Abstract
Rather than a localized alteration, increased visual reactivity in migraine patients seems to result from a complex interaction between several brain structures, mostly involving the ventral attention network. The hub of this network is the right temporo-parietal junction. In this report, complementing our previous findings, we describe the differences in seed-to-voxel resting-state functional connectivity seeded in the right temporo-parietal junction (right angular gyrus) between migraine patients and healthy controls. Resting-state functional MRIs of episodic migraine without aura patients in the interictal period (n = 19) and matched healthy controls (n = 19) were analysed. With the seed placed in the right temporo-parietal junction (right angular gyrus), seed-to-voxel connectivity was compared between groups. Electrophysiological, voxel-based morphometry (both groups) and specific region of interest (ROI)-to-ROI functional connectivity (migraine patients) data have already been published. Migraine patients showed a higher positive interaction between the right temporo-parietal junction and both temporal poles and a higher negative interaction between this same region and bilateral areas of the visual cortex. On the basis of our results, and because of their established properties as multisensory integration hubs, it is likely that the right temporo-parietal junction and both temporal poles are involved in the altered processing of sensory stimulus commonly observed in migraine patients. Therefore, more attention should be paid to these regions for migraine research in the future.
Introduction
Cumulative evidence has shown that the brain of migraine patients exhibits enhanced responsiveness to several stimuli, 1 to the extent of cataloguing migraine as a disorder of sensory processing. 2 For the case of visual responsiveness, in a recent study, we have reported how rather than a localized alteration, increased visual reactivity in migraine patients seems to result from a complex interaction between several brain structures, mostly involving the ventral attentional network. 3 This is in line with the current understanding of cerebral physiology, where most cerebral functions are comprehended as multi-aerial processes, neither localized nor limited to single cortical regions.
The ventral attentional network is in charge of directing our attention towards salient, behaviourally relevant stimulus, a mechanism that is likely altered in migraineurs. 4 –6 The hub of this network, the right temporo-parietal junction, coordinates the biggest part of this process. Alterations in this region in groups of migraine patients have been repeatedly described in the literature. 3 In this brief report, complementing our previous findings, 3 we describe the differences in seed-to-voxel resting-state functional connectivity seeded in the right temporo-parietal junction (right angular gyrus) between migraine patients and healthy controls.
Materials and methods
Twenty patients with episodic migraine without aura in the interictal period and 20 matched healthy controls underwent 3 T BOLD resting-state functional MRI (Allegra scanner; Siemens AG, Munich, Germany). Because of technical issues, MRIs from two participants (one from each group) had to be excluded from the analyses. Descriptive statistics of the 38 remaining participants are summarized in Table 1. Scans were performed in the Centre Hospitalier Universitaire de Liège (Pr R. Hustinx, Dr L. Tshibanda). Acquisition parameters are described in detail in the original study. 3 Data were preprocessed and analysed using SPM12 (Wellcome Trust Centre for Neuroimaging, http://www.fil.ion.ucl.ac.uk/spm) implemented in MATLAB 16 (Mathworks Inc., Sherbom, Massachusetts, USA) and CONN connectivity toolbox (Gabrieli Lab, McGovern Institute for Brain Research, Massachusetts Institute of Technology, Cambridge, Massachusetts, USA). 7 With the seed placed in the right temporo-parietal junction (specifically, a normalized-space region of interest in the right angular gyrus), seed-to-voxel connectivity was compared between migraine patients and healthy controls. This specific region was selected on the basis of a previous study suggesting its strong involvement in visual processing. 3 Positive and negative contrasts were carried out separately. An exploratory (p < 0.001 uncorrected, cluster size threshold to n < 20 voxels) analysis followed by a more stringent comparison (p family-wise error (FWE) < 0.05 correction at the whole brain level) were performed. Under the same parameters, connectivity of the left temporo-parietal junction (left angular gyrus) was evaluated for comparison purposes. This study was approved by the Institution’s ethics committee (Centre Hospitalier Régional de la Citadelle, Liège, Belgium – protocol n°1422). Written informed consent was obtained from all participants.
