support. While the need for an advanced trauma life support approach 15 is desirable for trauma cases, the rural practitioner should be at least competent in the basics of trauma support. A good source of information can be found in the Resident Manual of Trauma to the Face, Head and Neck 16 which is published as a downloadable e-book from the American Academy of Otolaryngology, Head and Neck Surgery Foundation of the USA.
When assessing the occlusion as part of a treatment protocol, it must be remembered that 20% of the population have an existing malocclusion. 17
The use of a telemedicine service 18 should be encouraged, with good links to a major trauma center, allowing a two-way exchange of information. For this, however, a suitable Internet connection would be necessary, and this would certainly be a limiting factor for many remote clinics.
Conclusion
The population demographics in a country such as India make remote health care a challenging subject. Injuries such as jaw fractures can be debilitating to the patient concerned and can have significant impact on their abilities to lead a normal working life. The undergraduate curriculum in India has to be seen as a starting point for the dental career, and the journey onward has to be supplemented with further education. For dentists in remote and rural locations, this process can be challenging. It would be a major improvement if these difficulties were recognized at the national level and further education programs were established to develop the skills needed by these practitioners. A teaching program of relevant oral surgery and an efficient telemedicine service would not only increase the skills base of the rural dentists but also provide a great service to the vast rural population within the country.
A Preoperative Dental Panoramic Tomogram (DPT) Radiograph Showing the Parasympheseal Mandibular Fracture in Case 2
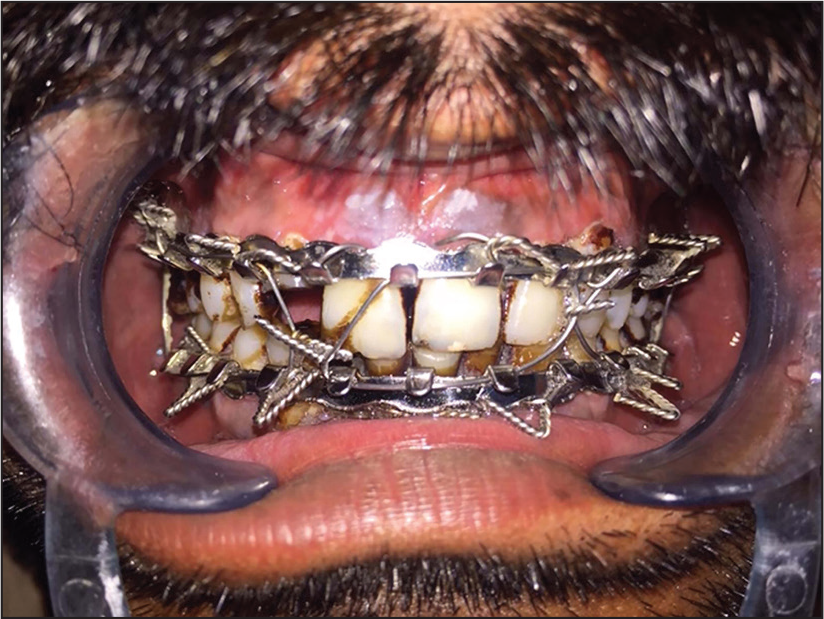
Maxillomandibular Fixation (MMF) Treatment to Case 2
A Preoperative Dental Panoramic Tomogram (DPT) of Case 3, Showing Fracture and Displacement
A Postoperative Dental Panoramic Tomogram (DPT) of Case 3, Showing Healed Site and Realignment of Occlusion
Footnotes
Acknowledgments
The authors would like to thank Professor Shadab Mohammad and his departmental staff at King George Medical University for their continuing help and support, and Mr Rory Morrison, Consultant Oral and Maxillofacial Surgeon at Aberdeen Royal Infirmary, for his input and editing of the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
