Abstract
Background and Purpose:
Sleep apnea (SA) is highly prevalent in the stroke population. Testing and treating SA in stroke patients is challenging due to inaccessibility to testing and impaired mobility. To address this problem, we designed and implemented an inpatient diagnosis and treatment program for managing SA in patients with stroke. Our main aim in this article is to assess the feasibility of this program.
Methods:
We tested 83 patients with a portable SA testing device and initiated treatment with auto-titrating continuous positive airway pressure (A-CPAP) for those who were diagnosed with SA during their stay in an inpatient stroke rehabilitation unit (SRU). Patients diagnosed with SA were given a 2- to 4-week trial of A-CPAP in their hospital bed with close follow-up from a sleep medicine service.
Results:
Of the 83 patients tested, 54 (67.5%) had SA and 46 (85%) agreed to a trial of A-CPAP therapy. Of the 46 patients, who trialed A-CPAP, 32 (70%) achieved average daily use of four or more hours and went home with it.
Conclusions:
This program provides a feasible and convenient means of testing and treating SA among stroke patients undergoing inpatient stroke rehabilitation.
Keywords
Many studies have shown that sleep apnea (SA) is highly prevalent in the stroke population. 1 There are two main types of SA, obstructive sleep apnea (OSA) and central sleep apnea (CSA). Compared to the general population, in whom only 3–7% of individuals have OSA, in the stroke population, the prevalence of OSA is much greater at 30–70%. 1 Similarly, compared to the general population, in whom the prevalence of CSA is less than 1%, in the stroke population, the prevalence of CSA is much higher at 6–26%. 2 –4 OSA in stroke patients is also associated with worse functional outcomes, 5 longer hospitalization, 6 increased chance of a second stroke, 7 and increased mortality after stroke 5,8 compared to patients without SA. There is some evidence to suggest that early diagnosis and treatment of OSA can have a positive impact on stroke patients’ recovery. For example, some trials showed that among stroke patients with OSA, early continuous positive airway pressure (CPAP) therapy improved motor and functional outcomes, accelerated neurological recovery, 9 –11 lowered blood pressure, 12 reduced depressive symptoms, 13 and reduced mortality from cardiovascular events. 14 In these trials, diagnosis was all conducted in the inpatient setting, and CPAP treatment was also initiated and continued during the hospitalization. The positive outcomes were all associated with good adherence to CPAP treatment with more than 4 h per night. 9,12 –14 One study also reported that patients’ acceptance to continue treatment at home at the end of hospitalization was quite high at 71%. In this study, patients were initiated on CPAP treatment and were supervised on the ward for more than 1 week. The authors suggested that initiation and intensive coaching of patients on CPAP use during their hospital stay played an important role in maintaining high treatment compliance. 12
On the other hand, there are also several clinical trials that found no significant benefit of treating OSA in the poststroke period with CPAP on cardiovascular morbidity and mortality or stroke recovery. 15–17 However, in two of these studies, CPAP was started in the outpatient setting, 15,17 while in the third, patients were started on CPAP during their acute hospital admission after stroke onset 16 and were discharged soon thereafter. This may have played a role in the negative outcomes of these trials, because CPAP compliance was relatively poor and hours of use may have been inadequate to induce improvements in stroke outcomes. Such inconsistencies limit one’s ability to assess the association between CPAP treatment of OSA and stroke outcomes.
These results demonstrate that OSA treatment-associated improvements in outcomes were observed in those trials with better CPAP compliance and that better CPAP compliance was achieved with intensive inpatient CPAP initiation versus outpatient initiation. Taken together, these observations imply that the longer the time a patient spends in hospital to acclimatize to CPAP treatment, the better the compliance and the easier for them to continue treatment once they are discharged home. Importantly, these studies were all experimental clinical trials. However, in the everyday clinical setting, it is difficult to diagnose patients in hospital early after their stroke due to their impaired mobility and limited access to clinical SA testing. Consequently, the diagnosis of SA is often either delayed or not made, resulting in either delayed treatment with insufficient time to acclimatize to CPAP while in hospital or no treatment at all. In addition, CPAP compliance can be enhanced by interventions such as mask and humidification optimization, topical nasal therapy, and SA education. 18 However, in stroke patients, such interventions can be difficult to accomplish if patients need to make multiple visits to a sleep clinic after discharge from hospital due to impaired mobility and necessity for a caregiver to accompany them. Conversely, such interventions can be applied much more easily during their hospital stay.
