Abstract
Background
Dry eye disease (DED) and migraine, two common disorders with public health concerns, may have a bidirectional relationship. Population-based studies have found that migraine patients have higher odds of DED and vice versa. We aimed to evaluate and compare the presence of DED symptoms and objective signs between migraine patients and non-migraine controls.
Methods
This was a case-control study. We prospectively enrolled 60 consecutive migraine patients (30 episodic and 30 chronic) presenting in the medicine outpatient department, aged 18–65 years, and 60 non-migraine healthy controls visiting the ophthalmology department for refractive errors between February 2019 and June 2021. Consecutive migraine patients and non-migraine healthy controls were assessed in the ophthalmology department at Hindu Rao Hospital, Delhi by the Ocular Disease Surface Index (OSDI) questionnaire for DED symptoms and objectively by measuring tear break-up time (TBUT), Schirmer test (ST), and Fluorescein staining (FS). DED severity was assessed by the Odessey algorithm.
Results
The mean OSDI score was significantly greater in migraineurs than in controls (31.2 ± 19.8 vs 22.7 ± 15.6; p = 0.010). 45% of migraineurs had DED compared to 18.3% in controls (p = 0.002), whereas 23.3% had severe DED compared to one (1.7%) in the control group (p < 0.001). Migraineurs, compared to controls, had significantly lower mean TBUT (10.1 ± 6.5 s versus 13.4 ± 5.8 s; p = 0.004), higher FS grade (1.57 ± 1.4 versus 0.92 ± 1.2; p = 0.008) and lower ST scores (11.5 ± 5.8 mm versus 14.2 ± 6.2 mm; p = 0.014). Migraineurs with DED, compared with those without DED, had longer migraine disease duration, higher frequency, pain severity, and disability. Compared to episodic migraine, chronic migraine patients had significantly lower TBUT (11.9 ± 5.9 vs 8.3 ± 6.7; p = 0.30) and higher OSDI scores (25.7 ± 20.1 vs 36.8 ± 18.2).
Conclusions
This study showed that migraine patients had an increased presence of DED and severe DED compared to controls. Further, increased migraine severity and chronicity were associated with increased subjective symptoms and objective signs of DED. Migraine patients with DED were more disabled.CM patients had more DED symptoms and signs.
Keywords
Introduction
Dry eye disease (DED) results from the dysfunction of the tear film mechanisms. There are two tear film layers: a thicker, muco-aqueous layer and a thinner lipid layer. The muco-aqueous layer interacts with the corneal epithelium, and the lipid layer prevents its evaporation by sitting on top of it. 1 DED can be due to either aqueous tear deficiency or dysfunction of evaporative mechanisms, or both. 2 Tear film stability can be impacted by many intrinsic and extrinsic factors affecting hyperosmolarity and activating osmotic and mechanical stress mechanisms. 3 Ocular surface stress can lead to ocular cell damage and the release of inflammatory mediators, which increases the potential for epithelial damage. 4 Among the ocular surface disorders, DED is highly prevalent. Two recent metanalyses reported the prevalence of DED to be 8.1% and 20.1% in the United States and Asia, respectively.5,6 The reason for this difference in prevalence rates may be due to differences in methodology used for diagnosing DED as many studies have only used symptom criteria for DED diagnosis which might have resulted in overestimation. 6 DED is also a disabling disease and significantly reduces the quality of life.
