Abstract
Introduction:
Reverse-flow sural flap is a valuable option in cases of lower extremity repair. In this study, we aimed to present our sural flap applications and modifications for the treatment of ankle and foot defects and to evaluate our results in the light of historical process and current literature.
Materials and Methods:
A reverse-flow fasciocutaneous flap was performed in 14 patients to repair foot and ankle defects. In 6 cases (42.86%), we chose to perform interpolation sural flaps where we aimed to repair the distal defects of the foot and/or in order to prevent patients from having trouble wearing shoes due to bulkiness of the flap pedicle at the ankle. In other cases (tunnel flap group, 57.14%), the pedicle of the flap was passed through the subcutaneous tunnel. Wide and meticulous dissection of the tunnel, nitroglycerine application on the flap, and close flap monitoring were our protective measures. Our results were analyzed statistically. The literature review was performed from Medline and PubMed.
Results:
Sural flap repair was performed in 14 patients. The mean age was 32.75 years. Etiologic factors were traffic accidents, spinal cord injuries, and hyperkeratotic lesions. The defects were localized in the ankle or proximal foot in 12 (85.71%) patients and the distal foot in the remaining patients (14.29%). The mean area of the defects was 46.75 cm2. Partial necrosis at the distal flap developed in 2 (25%) cases in the tunnel group and in 1 (16.67%) in the interpolation group (3 cases in total, 21.43% in the study population). No statistical difference was found between the flap groups in terms of patient distribution and complications.
Conclusion:
Wide dissection of the subcutaneous tunnel through which the pedicle is passed (in the tunnel group), application of nitroglycerin, meticulous hemostasis, and postoperative follow-ups are important factors for a successful reverse sural flap application. Sural interpolation modification is advantageous in several cases as the flap can reach farther and does not cause bulkiness in the ankle that would impair shoe wear. However, the disadvantage is that it requires 2 sessions.
Introduction
A reverse-flow sural flap is an ideal option for lower extremity repairs. Several clinical, anatomical, and experimental studies have been conducted in the last 20 to 30 years regarding this procedure 1- 42 ; nevertheless, publications on interpolation flap modifications are very limited. 42 The fact that it does not require complicated procedures increases the value of this flap procedure, especially in clinics where microsurgery is not available. Therefore, reverse flow sural flaps should be understood with clinical, experimental, and anatomical studies. In this study, we aimed to present our sural flap applications and modifications for the treatment of ankle and foot defects and to assess our results in the light of historical process and recent developments.
Methods
All patients were informed preoperatively regarding how the operation will be performed and its possible complications. The peroneal artery and small saphenous vein traces were examined with Doppler ultrasound. The flap was planned and drawn on the cruris midline according to the size and location of the defect. The deep fascia was included in the flap. A 3- to 5-cm-thick dissection was performed on the pedicle including the sural nerve and short saphenous vein. Dissection was avoided distally from a distance of at least 5 cm from the lateral malleolus. The fasciocutaneous flap was passed through the tunnel under the skin in the tunnel group. The tunnel was dissected as wide as possible to prevent postoperative edema in the pedicle. If there was not enough room inside the tunnel, then the flap was passed after the tunnel ceiling was opened; the resulting defect was covered with a skin graft. The interpolation flap option was preferred after the observation of several cases with complaints of shoe wear problems due to flap pedicle bulkiness at the ankle and aiming the flap to reach the distal foot defects (Figure 1). In interpolation flap applications, the pedicle was covered with a split thickness skin graft and the flap was separated from the pedicle after 3 weeks. This type of flap application was performed in a cross-leg style, when there was severe injury around the lateral malleolus on the traumatized side. Nitroglycerin ointment was applied for 1 week on the pedicle and flap. Other flap protection measures were meticulous hemostasis, drain application, and close follow-up of the extremity.
