Abstract
X-linked retinoschisis (XLRS) is an inherited retinal degeneration affecting males, characterized by splitting of the retinal layers. We herein present the outcomes of surgical treatment in a case of XLRS complicated by rhegmatogenous retinal detachment (RRD). A 22-year-old male presented to the emergency department due to decreased visual acuity and visual field defect in his left eye Oculus Sinister (OS) of 1 week duration. The patient reported an early onset retinal degeneration and decreased visual acuity in both eyes since childhood in his past ocular history. Upon presentation, best corrected visual acuity (BCVA) was 6/30 on the right eye Oculus Dexter (OD) and 6/120 OS. Fundus examination revealed areas of peripheral retinal schisis, and the characteristic spoke wheel pattern on the macula of both eyes. In OS, a temporal RRD involving the macula was identified. The patient underwent surgical treatment with pars plana vitrectomy with internal limiting membrane (ILM) peeling, endolaser, and silicone oil (SO) tamponade. BCVA in OS improved to 6/60 and schistic cavities resolution was observed in the immediate postoperative period. The patient’s BCVA further improved to 6/19 at 1 month, as foveal anatomy showed relative improvement. However, there was a rapid reappearance of schisis spaces in the macular area at this point, which was also followed by progressive deterioration of foveal schisis by 3 months post-operatively. The resorption and recurrence of lamellar macular schisis changes after ILM peel and presence of SO, highlights that although XLRS findings can temporarily improve upon surgical intervention, the pathogenetic mechanisms contributing to disease phenotype remain to be elucidated.
Introduction
X-linked retinoschisis (XLRS) constitutes the most common form of juvenile macular degeneration in males and is typically diagnosed during childhood or preadolescence due to early visual impairment. Its prevalence is estimated between 1 in 25,000 and 1 in 5000. 1 A variety of mutations in the RS1 gene (located on the Xp22.1 chromosome) are responsible for XLRS. RS1 gene encodes retinoschisin, a protein expressed in the retina predominantly in photoreceptors and bipolar cells, necessary for normal retinal cell adhesion, organization, and interaction. 2
The vast majority of XLRS patients exhibit maculopathy of a radial striae morphology due to foveal schisis whose persistence may lead to atrophy. Peripheral schisis is present in 50% of XLRS patients. 3 A decrease in b-to-a wave amplitude ratio is a typical finding in the full field electroretinogram. Vitreous hemorrhage is the most frequent complication, while 5–20% of XLRS cases progress to retinal detachment. 4
While no established medical treatment is available to date for XLRS, pars plana vitrectomy (PPV) with gas or silicone oil (SO) has been employed in complicated and progressive cases of XLRS with promising results, attributable to removal of the traction associated with the presence of intact vitreous in this young population of patients.5,6
We hereby describe an interesting case of XLRS complicated with rhegmatogenous retinal detachment (RRD) treated for with PPV and SO demonstrating a rapid recurrence of foveal and macular schisis in the presence of SO.
Case presentation
A 22-year-old male presented to the Ophthalmology Emergency Department of the University Hospital of Patras in September 2022 complaining of sudden deterioration of vision in his left eye of 1 week duration. His past ocular history (POH) included decreased visual acuity in both eyes since childhood due to an early onset retinal degeneration. During ophthalmic evaluation, his best corrected visual acuity (BCVA) was 6/30 in the right eye (OD) and 6/120 in the left (OS). Anterior segment examination was unremarkable. Dilated fundus examination revealed a large peripheral retinal schisis cavity and vitreous veils as well as the typical spoke wheel pattern in the macula in OD and similar fundus findings as well as macula involving RRD in the inferotemporal retina (from 2 to 8 clock hours) in the presence of two adjacent retinal breaks in the 4th clock hour in OS (Figure 1). Spectral domain optical coherence tomography (SD-OCT) demonstrated schistic macular edema in both eyes with large schistic cavities extending from the inner plexiform (IPL) to the outer plexiform layers (OPL) [Figure 2(a) and (b)]. Detachment of the temporal half of the macula was also evident in SD-OCT in OS [Figure 2(b)]. Based on the phenotype and the POH, the diagnosis of XLRS, complicated by a RRD in the left eye, was set. The patient and relatives refused any genetic testing for personal reasons.