Accordingly, it seems that there is greater potential for treatment of OSA to improve morbidity, mortality, and recovery from stroke if the diagnosis is made, and treatment initiated in the inpatient setting. Nevertheless, due to lack of awareness among stroke medical professionals about the potential for SA management to improve stroke outcomes and inaccessibility to a simple and reliable testing process that is easy to apply to stroke patients in a timely manner, SA in the stroke population is underdiagnosed, among both in- and outpatients. 19 Currently, in-laboratory polysomnography (PSG) is the standard means for diagnosing SA. However, it is seldom available for inpatient testing, is costly, and requires overnight supervision by a technician. 20,21 PSG is also inconvenient, especially for stroke patients who suffer from impaired mobility and who may require accompaniment by a caregiver to the sleep laboratory and who may need to remain there overnight. There is also very limited portable SA testing for stroke patients while in hospital, because most portable monitors are relatively complex and require substantial training to be administered by hospital personnel, which is generally impractical. Consequently, it is more common that stroke patients are scheduled for PSG testing once they are discharged. However, in our experience, testing and follow-up can be delayed by months after their stroke, and patients often choose not to be tested due to their physical limitations and difficulty scheduling for both them and their caregivers.
In view of the above, we have designed and implemented a stroke and sleep apnea management (SSAM) program in the stroke rehabilitation unit (SRU) of the University Health Network Toronto Rehabilitation Institute (TRI) to offer early testing and treatment of SA for stroke patients in the inpatient setting. In order to provide inpatient SA testing, a simple and accurate testing method is needed. To this end, investigators at TRI have developed a portable SA diagnostic device (BresoDX®, BresoTEC Inc., Toronto, Ontario, Canada) that can be easily administered in a person’s home or in the inpatient setting (see description subsequently and Figure 1). Following SA testing, sleep medicine consultation, treatment planning, and follow-up visits with patients and their families to initiate and maintain compliance with auto-titrating CPAP (A-CPAP) (if applicable) is implemented in the inpatient setting. The SSAM program aims to: (1) determine the feasibility of diagnosing SA and initiating treatment in stroke inpatients in an SRU using a portable, single-user device to diagnose SA and A-CPAP to treat it, (2) evaluate A-CPAP tolerance and compliance while in the SRU, and (3) evaluate treatment compliance after discharge from inpatient rehabilitation. This article will focus on the first two aims.
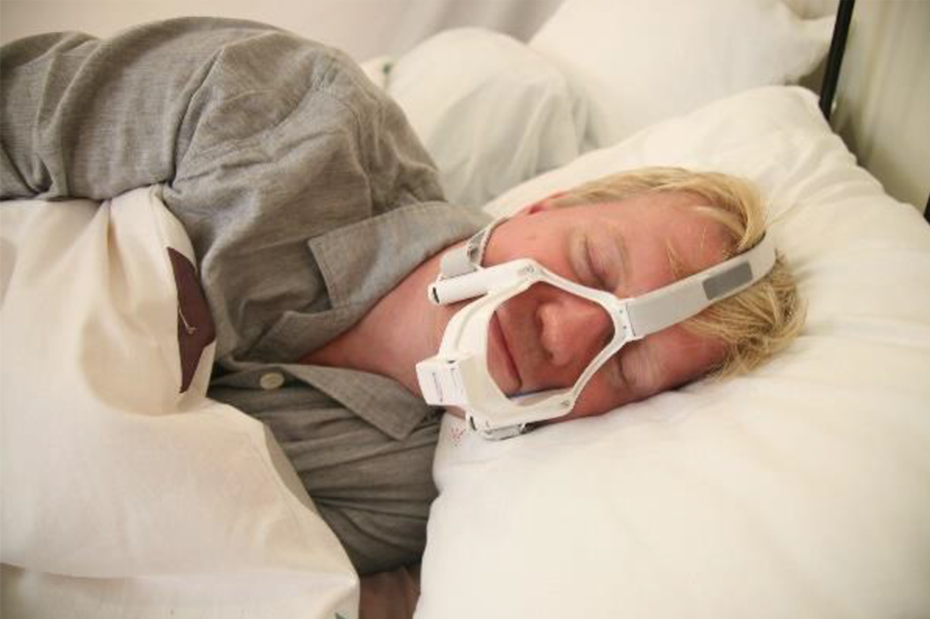
Portable sleep apnea testing device in use.
