Abstract
The purpose of this study was to compare the management of intracranial sinusitis complications in pediatric patients between members of the American Rhinologic Society (ARS) and the American Society of Pediatric Otolaryngology (ASPO). A cross-sectional web-based survey was distributed twice to the ASPO and ARS membership over an 8-month period. The overall survey response rate was 12.1% (7.5% of ARS members and 17.3% of ASPO members). Recommended management was similar with respect to the use of intravenous antibiotics, nasal saline irrigations, topical decongestants, and nasal steroid sprays. Recommendations diverged with regards to systemic steroid use and urgent/emergent endoscopic sinus surgery (ESS). ARS members were more likely to recommend systemic corticosteroids. ASPO members were more likely to recommend immediate ESS. Based on survey responses, we found differences in practice patterns among subspecialists, which indicates additional collaborative research between societies is necessary to develop and disseminate evidence-based guidelines for these patients.
Intracranial sinusitis complications (ISCs) are infrequent but have significant morbidity. Notably, 63% of epidural and subdural abscesses in the pediatric age group are of sinus origin. 1 Children are thought to be more susceptible to such complications due to thinner osseous sinus walls, larger vascular foramina, and patent suture lines.2,3
The initiation of intravenous (IV) antibiotic therapy as treatment of suspected ISC is uniformly accepted. There is less consensus with respect to additional medical and surgical management, including recent literature questioning the benefit of endoscopic sinus surgery (ESS) with respect to outcomes including length of stay, need for revision surgery, transfusion, persistent neurologic morbidity, or readmissions.4,5 The purpose of this study is to evaluate practice patterns among members of the American Rhinological Society (ARS) and the American Society of Pediatric Otolaryngology (ASPO) given the likelihood these 2 subspecialist groups care for children with ISC.
Methods
This survey study was exempt from Boston Children’s Institutional Review Board. An anonymous 8-question survey (see Supplemental Table S1 in the online version of the article) focusing upon management options for ISC was developed. The survey was reviewed and approved by the ARS and ASPO Research Committees and subsequently electronically distributed to both memberships twice over an 8-month period. The survey was accessed via a survey link through Survey Monkey. A binomial regression model with log-link function compared ASPO vs ARS responses. Results were tabulated using RedCap software and R statistical software.
Results
Of the 1504 individuals invited, 182 (12.1%) completed the survey: 66 (7.5%) of 875 ARS members and 110 (17.3%) of 635 ASPO members; 6 respondents reported dual membership.
Almost all respondents (>98%) recommended IV antibiotic therapy. Most respondents recommended nasal saline irrigations (71%-78%), nasal decongestants (79%-85%), and nasal steroid sprays (57%-59%). The use of systemic corticosteroids ranged from 30% to 40% depending upon the specific ISC. Half of the respondents (50%) recommended immediate ESS in the meningitis case, with this percentage increasing to 75% for epidural abscess, 76% for subdural abscess, 76% for cerebral abscess, and 86% for cavernous sinus thrombosis.
ARS members were approximately twice as likely to recommend systemic corticosteroids for all types of ISC ( Table 1 ). Recommendations as to the use of intravenous antibiotics, nasal saline irrigations, topical nasal steroid spray, and topical nasal decongestant did not differ significantly. ASPO members were significantly more likely to recommend urgent/emergent ESS than ARS members for the management of epidural abscess (88% vs 59%), subdural abscess (86% vs 56%), cerebral abscess (84% vs 61%), and cavernous sinus thrombosis (93% vs 74%). There was no significant difference between societies regarding recommended neurosurgical intervention.
Management of Intracranial Sinusitis Complications by Society Membership. a
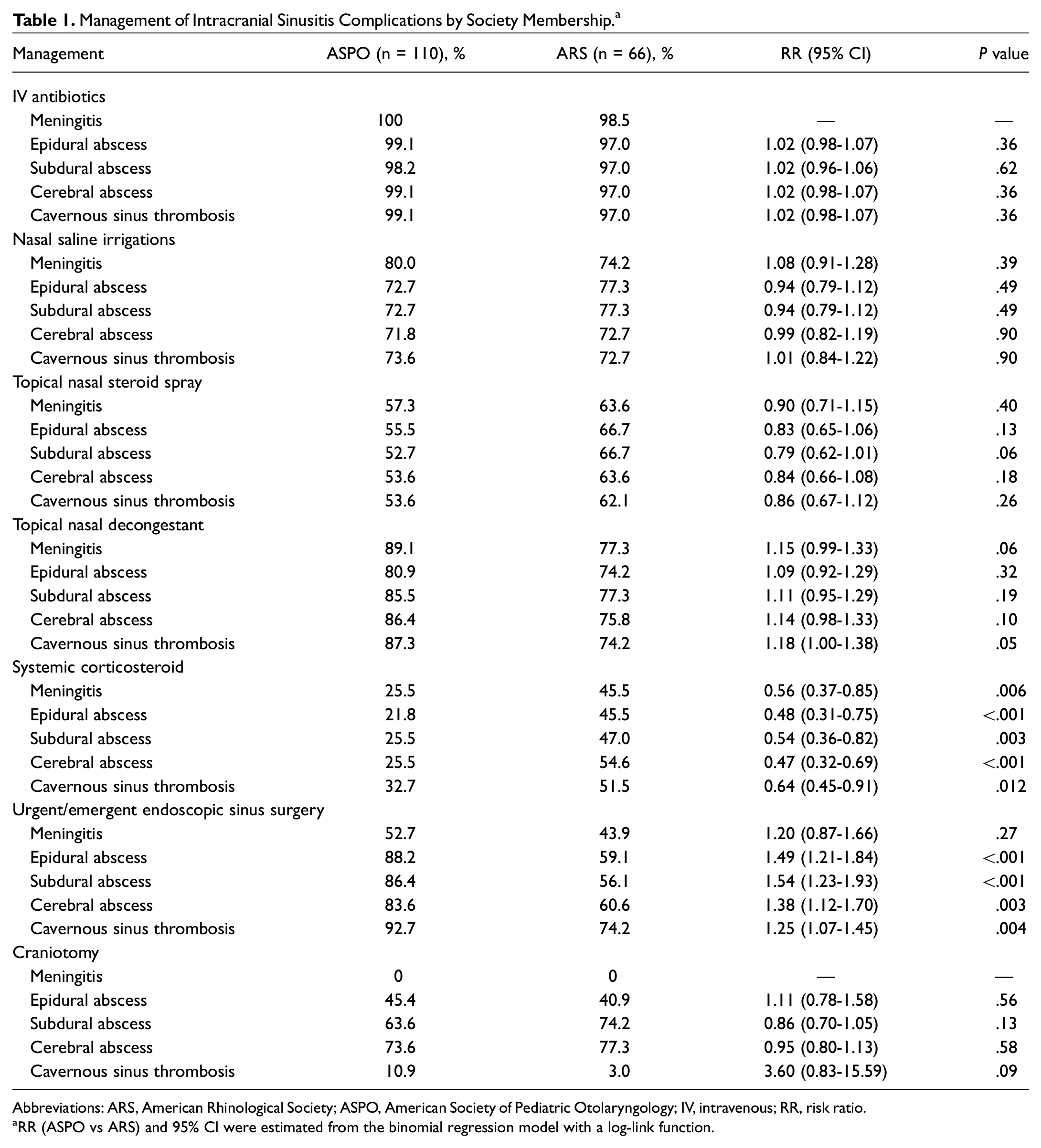
