Abstract
Aim
To quantify delays in migraine diagnosis and treatment in an Australian tertiary hospital headache clinic.
Methods
Data were collected from patients attending a tertiary headache clinic from February 2024 to November 2024 and entered into a secure REDCAP database. Patients fulfilling International Classification of Headache Disorders-3 (ICHD-3) diagnostic criteria for migraine were included in the study. Patients were asked the earliest age they could recall having migraine symptoms, when they first received a diagnosis of migraine from a clinician, and what preventive treatments they had tried for migraine. Statistical analysis with the Mann-Whitney U test for numerical data and Fisher's exact test for binomial data was then performed on SPSS.
Results
The median delay between migraine symptom onset and formal diagnosis of migraine was 6 years. 39% of patients (39/100) had not trialled a preventive prior to attendance at the clinic, including 27% (20/73) with 8 or more migraine days per month. There was a median delay of 11 years between reported symptom onset and commencement of prophylactic therapy.
Conclusion
There remain significant delays in migraine diagnosis and commencement of prophylactic therapy in Australian patients with migraine.
Keywords
Introduction
Migraine is a highly prevalent and disabling condition worldwide, and the greatest cause of morbidity in women aged 20–50 years. 1 Approximately 5 million Australians are thought to have migraine, although this is likely an underestimate. The Migraine in Australia White Paper from 2017 conservatively estimated the annual burden of migraine to be over $35.7 billion per year. 2
There is a paucity of Australian data exploring delays in the diagnosis of migraine and, by extension, potential delays in treatment. Previous epidemiological studies, such as the afore-mentioned Migraine in Australia White Paper and AHEAD study, provided broad data on the prevalence of migraine but did not explore the extent or effect of these delays. 3 By measuring the cost of migraine from the moment of diagnosis rather than the onset of symptomatology, we potentially underestimate the economic and health burden of migraine. Clinician-related factors, including a lack of focused headache clinics and limited education on headache disorders from the university level through to neurology specialist registrars (called neurology advanced trainees), are likely contributors. 4 Indeed, this same study indicated that a minority of neurology advanced trainees felt comfortable with either inpatient or outpatient management of headache disorders. There are currently only two headache fellowship positions in Australia, and only a handful of Australian neurologists are specifically fellowship trained in the treatment of headache disorders.
Furthermore, wider societal factors such as broad stigma surrounding patients with headache disorders, as well as underdiagnosis and underreporting of disease burden, may also contribute to these delays. 5 Underdiagnosis continues despite very clear diagnostic criteria from the International Classification of Headache Disorders 3 (ICHD-3). 6 The lack of Australian data to corroborate these findings has posed a challenge in proposing wider initiatives and obtaining funding for improving education on the diagnosis and treatment of migraine, which is likely to perpetuate these delays.
By identifying the delays in diagnosis and treatment experienced by patients with migraine in a tertiary headache clinic in Australia, we hope to better advocate for further initiatives, funding, and education on the diagnosis and management of this prevalent and disabling disorder.
Methods
Data were collected from consecutive patients attending a tertiary hospital headache clinic from February 2024 to November 2024 and entered into a secure REDCAP database. Patients fulfilling ICHD-3 diagnostic criteria for migraine were included in the study. All patients were assessed by a headache fellow with subspecialist expertise in headache disorders. Patients were sub-categorised as having episodic migraine (EM) if they had less than 8 days a month of migraine headache, high frequency EM (HFEM) if they had between 8 and 14 days of migraine headache a month, and chronic migraine (CM) if they had 15 or more days of migraine headache a month. Data were collected on patient-reported age of symptom onset as well as age of formal diagnosis of migraine by a healthcare professional and source of referral to our tertiary headache clinic. Data were also collected on previous and current use of prophylactic medication for migraine. Data were collected by detailed history taking through a single assessor using a standardised questionnaire, reducing the risk of interrater variability. Age of diagnosis was cross-referenced against previous medical records, including general practitioner (GP) referral letters or previous clinical letters where such data were available. Normality of the distribution of numerical data was assessed graphically by quantile-quantile plots, which showed the data were not normally distributed. Statistical analysis with the Mann-Whitney U test for non-parametric numerical data and Fisher's exact test for binomial data was then performed on IBM SPSS Statistical Software (Version 29). A result was deemed statistically significant if the P < 0.05. Ethics approval was obtained by the St Vincent's Hospital Human Research Ethics Committee (2024/ETH0997).
Results
There were 100 consecutive patients identified between February 2024 and November 2024 who attended the tertiary hospital headache clinic and fulfilled ICHD-3 criteria for migraine. Of these patients, 27% (27/100) had EM, 12% (12/100) had HFEM, and 61% (61/100) had CM. There were significantly more women (80%) compared to men (20%) in our cohort. The median age for the study cohort was 45 years, the median age for women was 44 years, compared to the median age of men being 49 years. Most patients (57%) were referred to the clinic by a GP, followed by other specialist clinicians (33%) and, least commonly, by emergency department clinicians (10%).
