Abstract
Objective
To compare diagnostic capability and patient pain between 25-gauge (25G) and 27G needles for ultrasound-guided fine-needle biopsy of thyroid nodules.
Study Design
Prospective blinded randomized trial.
Setting
Thyroid clinic in otolaryngology practice in a community.
Methods
A prospective randomized blinded trial was conducted on 148 thyroid nodules in 107 patients undergoing ultrasound-guided fine-needle biopsy. Needle gauge was randomized to individual nodule. Patients were blinded to the needle size used. All specimens were assessed via the Bethesda System for Reporting Thyroid Cytopathology and assigned a morphologic quantitative score based on number of thyroid cells and lymphocytes, amount of colloid, and degree of blood/fibrin artifact in each sample. Patient pain experience was scored. A chi-square test was used to compare nondiagnostic rates, and differences in cytologic morphology and pain scores were compared with 2-sample Student t tests.
Results
Of the 148 nodules, 77 were biopsied with 25G needles and 71 with 27G needles. Twenty-five percent (19/77) of the samples obtained with 25G needles yielded a nondiagnostic cytology result (Bethesda category 1) as compared with 11% (8/70) in the 27G group (P = .0282; 95% CI, 1.47%-25.97%). On average, samples from 25G needles had a higher blood/fibrin quantitative score (P = .043; 95% CI, −0.64 to −0.010). There were no differences in pain between groups.
Conclusion
Use of a 27G needle for fine-needle biopsies is not only safe and feasible but desirable and highly recommended, as it yields better diagnostic information.
Keywords
Thyroid nodules are a common finding, with an estimated prevalence >50% after the fifth decade of life in the general population. 1 Despite their ubiquity, workup of these nodules is indicated, as up to 10% may harbor malignancy. 2 The advent of ultrasound-guided fine-needle biopsy (USGFNB) in the 1990s has shaped contemporary management of these nodules. Published guidelines for stratifying risk of malignancy based on ultrasound features and cytopathologic reporting of fine-needle biopsies (FNBs) based on the Bethesda System for Reporting Thyroid Cytopathology have standardized many aspects of the workup and diagnosis of thyroid nodules. 3 USGFNB is a safe, effective, and accurate procedure. Nonetheless, even with ultrasound guidance, the rate of nondiagnostic (ND) cytopathology is estimated at 10%, with some studies reporting much higher rates.3-5 According to American Thyroid Association guidelines, a repeat FNB is recommended for current ND result. Many FNBs are ND due to the nature of the thyroid nodule, such as fibrotic nodules or predominantly cystic nodules, yielding hypocellular samples with an abundance of colloid or cystic fluid only. However, poor technique or wrong needle caliber may also yield an ND result due to obscuring blood and clotting artifact. 6 Thus, optimal needle caliber with good technique should minimize the number of ND results, providing an earlier diagnosis and minimizing patients’ unnecessary pain and anxiety while reducing the health care cost. Proper technique and appropriate needle gauge are essential in getting adequate diagnostic samples and minimizing patient discomfort and complications. We wanted to test the ability of a 27-gauge (27G) needle to yield an adequate specimen by comparing it with a 25G needle. We hypothesized that use of a 27G needle would cause less artifact in the cytology specimen and thus a lower ND rate. In addition, a finer needle would reduce patient discomfort.
Methods
A prospective randomized blinded trial was conducted on 148 thyroid nodules in 107 patients undergoing USGFNB. Protocol was approved by the Institutional Review Board at the Signature Healthcare, Brockton Hospital. Patients were informed of the research protocol, and written consent was obtained. The study cohort consisted of patients referred to a dedicated thyroid clinic for USDFNB between July 2017 and December 2017. Unselected patients with varied referral sources, including endocrinologists, primary care and family physicians, and thyroid surgeons, formed the entire cohort. No a priori sample calculation was performed. Block randomization was used to divide patients between the study cohorts.