Migraine is a common chronic neurological disorder with a 1-year prevalence of 14.7%. 7 It ranks second in terms of disability. 8 Migraine has been divided into two major subtypes, namely episodic migraine (EM) and chronic migraine (CM), depending on headache frequency. 9 CM patients have at least 15 headache days per month, of which at least 8 days have migrainous features. 9 Currently, the exact pathophysiology of migraine remains unknown. 10 However, a sterile neurogenic inflammation involving the trigeminovascular pathways is considered one of the important mechanisms for recurrent migraine headaches. 10 The cornea supplied by the trigeminal nerve represents a preferential target of neurogenic inflammation. 11 There is also strong support for the role of neurogenic inflammation in many ocular surface diseases, such as Sjogren syndrome. 12 Interestingly, the prevalence of migraine is higher in patients with Sjogren syndrome. 13 Therefore, there may exist a relationship between DED and migraine, both being hypothesized to be due to an inflammatory state.14,15
The relationship between migraine and DED and vice versa has been studied previously. In a meta-analysis, Qian et al. reported that patients with DED had an increased risk of migraine by 1.53-fold. 16 In contrast, a meta-analysis by Chen et al. reported the odds of morbidity due to DED to be 1.55 times in migraine patients. 17 Therefore, it appears that migraine and DED are comorbid, and there is evidence of a bidirectional association. There are, however, some uncertainties regarding the relationship between the two, and some aspects of this relationship need to be explored adequately. 18 For example, a few studies have reported subjective dry eye symptoms with a normal ocular surface,19,20 while others have also found objective evidence of DED.13,14 Further, the relationship between the grades of severity of DED and migraine, especially its subtypes, such as EM and CM, remains largely unexplored. Hence, more studies are needed to explore not only the associations between the symptoms and signs of DED in migraine patients but also to look carefully at whether the severity of DED has any relationship with episodic and chronic migraine. We hypothesized that severe DED should have a positive association with severe migraine and its chronification.
This study, therefore, aimed to evaluate the tear film functions and clinical symptoms of DED in patients with EM and CM and compare them with non-migraine patients. It also aimed to study the associations between headache characteristics like disease duration, frequency of attacks, pain intensity, and headache disability in migraine patients with DED and severe DED using a study design that not only replicated the methods of some of the previous studies but also separately studied the subtypes of migraine, which had not been done previously.
Material and methods
This cross-sectional observational-analytic hospital-based study was conducted between February 2019 and June 2021at the Ophthalmology Department of Hindu Rao Hospital, Delhi, India. The migraine patients were diagnosed and referred from the medicine outpatient department. Patients visiting the ophthalmology outpatient department for refractive errors and having no history of migraine served as controls. Both migraine patients and the controls were then screened for inclusion and exclusion criteria.
Inclusion and exclusion criteria
Migraine patients, both episodic and chronic with and without aura, 18 to 65 years of age diagnosed by the international classification of headache disorders, third edition (ICHD-3) criteria were included. Only those migraine patients who were preventive drug naïve, that is, not on any regular preventive medication for the last three months, were included. Migraine patients with acute medication overuse, as defined by ICHD-3, were excluded. The controls consisted of age- and sex-matched patients between 18 and 65 years visiting the ophthalmology department for refractive errors without any history of migraine headaches. Both the patients and controls with a history of ocular surface disorder, previous ocular surgery or ocular injury, allergic ocular disease, papillary conjunctivitis, contact lenses use, topical eye medication use within the previous three months, chronic drug use including the decongestants, antihistamines, beta-blockers in the last 3 months and history of chronic diseases like diabetes, Sjogren disease, rheumatoid arthritis, and systemic lupus erythematosus were excluded.
Diagnosis of DED and its severity
DED was diagnosed by noting the tear film break-up time (TBUT) of ≤ 10 s. Severe DED was diagnosed by using Odyssey criteria. 21 Patients with an OSDI score ≥33 and CFS score ≥3 on the Oxford scheme were diagnosed as having severe DED in patients whose signs and symptoms of the disease associate well. Those fulfilling only one of these two primary criteria, one or more of the following additional criteria, such as the presence of strands and / filaments on cornea, presence of meibomian gland dysfunction (MGD), filamentary keratitis and TBUT < 3 s, were required for the diagnosis of severe DED. 21 MGD was defined as a chronic, diffuse abnormality of the meibomian glands, commonly characterized by terminal duct obstruction (meibomian gland orifice plugging) and qualitative/ quantitative changes in the glandular secretion. 22
Patient evaluation and data collection
The primary demographic details, such as the age and sex of all included patients, were noted. Migraine patients were evaluated for headache characteristics, including the subtype (episodic and chronic), monthly migraine days (MMD), monthly headache days (for chronic migraine patients), presence or absence of aura, average attack duration, and the intensity of headache attack [by using a visual analog scale, 0–10 (VAS)]. The headache-related disability was measured by headache impact test-6 (HIT-6). 23 It consists of six items: pain, social functioning, role functioning, vitality, cognitive functioning, and psychological distress for the past month. The patients answered each using one of the five responses. These were summed to produce a total HIT-6 score (that ranged from 36 to 78); a higher score indicated a more significant impact.