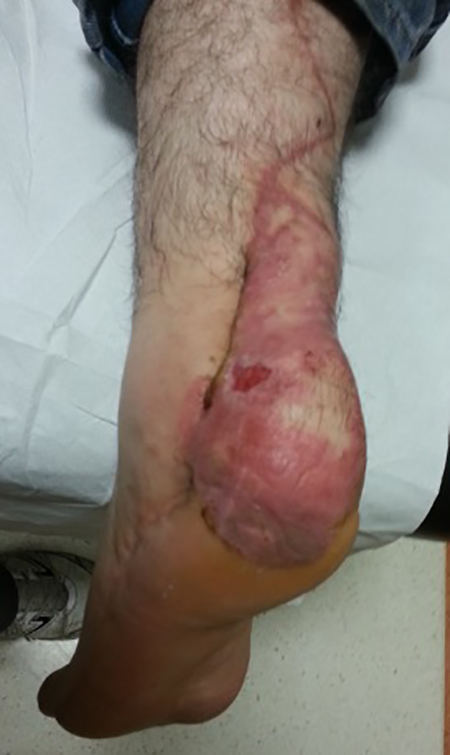
Postoperative Image of the case with a tunnel type reverse sural flap. Bulkiness in the ankle is notable in this figure.
The tunnel and interpolation groups were compared in terms of patient distribution (age, general health status, smoking, and defect size) and complications. An independent sample t test was used to analyze the difference between the 2 means to compare the patient distribution in the groups. Fisher exact χ2 test was used to compare the complications in the groups. SPSS 22.0 Windows version package program was used in the analysis. A P value <.05 was considered significant.
The literature review was performed using articles from Medline and PubMed. Clinical, experimental, and cadaver studies regarding reverse flow sural flaps were included. Historical processes and research over the last decade were reviewed.
Findings
In our clinic, 14 (10 men, 4 women) patients underwent repair with sural flap (Figures 2 -9). There were 8 (57.14%) cases in the tunnel group and 6 (42.86%) cases in the interpolation group. In addition, a cross-leg procedure was applied to 1 (7.14%) case in the latter group. There was no major comorbidity in the study population. There were 2 diabetic cases in each group that were under control with oral antidiabetics. Notably, the majority of the patients were smokers (11 of 14). The ages of the patients were between 12 and 45 (mean: 32.75 years) years. The etiologic factors were distributed as traffic accidents in 10 (71.43%) patients, spinal cord injuries in 2 (14.29%) patients, and hyperkeratotic lesions in 2 (14.29%) patients. The defects were localized in the calcaneal area in 5 (35.71%), the ankle in 4 (28.57%), the other proximal foot region in 3 (21.43%), and the distal foot in 2 (14.29%) patients. The area of the defect ranged between 30 and 70 cm2 (mean: 46.75 cm2). There were no significant differences between the tunnel and interpolation groups in terms of patient distribution and complications. There was no problem in the venous return of the flaps in the postoperative early period. However, limited distal necrosis was developed in 3 (21.43%) patients who were managed with wound care and debridement. All these cases were composed of smokers and one of them had diabetes. Partial necrosis was observed in 2 cases in the tunnel group and in 1 case in the interpolation group (25% vs 16.67%). No other complication was detected.
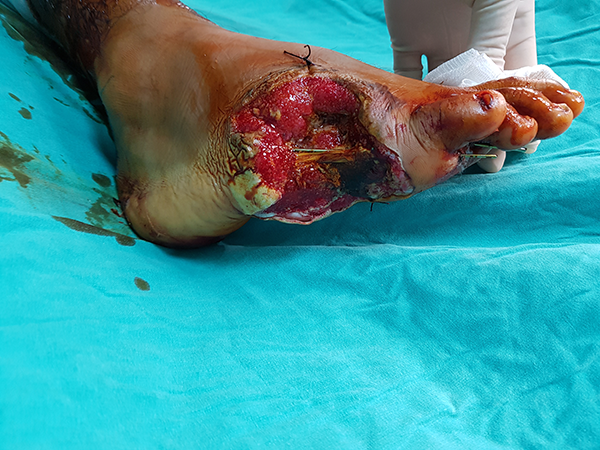
Preoperative image of the case after a gunshot injury with a defect on the distal lateral foot.
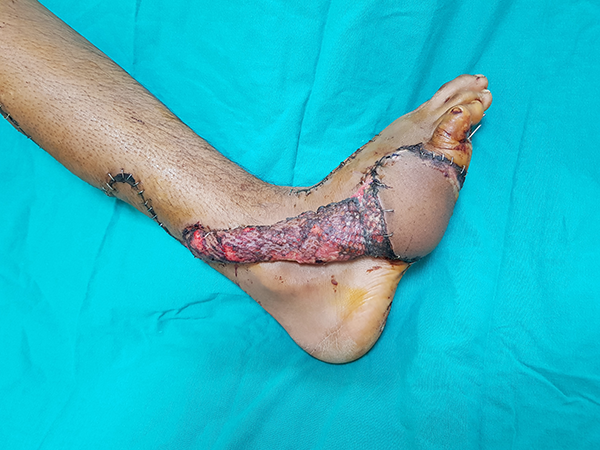
Image of the case with an interpolation reverse sural flap after 3 weeks.
