Abstract
Objectives
The primary objective is to evaluate the incidence of occult nodal metastasis in patients undergoing total laryngectomy with cN0 disease. Other objectives are to compare the survival between different treatments of the neck, identify possible associated risk factors, and evaluate the effectiveness of elective neck dissection in this population with regards to oncological outcomes.
Study Design
Retrospective review.
Setting
Tertiary hospitals in Hong Kong.
Methods
Retrospective study was performed on patients who underwent total laryngectomy from 2008 to 2017 in New Territories West and Hong Kong West Clusters of the Hospital Authority of Hong Kong as primary or salvage treatment for cN0 squamous cell carcinoma (SCC) of the larynx. Incidence of neck dissection, incidence of nodal involvement, possible predictors, and oncological outcomes were analyzed.
Results
Seventy-seven patients were included, of whom 61 underwent either ipsilateral or bilateral neck dissection. Most (90.1%) of the patients with total laryngectomy done had locally advanced disease. Overall occult nodal metastasis rate was 20.6%, and only 3.8% of them had contralateral nodal metastasis. Occult nodal metastasis was significantly less in salvage laryngectomy (P = .045), while midline involvement and pT3/4 disease seem to be predictors for contralateral nodal metastasis.
Conclusion
There is significantly lower incidence of occult nodal metastasis in cN0 laryngeal SCC in the salvage setting, and occult contralateral nodal metastasis is not common in the cohort. Neck dissection during a salvage laryngectomy for cN0 disease could be avoided while contralateral neck dissection might be considered in cases of locally advanced disease with midline involvement.
Keywords
In 2018, there were 204 cases of newly diagnosed laryngeal cancer in Hong Kong, and on average, there are 191 cases per year. 1 Total laryngectomy has been a common procedure for treating locally advanced laryngeal cancers or as a salvage surgery after failure of organ preservation treatment. The presence of metastatic lymph node disease has a great negative impact on survival, and failure in the neck has been shown to be the most likely cause of treatment failure and locoregional recurrence. 2 Therefore, ipsilateral or bilateral neck dissection is usually done with both primary and salvage total laryngectomy in our locality. However, with the known complications associated with neck dissection, there is no consensus on the guideline directing management of the neck in patients with cN0 disease.
The purposes of this study are to investigate the incidence of occult nodal metastasis in patients who underwent total laryngectomy as primary or salvage treatment for squamous cell carcinoma (SCC) of the larynx in our institutions, as well as the effect on survival between the treatment group (with neck dissection) and nontreatment group. Furthermore, we wished to evaluate the potential difference of oncological outcomes in the subgroups regarding the extent of disease and prior oncological treatment, as well as identify possible predictors for occult nodal metastasis. We aimed to make a reasonable conclusion in the role of elective neck dissection in the studied cohort.
Materials and Methods
Following the approval from the Cluster Research Ethics Committee/Institutional Review Board of the Hospital Authority, a retrospective review of 10 years was performed in patients who underwent total laryngectomy in the New Territories West and the Hong Kong West Clusters between 2008 and 2017. Electronic record of the consecutive patients being treated from January 1, 2008, to December 31, 2017, with a diagnosis code for “cancer of larynx” and procedure code for “total laryngectomy” was obtained from the electronic patient record systems. Patients’ data were reviewed, and only patients with clinically N0 disease, which was defined as no nodal metastasis being detected by clinical examinations and radiological studies, were included in the study. Exclusion criteria included patients who had no radiological imaging done before surgical treatments, patients who received total laryngectomy for reasons other than SCC of the larynx, and patients who had a history of SCC of other head and neck regions before the diagnosis of carcinoma of larynx.
Clinical data of the patients matching the inclusion criteria were reviewed, including demographic data, clinical staging, cancer history, investigation results, operations done, pathological report, subsequent oncological treatments, recurrence, and survival. Pathological reports were reviewed in detail on tumor staging, nodal status, perineural invasion, and lymphovascular infiltration. Tumors were restaged according to the the Union for International Cancer Control and the American Joint Committee on Cancer (UICC-AJCC) TNM eighth edition staging system to maintain consistency of the results.
Results
In total, 111 patients with cN0 SCC of the larynx underwent total laryngectomy from January 1, 2008, to December 31, 2017. Thirty-four patients were excluded from the study due to incomplete clinical data, absence of preoperative radiological studies, defaulted follow-up visits, presence of metastatic disease before the operation, total laryngectomy done for malignancies other than SCC, and death within 48 hours after the operation. Of the 77 patients included in the study, 49 (63.6%) had total laryngectomy as primary treatment and 28 (36.4%) had salvage laryngectomy for either a recurrent or residual disease after organ preservation treatment. Sixty-two (80.5%) patients had clinical T3 or T4 disease (55.8% and 24.7%, respectively) and 15 (22.1%) patients had clinical T1 or T2 disease (2.6% and 16.9%, respectively). Twenty-six (33.8%) patients had disease arising from supraglottis, 29 (37.7%) patients had glottic disease, and 22 (28.6%) patients had transglottic disease. There was no patient with subglottis disease primarily. Twenty-eight (36.4%) patients had the disease with midline involvement, and 30 (39.0%) patients had subglottic extension. Table 1 summarizes the characteristics of the included patients.