Abbreviations: ARS, American Rhinological Society; ASPO, American Society of Pediatric Otolaryngology; IV, intravenous; RR, risk ratio.
RR (ASPO vs ARS) and 95% CI were estimated from the binomial regression model with a log-link function.
Discussion
This survey demonstrates universal congruence regarding the role of intravenous antimicrobial therapy in the management of ISC. ARS and ASPO members are also uniformly supportive of nasal saline irrigations, topical nasal steroid sprays, and topical nasal decongestants and similarly acknowledge the need for neurosurgical intervention. However, 2 important differences in recommended medical and surgical management are evident according to society membership.
ARS members are more likely to recommend systemic corticosteroids for ISC than their ASPO counterparts. This result contrasts with a prior study reporting ARS members to be nearly 3 times less likely than ASPO members to prescribe systemic steroids for orbital sinusitis complications. 6 The difference in management for orbital vs intracranial sinusitis complications is unclear but likely reflects the lack of established efficacy for systemic steroid therapy for these indications.
With the exception of meningitis, ASPO members were more likely to recommend immediate ESS in the management of all ISC scenarios. Societal differences aside, among the 5 scenarios, the majority of total respondents (ranging from 50% for meningitis to 85.7% for cavernous sinus thrombosis) did recommend ESS. Such is consistent with current literature documenting ESS is performed in most (62.5%-100%) cases.7-13
Despite its frequent use, the benefit of urgent/emergent ESS remains controversial. A retrospective database assessment documented no significant outcome improvement in patients with ISC who underwent ESS in conjunction with a neurosurgical procedure compared to those who underwent a neurosurgical procedure alone. 4 A more recent pediatric-specific ISC case series similarly concluded the benefit of frontal sinus drainage with respect to measured clinical outcomes was unclear. 5 Although ESS is safe in experienced hands, it is still a surgical intervention that requires general anesthesia, and therefore it is important for future research to continue to question whether or not there is a role for ESS in these cases.
This study has several limitations. The response rates, although comparable to those of similar survey-based studies, are unfortunately low.6,14,15 The survey was purposefully brief in an attempt to engage more physicians and increase the response rate. In doing so, questions regarding the timing/duration of therapeutic interventions, comorbidities, orbital complications, and other complicating considerations were not included and may have affected response selections. Finally, survey respondents were subspecialists who practice primarily in academic settings (75.3% of respondents). Their opinions regarding management may diverge from those practicing comprehensive otolaryngology in the community. Although differences in management based on subspecialty may not be clinically relevant, it is important as academic otolaryngologists to recognize there are differences in practice patterns likely due to training and patient populations. This is particularly important when discussing these cases among trainees as they may receive conflicting opinions between subspecialists.
Conclusion
This survey study exhibits some divergences in subspecialty practice patterns and points to the need for more collaborative research to determine optimal ISC management and enhance patient outcomes.
Author Contributions
Disclosures
Supplemental Material
sj-docx-1-opn-10.1177_2473974X221120635 – Supplemental material for Management of Intracranial Sinusitis Complications in Children and Adolescents: Similarities and Differences Among Otolaryngology Subspecialists
Supplemental material, sj-docx-1-opn-10.1177_2473974X221120635 for Management of Intracranial Sinusitis Complications in Children and Adolescents: Similarities and Differences Among Otolaryngology Subspecialists by Eelam Adil, Jamie J. Kim, Kosuke Kawai and Michael J. Cunningham in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
