Abstract

Infectious complications following pituitary tumor resection are rare, encompassing <1% of all pituitary disorder.1,2 Some risk factors for infection include revision surgery, radiotherapy to skull base/sinus, cerebrospinal fluid leak, and sepsis. 3 Nonetheless, recent advances in pituitary surgical techniques, including sellar reconstructive options with various graft materials and local flaps, have kept the complications rates low. Interestingly, bone cements were often utilized in sellar reconstruction. We present 2 cases of transsphenoidal tumor resection reconstructed with bone cement and resulting in infrasellar infection nearly a decade later. This report was deemed exempt by the Kaiser Permanente Hawaii Institutional Review Board.
Case Presentation
Case 1
A 40-year-old woman presented to clinic 10 years after her suprasellar meningioma resection, reporting progressive symptoms of nasal obstruction, hyposmia, and epistaxis. Her initial surgery involved transseptal transsphenoidal and transfrontal craniotomy. She then received radiation therapy for recurrence. Computer tomography scan showed a hyperdense mass in the posterior nasal cavity and nasopharynx with surrounding mucosal thickening ( Figure 1 ). Intraoperative nasal endoscopy showed fragments of calcified bone cement and granulation tissue in the sphenoid sinus and inflammation of the mucosal lining ( Figure 2A ). There was a fibrous and friable mass originating from the left sphenoethmoidal recess, extending down into the nasopharynx. Histopathologic analysis revealed inflammatory mucosal tissue and an infarcted sinonasal polyp. Culture revealed Staphylococcus aureus with resistance to clindamycin and erythromycin. Postoperatively, the patient was treated with antibiotic therapy with resolution of her preoperative symptoms.
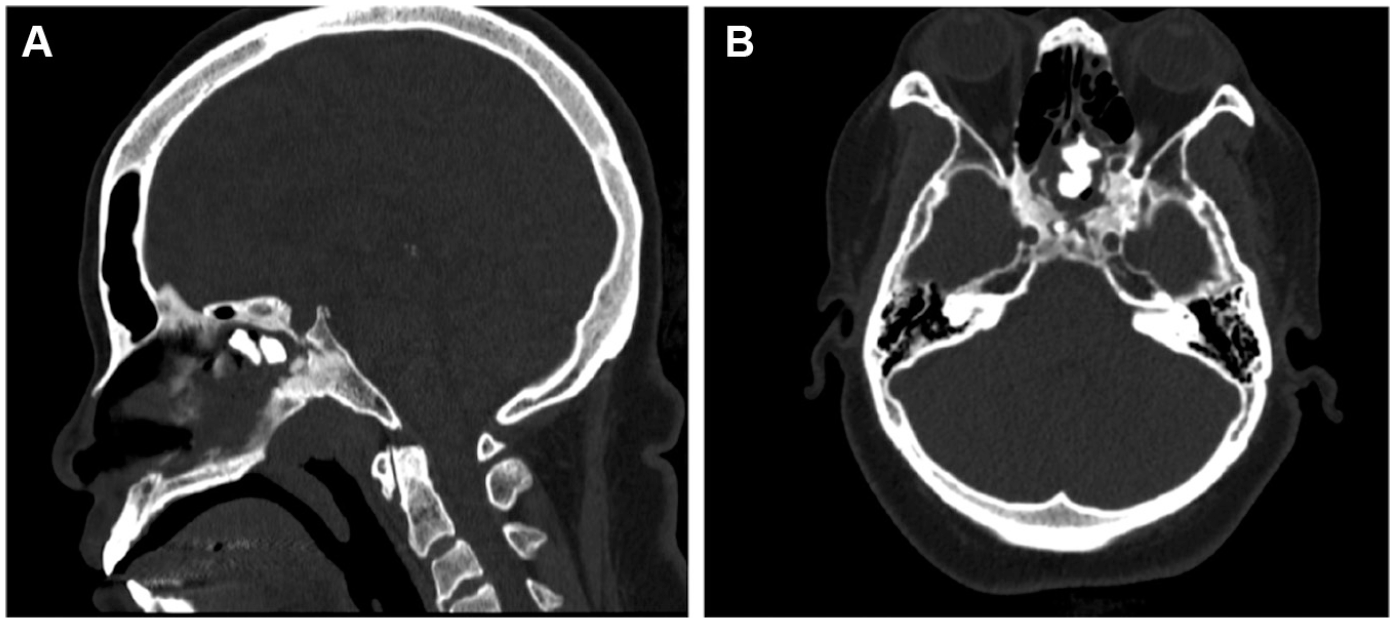
Computed tomography scan demonstrating hyperdense material inferior to reconstructed sellar region: (A) sagittal and (B) axial view.
