Abstract
Objective
The main objective of this study was to quantify daily pain and opioid use in patients after hemithyroidectomy and cervical lymph node biopsy (CLNB). The secondary objective was to identify factors associated with decreased pain and opioid use.
Study Design
Prospective cohort study from June 2017 to February 2019. Patients were given paper surveys to record daily postoperative opioid use and maximal pain on a visual analog scale.
Setting
Single institution (NewYork-Presbyterian/Weill Cornell Medical Center).
Methods
All adult patients undergoing hemithyroidectomy and CLNB by a single surgeon were consecutively selected for participation. Patients recorded daily pain and opioid analgesic use over a 2-week postoperative period.
Results
Of 33 patients enrolled, 29 (87.9%) returned a survey. Thirteen underwent CLNB, and 16 underwent hemithyroidectomy. Pain resolved after both procedures by the end of the 2-week period. CLNB patients used a median (interquartile range) of 15.0 (0-41.2) morphine milligram equivalents (MME), and 95% used 70 or fewer MME. Hemithyroidectomy patients used a median of 8.2 (4.5-13.9) MME, and 95% used 30 or fewer MME. Use of nonopioid analgesics was associated with a statistically significant decrease in pain (56.1 vs 171 visual analog scale, 95% confidence interval [CI] of Δ = [12.0 to 217.8]) and opioid use (12.2 vs 48.8 MME, 95% CI of Δ = [5.0 to 68.1 MME]) in CLNB but not in hemithyroidectomy.
Conclusion
Patients have low pain and opioid requirements after hemithyroidectomy and CLNB. Head and neck surgeons should evaluate their opioid-prescribing patterns for opportunities to safely decrease postoperative prescriptions.
Pain management is critical in the postoperative period and has a profound influence on surgical outcomes. This importance has been underscored by nationwide efforts to recognize pain as the “fifth vital sign” and to aggressively treat it as such. 1 Unfortunately, the 2 decades following these initiatives have been marked by a significant rise in rates of opioid abuse and overdose, and opioids are now the leading cause of deaths from drug overdose in the United States.2,3 This has coincided with a rise in sales of opioids, suggesting that increased medical use and prescription of opioids has contributed to the increase in opioid poisoning. 4 Indeed, the number of Americans abusing opioid prescriptions has more than doubled from 1992 to 2012. 5 It is thought that opioid diversion, meaning the transfer of opioids to those other than the intended individual, has become an increasingly significant contributor to the rise in opioid overdoses. 3
Surgeons prescribe a significant amount of opioids, second only to pain medicine specialists, as reported in one study, 6 accounting for a large quantity of opioids that enter public circulation and potentially become available for diversion. Studies demonstrate that up to 71% of opioids prescribed postoperatively are not taken by the patient for whom they were intended. 7 Until recently, there has been a paucity of data regarding the degree of perceived pain and opioid analgesic requirements for patients in the immediate postoperative period to guide prescribing patterns. Knowledge of these parameters could allow surgeons to prescribe a course of analgesics tailored to the analgesic needs of patients undergoing particular procedures, possibly lowering the total quantity of opioids prescribed and thus curbing the potential for opioid diversion.
The primary goal of this study is to characterize the quantity and duration of opioid analgesics necessary for pain management in the immediate postoperative period following hemithyroidectomy and cervical lymph node biopsy (CLNB), 2 common outpatient head and neck procedures. In addition, we sought to characterize the severity and time course of pain following these procedures. A secondary objective of this study is to identify patient-specific features that may be associated with postoperative pain and opioid usage.
Methods
This was a prospective cohort study at a single academic medical institution that used postoperative surveys to evaluate postoperative pain management. Following Weill Cornell Medicine institutional review board approval, patients who planned to undergo hemithyroidectomy and CLNB were prospectively enrolled from June 2017 to February 2019. Patient demographic information including age, sex, education level, marital status, and history of chronic pain and analgesic use was collected preoperatively. Patients then underwent standard outpatient hemithyroidectomy or CLNB by a senior author of this study (D.I.K.). Surgical and anesthetic techniques were not standardized but performed according to the standard practice of the surgeon and anesthesiologists involved. Local anesthesia was performed by local infiltration of lidocaine with epinephrine into the site of incision. Patients did not receive any preoperative pain medication. No topical anesthetic medications were applied. For postoperative analgesia, patients were prescribed either oxycodone 5 mg/acetaminophen 325 mg or codeine 30 mg/acetaminophen 300 mg. Patients were not required to return unused pills at the end of the study period.
