Abstract

Keywords
Dieulafoy’s lesions (DLs) were first described by the French surgeon Georges Dieulafoy in 1898 in his report of 3 cases of upper gastrointestinal (GI) bleeding in the proximal stomach, resulting in fatal gastric hemorrhage in otherwise asymptomatic young men. 1 While most cases present in the stomach or along the GI tract, there are reports of the lesion in extra-gastrointestinal locations such as the bronchus and head and neck. 2 In the head and neck, the pathology is conserved but is referred to as either cirsoid aneurysm (on the scalp) or submucosal arterial malformation. 3 DLs are a source of profound bleeding, and to our knowledge, this is the first report of a DL as a source of recurrent epistaxis.
Case Report
This report was exempt from review by the University of Massachusetts Institutional Review Board.
Presentation
A 55-year-old man with no significant medical history presented to a tertiary care otolaryngology clinic for evaluation of recurrent unilateral epistaxis. A vascular 1-cm submucosal lesion was identified on nasal endoscopy and was suspected to be the source of the epistaxis, often triggered by coughing and sneezing. The lesion was excised under endoscopic guidance in the operating room and the recurrent epistaxis resolved. A gross specimen and a hematoxylin and eosin–stained specimen were examined. Histopathology confirmed the mass to be a DL.
Endoscopy
Endoscopically, a DL typically appears as an isolated protruding vessel surrounded by normal mucosa, without an associated ulcer. 1 In this case, endoscopy revealed a friable raised lesion with surrounding hyperemic mucosa on the right nasal floor ( Figure 1 ). The lesion was located beneath the inferior turbinate and required infracture and superior displacement of the turbinate to allow room for excision.
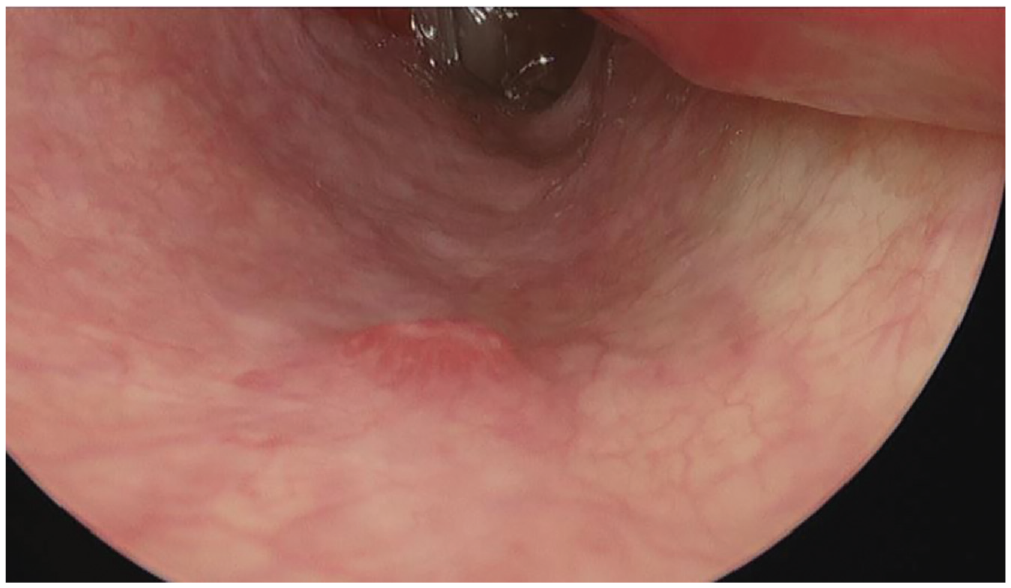
Endoscopic image of the Dieulafoy’s lesion on the nasal floor.
Gross Pathology
A DL is a histologically normal vessel with an abnormally large diameter (1-3 mm) that completes an indirect course within the submucosa and protrudes through a mucosal defect (2-5 mm) without surrounding ulceration. 1
Histopathology
Histology shows a large tortuous vessel underneath an area of thinned sinonasal mucosa with seromucinous glands ( Figure 2 ).
