Abstract
Objective
This study was performed to introduce our surgical strategy and experience in applying a repeated reverse sural fasciocutaneous flap (RSFF) to repair large areas of tibial exposure.
Methods
During a 3-year period, 10 patients with a large area of tibial exposure and intact posterior skin and soft tissue after trauma were treated in our hospital using a repeated RSFF. First, most of the area of proximal tibial exposure was covered by an RSFF. Three weeks later, another smaller RSFF was designed from the original flap and rotated to repair the remaining exposed area of the tibial wound.
Results
All 10 patients’ wounds were completely healed after 2 to 4 operations. The wounds had healed well after 6 months. The patients were satisfied in terms of both appearance and function.
Conclusion
The repeated RSFF is a good treatment strategy for patients with large areas of tibial exposure with intact posterior skin and soft tissue.
Keywords
Introduction
Trauma-induced pretibial skin defects with tibial exposure are very common in the clinical setting. Several clinical treatment methods are available for pretibial skin defects with tibial exposure, such as local skin flap transfer, free flap transfer, 1 split-thickness skin grafting after granulation tissue formation and drilling of the tibial surface, 2 and split-thickness grafting after the use of tissue-engineered dermal wound coverings to grow granulation tissue.3–5 However, large skin defects on the anterior side of the lower leg with large areas of tibial exposure, especially areas longer than 20 cm, are difficult to repair. The authors believe that a repeated reverse sural fasciocutaneous flap (RSFF) followed by large free flap repair is preferred for treatment of large areas of tibial exposure and that split-thickness skin grafts and skin substitutes are not suitable for repairing such wounds. In this study, we used a repeated RSFF to treat patients with large areas of tibial exposure and achieved good effects; the same method was used in the subsequent treatment of nine other similar patients. All of these patients were cured with good results. In this paper, we summarize and share our experience with this treatment.
Clinical data
General information
This study included patients with large areas of trauma-induced tibial exposure with intact posterior skin and soft tissue who were admitted to a level III hospital in Liu Zhou, Guangxi, China from January 2015 to January 2018 and treated with a repeated RSFF. Ethical approval was obtained from the Ethics Committee of the First Affiliated Hospital of Guangxi Medical University. All patients provided written informed consent for the surgical procedures. The publication of the images was not disputed because the images contained no patient names or characteristics.
Surgical strategy
All wounds of the admitted patients were assessed. If necrotic tissue was present on the wound surface, debridement was first performed to completely remove the necrotic tissue; this was followed by vacuum-assisted closure. If the wound was clean, RSFF surgery could be performed directly; however, in cases of tibial fracture, fracture reduction and internal fixation were performed first. The operative procedures are shown in Figure 1. The flap was designed as follows. The line connecting the midpoint of the calcaneus and external malleolus to the midpoint of the popliteal fossa was the flap axis. The point of flap rotation was located 5 to 8 cm proximal to the midpoint of the calcaneus and lateral malleolus. The pedicle was ≥5 cm wide. The flap size was determined based on the size of the defect. The flap was lifted from the deep fascia and muscle surface during the operation, and the sural nerve was preserved inside of the flap. The deep fascia and skin were sutured at the edge of the flap to avoid separation.

Flow chart of patients and corresponding treatments. RSFF, reverse sural fasciocutaneous flap; RRSFF, repeated reverse sural fasciocutaneous flap; VAC, vacuum-assisted closure.
The flap was lifted from the distal end to the pedicle, and blood flow to the end of the flap was observed. If the blood flow was normal, the flap was rotated to cover the exposed surface of the tibia and sutured to the surrounding tissue. Thin skin grafts from the thigh were transferred to cover the wound of the flap donor site and other wounds. The flaps in this group of patients were up to 20 to 30 cm in length, and the distal width was 15 to 20 cm (Table 1). This operation covered most of the proximal part of the exposed tibia. A small amount of exposed tibia at the distal end could not be covered because the flap was not wide enough. Three weeks after the surgery, the original flap had established blood circulation between the base and the surrounding tissue; thus, another pedicle flap could be designed on the posterolateral side of the calf. The location of the pedicle was the same as that of the original flap. The size of the flap was designed according to the amount of exposed tibia. The flap was freed in a retrograde manner and rotated inward to cover the exposed tibial wound at the distal end. Blood flow to the end of the flap was observed. The edge of the flap was then fixed to the surrounding tissue, and the remaining wounds were covered using split-thickness skin grafts. The wound was opened 1 week later, and flap blood flow was observed after the operation. Photographs of a typical operation are shown in Figure 2.