Gender and age of the participants.

Results
Migraine patients showed an increased positive interaction between the right temporo-parietal junction (right angular gyrus) and both temporal poles and an increased negative interaction between this same region and bilateral areas of the visual cortex on exploratory analyses (Figure 1; Table 2). No voxels on either contrast were statistically significant at a 0.05 peak-voxel p[FWE]-corrected threshold.
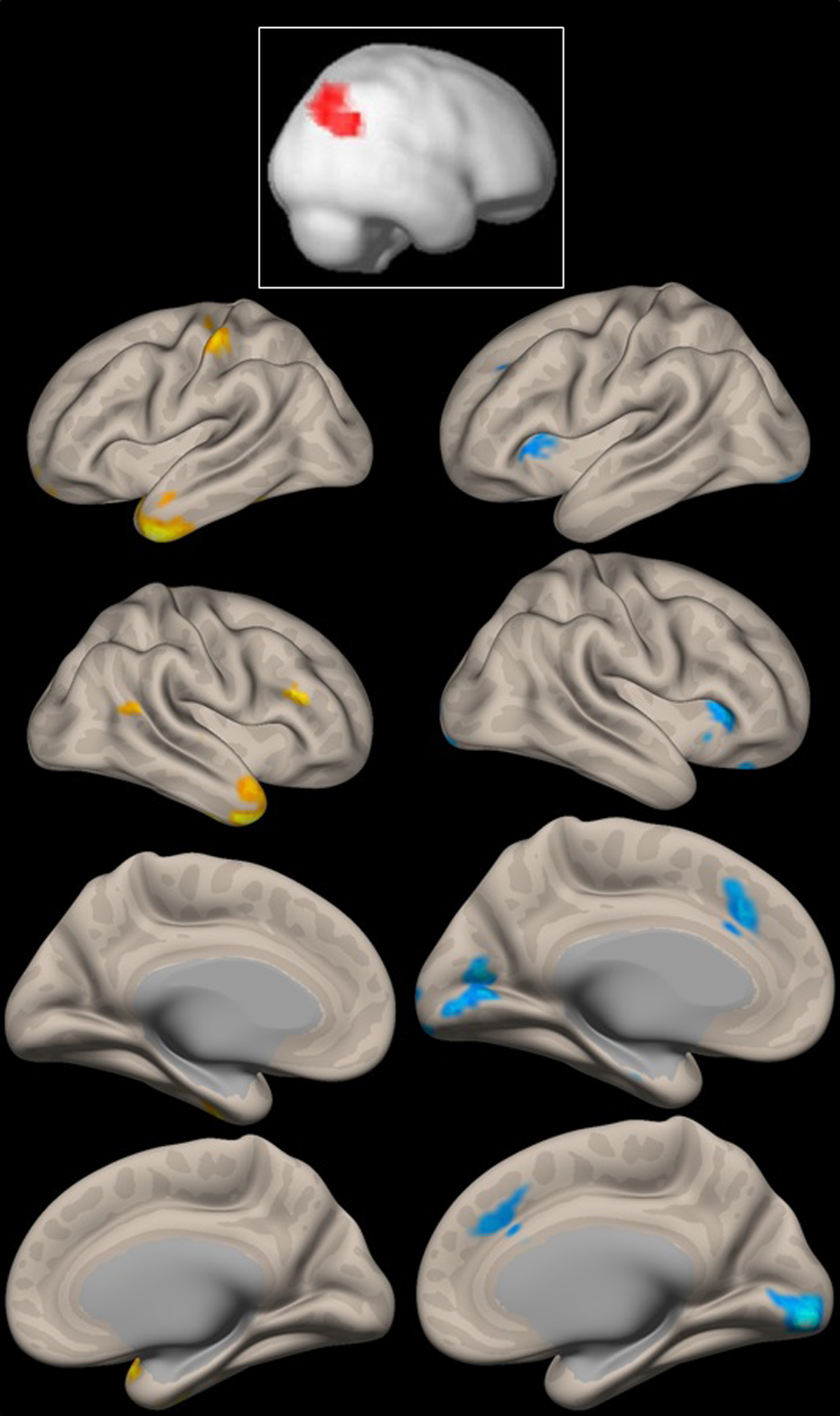
Top: Seed in the right temporo-parietal junction (right angular gyrus). Columns: Voxels where functional connectivity seeded in the right temporo-parietal junction is higher in migraine patients with respect to controls. Left column: positive contrast; right column: negative contrast. The p-value is set to <0.01 for displaying purposes. For details, see text.