All biopsies were performed in an office-based community setting by a single otolaryngologist (J.K.D.). Local anesthetic (1-3 mL of 1% lidocaine with 1:100,000 epinephrine) was injected with a 27G needle under ultrasound guidance. USGFNB was performed with a 25- or 27G needle attached to a 10-mL syringe gauge via a capillary technique. A total of 5 to 10 oscillations over 5 seconds were performed. Needle gauge was randomized to individual nodule. Patients were blinded to the needle size used. Two passes were made for each nodule, and specimens were placed and transported in CytoLyt solution.
Once at the pathology laboratory, samples were processed via liquid-based techniques into monolayer slides (ThinPrep 5000; Hologic). The residual sample was processed into a cell block (Cellient; Hologic), which was also assessed by the cytopathologists. All specimens underwent cytologic analysis by the same 2 cytopathologists (L.L.O., C.A.S.), who were blinded to the needle gauge used to procure the specimens.
In addition to the Bethesda system categories, a predetermined scoring system was designed for this study to allow for reproducibility and quantitate (objective) statistical analyses of the descriptive terminology most commonly used in cytopathology reports. This range-based system served to rank-score the differences in cytologic morphology, such as number of thyroid cells and lymphocytes, amount of colloid, and degree of blood/fibrin artifact in each sample ( Table 1 ).
Cytology Morphologic Scoring System. a
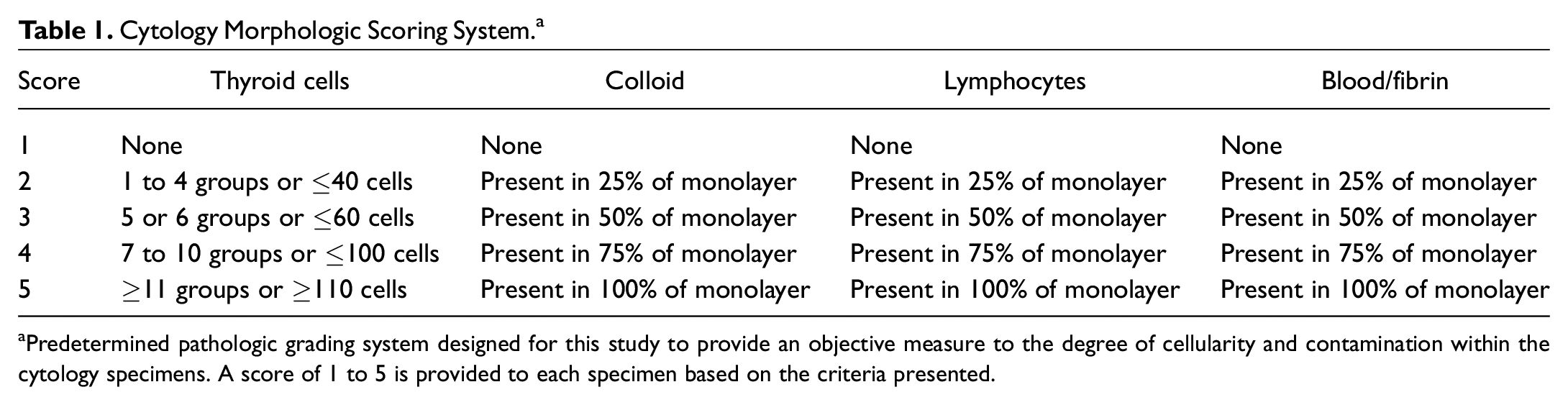
Predetermined pathologic grading system designed for this study to provide an objective measure to the degree of cellularity and contamination within the cytology specimens. A score of 1 to 5 is provided to each specimen based on the criteria presented.
A chi-square test was used to compare ND rates (Bethesda category 1) with 2 needle sizes. Differences in cytologic morphology were compared by 2-sample Student t tests. In addition to diagnostic capability between 25- and 27G needles, we evaluated and compared the pain experienced by patients. Our evaluation included patients undergoing a Short-Form McGill Pain Questionnaire 7 immediately after the procedure. This questionnaire includes a numeric descriptor and visual analog scale to formulate a final score out of 50.