Table 1 shows the differences in migraine symptom onset, formal diagnosis of migraine, and median delay between comparator groups.
Comparison between groups.
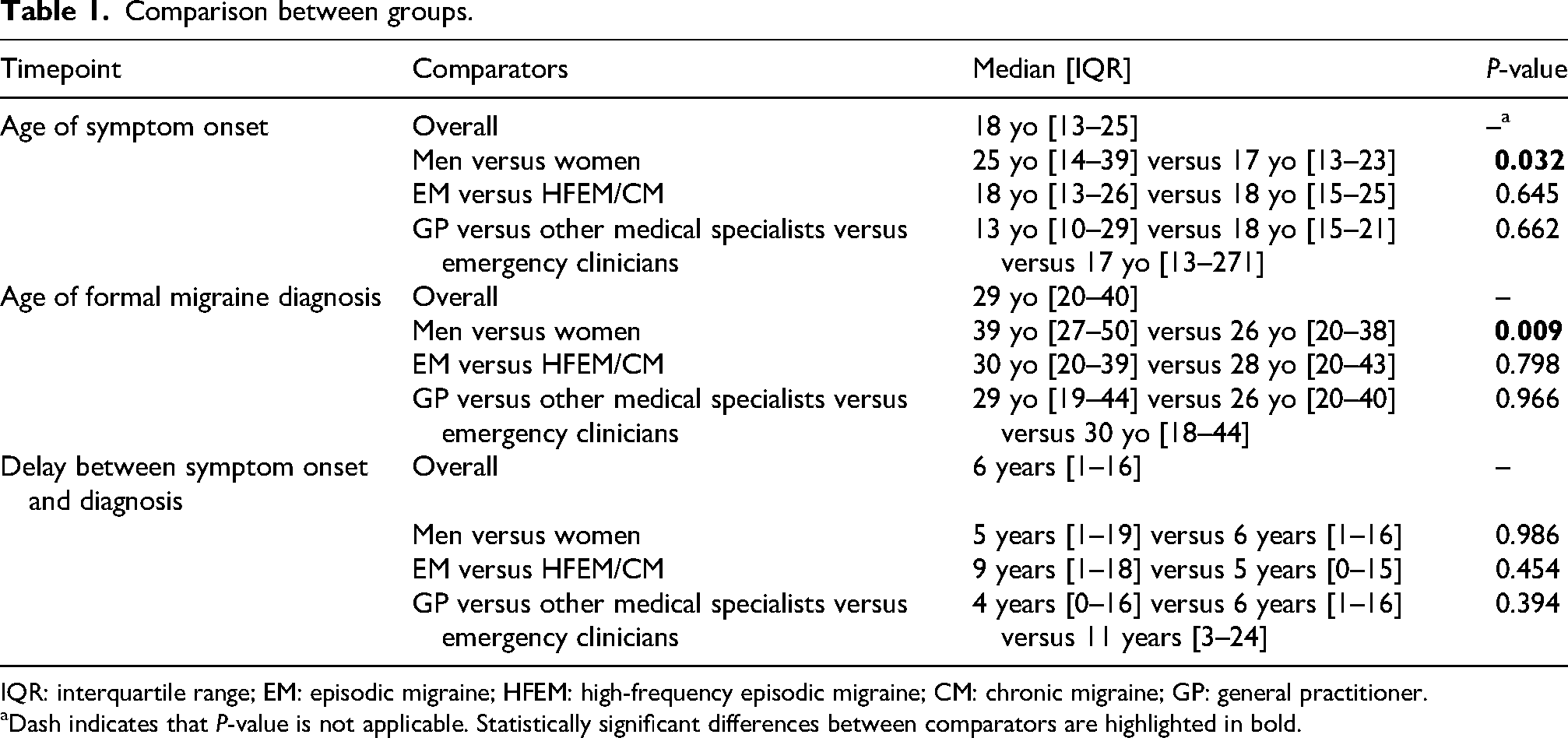
IQR: interquartile range; EM: episodic migraine; HFEM: high-frequency episodic migraine; CM: chronic migraine; GP: general practitioner.
Dash indicates that P-value is not applicable. Statistically significant differences between comparators are highlighted in bold.
Over one-third of patients (39%) had not trialled a preventive prior to their review in our clinic, including 27% (20/73) of patients with eight or more migraine days a month. Of the 20 patients with eight or more migraine days a month who had not previously been on a prophylactic prior to their review in our clinic, there was a median delay of 11 years [IQR 2–18] between reported symptom onset and commencement of prophylactic therapy. Patients referred by other medical specialists were more likely to have never tried prophylactic therapy compared to patients referred by emergency departments (70% vs. 27%, P = 0.024). No other statistically significant differences were found between referral sources. Out of the patients who had previously tried a preventive, amitriptyline was the most common previously tried preventive (58%), followed by propranolol (51%) and then topiramate (39%). The median number of preventives tried prior to the first review in our clinic was 2 [IQR 1–4].
