Abstract
Objective
To evaluate pediatric otolaryngologists, neurotologists, and otologists on awareness and knowledge of congenital cytomegalovirus (cCMV).
Study Design
Pilot cross-sectional online survey.
Setting
Otolaryngology practices.
Subjects and Methods
An electronic multiple-choice questionnaire was sent email listserv to physician members of the American Society of Pediatric Otolaryngology and American Otological Society. The survey assessed demographics, physician awareness, and practice patterns. Data were collected and analyzed.
Results
Seventy (14.5%) pediatric otolaryngologists and otologists responded. All responded that they are familiar with cCMV. Most were familiar with symptoms associated with cCMV with the exception of petechia/purpura. Less than 50% knew the incidence/natural history of cCMV-induced hearing loss. Only 63% knew that saliva or urine polymerase chain reaction/culture should be performed prior to 3 weeks of age. Less than half knew the indications for dry blood spot testing, and many incorrectly recommended serologic saliva or urine testing in a child >3 weeks old. Most respondents do not offer any diagnostic testing for cCMV or referral for antiviral therapy for those who may benefit from this treatment. Most either did not know the cCMV screening policy or did not have one at their institution.
Conclusion
Despite a relatively low overall response rate, this study suggests several knowledge gaps and underutilization of cCMV testing by physicians who frequently encounter pediatric hearing loss. The findings from this pilot study demonstrate the need for further educational directives focused on cCMV to improve knowledge and incorporation of cCMV best practices.
Keywords
Congenital cytomegalovirus (cCMV) has enormous public health implications, as it is the leading cause of neurodevelopmental delay and environmental hearing loss.1,2 Approximately 90% are asymptomatic with no signs or symptoms and 10% are symptomatic. cCMV is considered symptomatic if a child has 1 or more signs of cytomegalovirus (CMV), including thrombocytopenia, microcephaly, intrauterine growth restriction, hepato/splenomegaly, petechia/purpura, hepatitis, central nervous system (CNS) involvement (microcephaly, intracranial calcifications), chorioretinitis, and sensorineural hearing loss. In children with symptomatic cCMV, hearing loss has been reported in up to 75%; those with asymptomatic cCMV will have a 10% to 15% chance of developing hearing loss. 3 Approximately 15% to 35% of patients with bilateral moderate to profound loss are due to cCMV.2,4 Frequently, cCMV goes undiagnosed as children often do not show visible signs of disease. Currently, there are no standard guidelines for screening or treatment in children with asymptomatic cCMV. Utah, Connecticut, and Iowa have adopted hearing-targeted cCMV screening, where children who fail the newborn hearing screen are evaluated for cCMV within the first 3 weeks of life. Given the high likelihood of hearing loss progression in children with cCMV and hearing loss, a screening program allows children to be identified earlier and closely followed.
Despite the burden of neonatal cCMV infections, the knowledge of its symptoms and transmission was poor among medical providers in multiple studies. In a survey distributed by Muldoon and colleagues, 5 35.8% of physical and occupational therapists either had low familiarity or never heard of cCMV. Both Cordier et al 6 and Korver et al 7 found that providers in both the Netherlands and France had poor knowledge of cCMV transmission routes and symptoms.
In light of the poor awareness that has been reported in the literature, we wanted to evaluate the knowledge among otolaryngologists, who frequently evaluate pediatric hearing loss. With the impact of early detection of hearing loss and implication of early treatment with children with cCMV, it is important that the physicians who are likely to evaluate these patients have adequate knowledge of this disease process and its management. In this article, we report the results of a cCMV awareness survey conducted among pediatric otolaryngologists and otologists. While this is a descriptive study, we anticipated that our cohort who regularly evaluate pediatric hearing loss (HL) would have a high degree of awareness and knowledge of cCMV.
Methods
The Emory University Institutional Review Board granted approval for this study. The American Society of Pediatric Otolaryngology (ASPO) and the American Otological Society (AOS) were contacted for approval and access to their email listserv. ASPO is the largest pediatric otolaryngology society and AOS is the largest otology society in the United States. After access was granted, a multiple-choice survey was sent electronically to members of their respective societies, which includes pediatric otolaryngologists and otologists/neurotologists ( Figure 1 ).

Congenital cytomegalovirus awareness survey. Correct answers are in bold.