Detailed information of the enrolled patients.
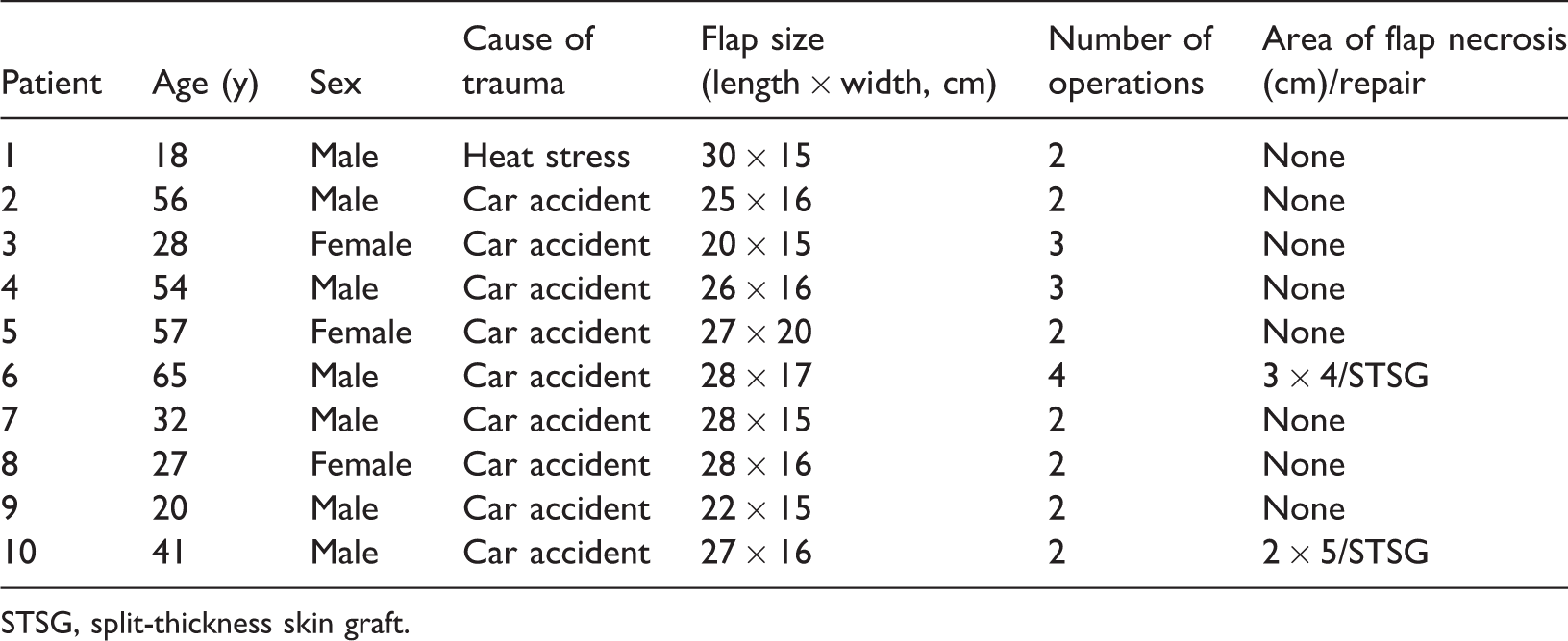
STSG, split-thickness skin graft.

Photographs of the surgical area at different stages of a typical surgical repair. (a) The length of the tibia that was exposed after traumatic debridement was 33 cm. (b) The first RSFF operation. (c) The first RSFF operation. (d) After the RSFF operation, a small amount of flap necrosis was present. (e) After the RSFF operation, a small area of the distal tibia was still exposed. (f) After the RSFF operation. (g) Repeated RSFF preparation. (h) Lifted repeated RSFF. (i) Repeated RSFF rotated to cover the exposed end of the distal tibia. (j, k) Complete coverage of the wound. (l) The result after 6 months. RSFF, reverse sural fasciocutaneous flap.