After surgery, patients recorded their daily peak postoperative pain and use of opioid and nonopioid analgesics on a postoperative log over 14 days. A study coordinator contacted each patient on postoperative day (POD) 2 to remind him or her to fill in the log on a daily basis rather than all at once at the end of the study period to decrease recall bias. Pain was recorded on a visual analog scale (VAS) and measured in millimeters (range, 0-100 mm). Patients returned the log either by mail or in person at their postoperative follow-up visit. The Centers for Disease Control and Prevention conversion calculator was used to convert opioid analgesic use into morphine milligram equivalents (MME). 8 Postoperative prescription quantities were recorded from the electronic medical record. All data were de-identified and stored in an Excel spreadsheet (Microsoft, Redmond Washington). Descriptive statistics were reported for patient characteristics, postoperative pain levels, and postoperative analgesic usage. Linear regression was performed to analyze the correlation between total reported pain and total opioid usage. Bivariate analysis was performed with primary outcomes of pain level and opioid usage by comparing 95% confidence levels of those outcomes, with statistical significance determined by nonoverlapping intervals. The following variables were tested in the bivariate analysis: gender (male vs female), age (older vs younger split by mean age), marital status (married vs single, divorced, or widowed), education (completed graduate school or college vs completed high school), history of chronic pain, and use of nonopioid analgesics in the postoperative period.
Results
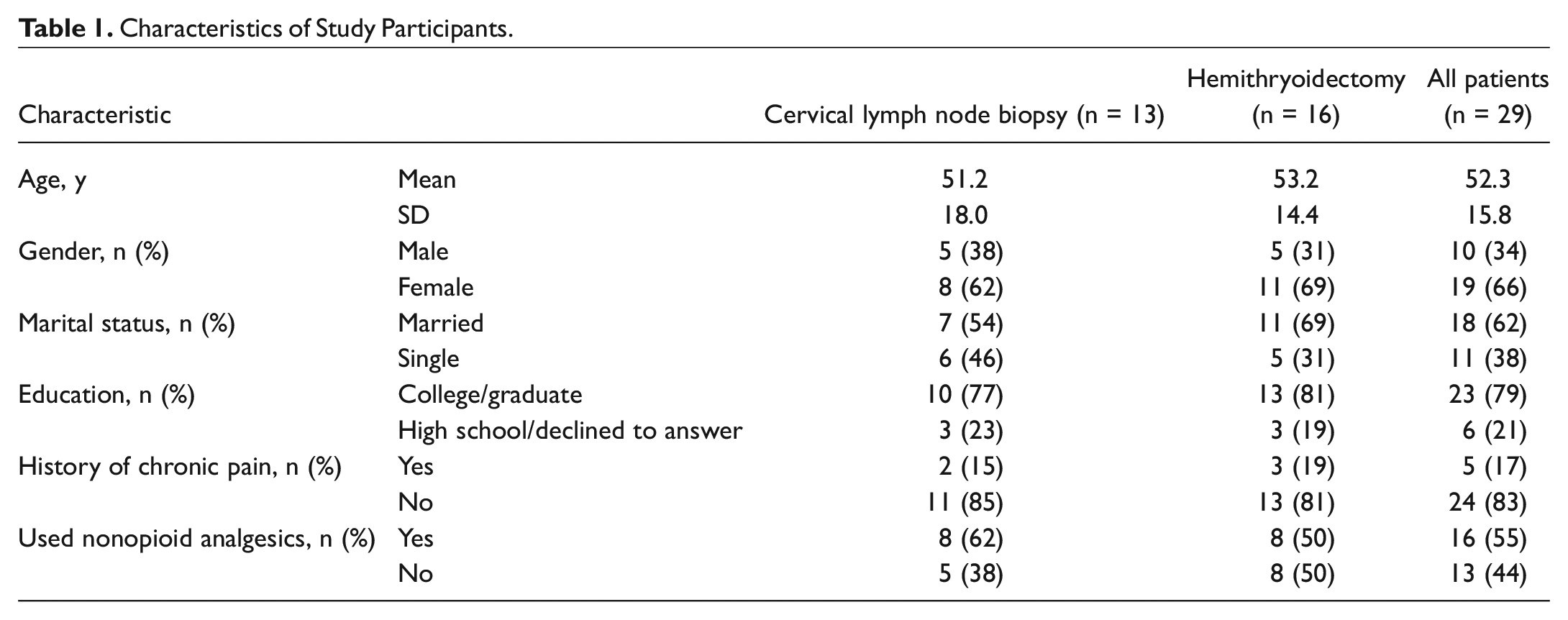
Thirty-three patients were enrolled between June 2017 and December 2019. Twenty-nine (87.9%) completed and returned the survey. Nineteen (65.5%) patients were female. Sixteen (55.2%) patients underwent hemithyroidectomy, whereas 13 (44.8%) underwent CLNB. The characteristics of the patients are summarized in Table 1 . Five (17.2%) patients reported a history of chronic pain. Five (17.2%) patients reported long-term use of analgesic medications; however, no patients reported long-term opioid use.