The email contained a brief description of our study and the hyperlink for the survey using Survey Monkey (Survey Monkey, San Mateo, California). Prior to proceeding, all respondents signed a consent form. The following demographic variables were addressed: sex, age, years of experience, practice environment, and percentage of patients evaluated for hearing loss in their practice. The questionnaire assessed knowledge of signs and symptoms of cCMV, transmission, prevalence and effect on hearing loss, and diagnosis. The last portion queried the current management of cCMV at the individual’s institution. The responses were collected between May and September 2017.
The results were compiled on the online form and then transferred to a spreadsheet using Microsoft Excel (Microsoft Corp, Redmond, Washington). Frequency responses to all questionnaire items were determined, and overall scores were calculated per questionnaire item. This overall score was based on the sum of the correctly stated true answers, assigning 1 point per correct answer. The maximum achievable score varied between 4 and 11 points, depending on the category of the questionnaire item. Prior to performing statistical analysis, some of the groups were combined to increase the total number within a given subgroup. Since our data were nonparametric, we used the Wilcoxon rank-sum test to compare differences in the median between groups, with statistical significance determined as P < .05. The median was calculated using the median function in R. This function provides the value at which 50% of observations are above and below that value. Given our skewed data, the median is a better measure of central tendency than the mean.
Results
Demographics
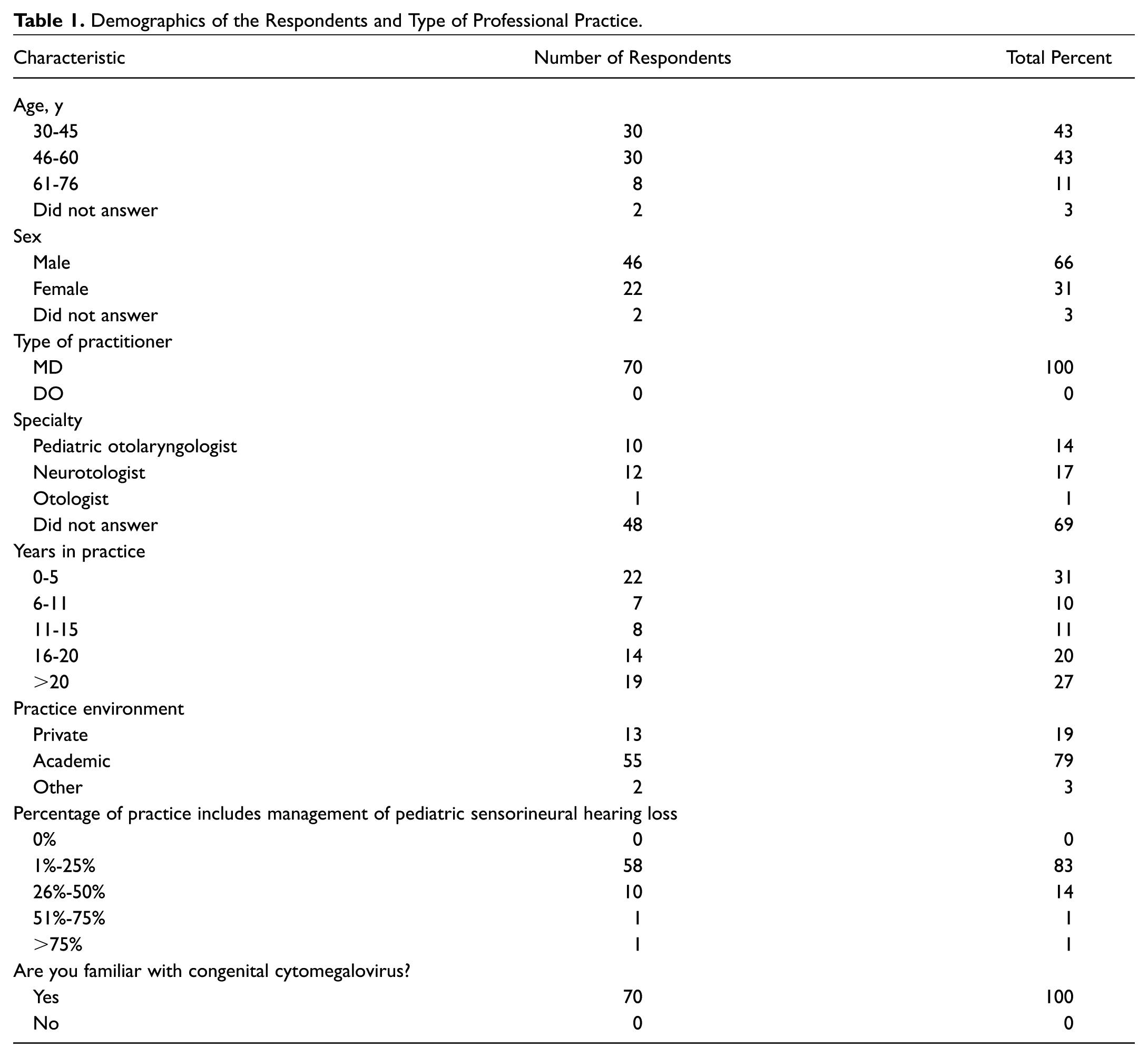
A total of 484 members opened the email link (215 ASPO and 269 AOS), of whom 92 clicked on the link (19 AOS, 73 ASPO). We had a 14.5% response rate, with 70 respondents who completed a majority of the questions. All participants were physicians practicing in pediatric otolaryngology, otology, or neurotology. All respondents stated they were familiar with cCMV. Unfortunately, only 23 responded to what their particular specialty was, with 10 (43%) being pediatric otolaryngologists, 12 (52%) neurotologists, and 1 (4%) otologist. Fifty-four (77%) respondents were in an academic practice. The average age of participants was 48 years (range, 33-76 years), with 68% being male. Years of experience in practice varied with the majority either at the beginning of their career (0-5 years, 31%) or late in their career (>20 years, 27%). Interestingly, 83% of participants stated only 1% to 25% of their practice incorporated management of pediatric HL ( Table 1 ).