Study Population Data.
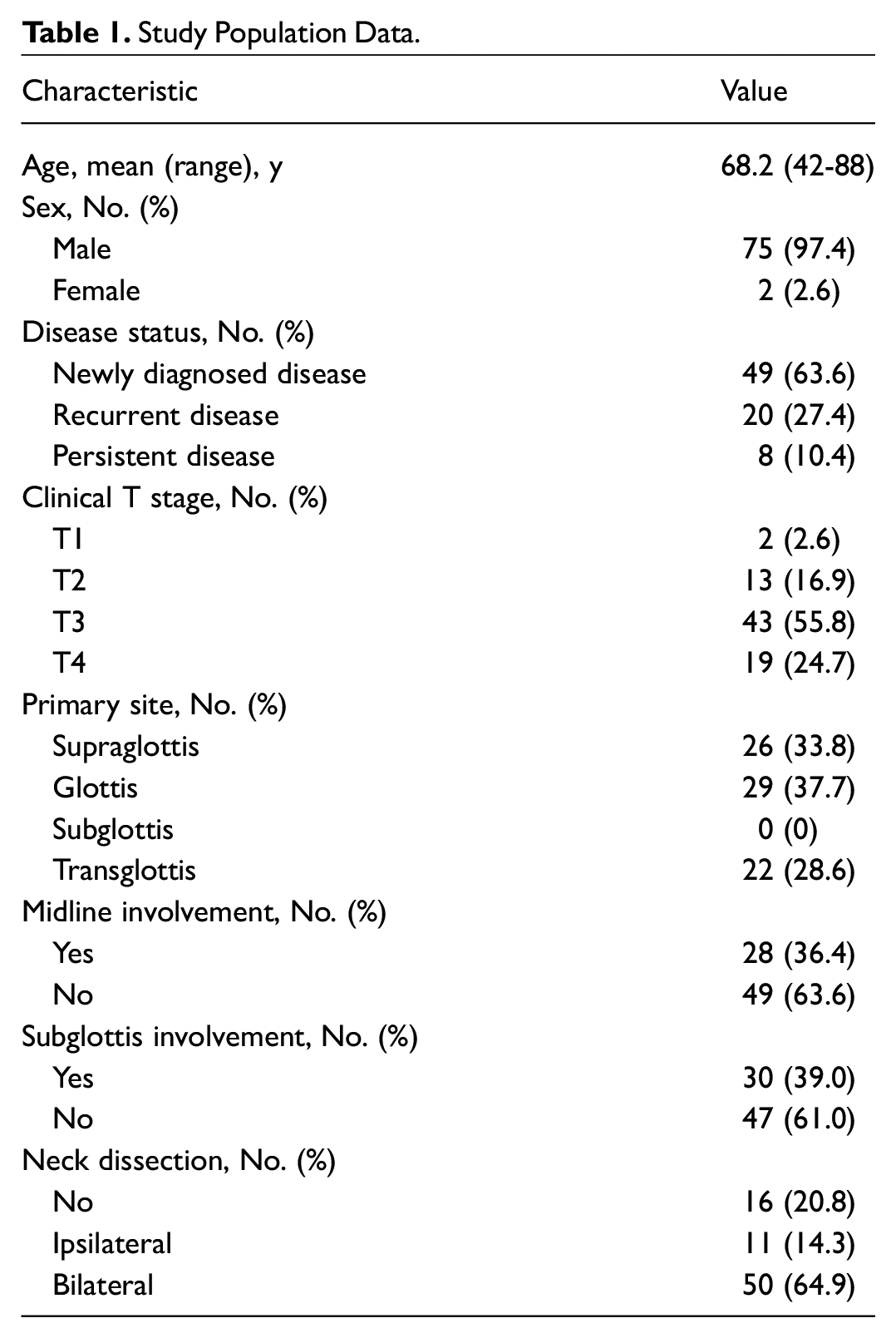

Fifty patients (64.9%) received bilateral neck dissection, 11 patients (14.3%) received ipsilateral neck dissection, and 16 patients (20.8%) had no neck dissection, yet 2 of them underwent excisional of bilateral level II lymph nodes, and therefore the pathology results were included in further analyses.
Table 2 outlines the pathological and oncological results of the patients. Upon review of the pathology reports, most patients had locally advanced disease of pT3/4 (90.9%). Overall, 13 patients had positive nodal metastasis.
Data on Pathological and Oncological Results.

Abbreviations: NA = not available; RT= radiotherapy.
Table 3 lists the pathological lymph nodes status of the 63 patients who had neck dissection (n = 61) or bilateral level II lymph node biopsy (n = 2). Fifty-one (79.7%) patients had negative nodal involvement. Among the 50 patients who had bilateral neck dissection done and the 2 patients with bilateral lymph node excisional biopsy, 2 of them (3.8%) had positive contralateral lymph node involvement.
pN Stage and Lymph Node Involvement in Patients Who Underwent ND (N = 63).