The Ocular Surface Disease Index (OSDI) questionnaire initially assessed all patients for DED symptoms. 24 Based on the score, the patients were categorized as having a normal ocular surface (0–12) or having mild (13–22), moderate (23–32), or severe (33–100) ocular surface disease. Then they underwent a complete ophthalmic examination that included best corrected visual acuity (BCVA), slit lamp examination, intraocular pressure measurement, fundus examination, and diagnostic tests for DED, including tear break-up time (TBUT), Schirmer test (ST), Fluorescein staining (FS). Both eyes were evaluated. The worst eye measures were considered for analysis. The worst eye was defined as the eye with a lower TBUT. Slit lamp biomicroscope examination of the preocular tear film was done to look for luster, debris, or overlying mucus strands. Lid margin signs looked for included posterior lid margin erythema or hyperemia, lid margin thickening or irregularity, meibomian gland orifice plugging, turbidity of meibomian gland secretions, lid margin telangiectasia, and meibomian gland plugging.
For the diagnostic tests of DED, the following sequence of ocular surface examination was maintained to prevent reflex tearing. On staining the cornea with fluorescein stain, the TBUT was noted, followed by grading the FS score of the cornea using the Oxford grading system. Then, the ST was performed in each eye. The interval between FS and ST was maintained at more than 10 min.
Ethical approval
The institutional ethics and scientific committees of the Hindu Rao Hospital, New Delhi, India, approved the study. Informed consent was obtained from all the patients and the patient confidentiality was ensured.
Statistical analysis
Statistical testing was conducted using the statistical package for the social science system version SPSS 25.0. Continuous variables are represented as mean ± SD, and categorical variables are presented as absolute numbers and percentages. The normally distributed continuous variables were compared between the groups using the student's t-test. Nominal categorical data between the groups were compared using the appropriate Chi-square test or Fisher's exact test. p < 0.05 was considered statistically significant.
Results
Sixty migraine (cases) and sixty non-migraine (controls) patients were studied. Of the sixty migraine patients, thirty had EM, and thirty had CM. Figure 1 depicts the flow of the study.

Flow of the study.
Demographic profile
The mean age at presentation was 33.5 ± 7.1 and 33.2 ± 7.4 years in cases and controls, respectively (p = 0.82). There were 46 (76.7%) females and 14 (23.3%) males among the migraine patients compared to 44 (73.3%) females and 16 26.6% males in the control group (p = 0.83).None of the migraine patients were taking preventive drugs for the last three months. All of them were on acute medications, but patients with medication overuse were excluded. Five patients each with chronic migraine, had received Botulinum toxin injections and greater occipital nerve blocks from a tertiary care center three months before inclusion in the study. None of the controls took anticholinergic drugs at the time of inclusion in the study.
Headache characteristics of migraine patients
The mean disease duration was 5 ± 3.1 years. Twelve patients (20%) had visual aura. The MMD was 9.6 ± 5.4. The mean headache intensity score by VAS was 6.6 ± 1.4, and the mean migraine disability by HIT-6 score was 45 ± 11.5
Routine ophthalmological examination
The distribution of worst eye (left versus right) in migraine patients and controls was similar (24/36 vs 26/34). The two groups’ best-corrected visual acuity and IOP measures in the worst eyes were also similar (Table 1). The fundus examination was normal in all subjects. MGD was present in 31.7% of migraine patients compared to 30% in the control group (p = 0.598).
Comparison of demography and dry eye parameters between migraine patients and controls.

IOP: intraocular pressure; MGD: meibomian gland dysfunction; OSDI: ocular surface disease index; DED: dry eye disease; TBUT: tear break-up time; FS grade: Fluorescein staining; ST: Schirmer's test.
a: Compared using the student's t-test. b: Compared using the Chi-square test or Fisher's exact test. p < 0.05 was considered statistically significant. c: The worst eye was defined as the eye with lower TBUT.