Characteristics of Study Participants.
The mean prescription for the entire cohort was 124.3 ± 51.8 MME (range, 45-225 MME). The mean prescription for the CLNB group was 110.2 ± 48.0 MME, and the mean prescription for the hemithyroidectomy group was 136.5 ± 53.5 MME. In terms of number of doses, the mean prescription was 19.2 ± 6.8 pills (range, 10-30 pills) for the entire cohort, 15.9 ± 7.3 pills for the CLNB group, and 21.9 ± 5.0 pills for the hemithyroidectomy group.
In the entire cohort, the average opioid consumption was 17.7 ± 22.5 MME (range, 0-97.5 MME), and the median opioid consumption was 9.0 MME (interquartile range [IQR], 4.5-22.5 MME) over the postoperative period. Patients in the CLNB group consumed an average of 26.2 ± 30.4 MME and a median of 15.0 MME (IQR, 0-41.2 MME). Patients in the hemithyroidectomy group consumed an average of 10.7 ± 9.7 MME and a median of 8.2 MME (IQR, 4.5-13.9 MME). In terms of number of doses, the average consumption was 2.8 ± 3.6 pills (range, 0-14 pills) for the entire cohort, 3.6 ± 4.3 pills in the CLNB group, and 2.2 ± 2.9 pills in the hemithyroidectomy group. The median consumption was 2 pills (IQR, 1-3) in the entire cohort, 2 pills (IQR, 0-5.5) in the CLNB group, and 1 pill (IQR, 1-3) in the hemithyroidectomy group. Histograms of total opioid use are shown in
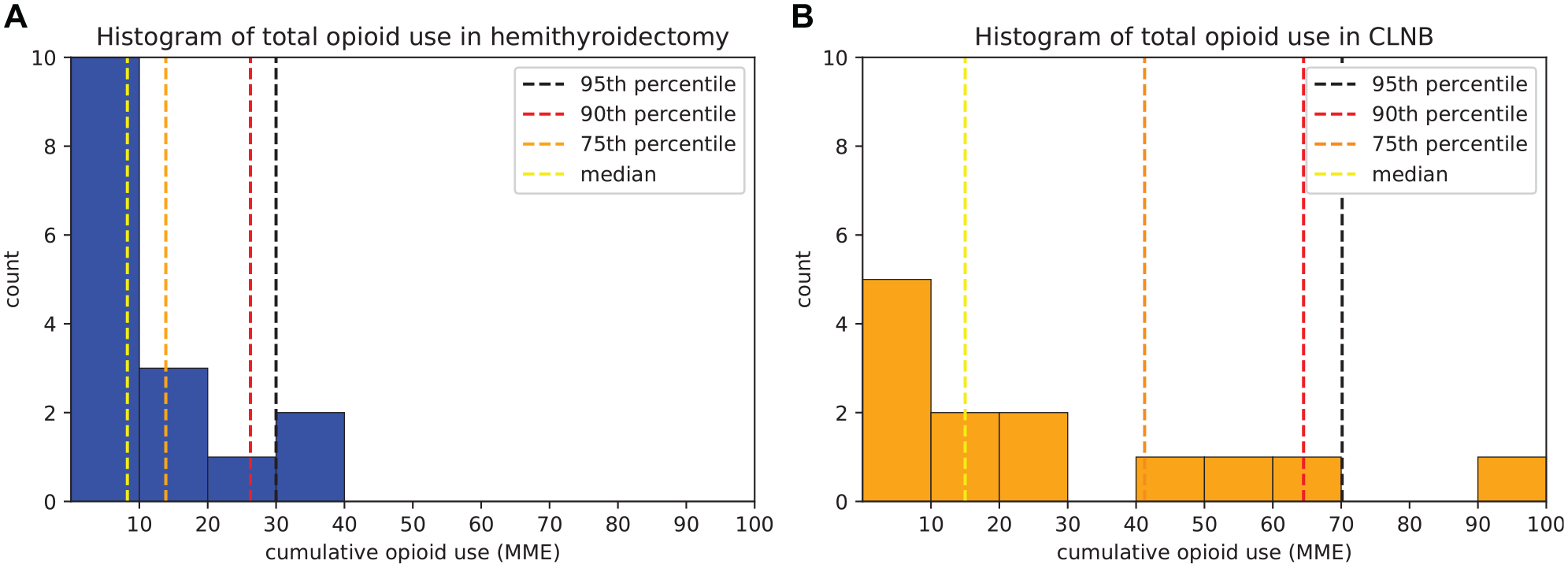
(A) Histogram of total opioid use by patients undergoing hemithyroidectomy. Vertical lines denote percentiles of opioid use. (B) Histogram of total opioid use by patients undergoing cervical lymph node biopsy. Vertical lines denote percentiles of opioid use.
