Abstract
Various molecular triggers define heterogeneous subsets of gastrointestinal stromal tumors (GISTs), differing in clinical behavior and drug sensitivity. KIT/PDGFRA-wild-type GISTs, including those succinate dehydrogenase (SDH)-deficient, are overall unresponsive to the tyrosine kinase inhibitors commonly used, fostering the development of specific alternative therapeutic strategies. Epigenetic inactivation of O6-methylguanine-DNA methyltransferase (MGMT) through promoter methylation leads to effectiveness of alkylating agents in several human cancers. SDH-deficient GISTs typically feature widespread DNA methylation. However, the actual occurrence of MGMT methylation in these tumors, potentially predisposing them to respond to alkylating drugs, has not been investigated so far. Here we discuss the recent findings concerning the occurrence of MGMT methylation in different GIST subgroups, including SDH-deficient ones, as a premise for a possible reappraisal of alkylating agents specifically targeting these small, otherwise overall chemorefractory, GIST subgroups.
Keywords
Introduction
Following decades during which gastrointestinal stromal tumors (GISTs) were not identified as an independent entity due to the lack of proper diagnostic tools, the groundbreaking discovery of the pivotal role of receptor tyrosine kinase KIT, both as molecular trigger and diagnostic marker in these tumors, allowed GISTs to be separated from smooth muscle tumors and other mesenchymal neoplasms. 1 Shortly after, the tyrosine kinase inhibitor (TKI) imatinib proved to be dramatically active in a patient affected by unresectable metastatic GIST, 2 paving the way for the approval of this drug for treating GIST in record time. However, it was clear, within a short time, that not all GISTs respond to imatinib and that imatinib-responsive tumors eventually develop secondary resistance. In addition, over the years, GIST triggers alternative to KIT have been progressively discovered, and, increasingly, rare molecular defects are still being detected. 3 For these reasons, several drugs alternative to imatinib have been tested with the aim of overcoming imatinib resistance, either primary or secondary, in GIST (for reference, a list of drugs considered for the treatment of GIST, including their mechanisms of action, is presented in Table 1). However, coherent with the epoch of the studies, past GIST clinical trials often suffered from the lack of a proper selection of cases on the one hand, and uncommon GIST subsets, possibly ignored at the time of the referred trials, were barely represented among the tested patients on the other. This fact possibly disguised the activity of experimental drugs, which were ineffective on most of the GISTs, on rare GIST types.
Main classes of drugs considered in GIST treatment.
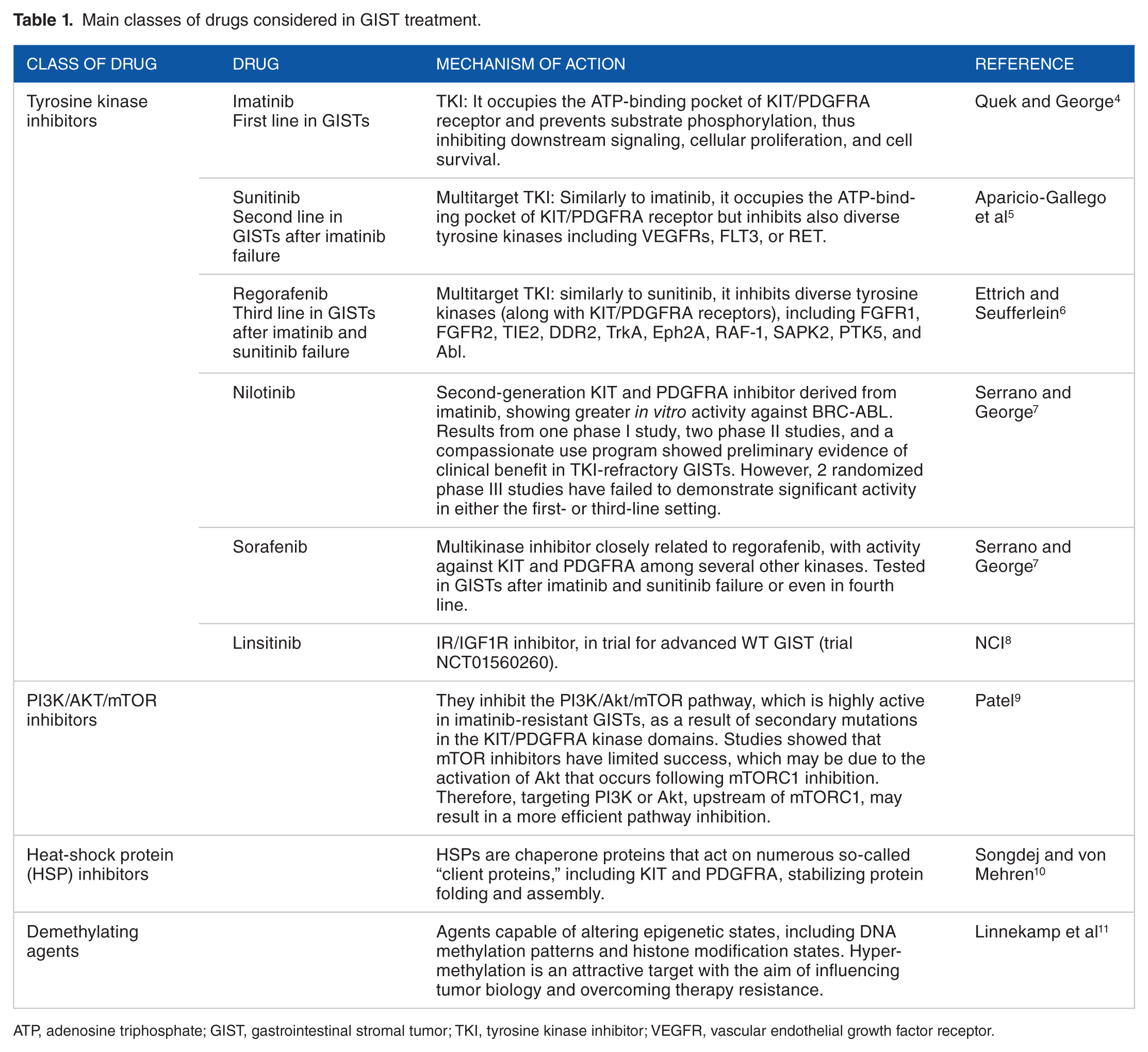
ATP, adenosine triphosphate; GIST, gastrointestinal stromal tumor; TKI, tyrosine kinase inhibitor; VEGFR, vascular endothelial growth factor receptor.
Succinate-Dehydrogenase-Deficient GISTs: Let Sleeping Dogs Lie