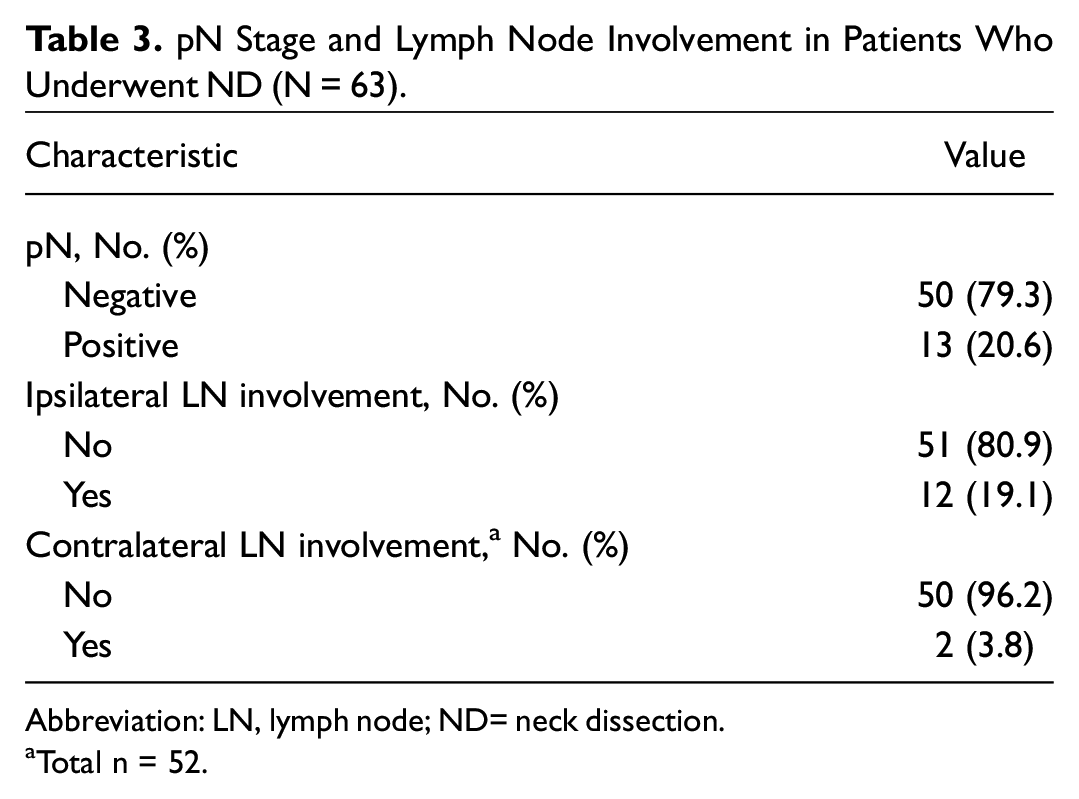
Abbreviation: LN, lymph node; ND= neck dissection.
Total n = 52.
The whole investigated cohort had a 5-year overall survival (OS) rate of 64.6% and median OS of 77.9 months. The 5-year disease-free survival (DFS) rate was 72%. Analysis was done for the effect of neck dissection. The median OS of patients without neck dissection and with ipsilateral and contralateral neck dissection were 66 months, 78.1 months, and 122 months, respectively (P = .614), and the 5-year DFS rate of patients was 72.1%, 72.7%, and 73.8% for these 3 groups of patients correspondingly (P = .982). The detailed survival curves are shown in Figure 1 . The overall complication rate of the procedure was 3.9% (3/77), with 2 patients having postoperative pharyngocutaneous fistula formation and 1 of them with dehiscence of the tracheostome. All of them underwent bilateral neck dissection.
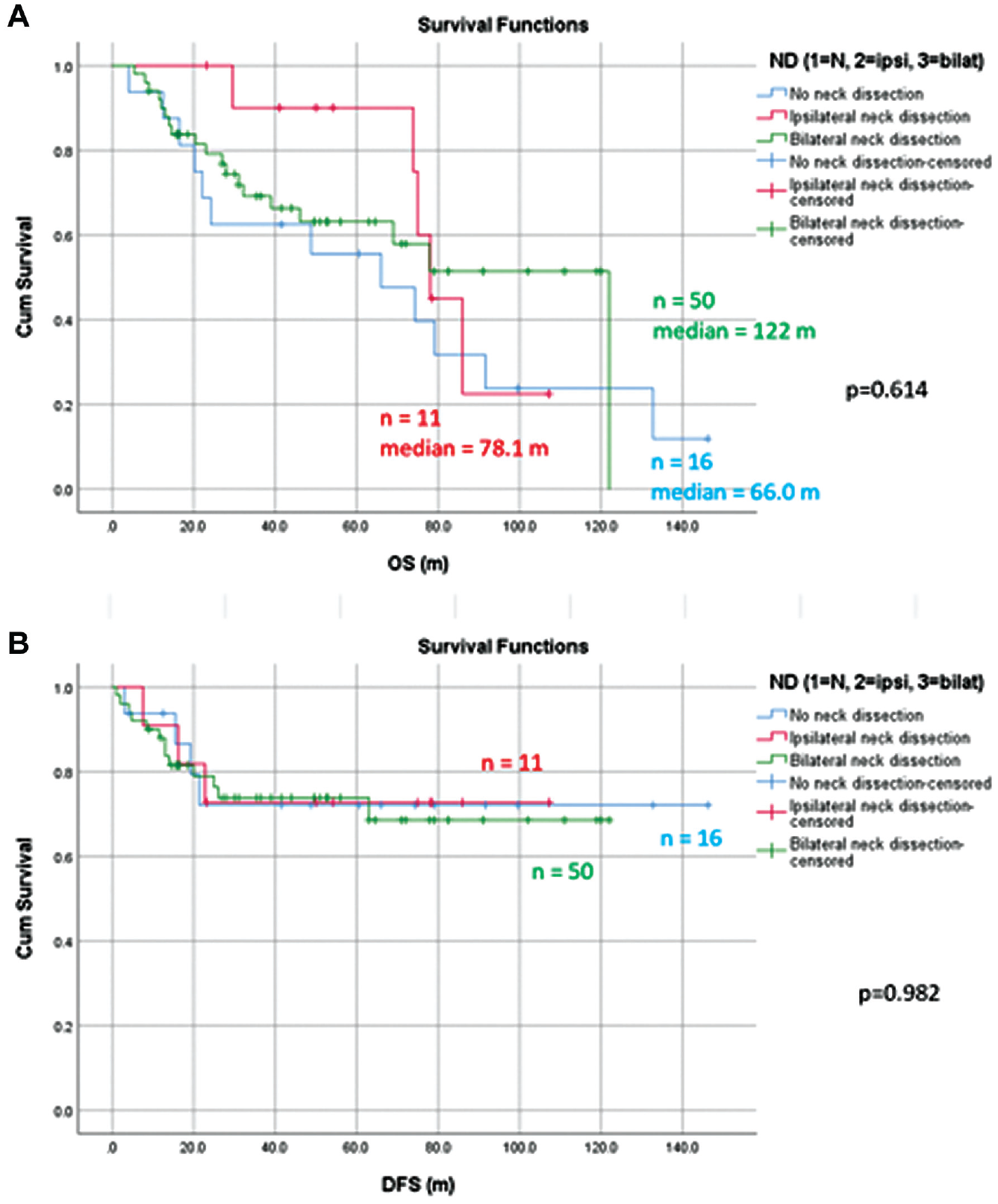
Kaplan-Meier curves depicting (a) overall survival (OS) and (b) disease-free survival (DFS) for the whole cohort comparing no neck dissection, ipsilateral dissection, and bilateral neck dissection.