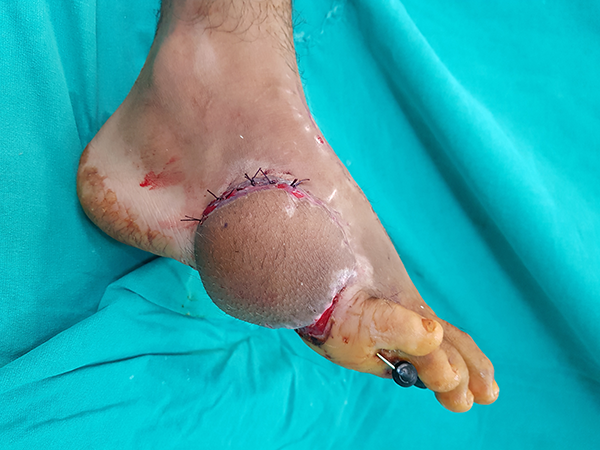
Image of the case after the pedicle has been detached.
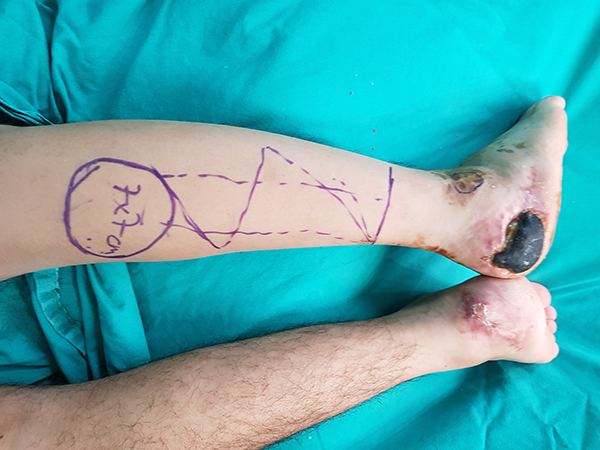
Preoperative image of the case after a crush injury on the posterior heel.
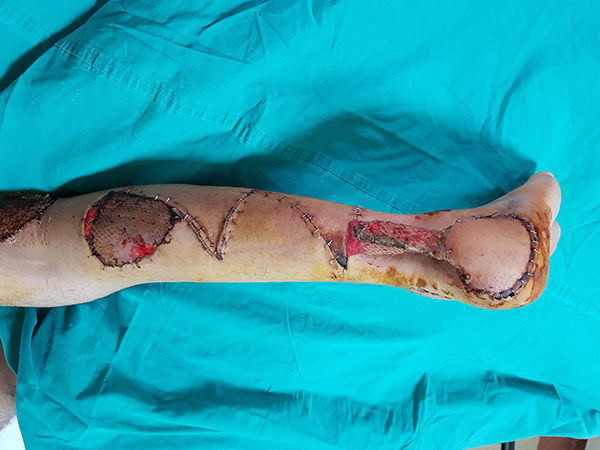
Image of the case with an interpolation reverse sural flap after 2 weeks.
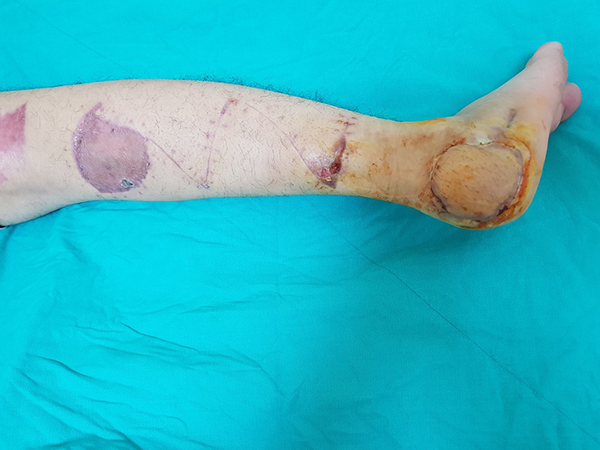
Image of the case after the pedicle has been detached.
