Abstract
Takotsubo cardiomyopathy (TTC) is a rare, distinct type of acquired cardiomyopathy. It is characterized by profound left ventricular contraction abnormalities that lead to acute cardiac failure in the absence of obstructive coronary disease. It has also gone by the names stress-induced cardiomyopathy and broken heart syndrome because of its association with triggers of physical or emotional stress. Surgery is known as one potential inciting factor for TTC; however, there are no reports of TTC following surgery in the otolaryngology literature. We report 1 case of TTC following major head and neck surgery that demonstrates the diagnostic criteria and highlights the possibility of this complication following head and neck surgery.
Case Report
Institutional review board exemption was obtained from Oregon Health & Science University. Retrospective chart review was performed. A 64-year-old white woman with supraglottic squamous cell carcinoma (T4aN1M0) underwent total laryngectomy with bilateral selective neck dissection. She had no previous cardiac history, and preoperative electrocardiogram (ECG) was unremarkable. She did well initially but developed chest pain and dyspnea on postoperative day (POD) 6.
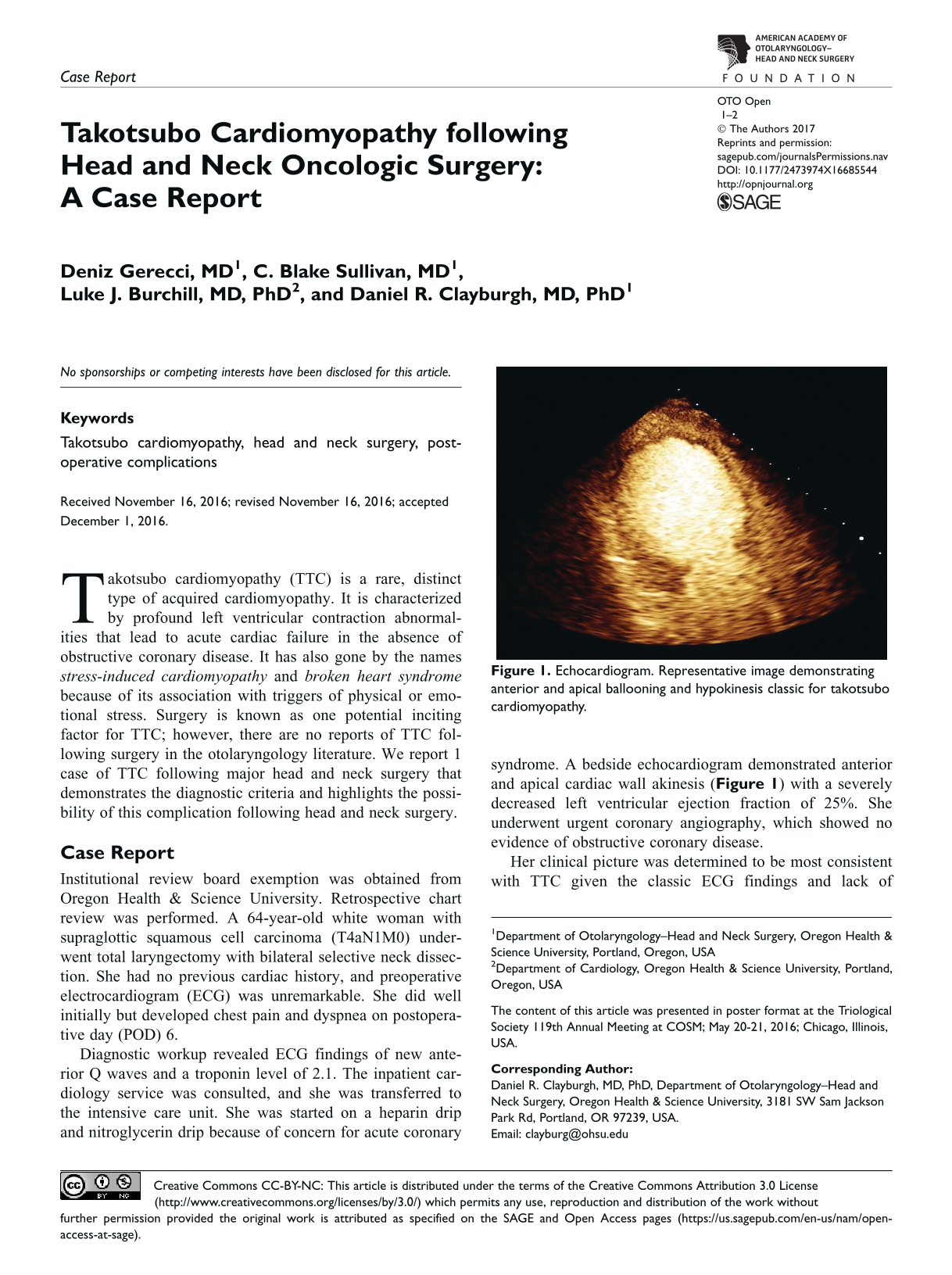
Diagnostic workup revealed ECG findings of new anterior Q waves and a troponin level of 2.1. The inpatient cardiology service was consulted, and she was transferred to the intensive care unit. She was started on a heparin drip and nitroglycerin drip because of concern for acute coronary syndrome. A bedside echocardiogram demonstrated anterior and apical cardiac wall akinesis ( Figure 1 ) with a severely decreased left ventricular ejection fraction of 25%. She underwent urgent coronary angiography, which showed no evidence of obstructive coronary disease.
