Abstract
Digital blocks are routinely used for excision of lesions. We describe a unique presentation of digit necrosis after excisional biopsy with digital block and finger tourniquet in a pregnant patient with a history of ulcerative colitis. The patient had a history of a long-standing painful dorsal PIP joint mass and was scheduled for excision under local anaesthetic. On the day of the procedure, she disclosed that she was pregnant in the second trimester. After extensive discussion of risks and benefits between the patient and the surgeon, the decision was made to proceed with an excisional biopsy of the lesion because of its impact on her quality of life. Twelve hours after the procedure, she presented to the emergency department with blistering and severe pain to the digit. Doppler ultrasound showed flow through both digital arteries and the digit appeared viable. Over the coming days her pain continued to worsen and on post-operative day 3, she was admitted to hospital for attempted salvage of the digit using conservative methods. Her digit went on to demarcate at the level of the middle phalanx. Five weeks after her initial procedure, the patient underwent partial amputation of the small finger at the level of the DIP joint and 2-stage groin flap for soft tissue coverage. We discuss the effects of pregnancy and ulcerative colitis on thromboembolic events, and review the literature on digital blocks, digital tourniquet use and management of early digit necrosis. This case highlights the importance of delaying elective hand procedures in pregnant patients, especially if they have additional comorbidities such as pro-thrombotic diseases like inflammatory bowel disease.
Introduction
The impact of pregnancy and inflammatory bowel disease on elective hand procedures are currently unknown. This case report presents a pregnant patient with ulcerative colitis who sustained digital necrosis requiring partial amputation of her right small finger and soft tissue coverage after elective removal of a benign lesion. Ulcerative colitis has been implicated in both arterial (ATE) and venous thromboembolic events (VTE), with several reported cases of embolic events in the upper extremity. 1-3 However, all reported cases are in the setting of spontaneous embolic events not associated with surgery; 1-3 the effect of this disease in the setting of elective procedures is unknown. Similarly, pregnancy is a hypercoagulable physiological state, with increased rates of thromboembolism reported following abdominal surgery in comparison to their non-pregnant cohort. 4 No studies of complications after elective hand procedures in this patient population exist. This case report highlights the inherit risks of elective hand surgery in patients who are pregnant with underlying inflammatory disease, and is the first case report found in the surgical literature.
Patient Information, Clinical Findings, and Diagnostic Assessment
The CARE Case Report Guidelines were used to guide the write-up of this case report. 5 A 34-year-old female office worker with ulcerative colitis (UC) presented with a 1-year history of a painful dorsal mass of her dominant hand small finger PIP joint. She had had not sought treatment for this previously. There was no personal or family history of hand masses; there was no history of Raynaud’s phenomena or other hand-related concerns. Her past medical history was only significant for UC which was well-controlled with long-standing Pentasa and Imuran. She was a lifetime non-smoker. On physical exam, the mass was located on the dorsum of the small finger PIP joint. It was tender to palpation. The small finger was neurovascularly intact. Ultrasound workup was consistent with a ganglion cyst. She was scheduled for elective removal of the mass.
The timeline of events is shown in Figure 1.

Timeline of Events. POD: post-operative day, POW: post-operative week
Timeline, Therapeutic Intervention, Follow-Up, and Outcomes
On the day of her procedure, the patient disclosed she was 14 weeks pregnant. After extensive discussion of risks and benefits with her surgeon, the decision was made to proceed with excision given the painful nature of the lesion and the impact on her quality of life. Consent for the procedure was obtained. A dorsal digital block using 5 cc of buffered 50/50 mix Marcaine/lidocaine with 1:200,000 Epinephrine was infiltrated into the right small finger. A digital tourniquet (penrose drain) affixed with a snap was used for the duration of the procedure. The skin was incised using a dorsal longitudinal incision over the PIP joint. The lesion appeared solid in nature and adherent to the extensor tendon mechanism (pathologic diagnosis: fibromatosis). It was carefully removed from the extensor tendon. The wound was closed using simple interrupted sutures and the tourniquet was removed. The digit was well perfused at the conclusion of the procedure. A dressing of adaptic and gauze was applied.
On the evening of the procedure, the patient presented to the Emergency Department with severe digital pain and blistering. She was evaluated by the plastic surgeon on call. She denied the use of a hot compress which may have burned the insensate skin after her procedure. Vital signs were stable and the digit appeared neurovascularly intact. A doppler ultrasound showed flow through both digital arteries. A discussion about the role for phentolamine was had. However, given the patient’s presentation 12 hours after the procedure it was felt there was no longer any role for phentolamine given that the effect of epinephrine had worn off, and the risk for further impaired flow with additional fluid volume into the digit. Elevation of the hand was recommended, and close follow-up was arranged.