Demographics of the Respondents and Type of Professional Practice.
Symptoms and Transmission of cCMV
A majority recognized some symptoms associated with cCMV, especially hearing loss (100%), and 67% to 94% recognized the other symptoms. Nonetheless, only 25 (36%) identified all the symptoms, and 52 (74%) knew >50% of the symptoms associated with cCMV. Of all the symptoms, most were not aware that petechia/purpura could be associated with cCMV. Furthermore, less than half of respondents knew that cCMV was the most common environmental cause of hearing loss, its incidence, and disease progression.
Respondents did not perform as well when asked about methods of transmission; almost one-third of respondents were not aware of the methods. A transmission route for CMV was correctly identified 46% to 61% of the time. However, 19 (27%) correctly identified all transmission routes, with 29 (56%) recognizing >50% of the transmission routes for cCMV ( Table 2 ).
Symptoms and Transmissions of cCMV.
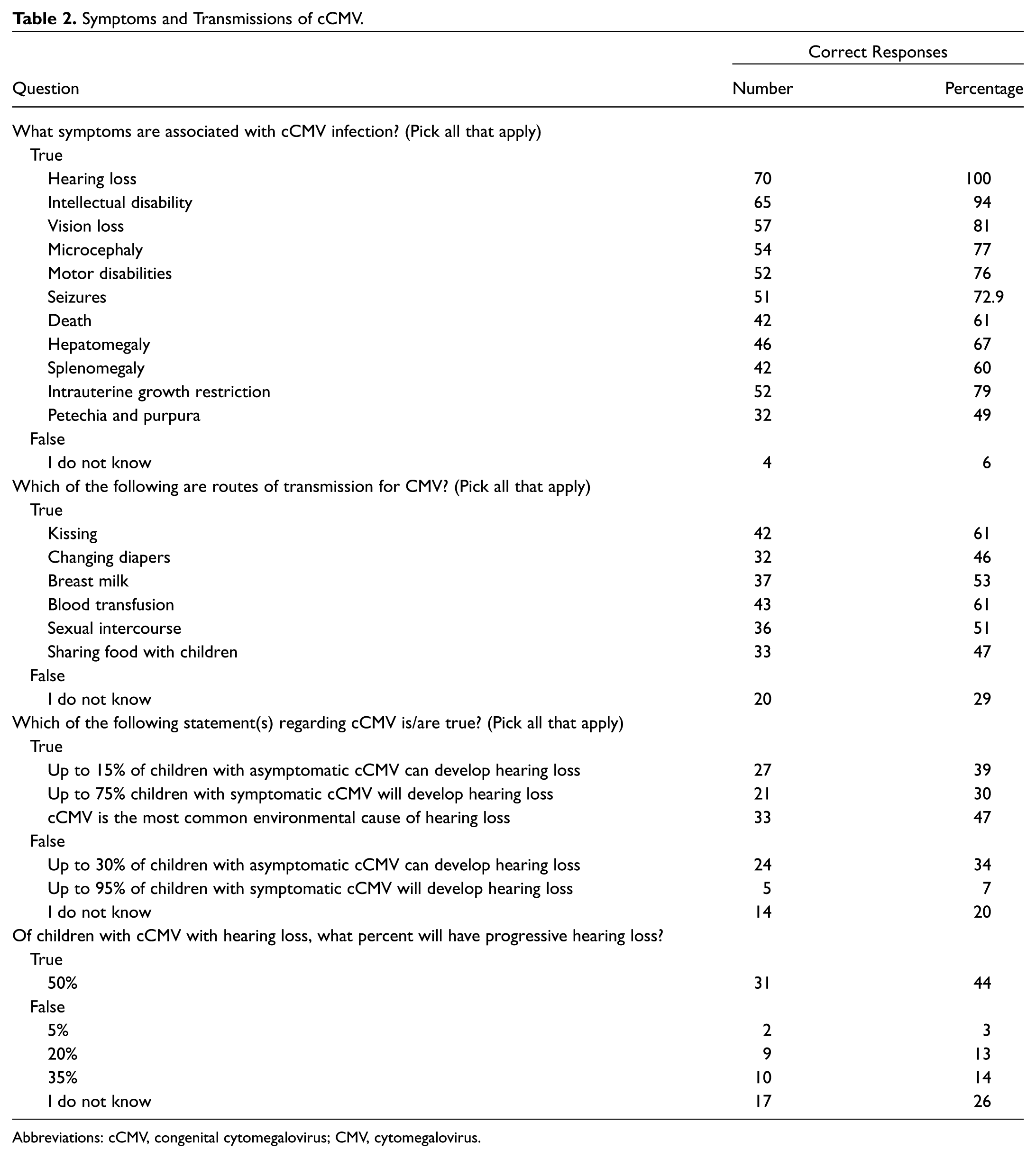
Abbreviations: cCMV, congenital cytomegalovirus; CMV, cytomegalovirus.
Diagnosis of cCMV