Description of the SSAM program
Patients
Inclusion criteria for the SSAM program are (1) men and women ≥18 years of age; (2) with an embolic, thromboembolic, or hemorrhagic stroke confirmed by clinical assessment and computerized tomography or magnetic resonance imaging of the brain admitted to the TRI SRU within 4 weeks of stroke onset; (3) participating in rehabilitation with an estimated length of stay of at least 2 weeks; and (4) able to follow simple commands in English. Exclusion criteria are (1) severe dysphagia requiring percutaneous endoscopic gastrostomy or nasogastric feeding or an otherwise increased risk of aspiration when wearing an A-CPAP mask; (2) craniectomy without bone flap replacement; (3) patients unable to remove a face mask independently in case of emergency; (4) severe aphasia preventing informed consent; (5) functional independence measure <40; (6) other diseases affecting the central nervous system, such as dementia, acute delirium, or confusion; (7) active psychotic disorder which precludes the ability to follow instructions; (8) stroke secondary to traumatic or anoxic brain injury; (9) severe cardiac or respiratory conditions with hypoxia, or on supplemental oxygen; (10) unwillingness to be treated for SA should it be found on a sleep study; and (11) necessity to sleep with the head of the bed elevated due to the stroke.
Portable SA testing device
SA testing was performed using a portable, single-user, AAA battery-operated, cordless acoustic recording device (BresoDX). It is a lightweight open face frame that is held in place by a head strap during sleep (Figure 1). This device consists of two embedded sensors: (1) a microphone that captures breath sounds from which it derives airflow, apneas, and hypopneas and (2) an accelerometer that captures head position and movement to determine posture and estimate sleep time, respectively. In a general sleep clinic population, it has been validated against simultaneous PSG 22 and in patients’ homes 23 to quantify the apnea–hypopnea index (AHI) and to diagnose SA. It has also been validated for the AHI and diagnosis of SA in stroke patients in the TRI SRU, both during simultaneous PSG and in the patient’s hospital bed. 24 The data from the overnight study are stored on a microSD card that is removed and analyzed automatically by computerized algorithms to determine the AHI, head position, and an estimate of sleep time as previously described. 22,25,26 In case the overnight study needed to be repeated, due to insufficient data collection or ambiguous results, the device was reused in the same patient by replacing the microSD card and batteries.
Protocol
After admission to the SRU, the attending physician orders a portable SA diagnostic test in eligible patients. Just prior to bedtime, a nurse activates and applies the SA diagnostic device to the patient in his/her hospital bed. The next morning, a nurse removes the device. A technician then removes the microSD card and inserts it into a computer that automatically generates a report that includes the AHI, head position, and an estimated sleep time. The report is then sent to both the SRU and the sleep medicine consult service. If the patient’s AHI is 10 or greater, a sleep medicine physician assesses the patient in the SRU. If the sleep physician judges that the patient has an indication to treat SA, an A-CPAP device with built-in adjustable heated humidification (DreamStation Auto CPAP, Philips Respironics, Murrysville, PA, USA) is prescribed. It is then delivered to the patient’s bedroom where it is set up by a respiratory technician who trains the patient and family or other caregiver on how to use and maintain the A-CPAP device. An A-CPAP interface is chosen according to best fit and ease of use for patients with neurological disabilities. A-CPAP is then initiated at night by the patient with assistance from their nurse. Once the patient has started treatment, the sleep medicine service monitors compliance data using encoreanywhere™, a web portal that receives daily patient compliance data from the A-CPAP. The sleep medicine service also visits the patient once or twice a week to monitor the patient’s use of the A-CPAP and make adjustments (such as prescribing a change of mask, and adjusting humidification, etc.) to enhance the patient’s comfort and compliance. During their stay in the SRU, patients are taught how to use the A-CPAP themselves. Patients normally have 2–4 weeks to trial the A-CPAP in the hospital before they are discharged. The sleep medicine service then decides whether the patient should take the A-CPAP home to continue treatment based on his/her hours of use during the hospital stay. When a patient is discharged with an A-CPAP, a follow-up appointment is made for the patient to be seen in the hospital’s sleep medicine clinic 3 months later (Figure 2).

SSAM program protocol. SSAM: stroke and sleep apnea management; SA: sleep apnea; SRU: stroke rehabilitation unit; AHI: apnea–hypopnea index; A-CPAP: auto-titrating continuous positive airway pressure.
Observations
The SSAM program was launched in December 2016, and as of February 20, 2018, 83 patients underwent a BresoDX test. Two patients refused testing and one patient’s recording was not valid because she could only sleep with her upper body elevated after the stroke, which was not representative of her usual sleeping position. Accordingly, she was booked for an outpatient PSG once she had been discharged from the SRU and resumed her normal sleeping position. Eight patients required a second portable SA test for the following reasons: (1) estimated sleep time was shorter than 2 h and the test was deemed inconclusive, (2) one patient with aphasia did not understand that the device needed to be kept on for the entire night and took it off at the beginning of the night, (3) one patient accidentally turned the device off at the beginning of the night, and (4) one patient had been previously diagnosed as having OSA and was being treated with a mandibular advancement device (MAD). While in the SRU, he was found to have severe OSA (AHI = 50) while not wearing the MAD and was given a trial of A-CPAP, which he did not tolerate. He was then retested with the portable SA monitoring device while wearing the MAD and his AHI decreased to 12, indicating that the MAD was reasonably effective in controlling his OSA. Thus, we were able to make a treatment decision that his severe OSA was better managed by the MAD than A-CPAP. In all of the above situations, the second night testing was done using the same device with a new set of batteries and microSD card. This demonstrates the ease with which multiple night testing can be accomplished with this portable SA monitoring device, since it is a personal device. Of the 80 patients who had valid portable SA tests, 54 (67.5%) had an AHI ≥ 10 and were diagnosed as having SA. This diagnostic rate is comparable to that reported in the literature. 1 Of these 54 patients, 12 had mild SA (AHI of 10 to 15), 16 had moderate SA (AHI of 15 to <30), and 26 had severe SA (AHI ≥ 30).