Discussion
This study demonstrated a significant gap between migraine symptom onset and diagnosis of migraine for both men and women. Men generally reported later symptom onset and age of diagnosis. Furthermore, a substantial proportion of patients, including patients with eight or more headache days a month, had not previously been trialled on a preventive agent. International guidelines generally recommend commencement when patients have four or more migraine days a month.
The chronification of migraine is likely in part due to inadequate treatment of migraine attacks when they are still episodic. Proactive treatment of migraine has been shown to yield better outcomes over time. 7 Many migraine are treatable by readily available medications. Patients in Australia with CM refractory to at least three preventives now have access via the Pharmaceutical Benefits Scheme (PBS) to CGRP monoclonal antibody therapy, with data showing over 50% of patients receiving these treatments achieving over a 50% reduction in headache burden. 8 A delay between symptom onset and diagnosis of migraine represents many years of missed opportunity to manage this condition. This is represented by the median delay of 11 years between reported symptom onset and the commencement of a prophylactic among patients with HFEM/CM. Our study results highlight that this suboptimal treatment may be a result of delays in reaching a formal diagnosis of migraine by a healthcare professional and in the initiation of treatment once a diagnosis is reached.
The data were collected based on patient history and, as such, are subject to potential recall bias. This sample size is small for a highly prevalent disease and is biased towards more severe cases. Hence, the proportion of CM referred to a headache clinic compared to EM would be significantly higher than that of the Australian population as a whole. However, this may mean that our study in fact underestimates these gaps, as our study cohort potentially reflects patients and referring practitioners who are more proactive with seeking diagnosis and management. The study was limited to a single centre primarily due to the lack of other regular public hospital headache clinics in the state of New South Wales; future studies collaborating with centres elsewhere in the nation could corroborate these results.
This may also reflect issues with accessibility. For example, our headache clinic is the only public hospital dedicated to headache clinic in the state of New South Wales. It is possible that patients, therefore, may not be accessing specialist care for headache due to the lack of availability of such clinics and financial or logistical difficulties with headache subspecialist follow-up in the private sector. This lack of availability of dedicated headache clinics also suggests that patients rely on the diagnosis and management of migraine being driven by primary care physicians and neurologists not subspecialised in headache disorders. Our study did not show that sex, referral source, or frequency of migraine were predictors for delays in diagnosis or treatment, with delays universal across the spectrum of migraine patients. This possibly augments the argument that delays in migraine treatment and diagnosis might be primarily driven by societal and system factors rather than individual patient factors. This is in keeping with a large study exploring barriers to care in the United States population, which identified several predictors for seeking consultation with a headache specialist, the strongest predictor being coverage by health insurance rather than the migraine characteristics of the patient. 9
The results of our study therefore indicate the need for greater emphasis on headache education and training for both primary care as well as specialist clinicians. Patients may also be presenting to clinicians late due to a lack of awareness regarding treatment options or stigma. Initiatives to raise awareness of migraine amongst the general Australian population, therefore, may also prove to be useful in prompting migraine sufferers to seek medical attention earlier.
There are significant delays between symptom onset and formal diagnosis in patients with migraine, as well as gaps in commencing prophylactic treatment. The lack of availability of specialty headache clinics in the public healthcare system is counterintuitive, particularly when considering the well-documented burden of disease and the huge direct and indirect costs. The delays in diagnosis despite readily available diagnostic criteria for migraine also indicate gaps in education and training amongst clinicians, and also reflect a need to raise awareness of migraine amongst the general population. These gaps may be contributing to the significant disability and economic cost of migraine and are important to address with more proactive initiatives to diagnose and treat this highly prevalent disorder.
Public health relevance
In our study cohort, there was a median delay of 6 years between the onset of migraine symptoms and formal diagnosis of migraine.
27% of patients in our cohort who had HFEM or CM had not previously trialled migraine preventive treatment.
Of the patients who had high-frequency episodic or CM within our cohort, the median time between onset of migraine symptoms and initiation of prophylactic therapy was 11 years.
Footnotes
Acknowledgements
Not applicable.
Ethical considerations
Ethics approval was obtained by the St Vincent's Hospital Human Research Ethics Committee (2024/ETH0997).
Consent to participate
All participants were provided with written information about the study and provided informed consent.
Consent for publishing
Yes.
Author contributions
Both authors contributed equally.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The information is provided upon reasonable request to the corresponding author.
Open practices
Not applicable.