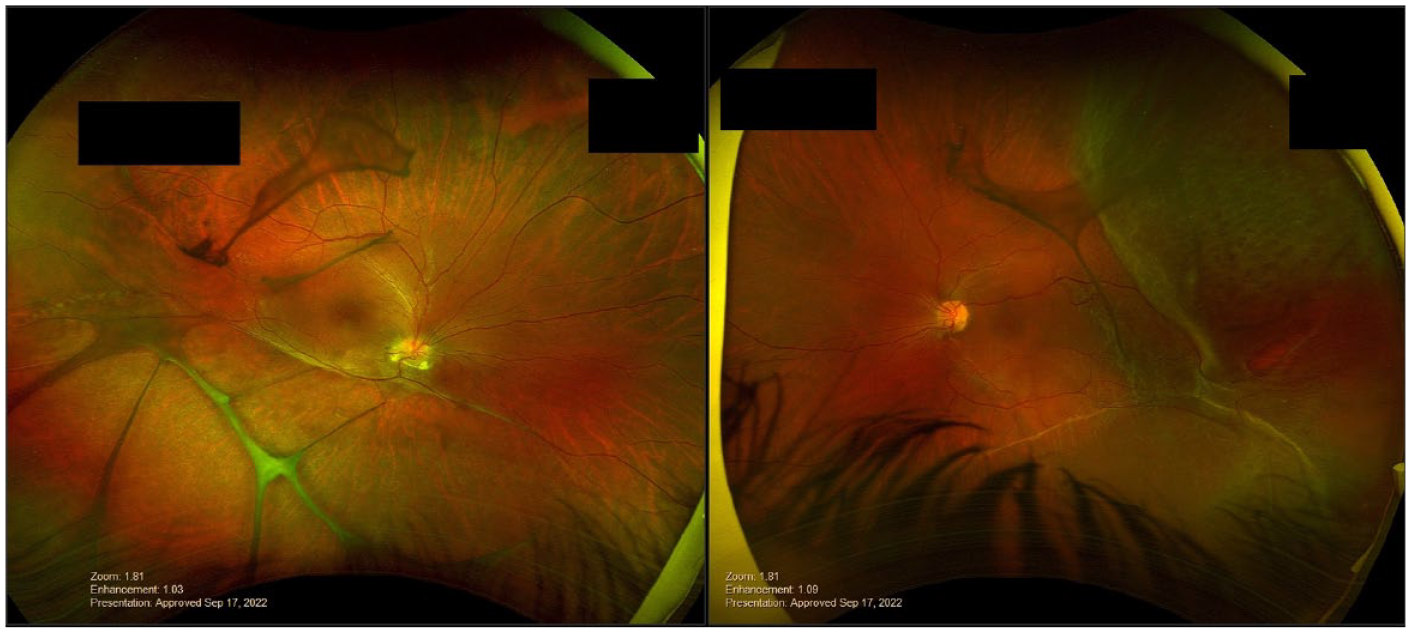
Ultra-wide field fundus photography at presentation demonstrating peripheral retinoschisis with vitreous veils in both eyes and inferotemporal rhegmatogenous retinal detachment in the left eye.

(a) SD-OCT of right eye illustrating foveal and lamellar macular schisis at the level of the outer plexiform layer. (b) Preoperative SD-OCT of the left eye showing macular retinoschisis and retinal detachment with macular involvement. (c) SD-OCT on the first postoperative day demonstrating significant resolution of macular schisis and retinal thinning due to collapse of schistic cavities in the left eye. The anterior most hyperreflective layer corresponds to silicone oil.
The patient underwent a 23G PPV for the management of the RRD. Briefly, successful posterior vitreous detachment (PVD) in the presence of vitreoschisis was achieved with the use of forceps (Alcon Grieshaber® Revolution DSP ILM Forceps, 23 G, Alcon Inc, USA) following triamcinolone staining. An atraumatic internal limiting membrane (ILM) peeling was performed centrally within the macula after staining with MembraneBlue-Dual™. The size of the ILM peeling was intentionally narrow, extending approximately at less than a disc diameter outside the foveal avascular zone(FAZ) area, in order to reduce the chance of further neural damage to an already greatly compromised retina from the XLRS itself. Inspection for proliferative vitreoretinopathy revealed an area of preretinal proliferation with neovascularization inferiorly, at 4 and 5 clock hours, which was treated with segmentation scissors and diathermy. After subretinal fluid drainage through the break, fluid air exchange, endolaser, and cryopexy in areas of possible small breaks were also performed followed by air/SO (5000 CS) exchange.
On the first postoperative day, BCVA in OS was 6/60 and retina was attached. SD-OCT showed significant resolution of the foveal and macular schisis [Figure 2(c)]. The immediate post-operative period was uneventful. At the 1-week follow-up, BCVA had improved to 6/24 in OS and SD-OCT demonstrated a subtle reappearance of the schisis cavities only nasally to the fovea. Although the foveal depression was present, thinning/collapse of the outer nuclear layer and coalescence of the rest of retinal layers was observed in the foveola [Figure 3(c)]. This disorganization of the fovea corresponded to an abnormal FAZ seen on OCT-angiography (OCTA) in this stage [Figure 3(a) and (b)]. One month after surgery, patient’s BCVA was 6/19 but on SD-OCT schistic spaces throughout the macula had moderately increased [Figure 3(f)]. Areas of reduced density were observed in OCTA in the deep capillary plexus (DCP) accompanied by flow voids in the choriocapillaris (CCP) layer mainly nasally as well as inferiorly, corresponding to the areas where schisis had reappeared [Figure 3(d) and (e)]. At 2 months post-op, BCVA has risen to 6/15 as the fovea remained flat. Three months post-operatively, in spite of a substantial deterioration regarding the size of schisis cavities, and while schisis had now involved the fovea [Figure 3(i)], BCVA remained stable at 6/15. Previously noted DCP and CCP flow void areas had increased possibly corresponding to shadowing effect from the schistic spaces located between inner plexiform layer (IPL) and outer plexiform layer (OPL) together with artifacts from SO [Figure 3(g) and (h)]. The patient remains under close observation to date.