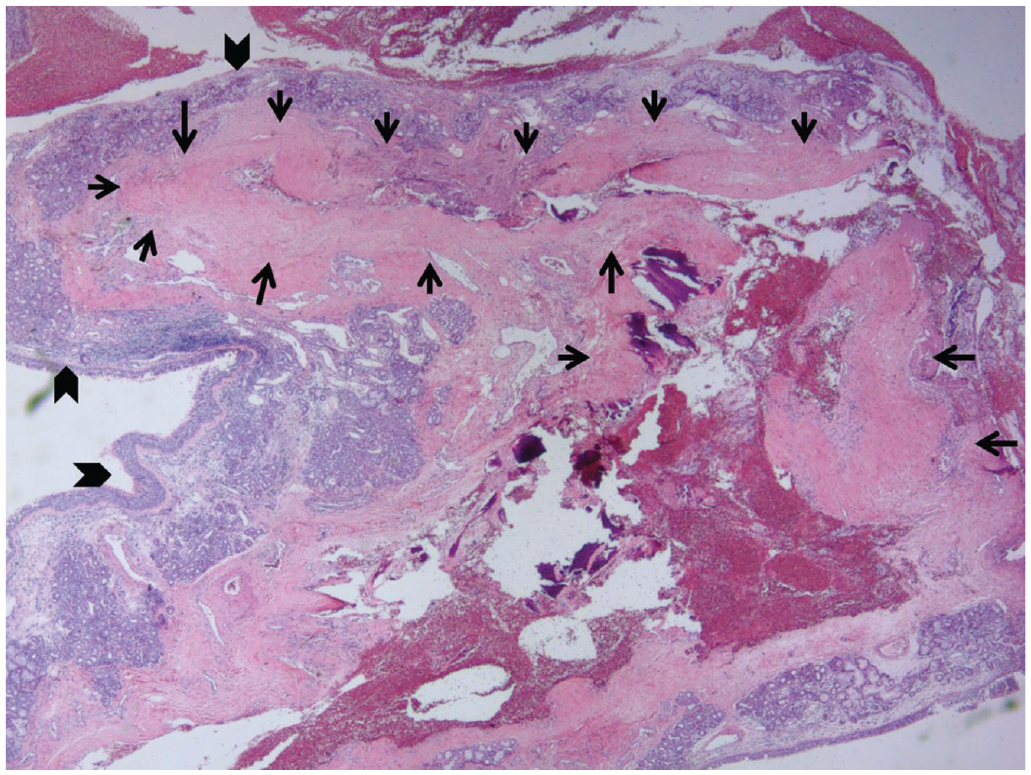
Hematoxylin and eosin staining of surgical specimen at 20× magnification showing large tortuous vessels (arrows) underneath sinonasal mucosa (arrowheads).
Pathophysiology
While the pathogenesis is not well understood, the prevailing theory is as follows: pulsations in a large, tortuous, submucosal arteriole can lead to the disruption of overlying epithelium (which may be intrinsically vulnerable). Epithelial disruption results in areas of localized ischemia and allows for further superficial mucosal erosion and resulting rupture. 1
Of note, DLs are pathologically distinct from other vascular lesions; they do not contain arterial and venous intercommunications that characterize arteriovenous malformations, and unlike hemangiomas, DLs consist of a single circuitous large-caliber vessel rather than a collection of numerous small vessels. In addition, they are generally unifocal and noninherited, unlike hereditary hemorrhagic telangiectasias (HHT). 1
Treatment
The management of DL depends on the specific presentation and location of the lesion. In the GI tract, endoscopic combination therapies (epinephrine with either fulguration or mechanical monotherapies) are preferred initially, followed by angiography with embolization. Failure of either of the former approaches necessitates surgical excision. 4
In this case, the lesion was excised endoscopically in the operating room, and on follow-up, the patient showed no signs of recurrent epistaxis. Fulguration in the nasal cavity would have been a possible initial treatment, but excision allowed for pathologic examination to confirm the diagnosis. Electrocautery was still required to achieve postsurgical hemostasis.
Discussion
DL is a rare vascular lesion that has been identified primarily in the stomach and GI tract and is recognized as a source of GI hemorrhage. Given our experience here, DL is a clinical entity that should also be considered in the differential diagnosis of recurrent epistaxis for patients with a history negative for trauma, inflammation, underlying hematologic pathology, and structural abnormalities of the nasal mucosa and septum. 5 Therefore, the case presented here demonstrates the necessity of endoscopic evaluation for recurrent and unilateral epistaxis in the clinic. If appropriately recognized, management of DLs can be completed with surgical excision, avoiding additional procedures such as embolization or sphenopalatine artery ligation.
Author Contributions
Disclosures
Footnotes
This article was presented at the AAO-HNSF 2019 Annual Meeting & OTO Experience; September 15-18, 2019; New Orleans, Louisiana.