Sixty-three percent of respondents correctly identified urine and saliva testing with urine confirmation prior to 3 weeks of age will definitively diagnose cCMV. However, the responses were less clear with definitive diagnosis using the dried blood spot. Only 33% knew that this assay could be used at any age. There was also a poor understanding on what diagnostic methods could be used to definitively diagnose cCMV when the child is >3 weeks old. Only 36% responded correctly with dried blood spot as the only method. Other incorrect answers of using serology, imaging, urine, or saliva testing were selected by 11% to 39% of the respondents. Most participants (64%) did acknowledge that a negative dried blood spot test could not rule out cCMV as the etiology of hearing loss ( Table 3 ).
Diagnosis of cCMV.
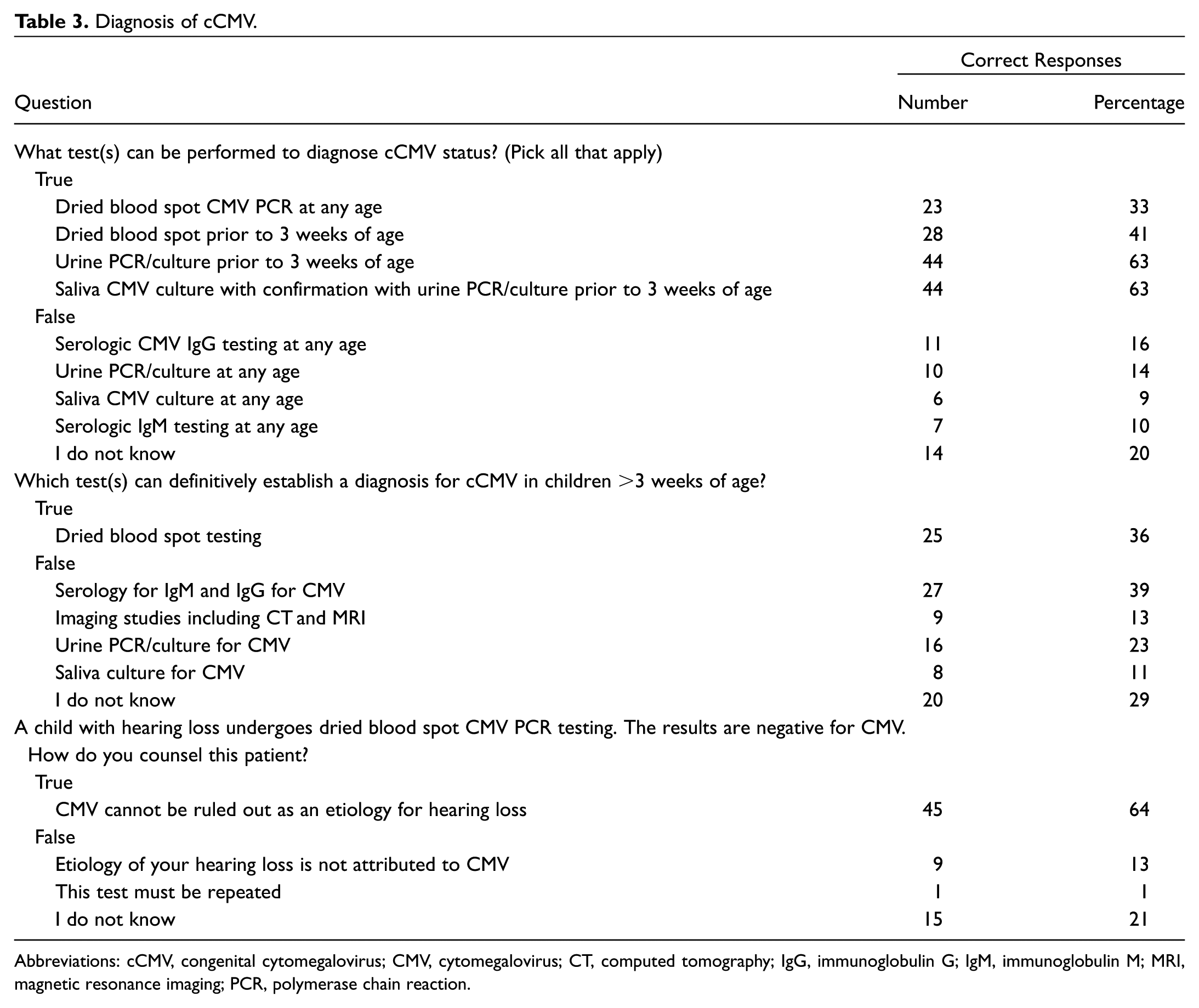
Abbreviations: cCMV, congenital cytomegalovirus; CMV, cytomegalovirus; CT, computed tomography; IgG, immunoglobulin G; IgM, immunoglobulin M; MRI, magnetic resonance imaging; PCR, polymerase chain reaction.
Practice Patterns
Fifty-eight percent of respondents rarely or never incorporate CMV testing for children with idiopathic sensorineural hearing loss. Seventy-six percent do not offer a dried blood spot CMV PCR test. Seventy-four percent either did not have or did not know if early hearing targeted or universal cCMV screening was offered at their institution. Most physicians did not know when to refer a cCMV-infected child for antiviral therapy ( Table 4 ).
Individual Institutional Practice.
