Abstract
Objective
To demonstrate longitudinal follow-up for patients who underwent in-office superior laryngeal nerve (SLN) block with lidocaine and steroids for chronic neurogenic cough.
Study Design
Longitudinal follow-up study over 10 months.
Setting
Clinical.
Methods
A retrospective review of 30 patients who underwent in-office nerve block to the SLN for neurogenic cough, including the 10 patients whose outcomes were originally published in 2019.
Results
Thirty patients in this study who underwent a series of SLN blocks showed significant improvement in cough severity index (CSI). The average number of blocks was 3 (range, 2-8). Twelve patients underwent initial SLN block to the left side and 18 patients underwent initial SLN block to the right side. The mean follow-up from the first SLN block was 5.3 months. The mean pretreatment and posttreatment CSI scores were 27 and 11, respectively, for all 30 patients who underwent an SLN block. A Wilcoxon signed rank test shows that there is a significant effect on CSI (
Conclusion
Superior laryngeal nerve block is an effective long-term treatment for neurogenic cough. No additional treatment was required within 10 months of the SLN block.
Level of Evidence
Level IV.
The treatment of neurogenic cough is evolving as more information surrounding the pathophysiology of neurogenic cough becomes published. Neurogenic cough is a chronic cough (more than 8 weeks duration), and a diagnosis is made when common causes are excluded. The aim of treatment is to improve quality of life for these patients by decreasing cough symptoms. 1 The proposed mechanism includes hypersensitization of the larynx and involves the pathways of the superior laryngeal nerve (SLN).2,3 The internal branch of the SLN is the sensory innervation of the larynx. 4 Its anatomical location as it enters the thyrohyoid membrane as well as the integral involvement of sensory receptors within the larynx makes the SLN a target for treatment through a directed approach.
The author’s first study reviewed 10 patients who underwent a series of SLN blocks and demonstrated a statistically significant improvement in cough survey index (CSI) scores. 5 Publications on SLN blocks are growing, many of them demonstrating the feasibility, safety, and ultimately efficacy of peripheral nerve blocks to the SLN. 6 The aim of this article is 2-fold: to demonstrate the long-term effectiveness of SLN block on those original 10 patients and to review an additional 20 patients who underwent SLN block in a series, with reduction on cough symptoms and corresponding CSI scores. Our hypothesis is that there is longitudinal improvement in cough symptoms with a series of SLN blocks, making it a treatment option with long-term efficacy for patients with neurogenic cough.
Methods
Under an institutional review board–approved protocol by Johns Hopkins University, the medical records of all adult patient seen in the clinic from 2017 to 2020 who underwent SLN block were reviewed. Patients were identified by chronic cough
The SLN block was completed in the office with the technique described by Simpson et al. 6 Two milliliters or a 50:50 solution of triamcinolone acetonide 200 mg/5 mL and 1% lidocaine with 1:100,000 epinephrine was injected into the internal branch of the SLN at the thyrohyoid membrane. All patients underwent a single SLN block at 1 visit. The laterality of the SLN block at the first visit was decided upon by palpating along each superior thyroid cartilage toward the ipsilateral thyrohyoid space. If a trigger point was palpated, one that would trigger a cough, the injection was directed to that SLN. For those patients who did not have a trigger point, laterality was standardized to the right side.
All patients in this study underwent a minimum of 3 blocks based upon results of our previous study as well as Simpson et al, 6 spaced between 2 and 3 weeks apart. The main outcome was an improvement of at least 50% or more in cough symptoms. This was determined subjectively by questioning the individual patient. The patient continued with the blocks until their cough improved 50%. A contralateral SLN block was performed at each visit, independent of any palpable trigger point to the opposite side. No concurrent bilateral SLN blocks were performed. All patients filled out a CSI before each start of treatment on initial consultation and before each sequential SLN block. This was recorded in their electronic medical record. Longitudinal follow-up on the original 10 patients was completed by collecting CSI scores by encrypted correspondence through the patient’s electronic medical record. The longitudinal CSI score was determined upon the most recent correspondence.
Complications were defined as direct sequela of the SLN block that included negative changes to voice, breathing, or swallow function, measured by patient-reported symptoms. Any other noted patient-reported complaints were recorded as side effects of the SLN block.