Between-group comparisons
Demographic and other ophthalmologic features were similar between the migraine patients and the controls ). (Table 1). Twenty-one (35%) migraine patients had severe dry eye symptoms (≥ 33 OSDI score) compared to 12 (20%) in controls. The mean OSDI score in migraine patients was significantly greater than in controls (31.2 ± 19.8 vs 22.7 ± 5.6; p = 0.01). Twenty-seven (45%) migraine patients had DED compared to 11(18.3%) in controls (p = 0.002). Fourteen migraine patients (23.3%) had severe DED compared to one (1.7%) in the control group (p < 0.001). The mean TBUT in cases was 10.1 ± 6.5 s versus 13.4 ± 5.8 s in controls (p = 0.004). A higher grade of FS of ocular surface was observed in migraine patients compared to controls (1.57 ± 1.4 versus 0.92 ± 1.2; p = 0.008). The mean ST-I score was 11.5 ± 5.8 mm in cases and 14.2 ± 6.2 mm in controls (p = 0.014). ST-I < 10 mm was seen in 18 (30%) of cases compared to 12 (20%) in controls.
Within-group comparisons
Migraine patients with DED had longer disease duration (5.9 ± 3.6 vs. 4.3 ± 2.5; p = 0.037), higher MMD (12.5 ± 4.4 vs 7.1 ± 5; p < 0.001), more significant pain severity (7.6 ± 1 vs 5.9 ± 1.2; p < 0.001) and more significant disability (52.4 ± 13 vs. 39 ± 5; p < 0.001) compared to migraine patients without DED (Table 2). Migraine patients with severe DED showed similar trends except for disease duration (Table 3). Among the twelve migraine patients with aura, eight (66.7%) patients had DED, and among them, five (41.7%) had severe DED. Migraine patients with aura compared to migraine patients without aura had significantly higher OSDI scores (47.2 ± 12.9 vs 27.3 ± 17.6; p = 0.008), higher FS scores (2.6 ± 1.6 vs 1.3 ± 1.2; p = 0.020). TBUT and ST-I scores, though lower, were not statistically significant.
Comparison of headache parameters in migraine patients with and without DED.

DED: dry eye disease; VAS: visual analog scale; HIT-6: headache impact test-6. All parameters were compared using the student's t-test; p < 0.05 was considered statistically significant.
Comparison of headache parameters in migraine patients with and without severe DED.

DED: dry eye disease; VAS: visual analog scale; HIT-6: headache impact test-6. All parameters were compared using the student's t-test; p < 0.05 was considered statistically significant.
Comparison of DED and severe DED between episodic and chronic migraine patients
Demography, headache characteristics and eye findings in pateints with EM and CM are summarized in Table 4. Seven (23.3%) patients with EM had DED compared to twenty (66.7%) patients with CM (p = 0.001), whereas four patients (13.3%) of EM had severe DED compared to 10 patients (33.3%) of CM (p = 0.125). Compared to EM patients, CM patients had significantly lower TBUT (11.9 ± 5.9 vs 8.3 ± 6.7; p = 0.030) and higher OSDI scores (25.7 ± 20.1 vs 36.8 ± 18.2; p = 0.028). FS and ST scores, however, did not differ significantly (Figure 2A, B).

(A) Comparison of the presence of DED and severe DED between episodic and chronic migraine. (B) comparison of the objective parameters of DED between episodic and chronic migraine.
Demography, headache characteristics, and eye findings in patients with episodic and chronic migraine.