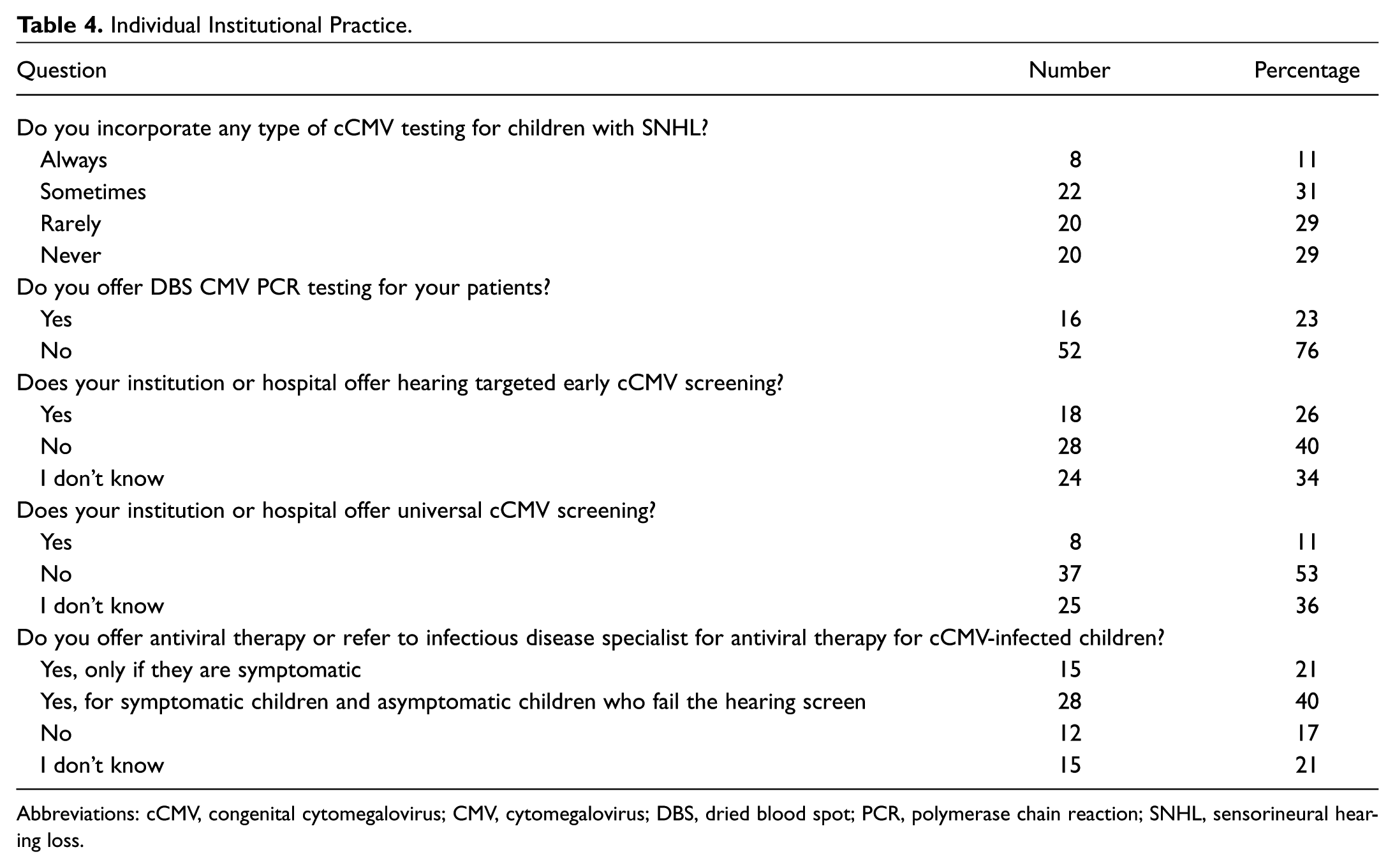

Abbreviations: cCMV, congenital cytomegalovirus; CMV, cytomegalovirus; DBS, dried blood spot; PCR, polymerase chain reaction; SNHL, sensorineural hearing loss.
Comparison among the Groups
In Table 5 , we compared the median scores within each group. Overall, most participants across all groups had their best scores with questions geared toward cCMV symptoms. When looking at the median across all categories, most answered questions regarding the effect on hearing loss and diagnosis of cCMV incorrectly. Within the subset of individuals who saw ≥26% of patients with pediatric HL (12 participants), they performed well in most categories, with the exception of diagnosis (mean score 67). In fact, these individuals outperformed respondents whose practice included ≤25% of pediatric HL with respect to symptoms, diagnosis, and prevalence (P < .05). Although the median value for transmission was also higher for this group, it was not statistically significant. We also identified that participants in academic medicine or in practice ≤15 years performed slightly better compared to those in private practice or in practice ≥16 years, but these differences did not reach statistical significance in any category.