Medical chart review included patient demographics, previous cough workup, indications for the SLN block procedure, and CSI scores.
7
The number of SLN blocks was recorded as well. Statistical analysis was done using the Wilcoxon signed rank test. A
Results
Thirty patients underwent SLN block for treatment of neurogenic cough between 2017 and 2020. Since the publication of the author’s first study, 5 an additional 20 patients have undergone SLN blocks. The original 10 patients did not require further SLN blocks.
All patients had a diagnosis of neurogenic cough based upon previous workup by gastroenterology, pulmonology, allergy, and review of medication lists. All 30 patients were included in the analysis. Table 1 displays demographics, number of SLN blocks, laterality of initial block, pre- and posttreatment CSI scores, and length of follow-up for each patient. Table 2 demonstrates the longitudinal follow-up for the original 10 patients and their most recent CSI score at last correspondence. Of the 30 patients, the mean age of the patient population was 53 years (range, 30-83 years), with 8 males and 22 females. The mean duration of cough prior to initial SLN block was 11.5 years (range, 1.5-30 years). None of the patients in our study were on concurrent neuromodulator therapy for cough treatment. All patients saw our SLP team for at minimum 1 session (1 hour) of respiratory retraining therapy and cough suppression techniques.
Demographics of 30 Patients Who Underwent SLN Block.
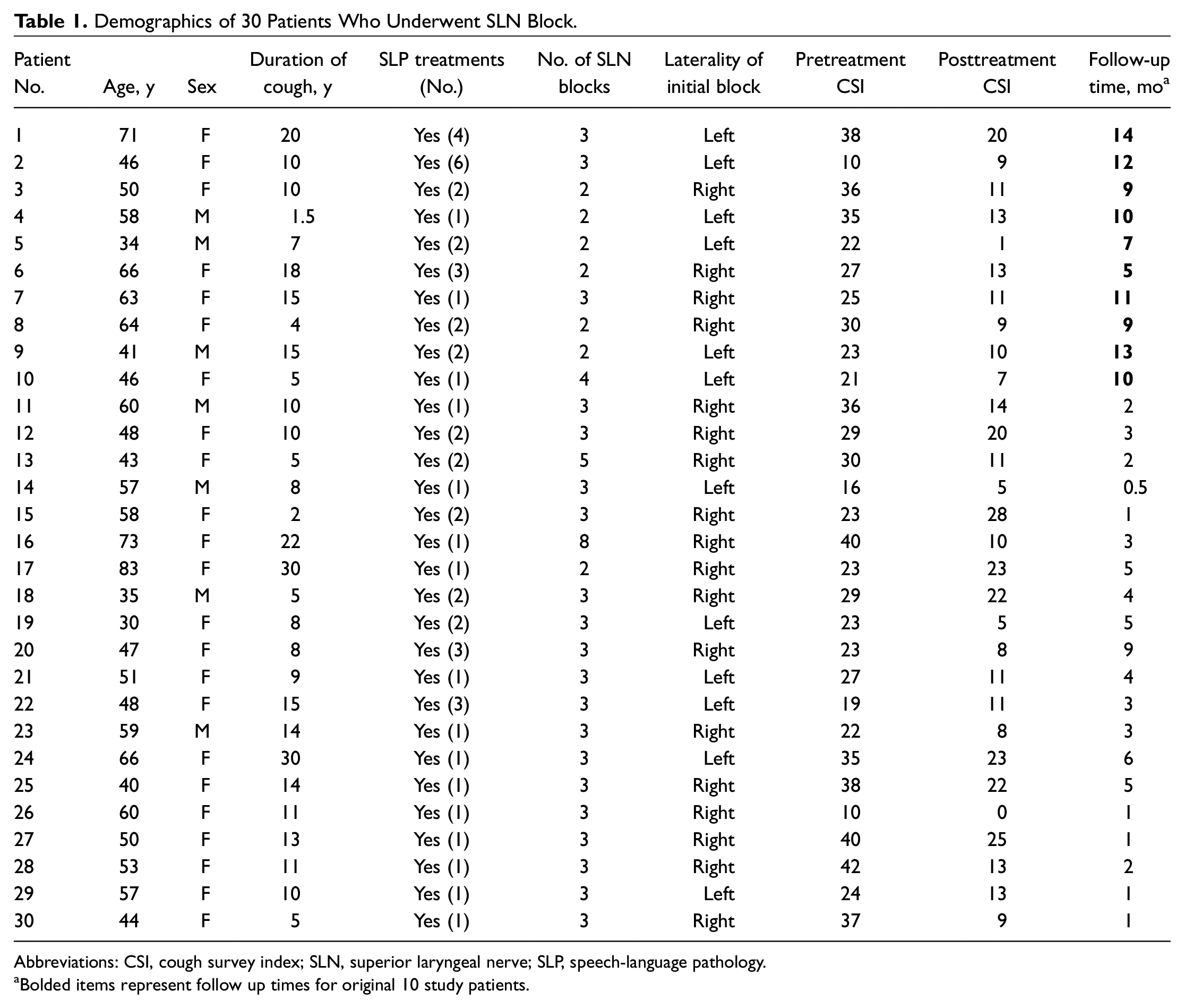
Abbreviations: CSI, cough survey index; SLN, superior laryngeal nerve; SLP, speech-language pathology.
