Abstract
Reducing false negative rates for sentinel lymph node biopsies (SLNB) in melanoma is important to accurately prognosticate and to guide treatment. Traditionally, SLNB has been performed with the adjunct of radiotracers and blue dye. Although sentinel node mapping is highly successful in axillary and inguinal node basins, identification of nodes in the head and neck is not as accurate with traditional methods. One reason for this may be failure of radiotracer migration. To augment standard technique using a radiocolloid, indocyanine green (ICG) combined with near infrared spectroscopy (NIRS), has shown promising results. We demonstrate a case of an individual undergoing SLNB in the head and neck region with failure of radiotracer migration. Identification of a sentinel node was accomplished with the use of ICG and NIRS. This technology offers an opportunity to salvage the SLNB when traditional methods fail.
Introduction
Sentinel lymph node biopsy has become part of the standard of care for melanoma, particularly for T1b lesions and above. 1 The status of the sentinel lymph node is the most important prognostic factor for survival. 2 Despite this, false negative rates, in which there is a melanoma recurrence in a nodal basin with a previous negative sentinel lymph node biopsy (SLNB), can be as high as 20%. 3,4 There are several proposed explanations for this, including factors arising from injection of radiotracer, pathologic analysis, and surgical technique. Additionally, while sentinel node mapping of the axilla and inguinal regions is highly successful, accuracy diminishes in the head and neck region and ectopic sites, such as the popliteal or epitrochlear area. 5
Traditionally, SLNB has been performed with a dual technique using a radiocolloid and a blue dye. Blue dyes have certain drawbacks, including allergic reactions and skin discolouration as well as inferior localization rates when used as a single modality. 6,7 Radiocolloids alone do not allow for real time visualization of lymphatics. Alternatives to blue dye, which would similarly allow visualization of lymphatics in real time but reduce the risk of allergy are desirable.
Indocyanine green (ICG) was first reported as an alternate to blue dye in 2009. 8 Similar to blue dye, ICG is injected intradermally after anaesthesia induction and detected in real time with the assistance of a near infrared imaging device during dissection of the sentinel lymph node. A number of reports describe improved detection of sentinel nodes with ICG use in addition to traditional radiocolloid. 9 A recent systematic review has identified the potential usefulness of ICG as an adjunct to traditional sentinel node biopsy techniques. 10
Herein we demonstrate the use of ICG in the case of a man undergoing a SLNB of the head and neck area for a melanoma located at the angle of the mandible. In this individual, radiotracer failed to migrate. Without the use of ICG, SLNB would not have been possible and the procedure aborted. We also identify an additional patient in which gamma probe did not allow detection of all nodes seen by lymphoscintigraphy. Once again, ICG allowed all nodes to be identified.
Case Presentation
A 22 year old male presented to the Cutaneous Malignancy clinic with a 1.1 mm, Clark III, non ulcerated, mitotic rate of 2, melanoma of the left mandibular angle. Using NCCN guidelines, this patient was offered a wide local excision and SLNB.
This patient underwent the routine institutional lymphoscintigraphy protocol with technetium-99 sulphur colloid administered by the nuclear medicine physician the morning of his procedure. Despite the routine waiting period, no migration of radiotracer was detected.
The TruNode (Faxitron, Arizona, USA) gamma probe was used in the usual fashion to attempt detection of radioactivity clinically in the nodal regions in the vicinity of the melanoma. No activity was detected.
Patent blue dye was not used in this patient due to the nature of the location of the primary melanoma and potential for permanent tattooing.
After induction of general anaesthesia, peritumoral intradermal injections of ICG (1 cc over 4 aliquots) was administered by the surgeon. SPY Elite (Stryker, Michigan, USA) technology was used prior to skin incision to mark fluorescence where it could be visualized transcutaneously.