Comparison of cCMV Awareness between Groups. a
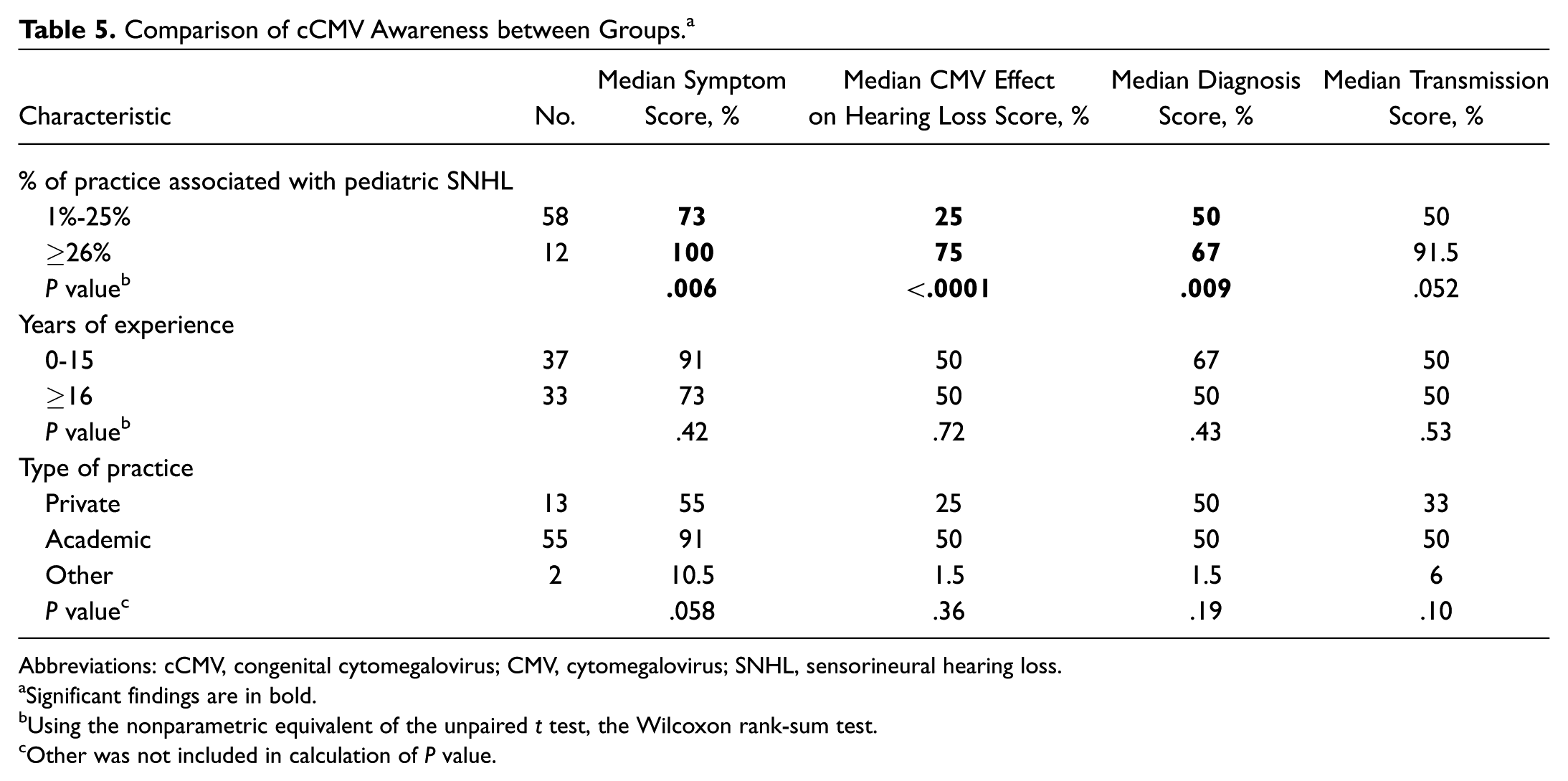
Abbreviations: cCMV, congenital cytomegalovirus; CMV, cytomegalovirus; SNHL, sensorineural hearing loss.
Significant findings are in bold.
Using the nonparametric equivalent of the unpaired t test, the Wilcoxon rank-sum test.
Other was not included in calculation of P value.
Discussion
This pilot survey suggests several knowledge gaps and insufficient implementation of cCMV testing by physicians who are expected to be the most competent to treat pediatric HL. Pediatric otolaryngologists or neurotologists, whose practice encompassed ≥26% of pediatric sensorineural hearing loss (SNHL), outscored their counterparts who evaluated or treated fewer pediatric HL patients. Even this group, however, did not demonstrate an impressive understanding of how to diagnose these patients. This may in part be due to the lack of awareness and the intricacy involved in understanding the virology of cCMV. Furthermore, familiarity of symptoms and transmission may stem from initial training in medical school; however, after this period, there may not be much of an emphasis on cCMV in residency training or as part of continuing medical education, which may account for the results.