On post-operative day (POD) 1, the patient was seen in clinic by her surgeon. On examination, capillary refill was present at all levels of the digit including the tip. Light touch was diminished on both the ulnar and radial side. There was blistering around the nail fold with no obvious swelling or ecchymosis around the base of the digit. A provisional diagnosis of injection injury to bilateral neurovascular bundles was made in the setting of a viable digit but decreased inflow. She was given medications to manage her pain and told to follow-up in 4 days or earlier as required. On POD 3, she re-presented to the emergency department with worsening pain. On assessment, ecchymosis extended from the DIP joint to the tip, with decreased capillary refill. Sensation was further decreased on both the ulnar and radial sides. She was admitted to hospital. Conservative measures including warming, elevation, nitroglycerin paste, and heparin soaks were started in an attempt to salvage the digit. On POD 4, the digit tip progressed to necrosis with no blood flow on pinprick. After extensive discussion with the patient and her husband, decision to await full demarcation of the digit was made. Consideration for hyperbaric oxygen therapy was made, but the patient did not quality because of her pregnancy. The patient was discharged home with close follow-up.
By POD 6, digit necrosis extended to the DIP joint and by POD 12 there was clear demarcation to the midpoint of the middle phalanx. A second opinion form colleagues was obtained weighing the options of possible debridement and groin flap coverage or more proximal revision amputation. Unfortunately, in the intervening 3 weeks the patient sustained a late second trimester miscarriage. In an attempt to preserve length, the patient wished to go ahead with groin flap soft tissue coverage. This flap has been used to for this purpose in individuals who sustained revision amputations from trauma, 6 burns, 7 and in complex hand injuries. 8 The flap was chosen as the patient preferred not to violate any other fingers for the donor site, use a reliable reconstructive option in light of a complication, and in the event of compromise a cross-finger flap would still be available. Five weeks after her initial procedure, the patient was booked for a revision amputation of the DIP joint and underwent the first stage of groin flap for soft tissue coverage. She underwent division of groin flap and tip contouring 5 weeks after the initial stage (post-op week 10). See Figure 2: Post-operative day 0, 3, 4, and post-reconstruction.
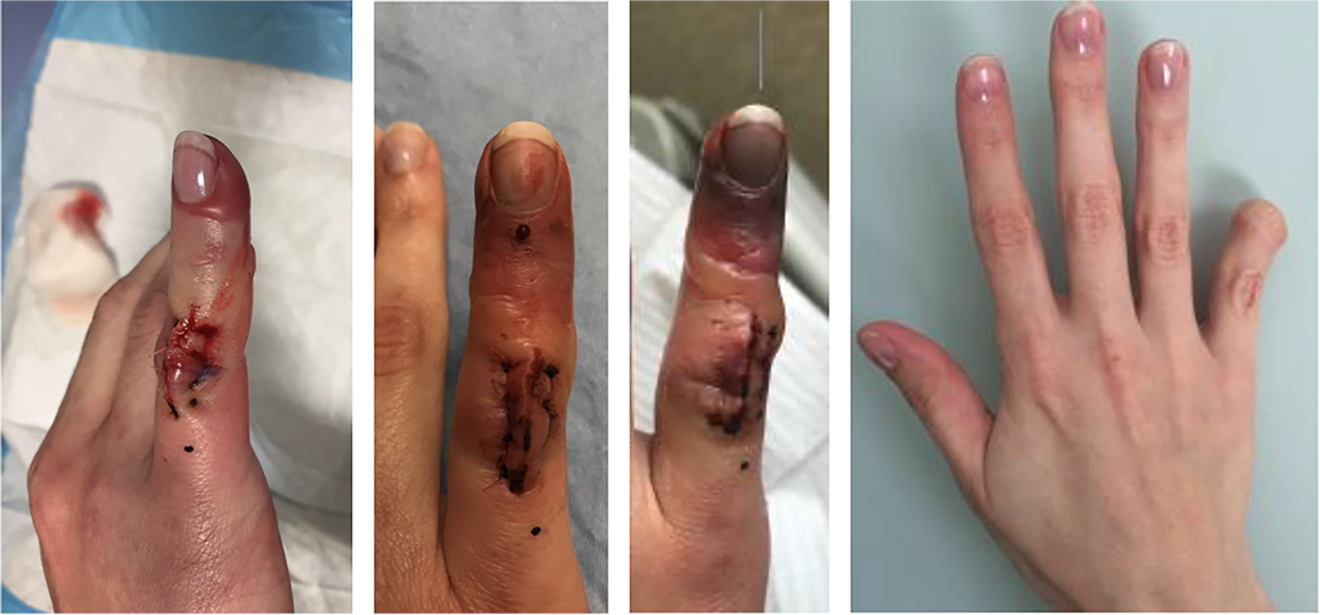
Post-operative day 0, 3, 4, and post-reconstruction. Legend: from left to right: post-operative day
Discussion
We present a case of digital necrosis after elective hand procedure under digital block and finger tourniquet requiring partial amputation of her dominant small finger and soft tissue coverage with a groin flap. This case report highlights the inherit risks of elective hand procedures in patients who are pregnant and have underlying inflammatory disease. It is the first reported case of digital necrosis in pregnancy found in the surgical literature.