An area of fluorescence was identified in Level V of the left neck. Using SPY intraoperatively, a sentinel lymph node was identified following skin incision and dissected. No other areas of fluorescence were detected transcutaneously. No radiotracer activity was detected, other than that at the primary melanoma site by the gamma probe. (Figure 1)
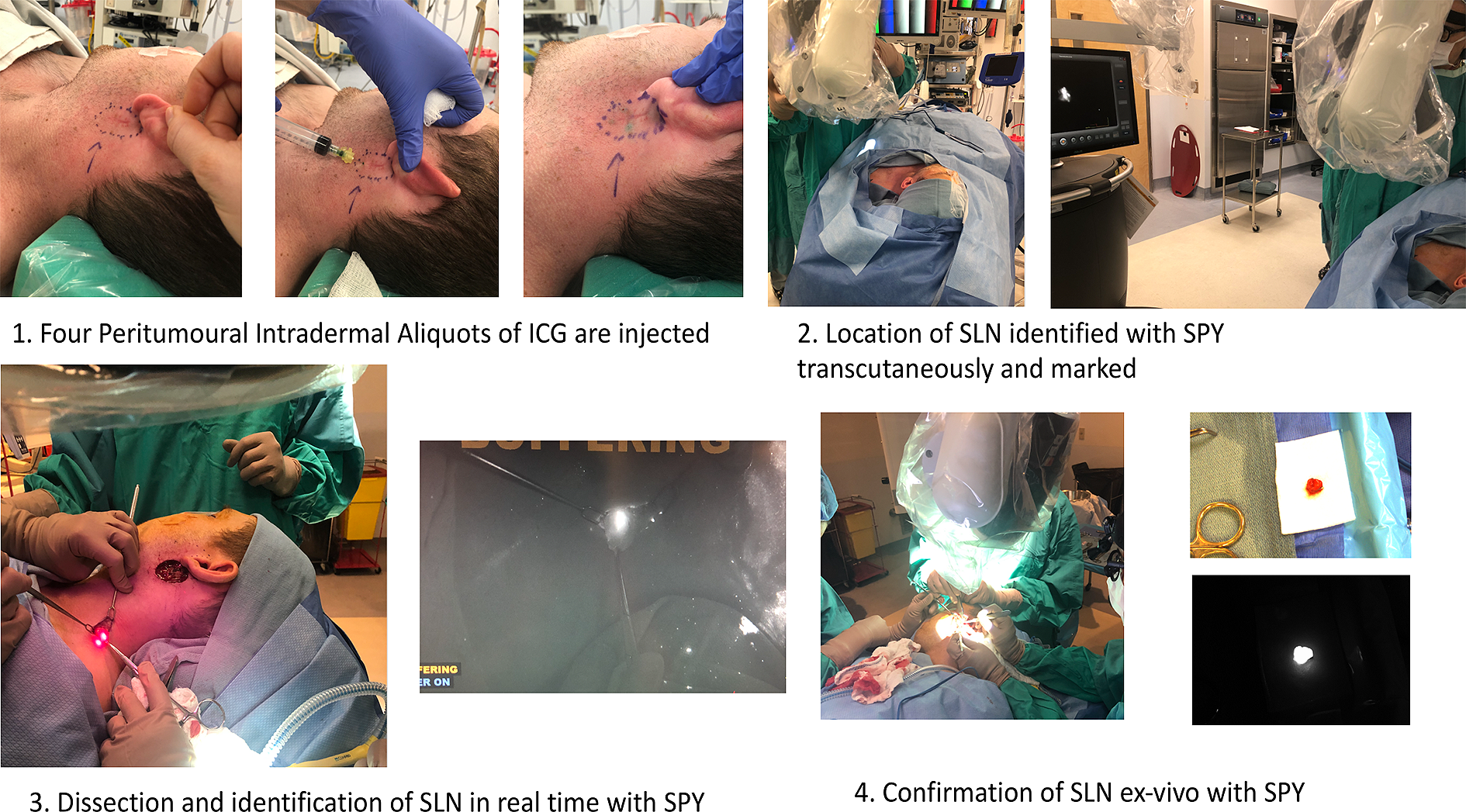
Using SPY/ICG to salvage SLNB.
Wide local excision of the melanoma was then performed.