All of the physicians who participated in our survey were familiar with cCMV but had little understanding of associated symptoms, natural history, and mode of transmission. Korver et al 7 performed a similar study evaluating physician knowledge in the Netherlands. Most respondents in this study were unaware of transmission through breast milk (34.6%), changing diapers (22.8%), and sexual intercourse (39.8%). Symptoms associated with cCMV were correctly identified by more than 50% of the cohort. Within the subset of physicians, 13 were otolaryngologists; they were correct approximately half of the time with respect to transmission route, natural history, and symptoms.
Only 44% of our surveyed physicians knew that hearing-impaired children with cCMV are likely to develop worse hearing. With respect to the severity of cCMV, 39% correctly identified the percentage of asymptomatic patients and 30% identified the percentage of symptomatic patients likely to experience progressive hearing loss. Only 47% of respondents knew that cCMV is the most common environmental cause of hearing loss. In addition, 26% “did not know” the percentage of progressive hearing loss, and 20% did not know the prevalence of hearing loss within the symptomatic or asymptomatic groups.
One of the most concerning findings from our survey is that many physicians did not know how to diagnose cCMV. Forty-seven percent of respondents did not know that either urine only or saliva with urine confirmation PCR/culture within 3 weeks is required to definitively diagnose cCMV. Sixty-seven percent did not know that dried blood spot testing could be used to diagnose cCMV at any time, even after 3 weeks. In fact, 39% incorrectly believed that immunoglobulin G and immunoglobulin M serology or urine PCR/culture (23%) could definitively diagnose cCMV in children older than 3 weeks. In addition, 20% did not know what test could be performed to definitively diagnose cCMV prior to 3 weeks, and 29% did not know what to order after 3 weeks.8,9 Given this lack of knowledge with diagnostic testing, it is perhaps not surprising that only 11% of respondents routinely order CMV testing for idiopathic SNHL. An international group of pediatric otolaryngologists published a consensus statement recommending that cCMV testing should be done first for idiopathic pediatric SNHL. 10 Park et al 11 reported that 30% of children who presented with idiopathic SNHL were determined to have cCMV when testing was incorporated into a hearing loss evaluation algorithm. They also found that when CMV testing is performed first, this approach had the lowest cost for all types of hearing loss except in the case of auditory neuropathy spectrum disorder. In that case, imaging had the lowest cost when ordered first.
Kimberlin et al 8 studied the impact of treating symptomatic CMV-infected infants younger than 1 month of age with the antiviral drug, valganciclovir. They reported that these infants treated for 6 months had better hearing and neurocognitive scores than those treated for 6 weeks. An earlier trial demonstrated better hearing outcomes in treating symptomatic cCMV infants younger than 1 month of age with ganciclovir compared to those untreated infants. These findings have resulted in a national consensus that symptomatic CMV-infected infants younger than 1 month should be treated with antiviral therapy when diagnosed. However, despite this national consensus, 12 only 21% of the respondents either referred or treated with antiviral therapy infants with symptomatic cCMV. Seventeen percent did not treat or refer to infectious disease, and 21% did not know. The lack of knowledge regarding treatment was also noted in a survey evaluating cCMV awareness among medical students. In that study, 58% of second- through fourth-year medical students either were not aware or did not know treatment existed. 13
The main limitation of our study is a low response rate of 14.5% and a total of 70 participants. In addition, we were not able to determine the specific otolaryngology specialty for most respondents as they did not respond to this question. We cannot exclude correct answers due to guessing as opposed to knowledge. Regardless of these limitations, we believe this initial survey demonstrates a clear lack of knowledge on the diagnosis and treatment of a common condition for otolaryngologists.
Conclusions
Our pilot study highlights the significant knowledge gaps and underutilization of cCMV testing among pediatric otolaryngologists, neurotologists, and otologists. Due to the time sensitivity of definitive diagnosis of cCMV and the high likelihood for otolaryngologists to see this population, we recommend that all otolaryngologists become well versed in diagnosis and management of cCMV. We have proposed the incorporation of additional education directives through our national boards and at the major otolarynogology meetings. Larger studies will be planned over the next 5 to 10 years to reevaluate knowledge and practice patterns after increasing awareness.
Author Contributions
Disclosures
Footnotes
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
This article was presented at the 2018 American Society of Pediatric Otolaryngology Meeting; April 20, 2018; National Harbor, Maryland.