Results
Between July and December 2017, 148 nodules underwent USGFNB as randomized to a 25- or 27G needle group per the aforementioned technique. There were 77 nodules biopsied with 25G needles and 71 with 27G needles ( Figure 1 ). There were 32 men and 76 women, with an age range from 23 to 93 years. The majority of the patients (n = 75) had a single nodule. The maximum number of nodules biopsied in a single patient was 4.
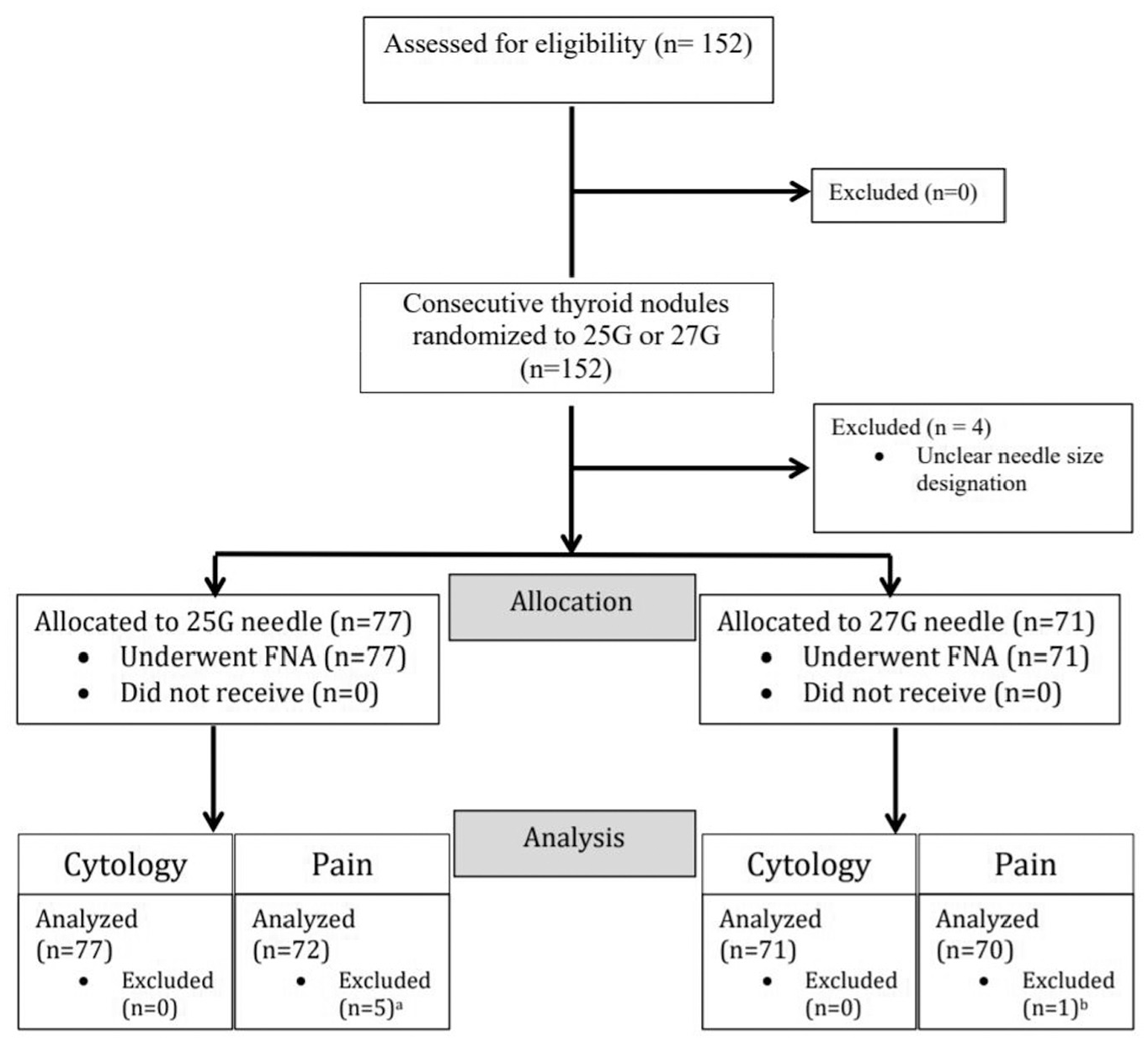
Flow diagram laying out exclusions within the study per the CONSORT guidelines. (a) Five patients were excluded for incomplete pain data. (b) One patient was excluded for incomplete pain data. FNA, fine-needle aspiration.