Succinate dehydrogenase (SDH)-deficient GISTs are rare, accounting for about 5% of GISTs as a whole. Their tumorigenesis hinges on either genomic or epigenetic defects of the heterotetrameric SDH complex, which participates in the Krebs cycle. These defects lead to succinate accumulation, which inhibits prolyl-hydroxylase and TET DNA-hydroxylases, causing hypoxia-inducible factor 1-α (HIF1-α) accumulation and impairment of the conversion of 5-methylcytosine to 5-hydroxymethylcytosine, respectively. These 2 events are oncogenic, on the one hand, through nuclear translocation and induced transcription of through tumorigenic genes by HIF1-α, and, on the other hindrance of DNA demethylation, ultimately leading to widespread DNA methylation.12,13 Clinically, SDH-deficient GISTs are often indolent, even though relatively often displaying metastases, likely because of their metabolic handicap secondary to SDH deficit. Metastases may present as late as 42 years after primary tumors. However, some cases are fatal in a few years, and accumulating data from increasingly extended follow-ups seem to indicate an overall mortality rate as high as 15%. 14 In case of clinically aggressive SDH-deficient GISTs, the room for maneuver currently offered to the oncologist is rather limited, as these tumors are usually unresponsive to the TKI therapies commonly used.15,16
State-of-the-Art of Therapy of SDH-Deficient and Other KIT/PDGFRA-Wild-Type GISTs: Bogs and Quicksand
Satisfactory clinical research on pure populations of SDH-deficient GISTs is rare because these tumors are uncommon and their identification is relatively recent.1,17 These events, in conjunction with the commonly extremely slow growth of these tumors, make it very difficult to collect significant data concerning not only the deceptive biology of SDH-deficient GISTs, but also their response to drugs, as time lapses of apparent disease stability could be independent of the latter’s effect. 18 Data on SDH-deficient GISTs have been therefore often inferred from cohorts of KIT/PDGFRA-wild-type (WT) GISTs, which are enriched in the former tumors. KIT/PDGFRA-WT GISTs as a whole constitute a pathogenetically heterogeneous subset accounting for about 10% to 15% of GISTs, which, similarly to SDH-deficient GISTs when taken separately, combine an overall indolent behavior with unresponsiveness to the commonly employed TKI in malignant cases.15,16 Based on the biology of these tumors, drugs of potential interest for their treatment include linsitinib, PI3K/AKT/mTOR inhibitors, nilotinib, sorafenib, heat-shock protein inhibitors, chemicals targeting HIF1-α, and demethylating agents. 19 Furthermore, different studies have recently shown that epigenetic modifications may represent alternative mechanisms to evade the pharmacologic response.20–22 The growing importance of epigenetics in cancer development has been recently recognized by the European Society of Medical Oncology (ESMO), which included it among the new horizons of soft tissue sarcoma and GIST research (ESMO Sarcoma and GIST Symposium 2018). 23 In this context, different trials are evaluating epigenetic therapies as modulators of drug resistance in solid tumors. 22 Regarding GIST, in recent years, epigenetic treatments have been proposed as alternative treatments to develop in the future, to bypass TKIs’ resistance.24,25 However, results are still at an early stage and further research will be pivotal in this novel field. In the current landscape, in which a clearly effective therapy for SDH-deficient GISTs is lacking, regorafenib and sunitinib might constitute possible exceptions.18,26
Alkylating Agents’ Ineffectiveness in GISTs: A “Bona Fide” Misdirection?