Bolded items represent follow up times for original 10 study patients.
Demographics of Original 10 Patients Who Underwent SLN Block With Longitudinal Follow-up After Treatment.
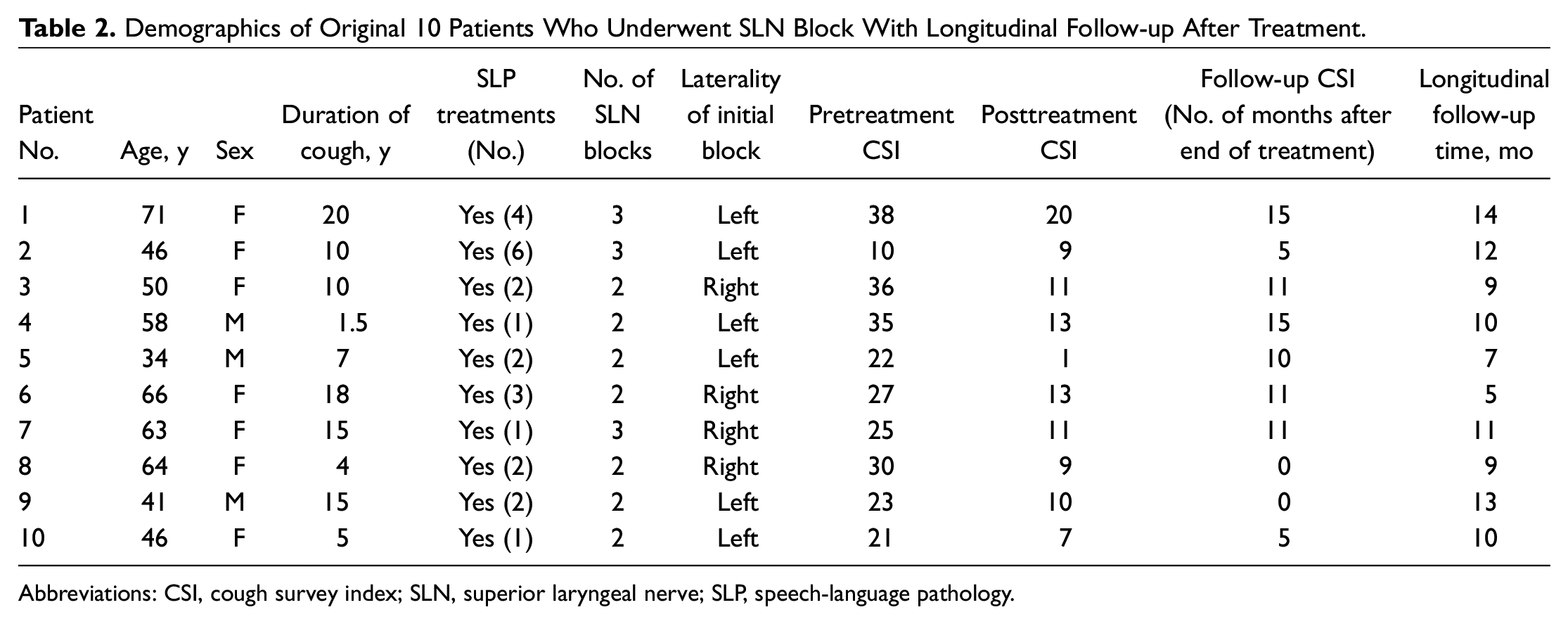
Abbreviations: CSI, cough survey index; SLN, superior laryngeal nerve; SLP, speech-language pathology.