Cytology
The Bethesda categories of the cytology findings are listed in Table 2 . Twenty-five percent (19/77) of the samples obtained with a 25G needle yielded an ND cytology result as compared with 11% (8/71) in the 27G needle group. This difference was statistically significant (P = .0282; 95% CI, 1.47%- 25.97%). Results from the Cytology Morphologic Scoring System are presented in Table 3 . Samples obtained with a 25G needle had a higher blood/fibrin quantitative score, which was statistically significant (P = .043; 95% CI, −0.64 to −0.010).
Bethesda Category and Needle Gauge.
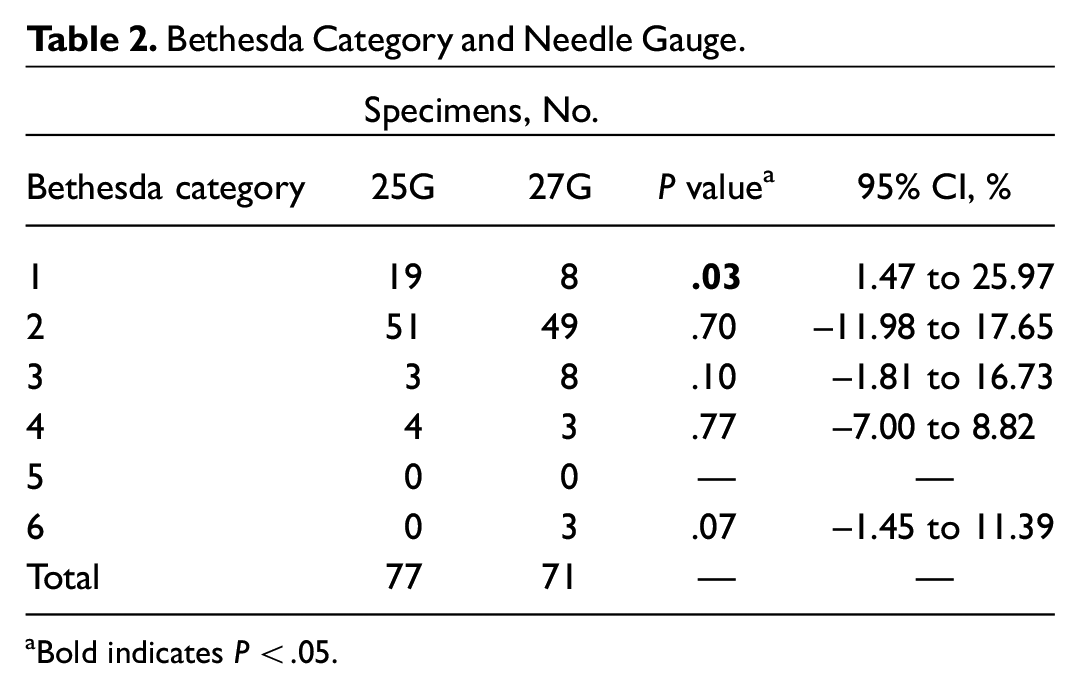
Bold indicates P < .05.
Cytology Morphologic Score and Needle Gauge.