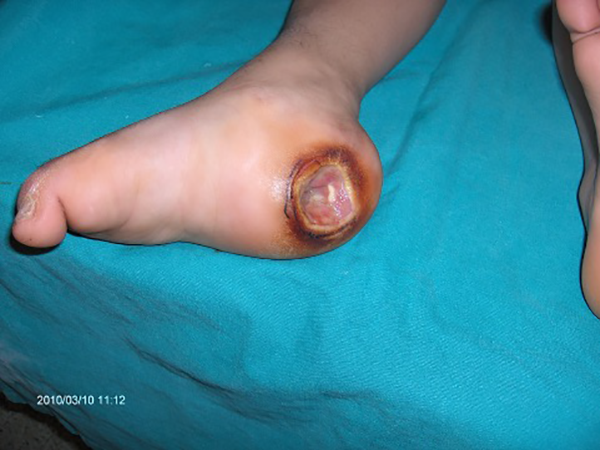
Preoperative image of the case with spinal cord injury and a defect on the medial heel.
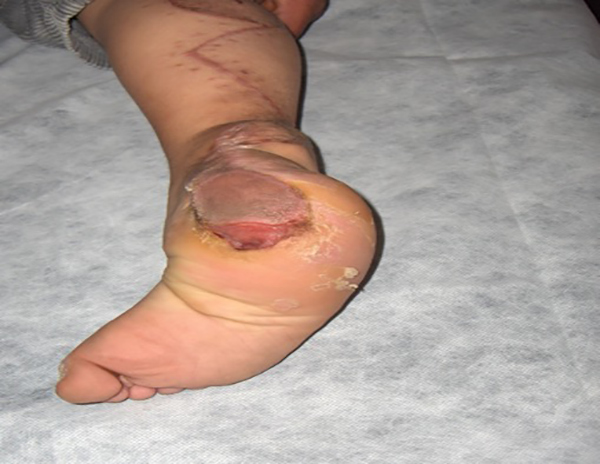
Postoperative image of the case 3 months after reconstruction with tunnel type reverse sural fasciocutaneous flap.
Discussion and Literature
Reverse-flow sural flap provides remarkable opportunities for reconstructive surgeons in lower extremity repairs. The first clinical and anatomical studies of fasciocutaneous sural flaps were performed by Ponten, Donski, Fogdestam, and Masquelet in the 1980s and 1990s. 27 The authors, however, stated that it was Masquelet who popularized the flap procedure. Yilmaz et al 4 maintained certain sizes of skin on the proximal flap pedicle and used this tissue as the ceiling of the tunnel through which the pedicle was passed. Hollier et al 10 suggested that the reverse-flow sural flap can reach up to the anterior part of the foot and is an ideal flap for the defects of the distal third of the lower extremities. According to Hasegawa et al, 1 the advantages of this flap are its thinness, the protection of a major artery, its reliable vascular supply, and its ability to be harvested quickly without the need for a Doppler flowmeter. The authors stated that the sacrifice of the sural nerve was a disadvantage. On the other hand, Costa-Ferreira et al 8 pointed out that they did not observe any loss of sensation or neuroma in the lateral aspect of the foot in their series of 36 cases. Jeng and Wei 3 presented the option of a sensitive sural flap for the repair of defects in the weight bearing areas. The authors included the lateral sural nerve in the flap and coapted it to the common sural nerve after the flap was brought to the defect area. Ayyappan and Chadha 11 reported that sural flaps with an area of 338 cm2 and the superior margin extending to the distal side of the popliteal line could be safely removed. The authors named their flaps as super-sural neurofasciocutaneous due to their sizes. Top et al 18 reported the safe application of these flaps in the treatment of chronic venous ulcers.
There are several points to be considered during the harvest of the flap. Hasegawa et al1 argued that the deep fascia should be included in the flap to protect the septocutaneous branches of the peroneal artery that nourish the sural flap distally. The authors emphasized the necessity to leave the skin 5 cm proximal to the malleolus intact for the same reason. On the other hand, Mojallal et al 33 advocated that the short saphenous vein and deep adipose tissue were important for the vascularity of the flap and the deep fascia provided only mechanical support in the light of 3D angiographic computed tomography studies on cadavers. Schmidt et al 35 concluded that the adipofascial flap was as reliable as the fasciocutaneous flap based on their retrospective study. The authors suggested the use of the adipofascial flaps in terms of the donor area appearance, if there is no reconstruction for a weight-bearing area. Hollier et al 10 listed the measures to protect the collaterals from the peroneal arteries as raising the flap’s pedicle as wide as possible, avoiding from the cut-back procedure, and finally leaving it exposed and covered with a skin graft, instead of passing the pedicle through the tunnel.