Twenty-eight patients reported improvement in their cough after completing the SLN block. Two patients had no improvement in their cough symptoms, and none reported worsening in their symptoms. Twenty-seven patients underwent 3 blocks. Three patients underwent more than 3 blocks. Two patients who underwent 3 blocks did not have any change in their cough symptoms. Overall, patients underwent an average of 3 SLN block procedures (range, 2-8). Twelve patients had a left-sided trigger point on palpation, and therefore laterality was to the left for the first SLN block. Of the remaining 18 patients, 10 patients had right-sided trigger points. Eight patients underwent right-sided SLN block as this was the standardized side in the absence of a trigger point. The mean interval between blocks was 14.9 days. The mean follow-up time was 5.3 months. Excluding the 10 patients from the original study, the mean follow-up time of the other 20 patients was 3.1 months.
The longitudinal follow-up for the original 10 patients whose results were published in 2019 5 is listed in Table 2 . The mean follow-up time was 10 months (range, 5-14 months) with no patients requiring or receiving additional treatment for their neurogenic cough.
CSI scores were obtained for all 30 patients at initial presentation and at the most recent follow-up visit, after the final SLN block. There was a statistically significant decrease in CSI scores after treatment. Mean pretreatment and posttreatment CSI scores were 27 and 11, respectively, for all 30 patients who underwent an SLN block (
Figure 1
). A Wilcoxon signed rank test shows that there is a significant effect on CSI (
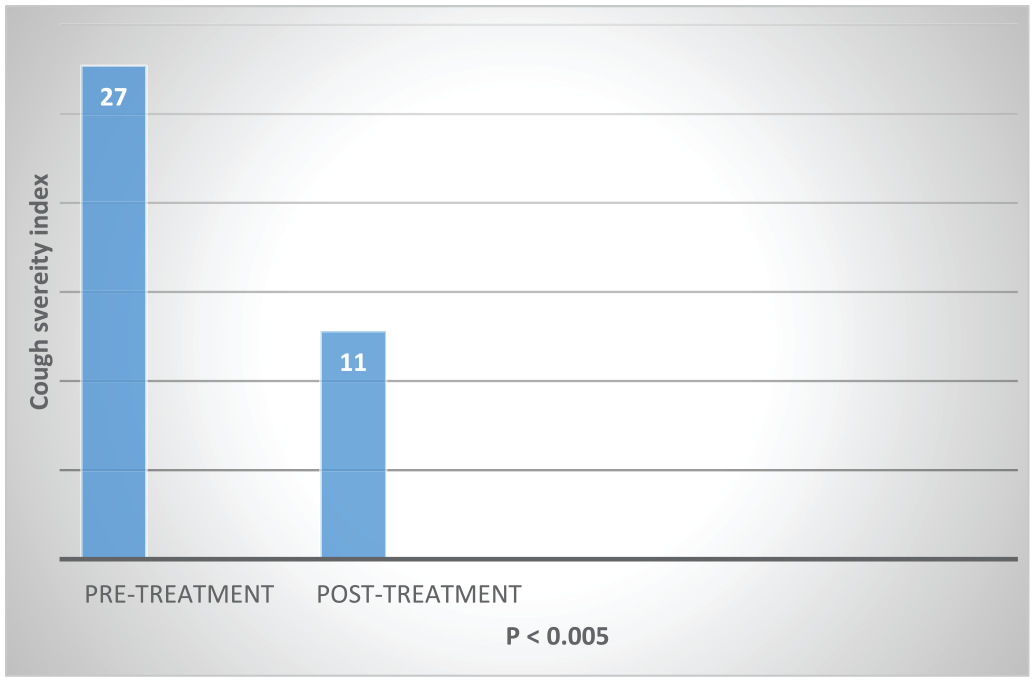
Mean pre- and posttreatment cough survey index scores for all 30 patients who underwent superior laryngeal nerve block for treatment of chronic cough.