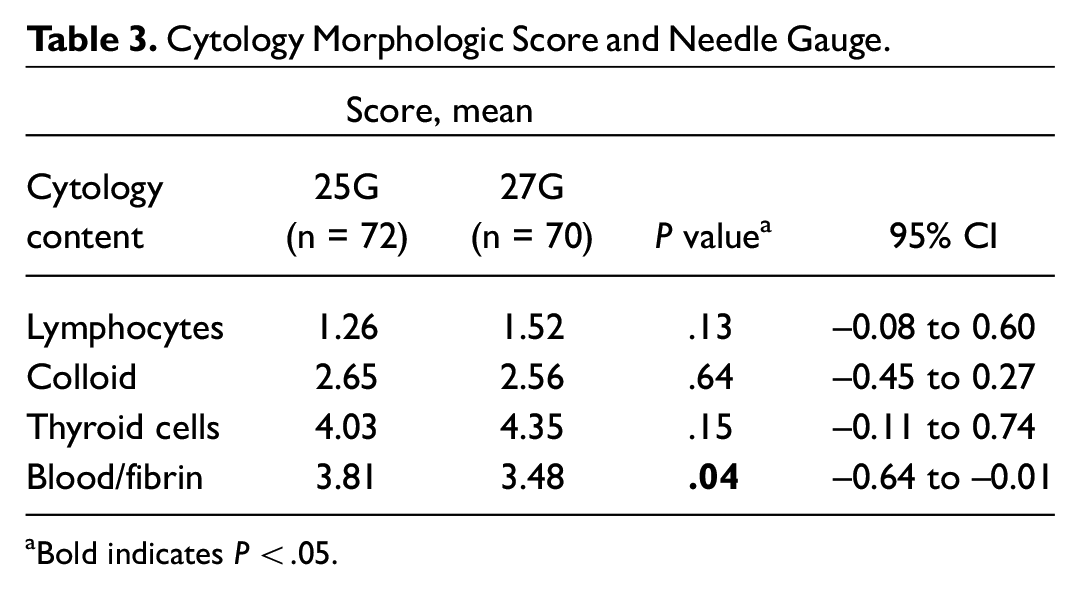
Bold indicates P < .05.
Pain
Pain scores were compared for the 2 needle sizes with the Short-Form McGill Pain Questionnaire as well as the average visual analog scale score. Findings are summarized in Table 4 . There was no statistical difference in the pain scores between the needle groups.
SF-MPQ Scores and Needle Gauge.
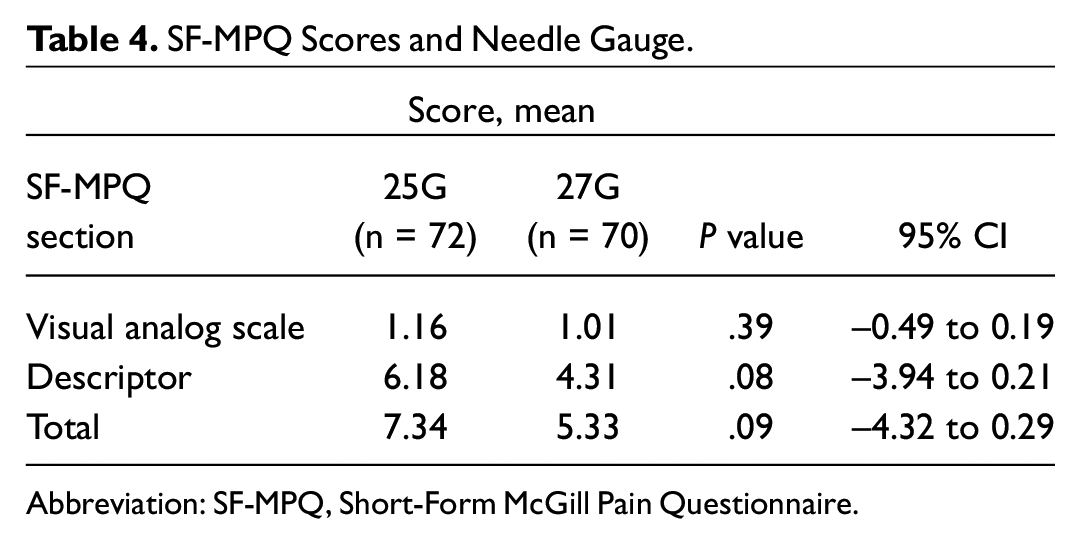
Abbreviation: SF-MPQ, Short-Form McGill Pain Questionnaire.