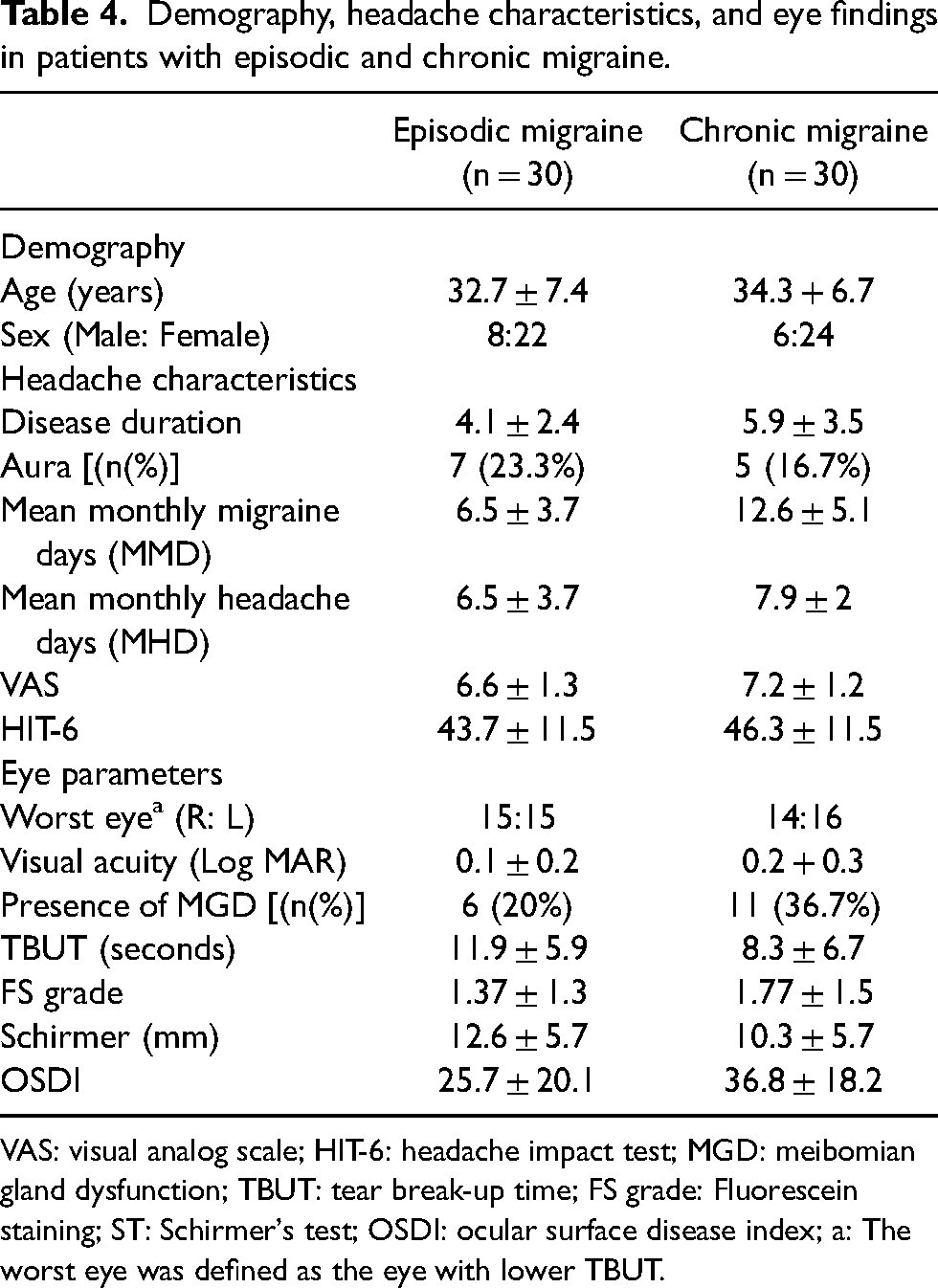
VAS: visual analog scale; HIT-6: headache impact test; MGD: meibomian gland dysfunction; TBUT: tear break-up time; FS grade: Fluorescein staining; ST: Schirmer's test; OSDI: ocular surface disease index; a: The worst eye was defined as the eye with lower TBUT.
Discussion
This study showed that the migraine patients complained significantly more DED symptoms and had a higher presence of DED and higher severity grades of DED compared to non-migraine controls. These findings are important in the context of uncertainties raised by previous studies that showed inconclusive associations between DED and migraine.25,26 The novelty of this study includes the finding that it's not just the presence of DED symptoms and disease that occurs more frequently in migraine patients but that migraine patients have more severe DED. Furthermore, CM migraine patients have more DED symptoms and signs compared with EM patients. To the best of our knowledge, no previous head-to-head comparative studies between CM and EM are available in the literature so far.