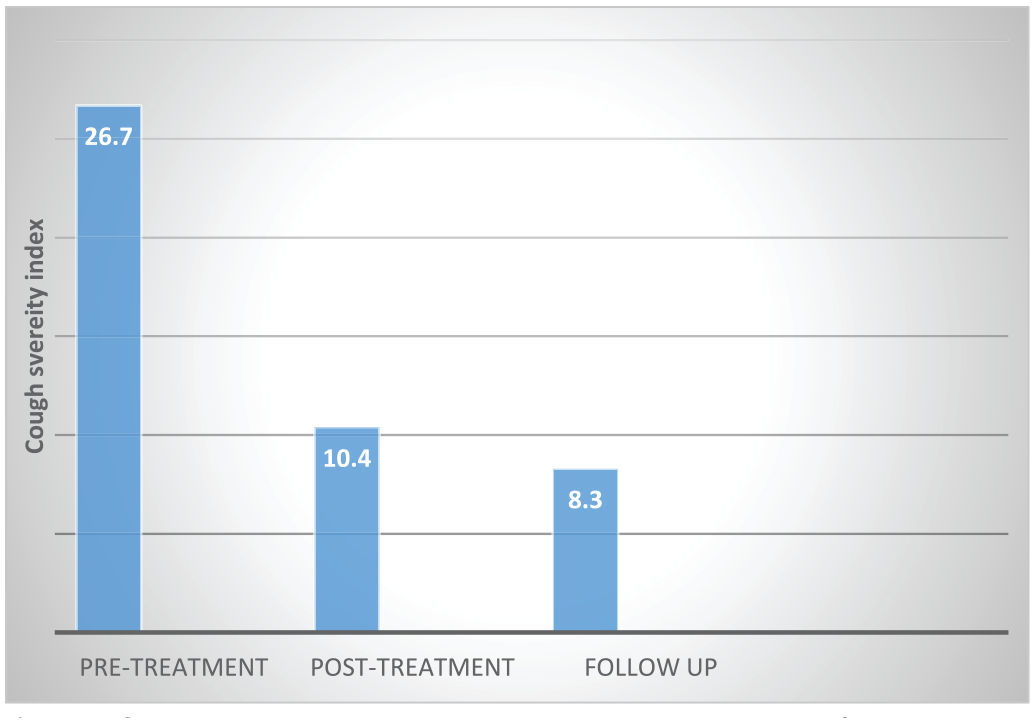
Mean pre-, posttreatment, and longitudinal follow-up cough survey index scores for the original 10 patients who underwent superior laryngeal nerve block for treatment of chronic cough.
There were no complications in our study. Ten patients noted a side effect of transient laryngeal anesthesia within the first 24 hours that occurred immediately after the injection on the side ipsilateral to the SLN block. Patients described this as “numbness” or a “lump in the throat” sensation. None of these symptoms lasted more than 24 hours. One patient noted swelling in the location of the injection that lasted 24 hours and fully resolved. One patient with type 1 diabetes noted an increase in her blood sugar levels monitored by an insulin pump and required additional insulin dosing the day of her SLN block. There were no long-term sequelae to blood glucose levels.
Discussion
This is a follow-up study to our original study that discussed the feasibility and efficacy of SLN block for neurogenic cough. 5 The results of this study demonstrate that there may be long-term benefit for patients receiving SLN block, within 10 months of treatment. The use of SLN block in the treatment of neurogenic cough has become more widespread within the field of laryngology. To our knowledge, the only published data on the efficacy of SLN block have been that of Simpson et al, 6 but the American Laryngological Association recently published an online resource guide to illustrate that the nerve block is among the treatment modalities for neurogenic cough. 8 There is registration of a clinical trial on the ANZCTR (Australian New Zealand Clinical Trials Registry) that aims to evaluate the role of SLN block vs placebo over the course of 12 months (ACTRN12619000237189p). 9
In this study, the original 10 patients who underwent SLN block had a mean follow-up of 10 months without requiring further treatment for neurogenic cough. Simpson et al 6 reported a mean follow-up time of 85.4 days. The mean follow-up CSI score was 8.3, with a statistically significant improvement in CSI scores pre- and posttreatment.