Of the 54 patients with an AHI of 10 or more, 46 (85%) accepted a trial of the A-CPAP treatment while in the hospital, while eight refused. A-CPAP uptake, compliance, and efficacy are shown in Table 1. The sleep medicine service visited these patients regularly with the aim of having them use A-CPAP at least 4 h/day and to keep their AHI below 10. If patients used A-CPAP less than 4 h/night, or the AHI was more than 10, the sleep medicine service made adjustments to the treatment accordingly. This approach included: (1) working with the patient or their caregiver on fitting their mask and teaching them how to put it on and adjust the straps to maximize comfort and minimize air leak; (2) changing masks if the current one was leaking or was not comfortable; and (3) educating patients and their caregivers on the relationship between SA and stroke, and how treating SA can improve recovery from stroke, thus motivating them to use A-CPAP. Their A-CPAP use generally improved over time. Of the 46 patients who trialed A-CPAP, 32 patients had average use of 4 or more hours per day at the end of their SRU stay and took the A-CPAP home. This means that 70% of patients who started A-CPAP treatment in the hospital continued the treatment with good compliance and decided to carry on with the treatment at home. The high rates of A-CPAP uptake and treatment compliance indicate a relatively high degree of SA treatment success in this inpatient setting. Thus, our experience in the SSAM program provides evidence that SA can be diagnosed and treated expeditiously in stroke inpatients. It also suggests that initiating therapy in such patients, who are limited by motor and/or cognitive impairment, is best accomplished in-hospital where close follow-up, which could not be accomplished in the outpatient setting, is possible.
A-CPAP uptake, compliance, and efficacy.a

A-CPAP: auto-titrating continuous positive airway pressure; AHI: apnea–hypopnea index.
a Data are expressed as number or mean ± standard deviation.
There are some limitations to the SSAM program. First, sleep disorders other than SA cannot be diagnosed with the portable SA testing device. Therefore, when other sleep disorders are suspected, especially if portable testing is negative for SA, PSG may need to be performed. Second, presently, the portable SA testing device used in this program does not distinguish central from obstructive events. Therefore, if CSA is present, A-CPAP may not be effective in suppressing it. In that case, PSG may also be necessary to make the distinction, to facilitate prescription of the appropriate therapy. However, several studies have demonstrated that in the stroke population, the great majority of cases of SA are obstructive. 1–4 Third, the SSAM program has not been in existence long enough to analyze outpatient clinic follow-up data, so that we do not know as yet whether A-CPAP compliance remained good following discharge from hospital.
In summary, this SSAM program provides a feasible and convenient means of testing and treating SA among stroke patients in the inpatient setting. Many factors contributed to the success of the program. These include (1) the inpatient design of the program made timely testing and treatment for SA feasible in disabled stroke patients and facilitated high diagnostic and treatment compliance rates; (2) the efforts of a multidisciplinary medical team who worked well together to coordinate SA testing, treatment and follow-up; (3) use of a simple, accurate, and easy to use personal portable SA testing device that required minimal time to train the nursing staff to administer; (4) use of A-CPAP with remote monitoring capabilities, so that the treatment could be instituted in the patient’s hospital bed; (5) close monitoring and follow-up by the sleep medicine service to maximize A-CPAP comfort, effectiveness, and compliance; and (6) the streamlined process required little additional work by physicians, nurses, and allied healthcare workers in a busy clinical setting and therefore was well accepted by staff and patients alike. These early observations suggest that similar inpatient SSAM programs could be implemented in other stroke units to improve access to SA testing and treatment in this vulnerable population.
Footnotes
Acknowledgements
The authors would like to acknowledge the assistance of Dr Mark Bayley in the design and support of this program.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This program was supported by the University Health Network Toronto Rehabilitation Institute Foundation. The work of TDB was supported by the Clifford Nordal Chair in Sleep Apnea and Rehabilitation Research and the Godfrey S Pettit Chair in Respiratory Medicine.