The arterial supply of sural flaps has been the subject of several studies. With their microangiographic studies, Nakajima et al 5 demonstrated perforators from the sural artery to the skin and anastomosis between the sural and peroneal arteries. Gascoigne et al 38 studied the vascular structures accompanying the superficial cutaneous nerves of the leg. The authors described the 2 basic arterial structures accompanying the medial sural cutaneous nerve and saphenous veins as the superficial sural artery and the saphenous artery. Additionally, the researchers demonstrated the presence of anastomotic connections between these basic arterial structures as well as between these structures and both the posterior tibial and peroneal arteries. Sladjana et al 17 showed that superficial sural arteries originate from the medial and lateral sural arteries and rarely from popliteal arteries in the lower extremities based on their studies with cadaveric fetuses. The researchers found that the existence of the median (sural flap pedicle artery), lateral, and medial superficial sural arteries were 83.3%, 80.9%, and 16.7%, respectively. The median superficial sural artery is under the fascia at the proximal third of the leg; at this level, it originates from the lateral sural artery and is located lateral to the short saphenous vein and the medial cutaneous sural nerve. At the junction of the proximal and middle thirds of the leg, it is observed to penetrate the fascia and proceed in the direction of the lateral malleolus with the short saphenous vein. At the junction of the middle and lower thirds of the cruris, the artery is observed to pass into the medial side of the vein. Zhang et al 19 demonstrated that the peroneal artery is divided distally into 2 branches as the posterior lateral malleolar artery and lateral calcaneal artery in a study of cadavers; additionally, both branches send perforators to the skin 1 and 3 cm proximal to the lateral malleolus. The authors stated that the vascularity of the flap can be strengthened by including these perforators in the area of the pedicle pivoting 1.5 cm proximal to the lateral malleolus. Yang et al 12 performed an angiographic study in 10 cadaveric legs and found similar results to those of Zhang et al. 19
It is important to understand the neural anatomy of the region. Gascoigne et al 38 observed that the lateral sural cutaneous branch has a highly variable anatomy, even absent in some cadavers. They showed that the medial sural cutaneous nerve starts from the middle part of the popliteal fossa and perforates the deep fascia in the middle 1/3 of the leg and then advances posterior to the lateral malleolus accompanying the short saphenous vein. According to Sladjana et al, 17 the medial cutaneous sural nerve originates from the tibial nerve and proceeds between the median superficial sural artery and the short saphenous vein. At the junction of the middle-lower third of the cruris, it joins with the fibular communicating branch as the sural nerve and becomes superficial by piercing the fascia. According to their work on fetuses, Ugrenovic et al 41 stated that the medial and lateral (also known as peroneal communicating branch) cutaneous sural nerves are derived from the tibial and common fibular nerves, respectively. In 67% of the cases, the 2 nerves converge to form the common sural nerve at the distal 1/3 part of the cruris. This nerve descends 1-1.5 cm behind the lateral malleolus. In the remaining cases, these 2 nerves did not join and the continuation of the medial cutaneous sural nerve is called the sural nerve. In rare cases, the medial branch is very weak and the sural nerve is the continuation of the lateral cutaneous branch. As a result of their studies in 40 cadaver cases, Kim et al found that the medial and lateral cutaneous nerves merge creating the sural nerve in 72.5% of the cases which they referred to as the combined pattern. 39 They defined the diminished type in 17.5% of the cases in which a weak lateral cutaneous nerve and a medial cutaneous nerve that continues as the sural nerve. Finally, they described a parallel pattern in 10% of the cases in which both cutaneous nerves proceeded in a parallel manner.