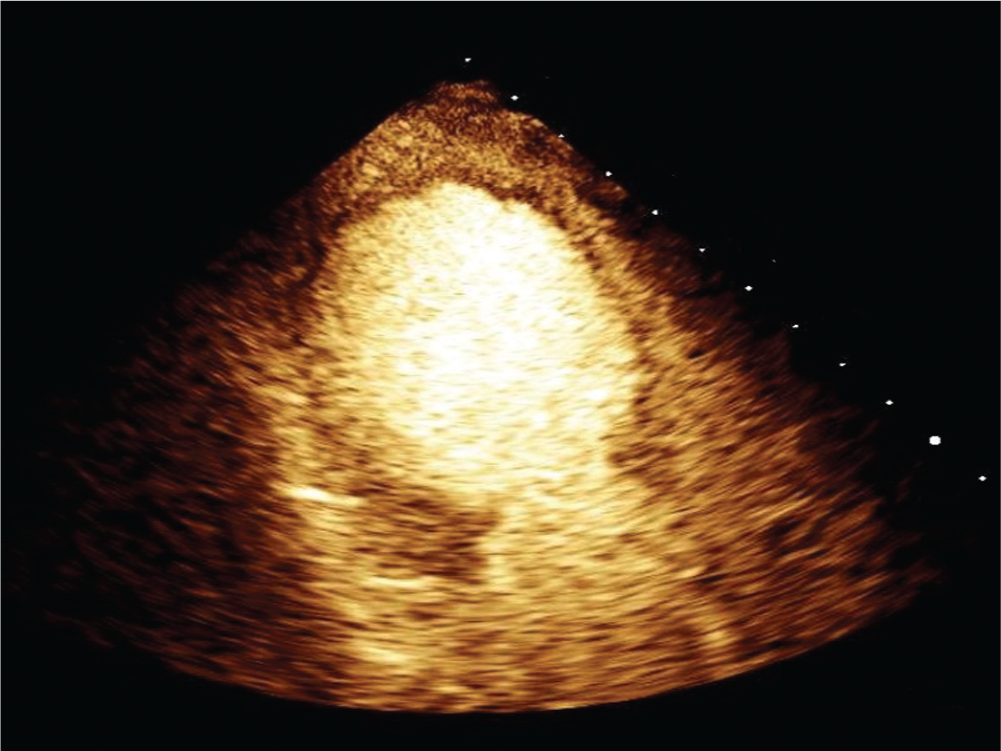
Echocardiogram. Representative image demonstrating anterior and apical ballooning and hypokinesis classic for takotsubo cardiomyopathy.
Her clinical picture was determined to be most consistent with TTC given the classic ECG findings and lack of obstructive coronary artery disease. She was treated supportively with medical therapy including aspirin, atorvastatin, metoprolol, and lisinopril. Over the next several days, she had resolution of symptoms with normalization of laboratory and imaging abnormalities. She was discharged home on POD 12 on the above medications. At 1-year follow-up, she was doing well with no evidence of adverse cardiac sequelae.
Discussion
TTC was first described in the Japanese literature in 1991. 1 The name was chosen given the resemblance of the left ventricular apical ballooning seen on echocardiogram to the “takotsubo,” a Japanese octopus trapping pot with a narrow neck and round bottom. The diagnosis was formally recognized by the American Heart Association in 2006. TTC accounts for 1% to 2% of all admissions for acute coronary syndrome in the United States. 1 Approximately 90% of patients are women, and the mean age at diagnosis ranges from 61 to 76 years. Previously reported stressors include emotional triggers (anger, financial or employment problems, grief, interpersonal conflict, etc) and physical triggers (acute respiratory failure, malignancy, infection, surgery, etc). The mechanism of action is not clearly understood but is thought to be due to catecholamine-induced acute myocardial stunning. 2
Chest pain and dyspnea are the most common presenting symptoms. TTC is a diagnosis of exclusion and is most commonly made according to the Mayo Clinic Criteria 3 ( Table 1 ). No specific treatment guidelines exist, but supportive care with medical therapy is the standard. Sequelae of TTC include life-threatening arrhythmias (seen in 2% of patients), cardiac arrest (4%), and embolic events 3 (5%). Despite the severity of acute heart failure and left ventricular systolic dysfunction, in-hospital mortality for TTC is low. It is estimated that >95% of patients have complete recovery of cardiac function. 3 Approximately 5% to 10% of patients with TTC have recurrence of the condition. 3
Mayo Clinic Criteria for Takotsubo Cardiomyopathy.

All 4 criteria must be met.
TTC has not previously been described following head and neck oncologic surgery. In the otolaryngology literature, there is 1 report of a patient with benign paroxysmal positional vertigo who developed TTC following a canalith repositioning maneuver. 4 In the oral and maxillofacial surgery literature, there is 1 report of a patient who developed TTC following arch bar removal under general anesthesia. 5 The case reported in this study exemplifies the profound clinical sequelae that can be seen with TTC and is the first description of this complication following head and neck surgery. Although the entity is rare, it is important for otolaryngologists to recognize this condition, as it can cause significant morbidity and can occur following head and neck surgery in patients without underlying cardiac disease.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
The content of this article was presented in poster format at the Triological Society 119th Annual Meeting at COSM; May 20-21, 2016; Chicago, Illinois, USA.