Subjective evidence of dry eyesymptoms using DEQ-5(Dry eye Questionaire-5 Questions) and OSDI scores have been reported previously.13,26Of note, OSDI incorporates diverse components such as pain, visual complaints, tearing, and activity limitations to reach a final score. 24 Migraineurs not only complain of headache and eye pain but may also complain of cranial autonomic symptoms, including tearing, a multitude of visual complaints (photophobia being the commonest), and limitations of activity during the attacks. 27 These overlaps in symptoms may affect the OSDI scores but possibly also suggest a common pathophysiological mechanism for the two conditions. Studies have shown that the reduced visual quality of life as assessed by the visual functioning questionnaire-25 (VFQ-25) in migraineurs is most closely correlated with the symptoms of dry eye as measured by OSDI. 28
In the present study, 45% of migraine patients had DED compared to 18.3% in controls. In a cross-sectional study by Celikbilek et al., involving 58 migraineurs and 41 controls, 62.1% of migraine patients had DED (defined by fulfilling two of three criteria: ST value less than ten mm/5 min, TBUT shorter than 10 s and OSDI value higher than 33) compared to 51.2% in controls (the difference was non-significant). 19 In another study involving 34 adults with migraine, 49.5% had evidence of DED (defined by tear osmolarity of 308 mOsm/Lor differences of >8 mOsm/L between the two eyes).The authors concluded this was significantly higher than the prevalence rate of DED in the general population (20%). 20 A large population-based study of 72,969 individuals found that those with migraine had a higher frequency of DED compared to controls (19.6% versus 12.7% respectively), with 1.42 (95% CI, 1.20–1.68) odds of having DED in patients with migraine than those without. 29 This study, however, was a retrospective study that relied on the case records of patients visiting the ophthalmology clinic. Few other population-based studies also reported higher odds of DED in migraine patients and vice versa.30,31 In a meta-analysis by Qian et al. involving 48 studies for risk factors of DED, patients with DED had an increased risk of migraine by 1.53-fold. 16 In contrast, a meta-analysis by Chen et al. involving seven studies reported the odds of morbidity due to DED to be 1.55 times in migraine patients. 17 Therefore, in the context of our results and these previously described studies, it appears that migraine and DED are comorbid, and there is strong evidence of a bidirectional association.
We used the Odyssey criteria 21 for grading DED and found that 23.3% of migraine patients, compared to 1.7% of controls, had severe DED. None of the previous studies have investigated the grades of the severity of DED using Odyssey criteria. These criteria were developed by ODYSSEY European Consensus Group and consisted of a clear and practical algorithm for DED evaluation. The use of these criteria facilitated the diagnosis of severe DED even in the event of discordance between signs and symptoms. One study, however, graded the DED severity by the older Dry Eye Workshop 2007 criteria 32 and reported that the DED severity significantly differed between the migraine patients and the controls. 13 Our study, therefore, adds further evidence that migraine patients not only had an increased presence of DED but also had severe DED using more recent diagnostic criteria for diagnosis of DED.
Previous studies have variably reported TBUT, ST value, and FS changes, raising doubts as to whether objective DED signs are more common among migraineurs. Two studies found that these tear metrics were not significantly different in migraineurs (although the DED symptoms were significantly higher),suggesting thereby that nerve dysfunction rather than DED drives the DED symptoms.25,26 However, the symptoms and signs of DED can be disparate, and a meta-analysis involving 33 studies showed that only 24% of 175 symptom-sign analyses yielded a concordance. 33 In contrast to the above studies, at least two studies found that the tear metrics were significantly altered in migraine patients compared to controls.13,18Some authors, however, suggested interpreting these alterations with caution because the mean ST scores were >10 mm/5minute in both studies. 34 We also found similar results (mean ST values in migraineurs were 11.5 ± 5.8) but additionally found that the ST < 10 mm was seen in 18 (30%) of our cases compared to 12 (20%) in controls. These findings probably indicate a more significant role of evaporative dysfunction rather than tear film production in the causation of DED in migraineurs.
