Abstract

While aspirin-exacerbated respiratory disease (AERD) is a routinely encountered diagnosis in the otolaryngology clinic, no previous cases of concomitant AERD and hereditary hemorrhagic telangiectasia (HHT) have been reported. HHT, or Osler-Weber-Rendu disease, is an autosomal dominant disease presenting with mucosal telangiectasias and arteriovenous malformations (AVMs) occurring in an estimated 1 in 2351 to 39,216. 1 The role of otolaryngology in the management of these patients routinely involves the treatment of recurrent severe epistaxis. Despite no standard first-line treatment, options include conservative measures, coblation or laser ablation of telangiectasias, and intralesional bevacizumab,1,2 among others. AERD, the triad of aspirin sensitivity, asthma, and nasal polyposis, is another common pathology seen in otolaryngology clinics, occurring in approximately 7% of patients with asthma. Traditional management of these patients with nasal polyps includes endoscopic sinus surgery (ESS) followed by aspirin desensitization. 3 However, required daily aspirin therapy and frequent polyp recurrence have led to an appealing medical alternative: dupilumab. While dupilumab has not been specifically studied for AERD, it has been shown to be effective in subgroups of patients with AERD and chronic sinusitis with nasal polyps (CRSwNP). 4 The Institutional Review Board of the University of Arkansas for Medical Sciences approved this study (261035).
Case Report
A 65-year-old woman was referred for workup and evaluation of epistaxis and chronic rhinosinusitis. The patient reported a 20-year history of sinus infections and received oral antibiotics multiple times per year. She developed worsening nasal congestion and intolerance to continuous positive airway pressure and so was referred to a local otolaryngologist. At that time, she was scheduled to undergo ESS for nasal polyposis. Her preoperative evaluation revealed a pulmonary AVM, and the patient was referred to interventional radiology for further management. The family history elicited was positive for HHT and chronic daily epistaxis in her children. The patient’s medical history included sleep apnea and nebulizer-dependent asthma, multiple gynecologic surgical procedures, and shoulder surgery. The patient uses daily fluticasone and oxymetazoline as needed for nosebleeds. The patient reported having anaphylaxis to naproxen as well. Nasal endoscopy revealed polyps in the middle meatus and 2 large septal telangiectasias ( Figure 1 ). The magnetic resonance imaging of her brain for workup of intracranial AVMs revealed nasal polyps and sinus opacification ( Figure 2 ). Genetic testing confirmed the diagnosis of HHT. In the presence of pulmonary AVMs and AERD, dupilumab therapy was recommended as a more conservative treatment than ESS and aspirin desensitization, which could exacerbate her bleeding.