Results
Ten patients were treated with the same surgical plan for wound repair. The patients comprised seven males and three females ranging in age from 18 to 65 years. Nine patients were injured in a car accident, and one patient was injured by heat stress. Two cases were complicated by a tibial fracture, and the length of tibial exposure ranged from 20 to 33 cm (mean length, 26 ± 7.8 cm). The duration of tibial exposure ranged from 5 to 20 days (mean,14 ± 7.3 days). After RSFF surgery, local skin flap necrosis occurred in two patients (the size of the necrotic area is shown in Table 1), and all wounds in the remaining eight patients healed. These necrotic sites were located at the extreme or marginal parts of the flap (Figure 2d). The necrotic sites were not located on the previously exposed surface of the tibia and were repaired using split-thickness skin grafts during the repeated RSFF procedure. In all 10 patients, the repeated RSFF survived without local necrosis. The wounds of all 10 patients healed; 7 patients underwent two operations, 2 patients underwent three operations, and 1 patient underwent four operations.
All 10 patients were followed for 6 months, and the wounds healed without infection or ulceration and with good limb function. All patients returned to their previous occupation and daily activities. There were no cases of pain or numbness at the wound site or at the end of the limb. The general condition of each limb was good. The doctors evaluated the results as satisfactory. Although scar hyperplasia developed in the area of the skin grafts and the edge of the flap, the limb function was minimally affected because the hyperplasia was not located at the joint. The overall outcomes were satisfactory.
Discussion
Calf injuries with resultant pretibial skin defects and tibial exposure are very common in the clinical setting and are often associated with fracture and nerve vascular injury. It is relatively easy to manage a small area of tibial exposure with a local skin flap; however, large areas of tibial exposure, especially areas longer than 20 cm, are difficult to completely cover using this strategy. 6 Local flap transfer is not a good choice in these cases because the tibial exposure is often accompanied by extensive anterior and peripheral skin defects. 1 When the length-to-width ratio of the skin flap is too large, the patient is more susceptible to blood flow disorders or even necrosis. When free flap transplantation is performed, 7 great damage at the donor site may occur when the tibia is exposed by more than 20 cm, and the operation is often complicated and time-consuming; furthermore, poor blood circulation can lead to necrosis and increase the surgical risk. Cross-leg skin flaps1,6,8 have also been used to repair such injuries, but patients with cross-leg skin flaps have difficulties in activities of daily living and require nursing care during the postoperative fixation period. For small areas of bone exposure, such as those less than 3 cm in diameter or after a tibial periosteal retention procedure, granulation tissue formation can be induced by drilling the cortical bone or using tissue-engineered dermal materials 9 ; the wound can then be covered using split-thickness skin grafts. However, when the wound is too large, especially in cases accompanied by periosteal loss, granulation tissue does not readily form on the surface of cortical bone. 10 Moreover, flaps are always recommended for the repair of large anterior tibial skin defects to avoid subsequent repeated collapse. 11 Therefore, cultivation of granulation tissue followed by application of split-thickness skin grafts is not recommended for large areas of tibial exposure. 12
Sural fasciocutaneous flaps include sural nerve flaps,13,14 sural neurovascular flaps, 15 sural flaps,16–19 and sural fasciocutaneous flaps.1,20,21 These flaps can be used either in the forward or reverse direction; when used in reverse, they are termed RSFFs. RSFFs are widely used in the clinical repair of soft tissue defects of the calf or foot.8,22 However, because of their width limitations, it is difficult to cover exposed tibial surfaces of more than 20 cm in length. If the flap covers the distal end of the tibia, the proximal wound is still exposed. If the proximal wound is covered, the distal wound is still exposed. Therefore, in the present study, we designed the flap according to the soft tissue defect in the anterior tibia. After rotation, the flap preferentially covered the proximal end of the exposed surface of the tibia, and the distal end was bandaged with removable dressings.
After the flap and basal tissue had healed for 3 weeks and blood circulation was established, the RSFF operation was performed again (i.e., repeated RSFF). The flap pedicle in the second operation was the same as that in the first operation. Because the first operation involved the lifting of a large proximal flap, the blood circulation from the pedicle was enhanced during the later revascularization. At 3 weeks after reconstruction, the flap survival rate was very high. The repeated RSFF was designed using the original flap tissue that did not cover the surface of the tibia after the first operation, and the corresponding flap was designed to cover the residual area of tibial exposure. Only two patients developed a small amount of skin necrosis at the edge of the RSFF, and all of the repeated RSFFs survived completely. The operative duration varied because some patients also had a tibial fracture and others had residual tissue necrosis.
In conclusion, if the posterior skin and soft tissue are intact in patients with large areas of tibial exposure, the repeated RSFF is a good surgical repair strategy.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
