Abstract

Spontaneous cerebrospinal fluid (CSF) leakage from the anterior skull base is frequently observed in overweight middle-aged women. CSF can be associated with idiopathic intracranial hypertension (IIH) without any triggering event. 1
The most frequent locations involved are the cribriform plate, lateral recess of the sphenoid sinus, ethmoidal roof, frontal sinus, and planum sphenoethmoidalis. 2 However, the leakage associated with the nasal septum/lamina perpendicularis of the ethmoid is rare. In the literature we found only 1 case reported. It describes an arachnoid cyst that, from the anterior skull base, has developed along the perpendicular plate of the nasal septum. 3
Case Report
The Joint Research and Ethical Committee of the University of Sharjah Medical School and the American Hospital Dubai approved this case report.
A 36-year-old woman who was overweight (body mass index, 26.8) with diabetes mellitus type 2 was receiving treatment for a few years for IIH, which caused severe headache. A history of on-and-off watery leakage in the left nostril in the past 2 months was reported. The IIH was treated by acetazolamide (250 mg, twice per day). The office endoscopic endonasal evaluation did not detect any clear sign of leak. Collecting the fluid was feasible with the head bent downward and enforced by the Queckenstedt maneuver. The β2-transferrin positivity in the unilateral left nasal discharge confirmed the fluid to be CSF.
Magnetic resonance imaging and computed tomography (CT), as done in another facility, were not able to clearly identify the site of the leakage. However, it was suspected to be at the left lamina cribra. To better identify the site of the lesion, a CT scintigraphy was performed. A malformation like an arachnoidal prolapse was detected at the level of the lamina perpendicularis of the ethmoid ( Figure 1 ). Pooling of CSF in the left sphenoethmoidal recess was also noted.
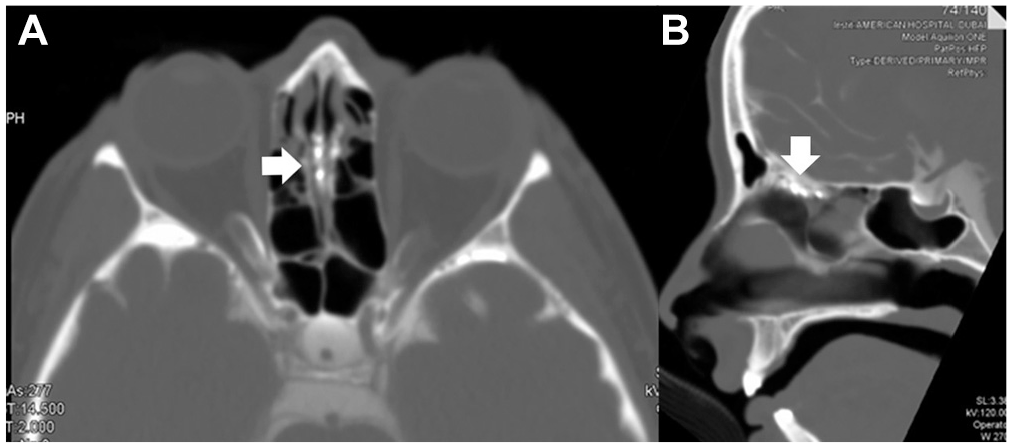
The computed tomography scintigraphy shows the sites of arachnoid prolapse (white arrows): (A) axial and (B) sagittal reconstruction.
Transnasal endoscopic leakage repair was done without using intraoperative fluorescein. To close the fistula, the middle turbinate was used as a donor of bone and mucoperiosteum. To get access to the roof and the lamina cribra, an ethmoidectomy was done. No active sites of leakage from the lamina cribra were detected.
Plentiful CSF leakage was found upon detaching the mucoperiosteum from the lamina perpendicularis of the ethmoid. The sealing of the leakage was done by using a turbinal bone fragment under the periosteum of the lamina perpendicularis, which was then covered by a turbinal mucoperiosteum patch bridged from the lamina perpendicularis to the ethmoid roof ( Figure 2 ).
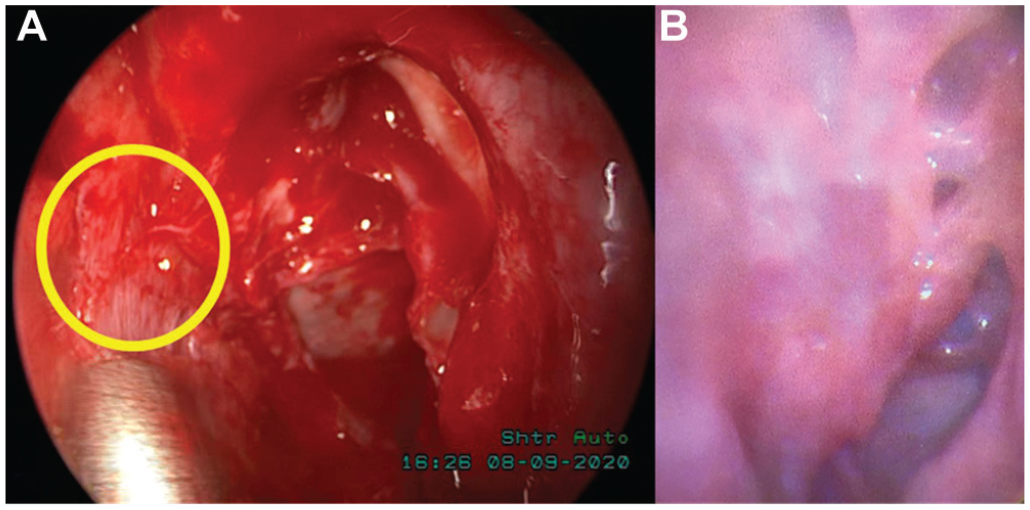
(A) The site of leakage (circle) on the lamina perpendicularis of the ethmoid. (B) The postoperative endoscopic results.
The IIH was treated with 500 mg of acetazolamide twice per day, which was tapered to 250 mg daily 1 month after surgery. As followed by an endocrinologist, the patient lost 5 kg in the first month and was encouraged to continue the diet regimen. After 1 year, no evidence of CSF relapse was observed.
Discussion
This is the second case in the English medical literature of CSF leaks from the lamina perpendicularis of the ethmoid. Routine imaging of the skull base was not able to highlight such anatomic variance, which instead was clearly detected by scintigraphy CT.
In IIH CSF leaks, fistula operations have a relatively high percentage of recurrence if compared with the posttraumatic/iatrogenic closure, reaching 9% in a huge case series. 2 A strict long-term follow-up treating the IIH is needed.
Scintigraphy CT scan can be a useful method to depict leakage in those cases where routine imaging does not.
Conclusion
In the case of CSF leak sites that are not clearly detected, scintigraphy CT adds significant value in the diagnosis. Spontaneous CSF leak from lamina perpendicularis of the ethmoid is rare condition that should not be neglected.
Author Contribution
Disclosures
Footnotes
Acknowledgements
We thank Prof Azzam A. Magazachi, Clinical Sciences Department, College of Medicine, University of Sharjah, for having reviewed the manuscript.
