Abstract

An 8-year-old male patient presented with a firm, fibrous, granular mass completely obstructing the left bony external auditory canal. He had resultant conductive hearing loss but otherwise no pain, otorrhea, or other constitutional symptoms. History was significant for transcanal biopsy of the ear canal component by an outside otolaryngologist 9 months prior, with findings of pathology-defined nonspecific granulomatous tissue with squamous hyperplasia. Four months later, the granulation tissue in the ear canal was found to have recurred. Subsequent computed tomographic scan indicated that the tissue filled the middle ear with extensive bony erosion of the inferior tympanic bone, with extension through the normal position of the tympanic membrane to involve the far medial aspect of the osseous external auditory canal. Magnetic resonance imaging ( Figure 1 ) indicated T1 isointense and predominantly T2 hyperintense enhancing soft tissue in the left infratemporal region centered in the stylomandibular tunnel, encasing the left internal carotid artery at the carotid foramen. The left internal jugular vein was compressed by soft tissue as well. The soft tissue also extended toward the left parapharyngeal space and abutted the posterior margin of the left masticator space. There was bilateral mild enlargement of the retropharyngeal lymph nodes as well. Our initial suspicion was malignant neoplasm due to the sheer extent of disease and bony destruction, as well as the rapid recurrence after resection. The possibility of rhabdomyosarcoma, lymphoma, or other malignancy was discussed with the patient’s mother. Left transcanal tympanoplasty with debridement and serial biopsy of the ear canal and middle ear component was performed under general anesthesia with grafting of the tympanic membrane. Frozen sections indicated the lesion to be histiocytic. Additionally, flow cytometry was performed, ruling out hematolymphoid malignancy. Subsequent definitive diagnosis of extranodal Rosai-Dorfman disease (RDD) was obtained via pathology indicating characteristic emperipolesis and typical immunostaining pattern (S100+, CD68+, CD1a–). The North Texas Institutional Review Board has ruled that the single-patient case report described in this submission does not meet the definition of human subject research and is exempt.
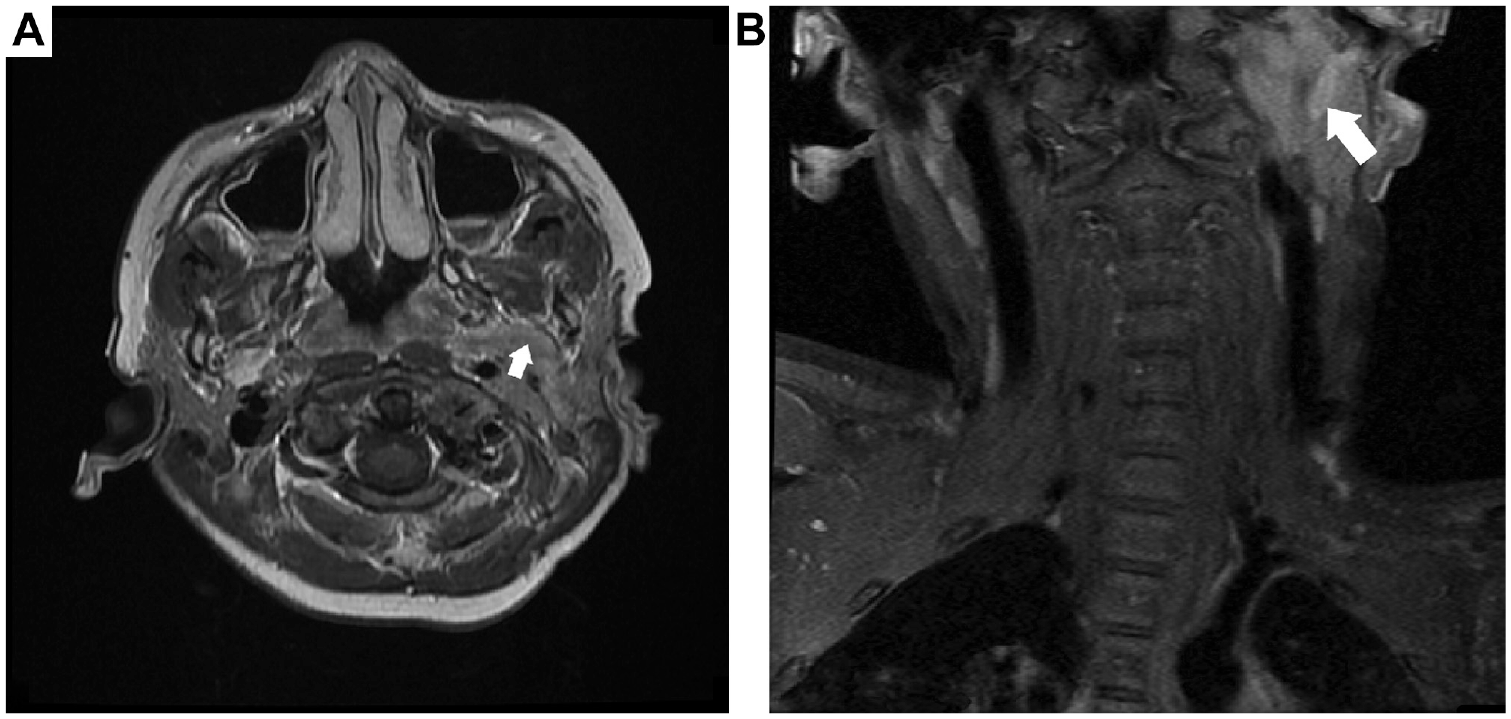
(a) Axial and (b) coronal magnetic resonance images show (arrows) soft tissue mass involving the left middle ear cavity, the proximal left external auditory canal, the left infratemporal region, and the left parapharyngeal space with encasement of the carotid artery.