Effects of Ulcerative Colitis and Inflammatory Conditions on Thromboembolism
Ulcerative colitis (UC) has been implicated as a risk factor for ATE and VTE. 9 -15 Specifically, patients have a 3fold increased risk of deep vein thrombosis (DVT) and pulmonary embolism (PE) compared to the general population. 15 There are a number of case reports describing spontaneous thromboembolism in the upper extremity in the setting of UC. 1 -3 One case reports describes a 58 year old woman with a history of severe UC presenting with severe ischemic rest pain due to a brachiocephalic trunk thrombosis resulting in ipsilateral hand microembolism. She was treated successfully with IV unfractionated heparin and transvenous lysis block of the forearm. 1 Another case report describes a 47 year old male treated for new onset UC with brachial, radial, and ulnar arterial thrombi. He required a distal brachial artery arteriotomy and Fogarty catheter removal of the thrombus with a 14-day course of heparin. 2 A third case report describes a 58 year old male with a history of UC who presented with a left upper extremity and neck thrombus treated with low molecular heparin with complete resolution of symptoms. 3 Finally, a 36-year-old male with severe UC sustained spontaneous necrosis of the distal thumb and index fingers after late presentation for symptoms that started 3 weeks prior. Digital arterial thrombosis was thought to be responsible for his presentation. 16 All of these case reports describe patients with spontaneous thrombi in the setting of new onset to severe UC. No case reports describe thromboembolic events in patients with UC in the setting of upper extremity surgery.
Pregnancy
Pregnancy represents a procoagulable state 17,18 with estimated rates of thromboembolism 4 to 5 times higher than non-pregnant women of the same age. 19,20 Specifically, 75-80% of pregnancy-associated VTE are deep vein thrombosis with approximately half occurring perinatally and the reminder in the post-partum period. 19 ATE represents approximately 20 to 25% of all thromboembolic events, with stroke being more common than myocardial infractions. 21 Physiological changes associated with VTE in pregnancy include increased coagulation factors (fibrinogen, factor VIII, von Willebrand factor), decrease in natural anticoagulants (specifically, protein S), increased venous distention, decreased venous outflow, and decreased mobility. In addition, personal risk factors including a history of thrombosis, thrombophilia, increased age, and high body index may contribute. 18,19 Systemic low-molecular weight heparin has been shown to be safe in pregnancy and as such, is the anticoagulant of choice for treatment of thromboembolic events. 22
Surgery in Pregnancy
In Canada, it has been estimated that approximately 1-3% of pregnant women undergo nonobstetric surgery, 23 similar to the rates seen globally. 24 Nonelective gastrointestinal (GI) and trauma surgeries are the most common. 25 Goals of perioperative care include appropriate positioning, elevated oxygenation, appropriate anesthetic drugs, preventing aspiration and hypothermia, and monitoring of fetal heart rate. Information on elective surgery in pregnancy is much more sparse. The American College of Obstetricians and Gynecologists (ACOG) recommends that elective nonobstetric surgery be postponed until after delivery, but there are no guidelines on procedures done under local anaesthesia. 26 Of note, lidocaine has not shown any teratogenicity 27 and is deemed safe to use by the American Society of Anesthesiologists Task Force on Obstetric Anesthesia and the Society for Obstetric Anesthesia and Perinatology. 28
Literature on plastic surgery procedures performed in pregnancy is scarce. A limited number of case reports describe an above-elbow arm replantation, 29 a free TRAM flap surgery for an anterior craniofacial defect with orbital exenteration, 30 and a combined latissimus dorsi-serratus anterior free flap for a degloved foot and ankle with a Gustilo IIIB fracture. 31 None of these cases report thromboembolic events. A single set of guidelines during microsurgery procedures in pregnancy have been published. 32 Recommendations are similar to those above with additional microsurgical considerations including use of anxiolytics to decrease anxiety related to bedrest, use of anticoagulants, vasodilators, and antibiotics.