The mechanism behind the occurrence of the reverse venous return of the sural flap in spite of the valvular structure is controversial. One of the views is that the desensitization of the vein disables the valves, making reverse-flow possible. Timmons 43 argued that the desensitization of the radial vein resulted in the inability of the valves to function, so that reverse current was possible. Wee 44 shared the same view while studying the reverse tibial flap. The author advocated dissection beyond the point of the pedicle to ensure the desensitization of the vein. On the other hand, Hasegawa et al 1 stated that the venous return of the distal sural flap may occur at the suprafascial level by means of the septocutaneous branches of the superficial sural, short saphenous vein, and peroneal vein. After their studies with Doppler ultrasound in cadavers and patients, Loonen et al 25 mentioned the difficulty of venous return due to the valvular structures in the short saphenous vein and stated that the small venous structures accompanying the arterial structures adjacent to this vein should be preserved. The authors found that these venous structures accompany the short saphenous vein on the right or left in a region of 3.5 cm in width. They merge with the short saphenous vein in a few places; thus, they bypass the valvular barriers before pouring into deep venous structures. According to these findings, the researchers advocated that the bypass veins should be analyzed by ultrasound on the crural area between the safety points that are 20 and 25 cm proximal to the lateral malleolus before the dissection, respectively. Gascoigne et al 38 pointed out the anastomoses between the saphenous system and deep venous system that increase distally based on their study on cadavers. The authors demonstrated avalvular venous structures that combine the star-shaped vena comitantes of the saphenous system and the sural flap perforators. They emphasized the importance of including the saphenous system in the flap as other systems are narrower. Zhang et al 19 determined that there is a communicating vein between the small saphenous vein and the peroneal vena comitantes based on their study of cadavers. Additionally, this vein accompanies the posterior lateral malleolar artery, which is one of the branches of the peroneal artery. The authors stated that the inclusion of this vein in the flap pedicle would enable the surgeon to safely move the pivot point in a more distal manner, thus allowing the flap to be used for more distal defects. Notably, the authors did not encounter flap nourishment problem in their series including 21 cases.
Venous congestion, which is frequently observed in the postoperative period, has been evaluated as a problem, and many clinical studies have been carried out to reduce it. Buluç et al 22 recommended intraoperative tissue expansion of the skin tunnel, where the flap pedicle passes to reduce venous congestion. Akyürek et al 14 experimentally and clinically demonstrated that the vascularity of the flap was further increased with delay application. Kneser et al 16 obtained similar results with a delay procedure in their clinical studies. The authors managed to safely remove the flaps of up to 19 × 12 cm. Parrett et al 32 recommended the delay procedure in patients with advanced age, smoking, obesity, diabetes, and peripheral vascular diseases in which the flap complication rates are increased. Tosun et al 20 also suggested that increased reliable flap vascularity would be achieved by implementing the delay procedure in the repair of diabetic foot defects.
As mentioned above, a major disadvantage of the sural flap is the sacrifice of the sural nerve. Although postoperative hypoesthesia due to nerve loss is not a major problem in paraplegic patients, there have been researchers who argue that this condition may be the subject of complaints in others and that the flap can be harvested without sacrificing the nerve. Mojallal et al 33 observed that the sural nerve included in the harvested flap did not significantly expand the vascular area. Nakajima et al 5 stated that the sural flap can be supplied by the superficial sural artery and the venocutaneous perforators even if the artery accompanying the sural nerve is damaged. Gascoigne et al 38 found long branches of the perforators along the medial sural cutaneous nerve trace originating from the superficial sural artery or mostly the peroneal artery. Demonstrating true large-caliber anastomoses progress on the longitudinal axis and shorter perforators on the oblique or transverse axis, they concluded clinical reflection of their findings as low blood supply in transverse designed flaps. The authors found anastomotic structures connecting the perforators instead of a prominent vascular trace in 5% of the cases and added that the absence of a significant vascular trace in these cases may be the cause of flap necrosis encountered by many researchers.