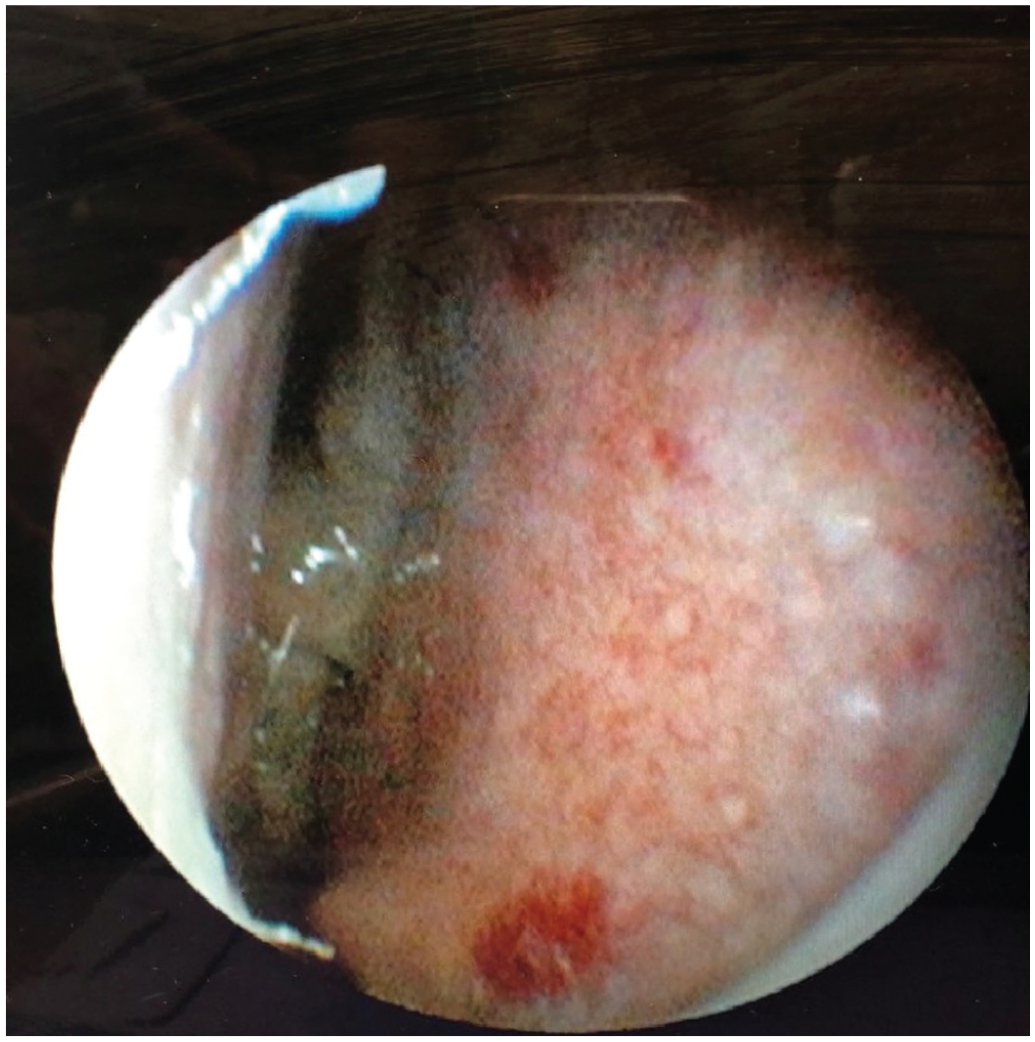
Right nasal endoscopy revealing 2 large telangiectasias and a polyp of the middle meatus.

Magnetic resonance image demonstrates nasal polyposis on T1 and T2 coronal sections.
Discussion
This patient represents the first confirmed case of concomitant AERD and HHT. It is unique presentation constituting an indication for biologic therapy as an alternative to aspirin desensitization.
The treatment paradigm for patients with AERD has been excision of nasal polyps, followed by aspirin desensitization. 3 The impetus for surgery prior to aspirin desensitization is the increased risk of intraoperative/postoperative bleeding after starting high-dose aspirin maintenance therapy. 5 Aspirin desensitization has been demonstrated to reduce hospitalizations, upper respiratory infections, and the use of systemic and inhaled steroids after 1 year of therapy. 3 Need for revision ESS has been shown to be reduced from once every 3 years to once every 10 years in patients with AERD who have undergone aspirin desensitization.3,5 However, cessation of therapy results in resensitization to aspirin that occurs within 5 days, so compliance with daily aspirin is crucial. 3 Recent biologic agents have demonstrated efficacy in nasal polyps in the setting of AERD and thus an appealing alternative to aspirin desensitization. 3
Given our patient’s baseline risk for increased bleeding and concurrent pulmonary AVM, dupilumab was thought to be a prudent therapy. In 2019, the Food and Drug Administration approved dupilumab to treat CRSwNP. 4 Dupilumab binding to the IL4 receptor inhibits binding of IL4 and IL13 to a shared receptor, leading to suppression of type 2 inflammatory responses. 4 No biologic has been approved for AERD specifically, but in a subgroup of a current phase 2a trial, dupilumab significantly improved CRSwNP disease endpoints and clinical improvement in respiratory symptoms. 4
Previous studies that demonstrated epistaxis secondary to HHT can be treated with conservative management for self-limited disease or laser ablation for moderate disease.1,2 The patient reported self-limited epistaxis approximately once per month for the last several years, which was controlled with topical oxymetazoline and pressure. Ablation of the nasal telangiectasias was not considered, given the patient’s mild epistaxis and primary presentation of CRSwNP.