Pathology of the node was negative for melanoma. Patient has had no nodal recurrence with a follow up of 14 months.
The use of SPY and ICG was again demonstrated in a subsequent head and neck patient when traditional gamma probe failed. A 77 year old male presented with a 2 mm non ulcerated, 15 mitoses, Clark IV melanoma of the left ear. He was offered wide excision and sentinel lymph node biopsy. The same protocol was followed as in the previous patient. Lymphoscintigraphy showed 3 nodes, 1 post auricular and 2 in level II of the neck. Intraoperatively, gamma probe identified only 2 nodes, 1 post auricular and 1 in level II, both fluorescent under SPY. With the use of SPY and ICG, a third node was identified in level II. All nodes were negative for melanoma. The patient had no nodal recurrence after 14 months.
This technique was subsequently used in 13 additional patients at our centre by one surgeon (CTO) from November 2019 to January 2020. The primaries included 5 truncal, 3 upper extremity, 1 lower extremity and 4 additional head and neck sites. Although no other cases involved radiotracer that failed to migrate, ICG was descriptively identified to aid in nodal detection and allowed for clipping lymphatics intraoperatively in real time with the aid of the SPY. None of the patients developed post operative seromas.
Discussion
ICG Combined with Gamma Detection may Decrease the False Negative Rate of SN Biopsy
The status of the sentinel node in melanoma care is important for prognosis in intermediate and thick melanomas. 2,11 Despite this, the false negative rate for this procedure ranges between 6 and 21%. 12 A false negative has been defined as a recurrence of melanoma in a nodal basin that has previously been sampled with a negative sentinel lymph node basin. The false negative rate is the ratio of patients with false negative results to the sum of patients with true positives and false negatives. 11 There have been a variety of reasons proposed to explain the cause of false negative results, including failing to retrieve the appropriate node, which could be related to challenging anatomic locations, shine through from the primary injection site close to the nodal basin, or poor technetium migration. 13
The use of ICG has been hypothesized to reduce false negative rates by increased detection of nodes. In a study of 34 patients, Fujiwara et al. determined that ICG as an adjunct to the gamma probe resulted in a higher nodal yield. 9 In our case report, we demonstrated the ability to salvage a SLNB where the technetium injection in nuclear medicine failed to migrate, but the ICG intraoperatively, did, resulting in successful nodal staging in this patient.
ICG is Particularly Helpful in the Head & Neck
The complex anatomy and variable lymphatic drainage patterns in head and neck melanoma have been noted to increase false negative rates of sentinel node biopsies. 14 Miller et. al demonstrated in their study of 154 head and neck patients a false negative rate of upwards of 30%. 15 Contributing factors include the high technical demand of the procedure due to multiple small lymph nodes in close vicinity to important neurovascular structures, as well as the increased frequency of the radiotracer failing to migrate. Stadelmann et al. demonstrated a non localization rate of 7% in their series of head and neck melanoma and Merkel cell carcinoma patients. 16 Furthermore, the primary melanoma in the head and neck may well overlie the nodal basin, reducing the ability of the gamma probe to direct the surgeon to the sentinel node when the surgical bed is radioactive.
We appreciated the back up of ICG to identify nodal basins and lymph nodes in head and neck cases where either the tracer did not migrate, as in our case, or where the nodal basin was close enough to the primary tumour to make gamma probe detection difficult, which occurred in 5 of our other patients (Figure 2). Additionally, the use of ICG aided in real time visual dissection (using SPY) in the head and neck, to allow preservation of neighboring structures and clipping of afferent lymphatics.