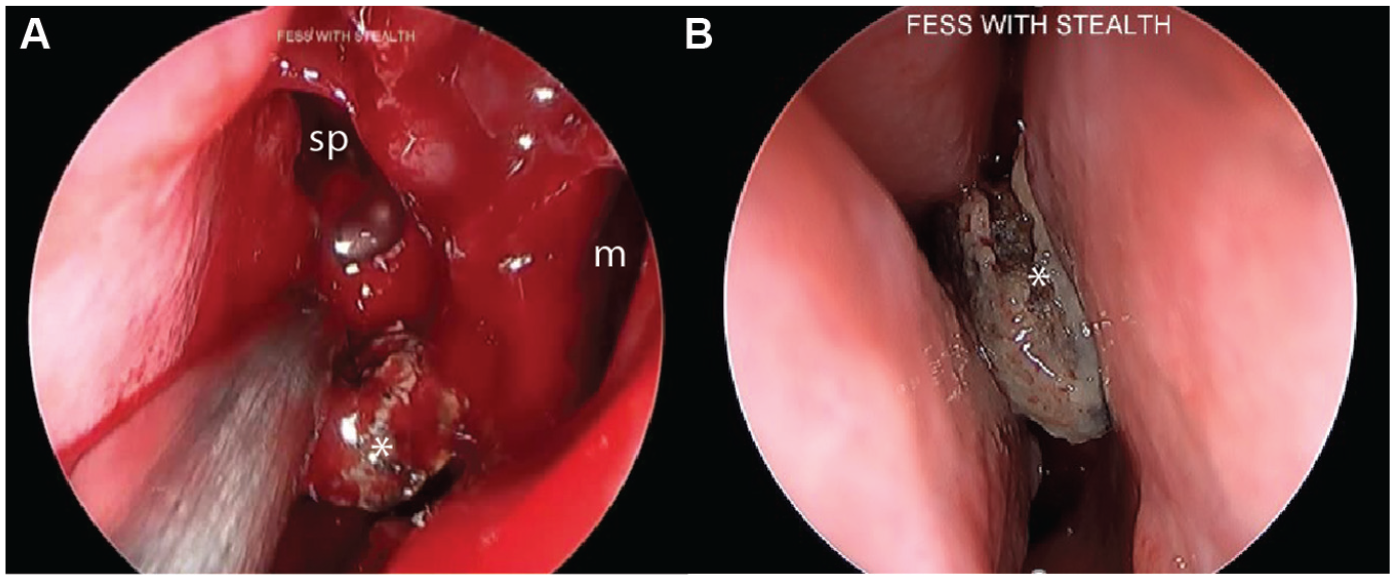
(A) Intraoperative view following removal of bone cement (asterisk) in the left sphenoid sinus (sp). Maxillary sinus (m) is shown. (B) Intraoperative nasal endoscopy demonstrating migrated bone cement (asterisk).
Case 2
A 68-year-old woman with a history of transseptal transsphenoidal pituitary adenoma resection in 2004, which was reconstructed with hydroxyapatite bone cement, presented 13 years later with epistaxis, foul odor, snoring, and right-sided nasal obstruction. Nasal endoscopy revealed dense white material occluding the right nasal cavity, mucopurulence, and surrounding tissue edema. Computer tomography demonstrated hyperdense material in the posterior right nasal cavity with involvement of the ethmoid/sphenoid and sphenoclival region. The patient then underwent endoscopic removal of the infected bone cement. Intraoperative findings included mucopurulence and edema around the bone cement in the right nasal cavity ( Figure 2B ), extending posteriorly to the sphenoclival region. The integrated bone cement was removed with a combination of cutting and diamond burr drill. Intraoperative culture revealed Serratia marcescens, Pseudomonas aeruginosa, and S aureus. Patient was then treated with antibiotics, and her preoperative symptoms resolved.
Discussion
Hydroxyapatite, a form of calcium phosphate abundant in human teeth and skeleton, has been described in the form of cement for reconstruction of the skull base, suboccipital region, and temporal bone. For instance, Snyderman et al described 19 patients who underwent hydroxyapatite cement obliteration of the frontal sinus. 4 They observed infectious complication attributed to bone cement that required explant in 2 patients; a third patient developed a chronic scalp abscess overlying an area where cement became sequestered in an ethmoid air cell. The time to presentation in each patient was not described; however, the longest patient follow-up in this study was 6 years. In addition, Friedman et al reported 31 patients with successful reconstruction of the frontal sinus with hydroxyapatite cement. 5 In their study, 2 patients required cement explant for infection within a year following surgery. The remaining patients at 1-year follow-up continued to have positive outcomes.
Limited data are available on the outcomes of hydroxyapatite use following pituitary and anterior skull base surgery. Interestingly, a recent case report described a female with skull base infection 9 years after endonasal pituitary surgery who had reconstruction with hydroxyapatite bone cement. 3 This patient presented with hypopituitarism, malaise, fatigue, and visual field and acuity deficits. To our knowledge, the case presented by Liu et al and our cases are the only examples of infection occurring nearly a decade following skull base reconstruction with hydroxyapatite bone cement. We postulate that the inflammatory reaction caused by the infected bone cement ultimately led to the breakdown of the cement, with subsequent migration of the material that acted as a nidus for microbial growth. These cases highlight the need to include infected bone cement in the differential diagnosis for patients with infectious nasal/sinus symptoms who have had remote history of pituitary/anterior skull base surgery.