In the CLNB group, peak pain occurred on POD 0 for 8 patients (61.5%) and POD 1 for 5 patients (38.5%). In the hemithyroidectomy group, peak pain occurred on POD 0 for 12 patients (75.0%), POD 1 for 3 patients (18.7%), and POD 2 for 1 patient (6.3%). Mean pain levels and opioid usage over the immediate 14-day postoperative period are represented in
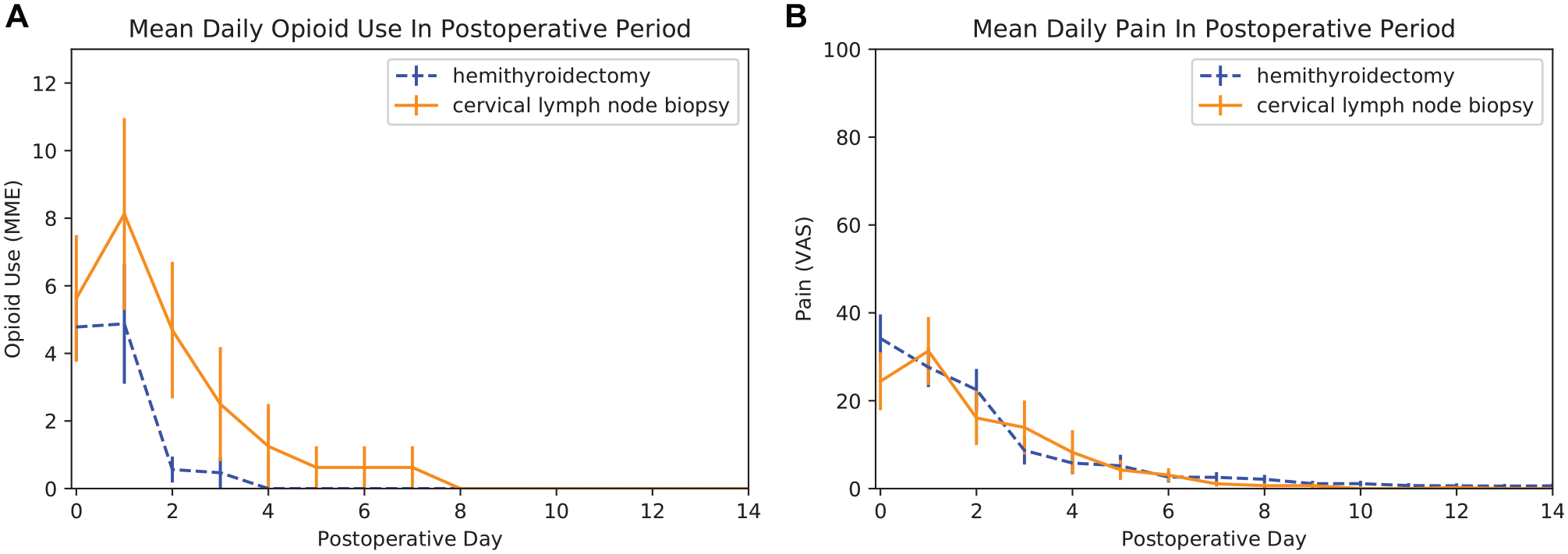
(A) Mean daily opioid use in the postoperative period for patients undergoing hemithyroidectomy and cervical lymph node biopsy. (B) Mean daily maximum pain in the postoperative period for patients undergoing hemithyroidectomy and cervical lymph node biopsy.