In view of the reported difference in the pooled rate of occult metastasis based on subsites and extent of the tumor, subgroup analysis was done. Table 4 lists the results concerning the correlation between different subsites and pathological nodal status. Occult nodal metastasis was present in 22.7% of supraglottic tumor and transglottic tumor, whereas only 13.6% of the glottic tumors had positive nodal metastasis. However, no statistical significance was noted (P = .579).
Pathological Nodal Status as per Primary Site of Tumor. a
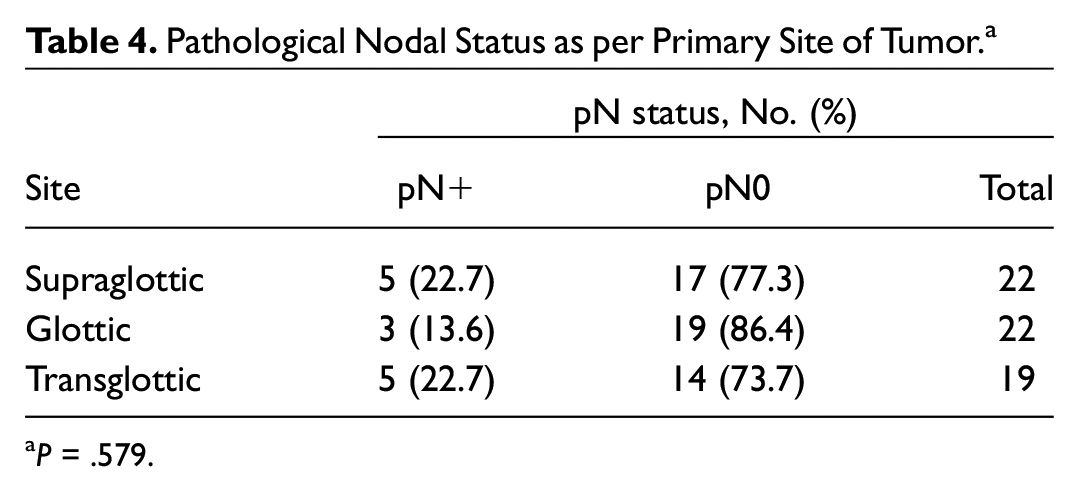
P = .579.
No significant association toward OS and DFS was observed in comparison to whether neck dissection was done in these subgroups. The 5-year OS rates for supraglottic disease without neck dissection and with ipsilateral and bilateral neck dissection were 60%, 80%, and 64.6%, respectively (P = .776), and 5-year DFS rates were 75%, 80%, and 73.9%, respectively (P = .924). The median OS rates for the glottic group without neck dissection and those with ipsilateral and bilateral neck dissection were 79.1 months, 73.9 months, and 77.9 months (P = .883), while 5-year DFS rates were 71.4%, 33.3%, and 82.9%, respectively (P = .232). The median OS rates in transglottic disease for the 3 groups were 20.2 months, 75.0 months, and 46.0 months, respectively (P = .450), and the 5-year DFS rates were 66.7%, 100%, and 61.4% for the 3 groups (P = .487).