Increased resting-state functional connectivity in migraine patients with respect to healthy controls.a

a Peak voxel coordinates, size, uncorrected p-value and anatomical location of positive and negative and negative contrasts were analysed.
Discussion
The main finding of this study is the presence of increased functional connectivity between the right temporo-parietal junction and the temporal poles in migraine patients with respect to the healthy controls. In addition, we show that the negative interaction between this same seed and the visual cortex that we have previously delineated using slightly different methods 3 is stronger in migraineurs.
During the last decade, on the basis of experimental findings, interest on the possible implication of the temporal pole in migraine’s pathophysiology has progressively increased. 8 –13 Indeed, although numerous species present a temporal cortex, the temporal pole is almost unique to humans and non-human primates, with a relatively recent development in terms of brain phylogeny. 14 Given its function in multimodal sensory integration, the possibility that the temporal pole is involved in migraine does not result surprising. This structure receives afferents from visual, auditory and olfactory cortices, which process information of the senses commonly irritated to a ‘phobia’ degree during migraine attacks. 15 Furthermore, it sends projections to numerous brain structures also linked to migraine disorders, such as the amygdala, the orbitofrontal cortex and, most notably, the hypothalamus, explaining the autonomic responses that take place when the temporal pole is stimulated. 15
Particularly in migraine, increased regional cerebral blood flow with respect to controls was observed in the temporal pole following olfactory stimulation. 8 In another experiment, in line with our findings, anodal (excitatory) transcranial direct current stimulation over the left temporal pole was capable of reverting abnormal visual responsiveness in migraineurs. 16 The absence of modifications for somatosensory responses reported in the same study underlines the connectivity patterns of this structure mentioned in the paragraph before. Finally, in one large imaging study, interregional cortical-thickness correlations with the right temporal pole helped to distinguish migraine patients from healthy controls at the structural level. 12 There is thus converging evidence linking this specific region with migraine, with a plausible involvement on the sensory alterations observed in the disease. However, further research is warranted.
Regarding negative interactions, in this study, we observed increased functional anti-correlations between the right temporo-parietal junction and the visual cortex in patients.
This not only underlines a high degree of functional lateralization but provides an insight into the pathophysiology of visual hyper-reactivity in this condition. Indeed, although both the left and right temporo-parietal junctions display increased multimodal (visual, auditory and somatosensory) functional connectivity, 17 the right temporo-parietal junction has a predominant role on directing attention towards salient, behaviourally relevant, visual stimuli, 4 a feature that is likely altered in migraine. 18
To conclude, functional connectivity between the right temporo-parietal junction (right angular gyrus) and the temporal poles is increased in patients with migraine without aura. In the past, to explore sensory hyper-reactivity in migraine, most studies have focused on primary sensory cortices. However, our current understanding of cerebral physiology suggests that cerebral functions are multi-aerial processes. Therefore, and because of their established properties as multisensory integration hubs, more attention should be paid to the right temporo-parietal junction and the temporal poles in the evaluation of enhanced cerebral responsiveness in migraine research in the future.
Footnotes
Acknowledgements
The contribution of the IRCCS - Fondazione Bietti in this article was supported by the Ministry of Health and Fondazione Roma.
Author contributions
Marco Lisicki and Kevin D’Ostilio equally participated in this study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project forms part of the EUROHEADPAIN project – FP7 n° 602633 – and received support from the Fonds d’Investissements de Recherche Scientifique (FIRS) of the CHU de Liège and the G. B. Bietti Foundation IRCCS.