Concerns have arisen regarding nerve-sparing surgery in terms of the prolongation of dissection time and vascularity of the flap. 39 Gascoigne et al 38 pointed out that although the vascular axis accompanies the nerve, it has a distinct pattern that explains the viability of the flap in a nerve-sparing flap design. However, the authors stated that it would be more appropriate to include the nerve in the flap in order to ensure the protection of a true anastomotic chain in the flap. Kim et al 39 claimed that the sural nerve can be divided safely into 2 during flap harvesting. The authors stated that the junction of the medial and lateral cutaneous nerves is approximately 13.6 cm from the lateral malleolus, which is close to the pivot point of the sural flap. Aydın et al 34 performed nerve-sparing interventions in 5 reverse flow sural flap cases and only encountered partial necrosis in 1 case. The authors concluded that nerve-sparing surgery did not impair the flap vascularity. Aoki et al 30 reported that dissection of the nerve did not cause significant bleeding when harvesting sural flaps. The researchers encountered adequate flap vascularity in 22 cases, partial necrosis in 5 cases, and complete necrosis in 1 case in 28 flap applications. The authors also performed angiographic studies on cadavers and concluded that the vascular structure around the sural nerve is more important than the intrinsic vascular structure. Therefore, it is important to preserve the vascular structures around the nerve and short saphenous vein during nerve dissection.
Almeida and Okawa 9 reported the complication rates of partial and total necrosis as 21.1% and 4.2%, respectively in their series of 71 cases. Akhtar and Hameed 23 reported partial necrosis, total necrosis, and infection rates in their series of 84 cases as 7.14%, 9.52%, and 4.76%, respectively. Baumeister et al 13 stated that factors such as advanced age, diabetes, and peripheral vascular disease may increase the complication rate of flap necrosis by 4 to 5 times. The authors encountered necrosis in 36% of their 70 cases with any of the risk factors. We did not encounter total necrosis in our cases, whereas our partial necrosis rate was 25% in cases with tunnels and 16.67% in interpolation cases. Our complication rate was comparable to those of Almeida and Okawa, and Akhtar and Hameed. 9,23 We included the sural nerve in the flaps in order not to affect flap vascularity. However, we did not encounter any significant morbidity and patient complaints related to sural nerve function. We accept the fact that the lower mean age of our cases and the etiologic factors mainly consist of traffic accidents had an effect on our results.
Wei et al 36 summarized the risk factors in sural flap applications based on their experiences from a series of 179 cases. According to the authors, the upper edge of the flap located in the proximal 1/9 of the cruris, the transverse ratio of the flap length of 5:1 or above, and the width of 8 cm or above are significant risk factors. On the other hand, Al-Qattan 26 claimed that the flap could be prepared safely 2 to 3 cm below the popliteal fold by including a layer of muscle tissue. As mentioned earlier, Ayyappan and Chadha 11 also stated that they successfully harvested flaps extending to the popliteal area.
Maffi et al 42 presented their interpolation sural flap series of 7 cases with the defects on the ankle, malleolus, or heel. The authors stated that they did not encounter a vascular problem except for a case with distal tip necrosis that was managed with readvancement and suggested the interpolation option for reliable vascularization. Contrastingly, we used an interpolation flap design in order to reach more distal foot defects. Additionally, we opted for a different approach by comparing the tunnel and interpolation cases. In the first group, partial necrosis was 2/8, whereas the rate was 1/6 in the latter. Although there is no statistically significant difference, we accept that our study population is small, and larger series studies are required for more precise opinions. However, we think that the sural interpolation modification may be a better choice in some cases due to the deep reach of the flap and does prevention of bulkiness in the ankle that would impair shoe wear in the postoperative period. Although, there is no statistical difference between our groups in terms of partial necrosis, we predict that the venous return in interpolation flaps may be more reliable, as advocated by Maffi et al. 42 We predict that the pressure on the flap pedicle, which is one of the main concerns in the tunnel method, can be avoided by preparing the pedicle outside. Moreover, 1 or 2 pads can be placed under the pedicle increasing its pivot angle and therefore augmenting the vascular supply. On the other hand, the necessity of 2 sessions is a disadvantage of these flaps.
Conclusion
In classical sural flap applications, the extensive dissection of the subcutaneous tunnel through which the pedicle is passed, application of nitroglycerin, meticulous hemostasis, and postoperative follow-ups is necessary for successful reverse sural flap applications. However, in the group of high-risk patients such as smokers, diabetics, the elderly, and so on, protective methods such as delay procedures may be considered. The sural interpolation modification is advantageous as the flap can reach farther and does not cause bulkiness in the ankle. Additionally, although we found no statistical difference between the flap groups for complications, we think that venous return problems might be lesser in the interpolation group since the pedicle does not pass through a tunnel. However, the disadvantage is that it requires 2 sessions.
Footnotes
Authors’ Note
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statements
I declare that this submission follows the policies of the Guide for Authors and the Ethical Statement of the journal.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