When dividing the cohort into early and advanced disease groups (ie, pT1/2 and pT3/4), it was found that 22.8% of the pT3/4 tumors and 0% of the pT1/2 tumors had occult nodal metastasis, and the results are not statistically significant.
As clinical tumor staging is important for preoperative planning in our practice, the effects of clinically early and advanced disease groups are separated for analyses of the correlation with occult nodal metastasis, and it was found to be nearly of clinical significance (P = .059), with the results listed in Table 5 .
Pathological Nodal Status as per cT Stage. a
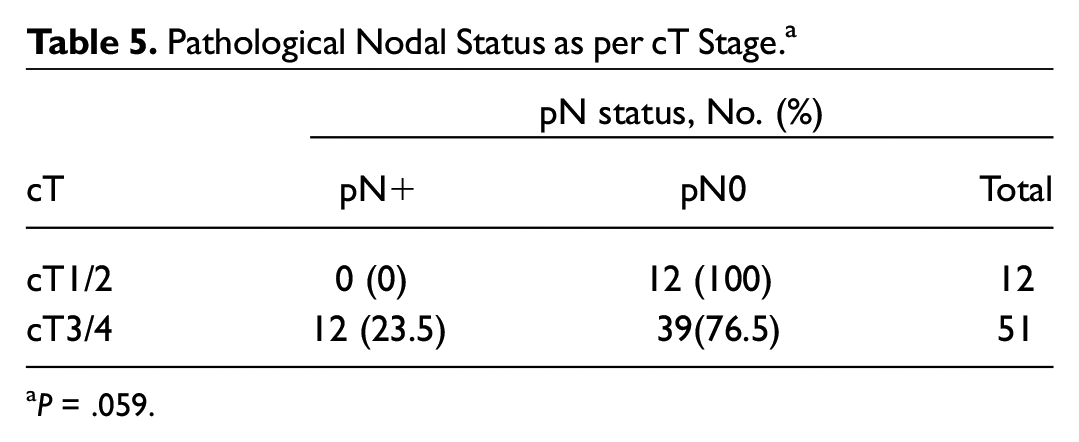
P = .059.
The advanced disease group (pT3/4) was separated for survival analysis. Fifty-five patients in the group had neck dissection done. Of the 10 patients with ipsilateral neck dissection, 3 (30%) patients had locoregional recurrence, while of 45 patients with bilateral neck dissection, 11 (24.4%) patients had locoregional recurrence. However, it was not statistically significant. Similar results were observed when analyzing the clinically advanced disease group, with no statistical significance found in the correlation between different neck treatments and locoregional recurrence (P = .947).
The median OS rates were 74.3 months, 78.1 months, and 77.9 months (P = .708) for the pT3/4 patients without neck dissection and those with ipsilateral and bilateral neck dissection, respectively, and the corresponding 5-year DFS rates were 71.8%, 70.0%, and 73.5% (P = .980). There was no significant effect on OS or DFS observed for the different surgical treatment of the neck in pT3/4 disease, and Figure 2 shows the detailed survival curves. Similar results were observed in the cT3/4 patients, with no significant differences between the OS and DFS in the different neck treatment groups (P = .622 and P = .988, respectively).