Studies evaluating the efficacy of neuromodulators have demonstrated good short-term effects but mixed results on long-term effects on chronic cough. Bowen et al 10 demonstrated that gabapentin and tricyclic antidepressants like amitriptyline showed short-term improvement in cough symptoms within 2 months, but most patients discontinued treatment prior to 6 months because of the risk for tachyphylaxis and side effect profiles. Gilberto et al 11 completed a meta-analysis of retrospective studies, a small randomized controlled trial, and prospective studies on gabapentin, amitriptyline, pregabalin, and baclofen and showed that side effect profiles of these medications limit the long-term efficacy of neuromodulators years after treatment. 12 On the other hand, our study suggests that SLN block may have some long-term effect on the cough reflex, by direct injection of a lidocaine/steroid compound. The use of triamcinolone in this as well as the previous study is based upon methodology per Simpson et al 6 inferring that there may be benefit through an anti-inflammatory pathway. Based upon our patient-reported outcomes, the systemic side effects of SLN block are minimal compared to the side effect profiles with a variety of neuromodulators. One patient in our study noted a change in blood glucose levels.
The decision to complete at minimum 3 blocks for our additional 20 patients was based upon the results of our original series, which demonstrated an average of 2.3 blocks as being successful in improving cough symptoms by 50%. Bilateral injections were avoided given the reported risk of aspiration. 6 The number of SLN blocks and criteria for continued blocks were based upon patient-reported outcomes. In this study, the 2 patients who did not have any improvement in their symptoms after 3 blocks were given the recommendation to continue but did not want to pursue further injections. The lack of a response in these 2 patients may represent a refractoriness to the block method but may also be secondary to the placement of injection, which is based upon landmark palpation alone. This may be operator dependent as well. There are limitations in using patient-reported outcomes as the main outcome for determining number of blocks and need for continued blocks, as this presents bias. Further objective instruments need to be developed such as routine testing of SLN sensory thresholds to consider maintenance of triggers with a dedicated cough threshold. This would likely assess how SLN blocks interfere with any infectious, chemical, and mechanical triggers that induce the afferent pathway of the SLN.13,14
The advantages and disadvantages of SLN block have been described previously.5,6 None of the patients in this study experienced any significant complications related to the procedure. One important complication is the embolization of materials into the vasculature of the neck, none of which occurred in our study. 6 The use of a steroid solution vs particulate steroid may be an option to prevent this, but this needs further investigation. This study has limitations, in that it is retrospective and includes potential patient and treatment bias given the subjective outcome of measuring patient-reported cough responses. Given the retrospective nature, there is a lack of a control group. Furthermore, our results were consistent with our working hypothesis, in that there was sustained improvement of cough symptoms 10 months after treatment. To our knowledge, this is the largest published retrospective review of patients with neurogenic cough who have undergone SLN block. Patients within our study did not express the desire to change to another treatment option during the course of the SLN block. A minority of patients who were informed of the treatment options prior to the office visit preferred the SLN block over medical management of their cough given their knowledge of the side effect profiles with neuromodulators. There is no current standard of care for neurogenic chronic cough as a diagnosis of exclusion when complete workup for the other causes of chronic cough is negative. A prospective randomized study is the next step in further elucidation of SLN block over other treatment modalities for this subgroup of patients.
Conclusions
This aim of this study was to review a larger cohort of patients undergoing SLN block for neurogenic cough. Our results were consistent with our working hypothesis, in that there was sustained improvement of cough symptoms after SLN block 10 months after treatment. SLN block is a viable treatment modality for neurogenic cough but requires longer follow-up and a prospective investigation with objective instrument measures to determine a treatment paradigm.
Author Contributions
Disclosures
Footnotes
This article was presented virtually at the AAO-HNSF 2020 Virtual Annual Meeting & OTO Experience, September 14, 2020.