There was no statistically significant difference in reported pain between the hemithyroidectomy and CLNB groups on any given POD. Similarly, there was no statistically significant difference in cumulative opioid usage throughout the postoperative course between patients who underwent hemithyroidectomy (95% confidence interval [CI] = [6.0 to 15.4 MME]) and those who underwent CLNB (95% CI = [8.8 to 43.6 MME]). There was also no statistically significant difference between the 2 groups in terms of the number of opioid doses consumed (95% CI of the hemithyroidectomy group = [0.9 to 3.7 pills], 95% CI of the CLNB group = [1.2 to 5.0 pills]). For both the hemithyroidectomy and CLNB groups, age, gender, marital status, education level, and history of chronic pain were not associated with differences in total opioid use or reported pain in the postoperative course.
Eight patients (61.5%) in the CLNB group used nonopioid medications such as ibuprofen or acetaminophen for analgesia during the postoperative course, and 8 patients (50%) in the hemithyroidectomy group used nonopioid medications for analgesia. In the CLNB group, patients who used nonopioid analgesics reported an average pain score of 56.1 on the VAS as compared with 171.0 reported by patients who did not use nonopioid analgesics (Δ = 114.9, 95% CI of Δ = [12.0 to 217.8]). In terms of total opioid use, CLNB patients who also used nonopioid analgesics used an average of 12.2 MME as compared with 48.8 MME used by patients who did not use nonopioid analgesics (Δ = 36.6 MME, 95% CI of Δ = [5.0 to 68.1 MME]). In the hemithyroidectomy group, use of non-opioid analgesics was not associated with statistically significant differences in pain or opioid use.
Discussion
Along with a growing awareness of the opioid epidemic, there has been increasing scrutiny of postoperative pain, opioid-prescribing practices, and opioid use patterns following surgery. This study adds to a growing body of evidence indicating that perceived pain and opioid use following minor head and neck procedures are generally low. In addition, the day-by-day data presented here provide granular information to support postoperative analgesic decision making as well as patient counseling regarding expectations for the postoperative period. In a retrospective study of patients undergoing thyroid and parathyroid surgery, Long et al 9 found that postoperative pain decreases rapidly, with most patients’ pain dropping to 2.6 of 10 by the time of discharge. Results from our study similarly demonstrate that the vast majority of patients report the greatest pain of their postoperative course on POD 0 or 1, with a precipitous drop in reported pain by POD 2. It should be noted that reported pain on POD 0 may be influenced by differences in analgesic administration in the recovery room before discharge, which was not adequately captured in this study. As such, it cannot be determined whether maximal pain occurs on POD 0 or 1, and patients undergoing CLNB and hemithyroidectomy should be counseled to expect maximal pain on either day. All patients in this study reported resolution of pain by the end of the 2-week study period, indicating that hemithyroidectomy and CLNB are unlikely to cause chronic pain. Patients undergoing hemithyroidectomy versus CLNB did not report any significant differences in pain, despite the generally more extensive nature of the hemithyroidectomy procedure compared with a CLNB.
With regard to opioid-prescribing practices by head and neck surgeons, prior studies have found that most surgeons prescribe between 10 and 30 opioid pills after thyroid and parathyroid surgery.10,11 The average prescription in this study was 124 MME, or 19.2 pills. A wide variation in opioid prescriptions was observed by Shindo et al, 12 who found the mean prescription following hemithyroidectomy to be 112 MME with a standard deviation of 102 MME. At our institution, similar variability was observed in prescriptions after both procedures. This variation may be attributed to the fact that at our institution, as in many others, postoperative prescriptions are ordered by resident physicians on the head and neck service.
The literature to date has shown that patients have low opioid requirements following minor head and neck procedures. In a prospective analysis of 313 patients, Lou et al 13 found that patients use a median of 3 MME following thyroid and parathyroid surgery. In the current study, most patients reported using the most opioids on POD 0, and most patients were no longer using any opioid medication by POD 3. Patients who underwent CLNB used more opioids than patients who underwent hemithyroidectomy on a day-by-day basis and in total throughout the postoperative course, but this difference was not statistically significant. The only statistical significance was observed on POD 2, but it should be noted that the difference in opioid usage on that day was only 4.3 MME, roughly equivalent to one 30-mg pill of codeine or half of a 5-mg pill of oxycodone.