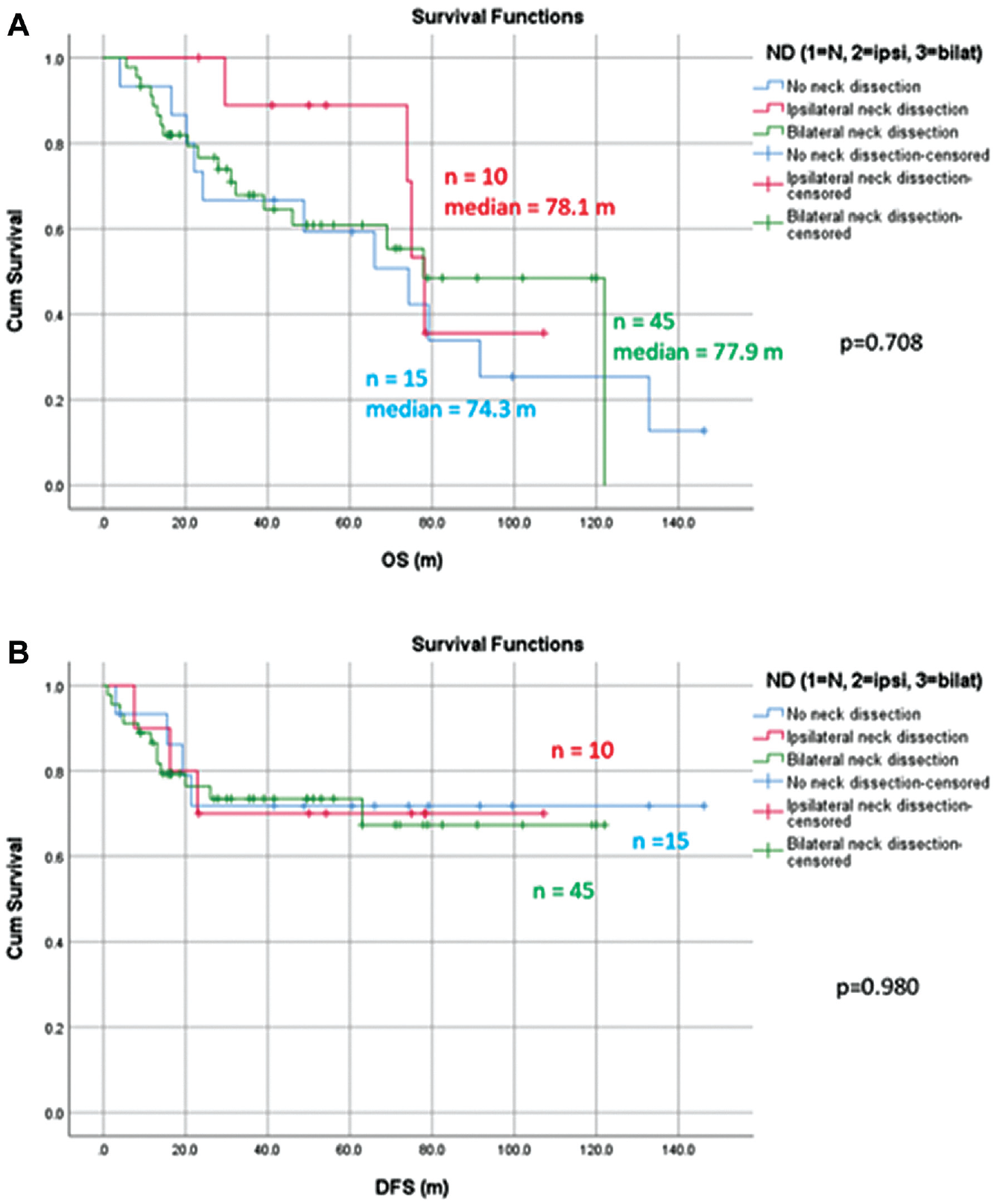
Kaplan-Meier curves depicting overall survival (OS) and disease-free survival (DFS) for pT3/4 disease comparing no, ipsilateral, and bilateral neck dissection.
Total laryngectomy was done for both primary disease and as salvage treatment in posttreatment failure patients. Therefore, subgroup analysis was done for the 2 groups. Pathological nodal status was available in 21 and 42 patients in the salvage group and primary disease group, respectively. Only 1 (4.8%) patient in the salvage group, who had the initial nodal stage of N0 before the first episode of radiotherapy, had positive nodal involvement compared with 12 (28.6%) of the 42 patients in the primary disease group. The results were of statistical significance (P = .045), and details are shown in Table 6 .
Correlation Between Prior Treatment and Lymph Node Involvement. a
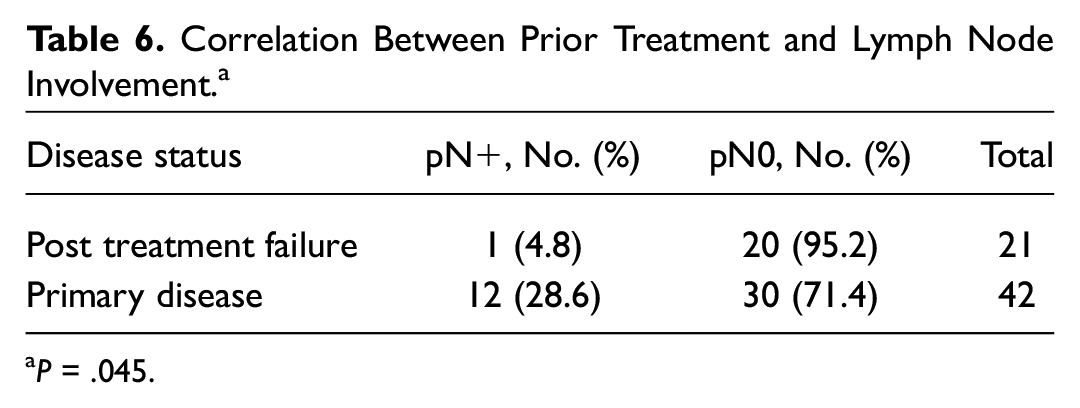
P = .045.
Despite the significantly higher probability for occult neck nodal metastasis in the primary disease group compared with the salvage group, there was no significant difference in the effect of neck dissection on the DFS rate in the 2 groups. The 5-year DFS rates were 83.3%, 80.0%, and 87.5% for salvage patients who underwent no neck dissection, ipsilateral dissection, and bilateral neck dissection, respectively (P = .954), and similar results were observed in the primary disease group (63.5%, 66.7%, and 66.8%, P = .975). Figure 3 shows the survival curves of DFS of the 2 groups.