The association between headache characteristics and DED has been sparsely studied. One study found that the presence of aura and the attack duration were associated with the presence of DED in migraine patients. 19 Another study found that the lifetime duration of migraine correlated positively with the OSDI scores and negatively with the tear function tests. 13 Wong et al. reported a weak association between the frequency of headaches and DED. 20 We also found that the migraine patients with DED had longer disease duration, higher MMD, and higher pain severity compared to migraine patients without DED. Migraine patients with aura, compared to migraine patients without aura, had significantly higher OSDI scores and FS grades. Overall, these findings suggest that the subjective symptoms and objective signs of DED have an association with migraine headache parameters and with aura, thereby suggesting a bidirectional relationship.
This study found that CM patients had significantly lower TBUT and higher OSDI scores compared to EM patients. This suggests that the chronification of EM into CM leads to the deterioration of evaporative dry eye mechanisms (as evidenced by lower TBUT) and makes the patient more symptomatic. No previous study compared DED in EM and CM patients, although two studies done exclusively in CM patients showed higher OSDI scores and significantly higher total, coma, spherical, and higher-order aberrations than controls.25,35
Both DED and migraine are disabling conditions and reduce the quality of life (QoL) of the sufferers significantly.36,37 We found that the migraine patients with DED and severe DED were significantly more disabled, as indicated by higher HIT-6 scores compared to those without DED. Previous research reported similar outcomes using different questionnaires for assessing QoL. Additionally, a significant correlation between HIT-6 and OSDI scores indicated that dry eye symptoms are a significant yet often overlooked issue for those with migraine. 28 Taken together, these findings suggest that the diagnosis and management of co-existent DED in migraine patients may help in decreasing migraine-related disability.
Migraine and DED may share some common pathophysiologic mechanisms, which have been highlighted in some previous reviews. 34 Pathophysiologically, migraine is now considered an inflammatory state involving trigeminovascular pathways with peripheral and central sensitization. It is postulated that a sterile neurogenic inflammation with the release of multiple neuropeptides, including calcitonin-gene-related peptide (CGRP), may drive the pain cascade during a migraine attack. Considering the close association between the trigeminal nerve and the lacrimal functional unit, neurogenic inflammation may create an environment promoting DED. 11 DED, especially with a hyper evaporative underlying pathology, causes tear film instability, accompanied by tear film hyperosmolarity, which induces a cascade of inflammatory events with potential damage to the ocular surface.4,14 This may result in peripheral sensitization predisposing to recurrent migraine attacks in susceptible individuals.
This study has its strengths and limitations. The strengths include adequate sample size, comprehensive migraine and dry eye parameters assessment, severe DED, and comparative analysis between EM and CM. An important limitation of this study is the lack of the evaluation of psychiatric co-morbidities and systematic documentation of remote use of anticholinergic medications in cases and controls that could have resulted in dry eye conditions. This is especially true for drugs like amitriptyline, which can cause significant anti-cholinergic side effects. Other limitations include a need for more objective assessment tools for DED, such as measurement of tear osmolarity and nerve fiber density by confocal microscopy, which would have further increased the diagnostic accuracy. Also, the study's cross-sectional nature precludes any definitive inference regarding the causal association. Despite these limitations, this study had some novel findings, such as an increased presence of DED and severe DED in migraine patients compared to controls. Also, it showed that increased migraine severity and chronicity were associated with increased subjective symptoms and objective signs of DED, and the CM patients have more severe DED than EM patients. Lastly, this study for the first time showed that the migraine patients with DED were more disabled compared to those without DED. These novel findings indicate that the identification and management of comorbid DED may improve the disability outcome in migraine patients.
Footnotes
Clinical implications
Both episodic and chronic migraine patients had significantly more DED symptoms and a higher presence and severity of DED compared to non-migraine controls. Migraine patients with DED had a positive association with headache severity, duration and frequency. Migraine with aura and chronic migraine patients were more symptomatic for DED compared to those without aura and episodic migraine respectively. Migraine patients with DED, especially severe DED, were significantly more disabled compared to non-migraine controls.
Acknowledgements
None
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical statement
The institutional ethics and scientific committees of the Hindu Rao Hospital, New Delhi, India, approved the study. Informed consent was obtained from all the patients, and patient confidentiality was ensured.