With regard to patient characteristics, there were no statistically significant differences in total opioid use when patients were stratified by gender, age, marital status, education level, or self-reported history of chronic pain in either procedure group. Ultimately, most patients used little or no opioid medications in their postoperative course, but a few patients consumed a much greater quantity of opioids. Surprisingly, although total reported pain was strongly correlated with total opioid use in CLNB patients, they were only moderately correlated in patients undergoing hemithyroidectomy, indicating the possibility that additional factors beyond the amount of pain experienced by patients may influence the use of opioid medications. For example, at our institution, CLNB is usually performed for patients with suspicion of recurrent malignancy, and these patients are more likely to have used opioids previously, whereas patients undergoing hemithyroidectomy may be more likely to be opioid naïve. Further investigation into these factors as well as possible predictive patient characteristics is needed to determine the proper opioid prescription that individual patients may require.
This study supports prior observations that postoperative prescriptions for minor head and neck procedures are generally excessive. Tharakan et al 14 noted that after thyroid and parathyroid surgery, patients received a median opioid prescription of 25 pills but consumed only a median of 2 pills. Similarly, in our cohort, opioid prescriptions far exceeded opioid consumption. Patients undergoing CLNB used an average of 26 MME despite receiving a prescription of 110 MME, and patients undergoing hemithyroidectomy used an average of 11 MME despite receiving a prescription of 137 MME. In terms of opioid doses, patients undergoing CLNB consumed an average of 3.6 of 15.9 pills prescribed to them, and patients undergoing hemithyroidectomy consumed an average of 2.2 of 21.9 pills prescribed to them. With conservative estimates of 150,000 thyroidectomies performed in the United States each year, 15 this represents a vast quantity of unused opioids that become available for diversion. Decreasing the typical postoperative opioid prescription for these procedures would remove millions of opioid pills annually from general circulation. These results suggest that head and neck surgeons should assess their current prescribing patterns and consider decreasing the initial opioid prescription after minor head and neck procedures. In our cohort, the 95th percentile of opioid consumption following hemithyroidectomy was 30 MME. This is consistent with a prior report by Lou et al 13 that found that 93% of patients undergoing thyroid procedures use 20 MME or less. Following CLNB in this cohort, the 95th percentile of opioid consumption was 70 MME. In terms of doses, the 95th percentile of opioid consumption was 6 pills in hemithyroidectomy patients and 11 pills in CLNB patients. Further studies with larger patient cohorts will allow for further refinement of the ideal prescription quantity. In all cases, patients should be educated on the proper procedures for disposing opioid medications, as most patients will not consume their entire prescription.
Prior studies have found that postoperative opioid consumption is decreased when nonopioid analgesics are administered concurrently.16-18 Other studies found that the use of nonnarcotic analgesics such as acetaminophen and gabapentin allow a significant proportion of patients to forego opioids altogether. 19 Consistent with prior studies, the use of acetaminophen or ibuprofen was associated with significantly less pain and opioid use following CLNB in this study. A similar association was not observed in patients undergoing hemithyroidectomy, however. As with all observational studies, causal relationships between nonopioid analgesics and pain and opioid use cannot be determined from the current study. Nonetheless, these findings indicate that surgeons should encourage patients to use nonopioid medications for postoperative pain to decrease or even eliminate opioid use.
This study has several limitations. To reflect best routine practice, surgical, anesthetic, and analgesic management were not standardized but were left to the discretion of the physicians involved. All data on pain and opioid usage were self-reported by patients, allowing for the possibility of both selection and reporting biases. The cohort size in this study was limited, so statistically significant associations between certain factors and the outcomes of pain and opioid use may not have been detected. Finally, this study was performed at a single, urban institution, which may limit the generalizability of the data, as it is known that there are disparities in rates and quantities of therapeutic opioid use among regions with different socioeconomic characteristics. 20
Conclusion
After hemithyroidectomy and CLNB, pain experienced by patients peaked by the first POD and quickly decreased to baseline. Patient factors such as marital status, education level, and history of chronic pain were not found to be associated with differences in postoperative pain or opioid usage. Patients undergoing these procedures generally had a low opioid requirement, with 95% of patients undergoing CLNB using 70 MME (11 pills) or fewer, and 95% of patients undergoing hemithyroidectomy using 30 MME (6 pills) or fewer. All patients in this study received prescriptions far in excess of what they actually used. Encouraging patients to use non-opioid analgesics for postoperative pain control has the potential to decrease opioid requirements. Likewise, reevaluating current opioid-prescribing patterns in common head and neck procedures represents an opportunity for otolaryngologists to counteract opioid overprescription and diversion.
Footnotes
This article was presented at the 2019 Annual American Head & Neck Society Meeting held at the Combined Otolaryngology Spring Meetings; May 1, 2019; Austin, Texas.