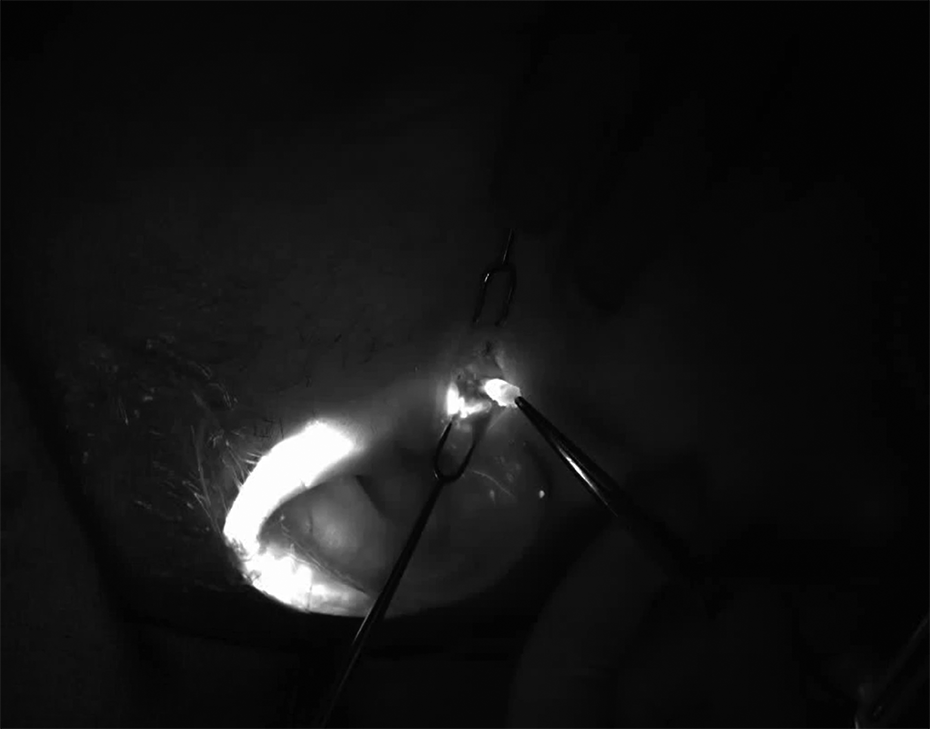
Localization of preauricular sentinel lymph node in close vicinity to the primary melanoma on the helical rim.
ICG Is Useful in Planning the Skin Incision
It is important to determine the location of the sentinel lymph node prior to skin incision. This is traditionally performed with the use of a gamma probe but the accuracy can be improved when the ICG illuminates the lymphatics and nodes transcutaneously. Namikawa and others reported the detection of nodal basins using ICG, especially in slender patients with head and neck or groin nodes. 17,18 Factors associated with increased detection included nodal basin location and body mass index. In our patient, SPY was instrumental in determining the location of the nodal basin and therefore incision planning. Although we are not suggesting preoperative lymphoscintigraphy be abandoned, when the radiotracer does not migrate, ICG and near infrared imaging can be very useful for accuracy in skin incision design.
ICG SPY May Reduce the Complications of SLNB
In the Sunbelt Melanoma trial, the risk of hematoma or seroma with sentinel node biopsy has been estimated to be over 2%. 19 The Multicenter Selective Lymphadenectomy Trial II demonstrated a lymphedema rate of 6.3% in those patients undergoing sentinel lymph node biopsy. 20 Multiple studies raise the possibility that ICG/SPY may reduce complications through real time visualization of lymphatics and by limiting removal of additional tissue. 5,17 Although our series of patients was small, no seromas were reported. We valued the ability to clip lymphatics under direct visualization (Figure 3). This technology also helped determine the peripheral limit of the lymph node when this was not easily clinically visually apparent, minimizing the removal of surrounding fatty tissue or adjacent nodes.

Clipping of lymphatics.
Conclusions
Avoiding false negative sentinel lymph node biopsies for patients with melanoma is key to good care. One such reason for this has been identified to arise when radiotracer does not migrate. We have demonstrated the ability of ICG/SPY to salvage a SLNB in a case where there was radiotracer migration failure, in a technically challenging anatomic area. Given the importance of the SLNB, further study of the use of this technology when traditional techniques fail is warranted.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics
Ethics approval was granted by the local institutional review board (University of Calgary HREBA.CC-20-0085). All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008. A waiver of consent was granted.
Informed consent was obtained for patient photographs and identifying details.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