Discussion
Sinus histiocytosis with massive lymphadenopathy (RDD) is a rare histiocytic proliferation of unknown etiology, classically with cervical lymphadenopathy. 1 Axial, inguinal, and mediastinal lymphadenopathy has also been documented, as well as extranodal involvement. 1 Definitive diagnosis is possible only with immunohistochemical staining and observation of isolated histiocytes with emperipolesis. 1
The differential diagnosis of malignant neoplasms of the temporal bone with infratemporal fossa extension in children includes rhabdomyosarcoma, Hodgkin and non-Hodgkin lymphoma, melanoma, leukemia, and Langerhans cell sarcoma. 2 In 2016, as demonstrated in Table 1 , the American Society of Hematology revised the classification of dendritic cell lineages to include 5 categories, of which the R group includes RDD and noncutaneous, non-Langerhans cell histiocytosis. 3 Tumors of the R group cannot be distinguished from the M group malignant histiocytosis with clinical presentation alone. RDD is most common in children and young adults, in males of African American descent, and classically with cervical lymphadenopathy. 2 However, as in this case, the ultimate diagnosis was RDD without observation of cervical lymphadenopathy. The rate of extranodal involvement in RDD is 43%. 4 This case demonstrates that RDD can present as an extranodal, extracranial middle ear mass visible on otoscopic examination as granulomatous tissue in the external auditory canal, without the additional presence of cervical lymphadenopathy. Documentation and awareness of extranodal RDD without cervical lymphadenopathy are important to temper patient expectations. Extranodal RDD has an estimated mortality rate of 5% to 11%, primarily in patients with concurrent immunologic disease. 5 The true incidence of extracranial RDD without cervical lymphadenopathy is unknown but should be considered in the differential diagnosis of infratemporal fossa neoplasms and may influence clinical discussion with patients about their suspected disease.
Current Classification of Histiocytoses. a
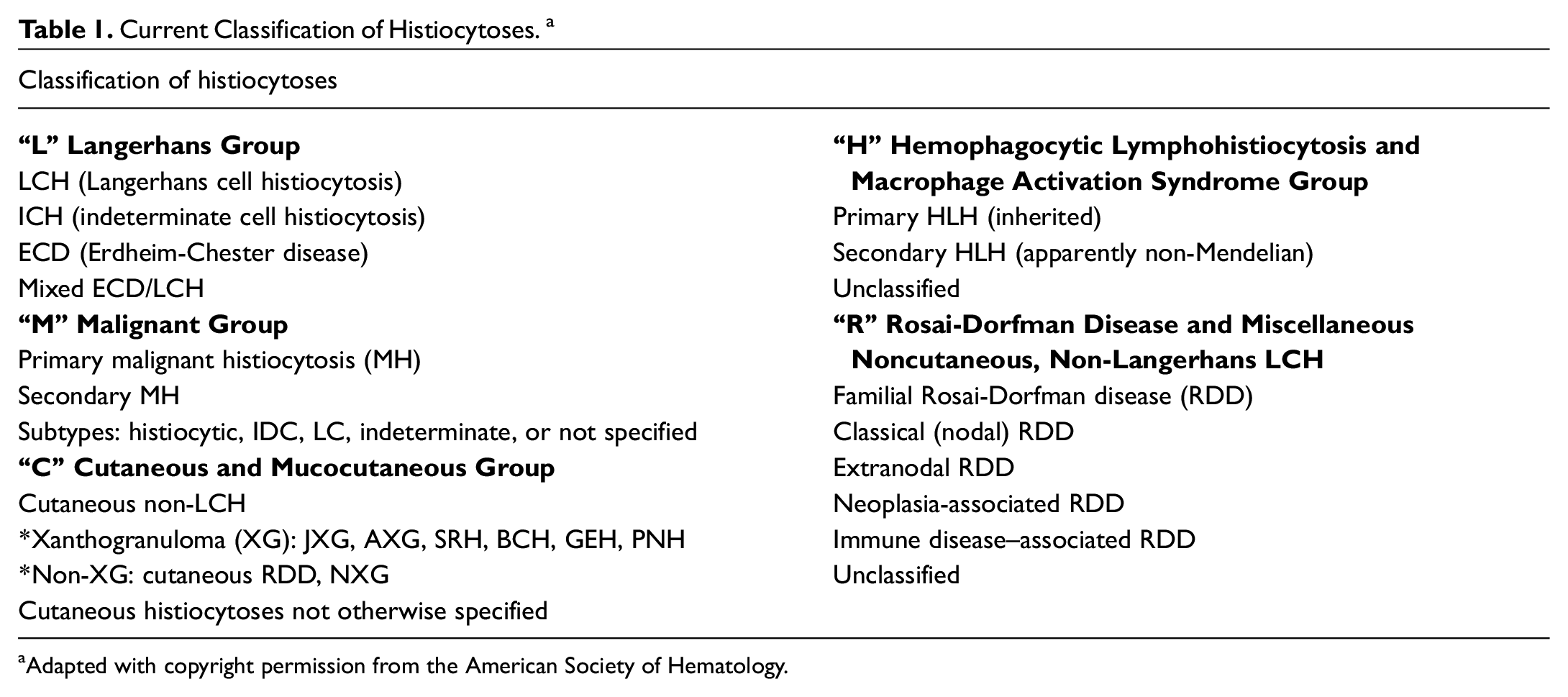
Adapted with copyright permission from the American Society of Hematology.