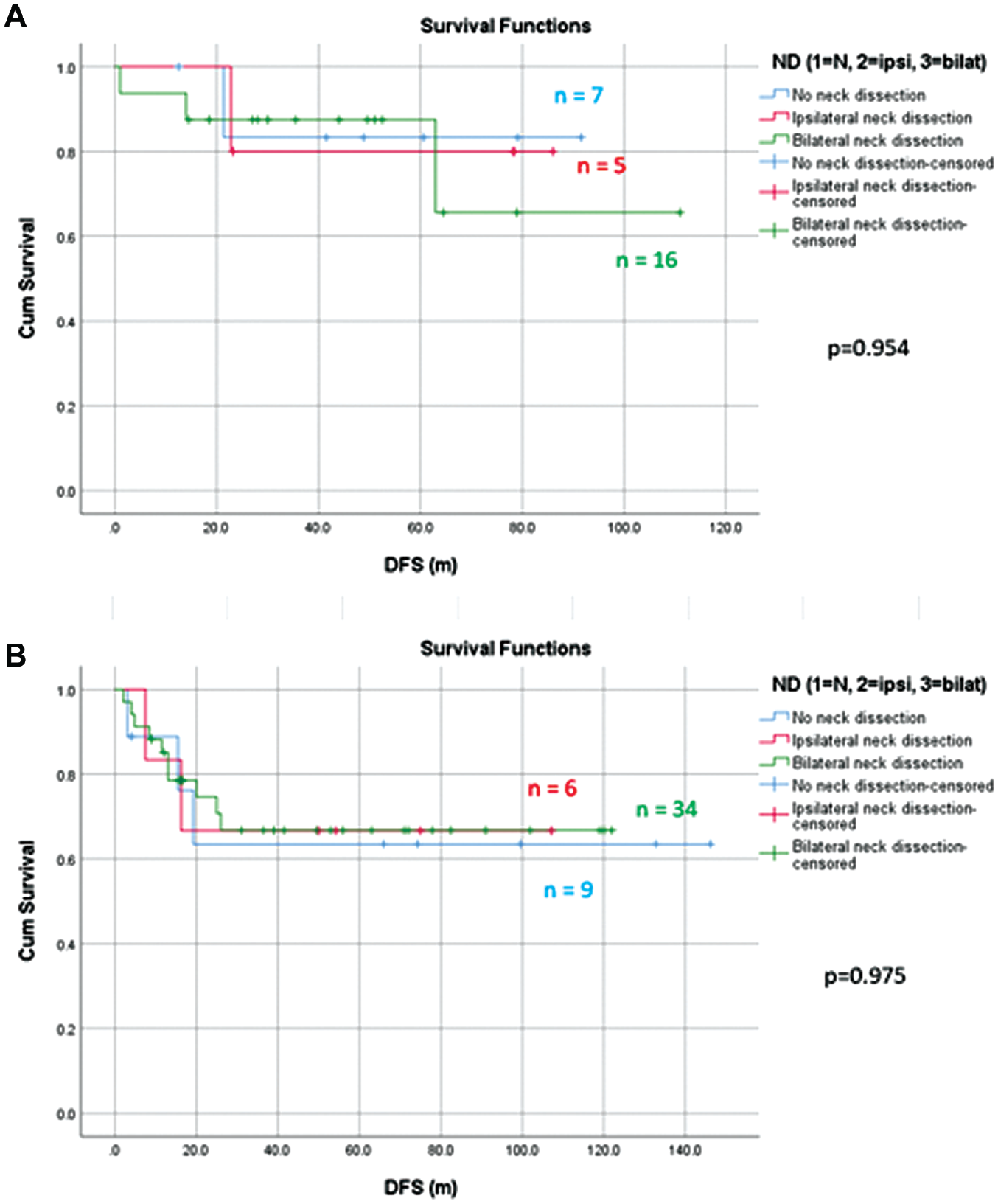
Kaplan-Meier curves depicting disease-free survival (DFS) for the (a) salvage and (b) primary disease groups comparing the effect of no, ipsilateral, and bilateral neck dissection.
As adjuvant treatment of radiotherapy or chemoradiation could potentially affect the rate of locoregional recurrence and hence OS and DFS, patients who had no adjuvant treatment were separated for further analysis. There was 30.8% locoregional recurrence in patients with no neck dissection. In patients who had ipsilateral and bilateral neck dissection, the rates of locoregional recurrence were 25.0% and 25.8%, respectively. The results were not statistically significant (P = .936).
The median OS rates were 66.0 months, 86.0 months, and 77.9 months (P = .297) for this group of patients without neck dissection and those with ipsilateral and bilateral neck dissection, respectively, with the corresponding 5-year DFS rates of 67.1%, 75.0%, and 76.6% (P = .915).
In the 50 patients with contralateral neck dissection and the 2 patients with bilateral neck lymph node biopsy, contralateral neck lymph node metastases were found in 2 patients (3.8%), and the patients’ characteristics are listed in Table 7 .
Characteristics of Patients With Contralateral Lymph Node Involvement.