Use of Epinephrine in Digital Blocks
The use of epinephrine in digital blocks has been widely debated. Numerous studies suggest the safety of dilute epinephrine in digits. Chowdhry et al (2010) reviewed 1,111 patients undergoing hand procedures. No cases of digital gangrene were noted in patients who underwent digital block with lidocaine and 1:100,000 Epinephrine Chowdhry et al (2010). 33 Another large case series showed no cases of digit loss with lidocaine or bupivacaine and epinephrine (1:100,000) in 3,110 hand/finger blocks. 34 A literature review examining 63 articles (12 of which were randomized controlled trials) encompassing 2,797 digital nerve blocks with epinephrine were performed without digital necrosis or gangrene. 35 Some older case reports do present patients with digital necrosis when epinephrine was used. Criticisms of these reports include the use of cocaine with epinephrine to slow the absorption of the local anesthetic, 36,37 the use of procaine, 38,39 or unknown concentrations of epinephrine. 34,37 Although unlikely, epinephrine with local anesthetic may have contributed to the digital necrosis.
Volume used in Digital Blocks
Digital blocks can be done via two dorsal (subcutaneous) or a single volar (transthecal) injections. 40,41 An RCT examining double dorsal versus single volar digital subcutaneous anesthetic injections for emergency department finger injuries showed similar pain levels for injections as well as success rates of anesthesia. 40 This finding was replicated by Williams and Lalonde in a group of volunteers who had both two-injection dorsal and volar subcutaneous local anesthetic injections. 41 The authors found that subjects preferred volar over dorsal blocks. 41 In both studies, no evidence of VTE complications were found.
Digital Tourniquet Techniques
Digital tourniquet techniques can result in neurovascular injuries as well as digital ischemia. A study using 400 volunteers examined the pressure of common tourniquet methods. The authors found the highest pressure recorded for the penrose drain was 727 mmHg, for the clamped rolled glove 439 mmHg, for the unclamped rolled glove 267 mmHg, for the tourni-cot 246 mmHg, and the T-ring 151 mmHg. While all methods were successful in occluding flow to the digit, only 3 methods were deemed safe: the unclamped rolled glove, the tourni-cot and the T-ring. 42 The recommended maximum pressure for upper extremity tourniquets is 300mmHg 43 with neurovascular injuries reported in pressures greater than 500 mmHg. 44,45 Many reports have suggested that excessive pressure from digital tourniquet use resulted in multiple complications including additional surgery or amputation, VTE, nerve injuries, or post-operative edema. 43,44,46 Further, the use of a digital tourniquet and local anesthetic with epinephrine have been used in individuals requiring additional hemostasis as was shown here. For example, an RCT randomizing 60 digital blocks to those with local without (arm 1) and with epinephrine (arm 2), requiring additional tourniquet use on top of the local with epinephrine in 9 of the 31 blocks in arm 2 (29.0%) resulting in no complications. 36 In this case report, the routine use of a clamped penrose drain may have contributed to this patient’s neurovascular injury.
Management of Early Digit Necrosis
Management of early digit necrosis includes differentiating between an arterial and venous etiology. In venous compromise, the finger presents as a blue/purple, edematous finger with increased capillary refill. Management includes the use of elevation, local and systemic anticoagulants, and leech therapy. In arterial compromise, the digit appears cold and pale with delayed capillary refill, and does not readily bleed when pricked with a needle. Management includes the use of warming, vasodilatory medications, and both local and systemic anticoagulants.
Case Discussion
This case report suggests that the combination of a hypercoagulable state of both pregnancy and UC, in addition to the use of a penrose finger tourniquet resulted in digital necrosis. Conservative measures for early management included the use of heparin, nitroglycerin paste, as well as elevation and warming of the digit. Doppler ultrasound of the digital arteries did not show signs of thrombosis. However, it is possible that thrombosis could have occurred more proximally in areas not assessed at time of presentation. Intra-arterial injection injury is possible but less likely given that both digital arteries would have to be involved. Given that the patient presented to the Emergency Department over 12 hours after the procedure, the use of phentolamine was not indicated as epinephrine would have worn off.
Take-Away
This case study reports the first case of digital necrosis in a pregnant female with long-standing ulcerative colitis following an elective hand procedure. This study suggests the need to change practice with 1) avoiding non-life or limb-threatening procedures in pregnancy until the post-partum period, especially in those patients with co-morbidities and 2) using a single volar digital block to decrease the volume of local anesthetic used, and a low pressure digital tourniquet. Finally, this case report highlights the need for plastic surgery guidelines in the pregnant population in order to better meet the needs of this patient population.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was obtained from all patients for being included in the study.
Informed Consent
Informed consent was obtained from the individual participant included in the study.