Over the years, SDH-deficient GISTs have been extensively characterized from a genetic and an epigenetic point of view, 14 and a wealth of evidence has markedly corroborated that SDH-deficient GISTs are deeply different from KIT/PDGFRA mutant GISTs. Among the distinguishing features of SDH-deficient GISTs, widespread DNA methylation is the most evident.12,13 SDH-deficient GISTs show a general hypermethylation, which, in turn, promotes the loss of expression of different proteins. The impaired activity of O6-methylguanine-DNA methyltransferase (MGMT) due to promoter methylation allows the effective employment of alkylating agents in human glioma, colorectal cancer, and diffuse large B cell lymphoma.19,27 Given these premises, the hypothesis that DNA methylation could affect MGMT in SDH-deficient GISTs, thereby predisposing them to respond to alkylating agents, appears reasonable. However, does existing evidence support it? Following reports on MGMT in GISTs, which did not consider SDH status,28–31 MGMT methylation and MGMT expression were recently studied for the first time in SDH-deficient GISTs, comparing them with other pathogenetic GIST subsets. Consistent with the above-mentioned expectations, SDH-deficient GISTs were significantly enriched in MGMT-methylated cases, which, in turn, displayed loss of MGMT protein expression, as detected by immunohistochemistry. KIT/PDGFRA-WT GISTs were significantly MGMT-methylated as well; but, unlike SDH-deficient GISTs, this result was not indicated by any particular theoretic premise, except the consideration that SDH-deficient GISTs are the largest, pathogenetically characterized subset of KIT/PDGFRA-WT GISTs, thereby significantly influencing the features of the latter tumors when globally considered. Conversely, MGMT methylation turned out to be a relatively rare event among KIT/PDGFRA mutant GISTs (i.e., the vast majority of GISTs 19 ; Figure 1). Therefore, although confirmatory studies on larger GIST series are warranted, it is most likely that not only SDH-deficient GISTs, but also KIT/PDGFRA-WT ones as a whole (i.e., GISTs commonly resistant to canonical TKIs) often bear an inactivated MGMT, a feature potentially permissive for the efficacy of alkylating agents. What has been the clinical outcome of alkylating agents in GISTs? To the best of our knowledge, the latter approach has been tested in a total of 36 GISTs, enrolled in trials studying temozolomide and carmustine in heterogeneous sarcomas, with negative results.30,32,33 However, these GISTs were neither selected by genotype nor, coherent with the time of the studies, selected and/or investigated for SDH. In addition, the only 2 cases in which MGMT was studied revealed baseline activity, without verifying its residual function after administering its inactivating substrate, O6-benzylguanine. 33 On top of that, none of these trials employed Choi criteria, the most sensitive method for assessing GIST response to therapy. 34 Therefore, the possible efficacy of alkylating agents in a predisposed fraction of GISTs could have escaped detection due to the lack of a proper case selection added to the rarity of these potentially predisposed tumors and to suboptimal criteria for evaluating tumor response.

Approximate distribution of MGMT methylation in GISTs, according to pathogenetic type. The pie chart illustrates the distribution of GISTs according to the molecular trigger. 1 The shaded area, representing GISTs featuring MGMT methylation, involves about two thirds of SDH-deficient GISTs, one fifth of NF1-associated GISTs, two fifths of the other KIT/PDGFRA-WT GISTs, and slightly more than one twentieth of KIT mutant GISTs; no MGMT-methylated cases have been reported so far among PDGFRA mutant GISTs.
Future Perspectives
The presented reasoning justified the reappraisal of alkylating agents in GIST therapy to the point that a phase II trial investigating temozolomide in metastatic SDH-deficient GIST was recently launched and is currently underway (ClinicalTrials.gov/NCT03556384). In case of positive results, an important new therapeutic approach will be available to oncologists, further expanding the efficacy of GIST treatment.
Footnotes
Funding:
This work was supported by grants from the Università Cattolica del Sacro Cuore (Linea D1 grants nos R4124500212 and R4124500331) to R.R.
Declaration of conflicting interests:
R.R. received speaker’s honoraria from Novartis. G.R. declares no conflicts of interest.
Author Contributions
GR and RR wrote and revised the manuscript.