(a, b) OCTA of the left eye 1 week post-operatively capturing abnormalities of the foveal avascular zone (a) at the level of the SCP and (b) DCP and loss of focal loss of DCP density in the left eye. (c) SD-OCT showing macular thinning temporally with collapse of the schistic cavities noted earlier and presence of residual intraretinal cysts nasally. (d, e) OCTA 1 month postoperatively revealed areas of flow loss (d) in the DCP also evident (e) in the CCP. (f) SD-OCT after 1 month showed subtle reappearance of the schistic spaces throughout the entire macula. (g, h) Enlargement of previously observed flow void areas in OCTA (g) in the DCP as well as (h) the CCP at the 3 months follow-up. (i) SD-OCT at 3 months demonstrated deterioration of macular schisis with loss of foveal contour.
Discussion
Retinal detachment constitutes a potentially devastating complication of XLRS and an absolute indication for surgical intervention. Favorable anatomic and functional outcomes of vitreoretinal surgery in retinoschisis have been reported in series of pediatric patients for complications of XLRS as well as progressive XLRS, providing evidence on the role of the vitreoretinal interface in the pathogenesis of the disease and its complications.4–6
In this case retinal reattachment and an initial morphologic realignment of the neuroretinal layers with collapse of the schistic cavities were achieved. Resolution of macular and foveal schisis has been documented in previous case reports treated with vitreoretinal surgery in combination with SO, as well as gas tamponade.5–7 However, recurrence has been frequently reported upon SO removal (SOR). 8 Interestingly, in our case a rather rapid and progressive recurrence developed in the presence of retained SO and peeled ILM.
The benefit of ILM peeling in XLRS is debatable. While ILM peeling in RRD is associated with reduced risk of retinal detachment (RD) recurrence and epiretinal membrane (ERM) development,6,8 some authors highlight the possibility of macular hole or iatrogenic tear occurrence due to the structural instability of the retina in XLRS. 7 In the case presented herein we opted for ILM peeling aiming to eliminate potential tractional elements, such as residual vitreous cortex and fibroglia, and reduce the risk of ERM formation.
Though past reports correlate older age, PVD and SO with reduction of schisis cavities,7,9 despite our patient’s young age, ILM peel and SO presence, a rather rapid recurrence of schisis was noticed. Recurrence has been described upon SOR with intact ILM. Sen et al. 5 observed schisis present under SO that resolved upon SOR only to recur 6 months later, and Goel and Ghosh 7 reported absence of schisis with SO and recurrence 3 weeks upon removal. On the other hand, García et al. 10 have reported resolution of schisis post SOR; however, the provided follow-up was limited to 3 months. Interestingly, vision was 6/60 at the time when foveal schisis had temporarily resolved and was 6/15 at the recurrence of schisis, showing the non-concordance between structure and function, at least at this stage. It is unclear in our case if the removal of ILM contributed to a more rapid recurrence of the schisis cavities. Another hypothesis that could explain the early recurrence of macular schisis is the accumulation of abnormal retinoschisin (cell adhesion protein) around the Muller cells that could consequently lead to the development of coalescent cystic cavities. 11 Furthermore, variable amounts of inflammation can confound our assessment of schisis due to RS1 changes versus cystic changes form classic inflammation. 12
Abnormalities of the shape and size of the FAZ have been documented in SCP and DCP in XLRS patients. 13 In this case, FAZ was irregularly small during the follow-up imaging possibly due to the disruption and collapse of the inner retinal layers in the postoperative period, while a relatively enlarged FAZ was observed in the fellow eye. Moreover, areas of flow loss were observed in the left eye in our patient in the DCP as well as the CCP. These microvascular alterations predominantly involving the DCP rather than SCP, have been described in literature as reduced density and microvascular protrusions located in pillar-like structures among cystic areas presumably due to debilitated vascular walls or direct mechanical effect from intraretinal fluid buildup, while no changes have been reported in the CCP layer. 13 Interestingly in our case these changes were notable only in OS which may argue for a role of the RD and the associated repair procedure with oil in these changes. Unfortunately, no preoperative OCTA is available to allow for comparison.
Conclusion
While PPV has been associated with beneficial outcomes in XLRS cases either complicated by RRD or not, in the present case PPV with SO resulted in short-term resolution of foveoschisis. Nonetheless, recurrence of macular schisis early in the presence of SO indicates the fundamental role of abnormal cellular adhesion which constitutes the pathogenetic basis of the disease. The role of ILM peeling in XLRS-related RRD remains unclear, as in this case it may have contributed to the early recurrence of the schistic macula. As the contributing biological factors and the clinical manifestations of XLRS have not yet been fully bridged, larger studies and long-term follow-up of surgical cases may provide insight and allow better comprehension of pathophysiology and the role that vitreoretinal interventions can assume in XLRS management.