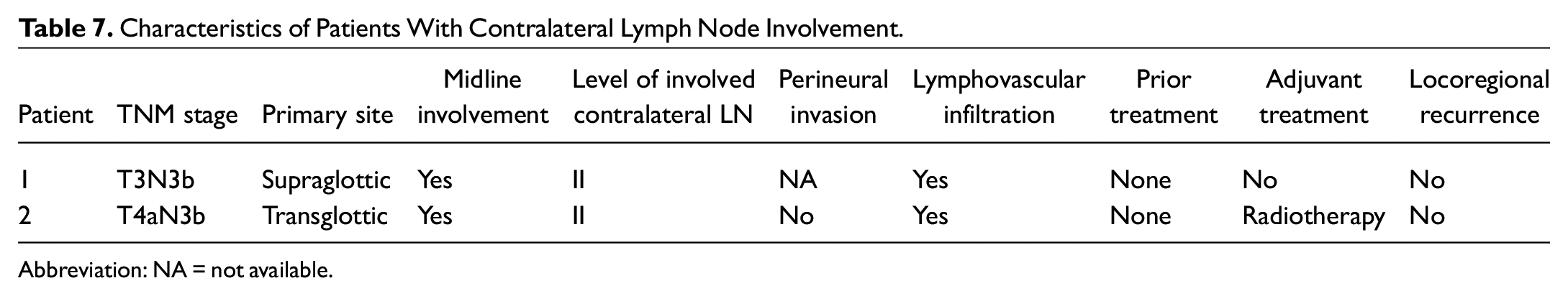

Abbreviation: NA = not available.
It is observed that both patients had locally advanced disease and midline involvement of the tumor. Positive lymphovascular infiltration was also observed in both surgical specimens. They had no locoregional recurrence after the surgery.
Discussion
This retrospective study examined the incidence of occult nodal metastasis, possible clinical predictors, and oncological outcomes in a series of 77 patients who underwent laryngectomy as primary or salvage treatment. In our series, the overall rate of occult cervical nodal disease was 20.6%, but there was no survival benefit demonstrated in patients who underwent ipsilateral or contralateral neck dissection compared with patients with no neck dissection in the whole cohort. In the subgroup analysis of primary laryngectomy, the rate of occult nodal metastasis was 28.6%, which is higher than the standard based on the Weiss et al 3 decision tree analysis to perform elective neck dissection in cN0 patients in the primary setting, yet its application to the salvage setting is not clear. In the salvage laryngectomy group, the rate of occult nodal disease was 4.8%, which was significantly lower than the primary laryngectomy group. A retrospective review of the role of neck dissection at salvage laryngectomy of a group of 171 patients with a history of carcinoma of the larynx (74.9%) and hypopharynx (24.1%) showed that the overall occult metastasis rate was 10.5%, with initial nodal positive disease being the only predictive factor. 4 However, it was not observed in our only pN+ patient in the salvage group. Larger sample size in our locality is needed for further study in this predictive factor. It was suggested that risk of occult nodal disease is higher in advanced T stage (pT3/4 or cT3/4), and supraglottic subsite and elective neck dissection is recommended by some authors based on the results.5-8 However, in our subgroup analysis, there is no significant difference in the rate of occult neck nodal disease regarding the subsites and the pathological T stage, although it nearly reaches statistical significance in the correlation between the advanced clinical T stage and the rate of occult nodal metastases (P = .059). The survival benefit for neck dissection in patients in the previously stated high-risk groups is not significant in this study, and there is no significant difference in the rate of locoregional recurrence between observations, ipsilateral dissection, and bilateral neck dissection in the advanced disease group. Besides, risk of occult contralateral nodal metastasis was low in our series, at only 3.8%. Upon analysis of the 2 cases with contralateral nodal disease, it was found that advanced local disease and midline involvement might be predictive of the occult involvement of the contralateral neck node, which is consistent with recommendations from the National Comprehensive Cancer Network guideline. 9
One important factor to consider is whether an elective neck dissection improves survival in these patients. A few studies reported a survival benefit to elective neck dissection,10,11 yet it was not demonstrated in the recent meta-analyses concerning salvage laryngectomy.12,13 There was no significant benefit demonstrated in both OS and DFS rates regarding neck dissection in the whole cohort and subgroup analysis in our study. However, the results might be limited by the small number of cases included and the postoperative adjuvant treatment given to the lateral neck. These limitations could be addressed with a well-designed prospective and/or randomized controlled trial comparing elective neck dissection to observation of the neck in cN0 laryngectomy. Although no survival benefit is shown in the entire neck dissection cohort compared with observation, there is prognostic value in determining pathological nodal status. Meanwhile, morbidity of the procedure is considered in the decision-making process of whether to perform elective neck dissection, especially in the salvage groups. Although there was no statistically significant increase in the risk of complications in the elective neck dissection group in the meta-analyses,12,13 Basheeth et al 14 found that the incidence of major wound complication is higher in bilateral neck dissection compared with ipsilateral neck dissection, especially in salvage surgeries, which was also observed in our study group despite the small number of complicated patients. Besides, it was reported that neck dissection has been associated with increased fistula formation in the setting of free flap reconstruction. 15 Based on the existing standard and the above data, ipsilateral neck dissection should be offered in patients who undergo total laryngectomy as primary treatment for laryngeal cancer, whereas it may be reasonable for conservative treatment in cases of salvage surgeries. It may also be appropriate to adopt a “wait-and-see” approach to the contralateral neck unless it is an advanced T stage disease with midline involvement.
Conclusion
The likelihood of occult nodal metastasis in cN0 laryngeal SCC with posttreatment failure is low in our series. Occult contralateral nodal metastasis is not common in the studied cohort, and midline involvement of locally advanced disease seems to be good predictor. Neck dissection during a salvage laryngectomy for cN0 disease could be avoided, while observation for contralateral neck might be reasonable in laryngeal tumors without midline involvement.