Discussion
The purpose of this study was to investigate whether the needle size of 27G has the ability to yield an adequate diagnostic sample as compared with the 25G needle, which we have traditionally used in performing our biopsies. Our hypothesis was that the smaller-caliber needle will reduce patient discomfort and yield less cytologic artifact and a lower ND rate. Previous studies in the literature have focused on higher-caliber needles.
In our study, the rate of ND samples for the 25G needles is 14% higher than that of 27G needles, which is statistically significant. We further interpret that this difference is due to the quality of the cytologic preparations. Samples obtained with a 25G needle had a higher blood/fibrin quantity (score), which was statistically significant at a 95% confidence level (P = .04). Tanaka et al also showed increased levels of contamination in the samples obtained with a larger-gauge needle. That study compared 22G and 25G needles, which is consistent with practices in Japan. 8 Several studies9,10 of thyroid fine-needle aspiration technique also found that smaller-diameter needles resulted in increased diagnostic quality, in part as a function of minimizing intragenic hemorrhage and blood contamination within the specimen. Although liquid-based cytology utilizes media preparation solutions and techniques that lyse blood, occlusion of the needle hub via blood clots and blood cells resulting in poor diagnostic quality and less adequate thyroid material is more as a function of the fine-needle aspiration technique and needle used. Also of note, the liquid preparation reduces the presence of fresh blood but can be oversaturated and is not able to completely clean or eliminate clots/fibrin. 11
In a meta-analysis of studies examining needle gauge and technique, Moss et al concluded that there was a nonsignificant trend toward a reduction in the relative risk of ND cytopathology when smaller needles were used. 12 Our study found a clear statistically significant difference, with the 27G needle yielding much fewer ND results.
In addition to diagnostic yield, we compared pain experienced by the patients, who were blinded to the needle size used. To our knowledge, ours is the only study to use a verified pain questionnaire. In our study, there was no significant difference in descriptor scores, visual analog scores, or total scores of the Short-Form McGill Pain Questionnaire between the needle sizes. These results are consistent with reports in the literature.13-15 We believe that no difference in the pain experience between the categories is due to the use of local anesthesia for all our FNBs.
Strength and Weakness of the Study
This study provides a prospective blinded trial that contributes additional evidence to the literature that smaller-gauge needles yield a high degree of diagnostic accuracy by minimizing smear artifact. Limitations to this study include being a single-center study with a small number of participants and minimal variance in the population. Another limitation is the external validity of the cytologic scoring system used in this study. To date, no other study or literature series has provided a validated scoring system of quality descriptors for thyroid fine-needle aspirations; in fact, studies typically identify a cytologic parameter, such as blood or artifact, and then assign a score to the finding. The score is necessary for the application of nonparametric statistical comparison methods. Our system is similar in concept but outright defines the value of each score via either cell count ranges or percentage of the liquid-based slide monolayer. The cellularity value was based loosely on the cellular adequacy guidelines from the Bethesda system. Like many previous studies, to reduce or eliminate assessment bias, the number of cytopathologists assigning the scores was kept at a minimal (2 cytopathologists), and they were blinded.
Conclusion
We conclude that the use of a 27G needle for FNBs is not only feasible but desirable and highly recommended, as it yields better diagnostic information. Since the completion of this study, we have changed our practice and perform all thyroid nodule FNBs using a 27G needle.
Author Contributions
Disclosures
Footnotes
This article was presented as a poster at the AAO-HNSF 2018 Annual Meeting & OTO Experience; October 7-10, 2018; Atlanta, Georgia.
