Abstract

Epistaxis may be a harbinger of a serious complication among patients who have previously undergone radiotherapy (RT) of the nasopharynx or cranial base. We present 2 cases of life-threatening epistaxis arising from major arterial sources in patients with a history of nasopharyngeal carcinoma (NPC) following definitive RT. Approval was obtained from the Stanford University Institutional Review Board.
Case Report
Case 1
A 64-year-old woman was evaluated for a “mass” in her sphenoid sinus. She had a history of T4N1M0 NPC and completed definitive chemoradiotherapy (CRT) in 2006. To date, she was disease-free. Over the past year, however, she developed intermittent minor epistaxis without nasal obstruction. Follow-up computed tomography reported a mass in her right sphenoid sinus and osteoradionecrosis (ORN); she was referred to our clinic for treatment.
Endoscopic examination demonstrated expected sequelae of previous CRT but no obvious mass or source of bleeding. Review of computed tomography and magnetic resonance imaging showed that instead of being a true mass within the sphenoid sinus, a suspected pseudoaneurysm of the internal carotid artery was present ( Figure 1 ). She was to be urgently admitted to the hospital for definitive treatment with interventional neuroradiology for the pseudoaneurysm; however, before this could occur, the patient developed massive epistaxis. Unfortunately, she died prior to receiving emergent medical intervention.
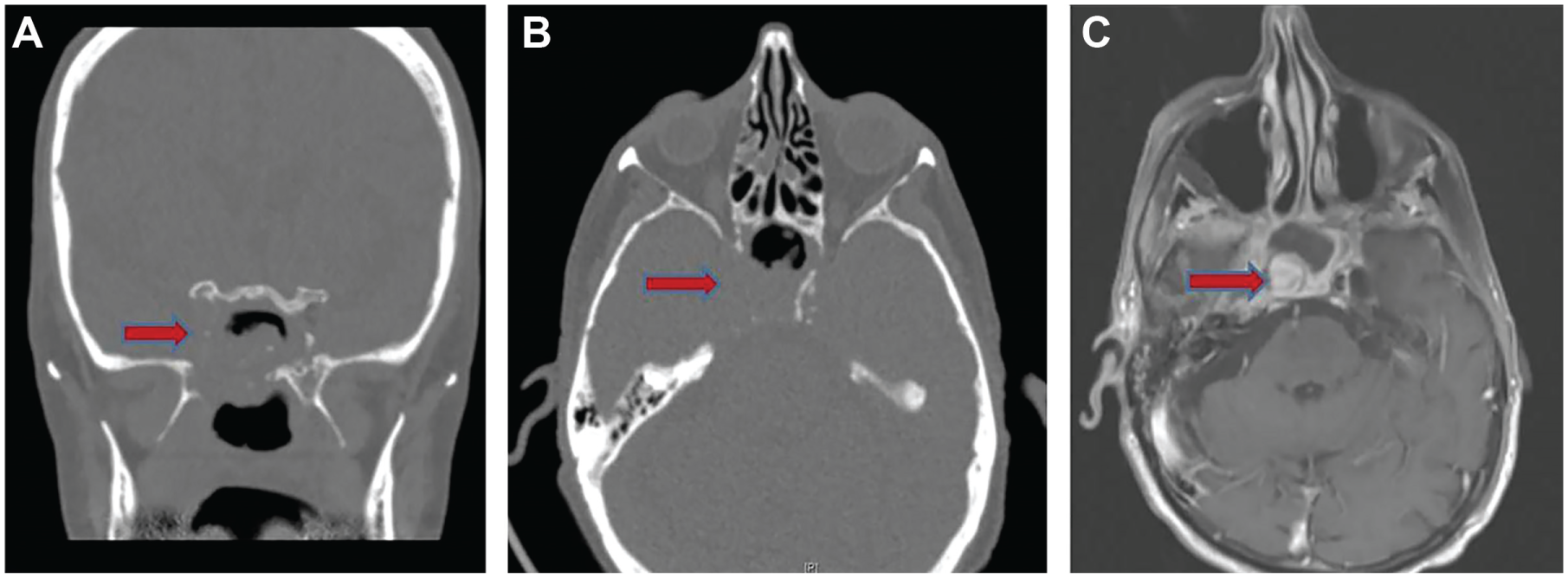
Imaging from patient 1. (A) Coronal and (B) axial computed tomography scans demonstrating bony erosion of the right sphenoid sinus (arrow). (C) Axial T1 postcontrast magnetic resonance imaging demonstrating classic “onion peel” layering of right internal carotid pseudoaneurysm (arrow).
Case 2
A 53-year-old man with history of NPC who completed definitive CRT in 1994 presented for an evaluation for epistaxis. He had known ORN but was otherwise disease-free. His baseline nosebleeds were self-limited, but more recently these had become heavier, necessitating emergency department visits and nasal packing. He reported a history of 2 episodes of heavy epistaxis in 2011 and 2013 requiring nasal packing. Endoscopic examination demonstrated expected sequelae of previous CRT, as well as signs of ORN, without active bleeding.
Due to his history of ORN and increasingly severe epistaxis, he was referred to interventional neuroradiology for angiography and possible embolization. The angiogram demonstrated a pseudoaneurysm arising from the descending palatine branch of the left internal maxillary artery. Embolization was performed with n-butyl cyanoacrylate glue with complete occlusion of the pseudoaneurysm ( Figure 2 ). To date, there have been no further episodes of epistaxis.
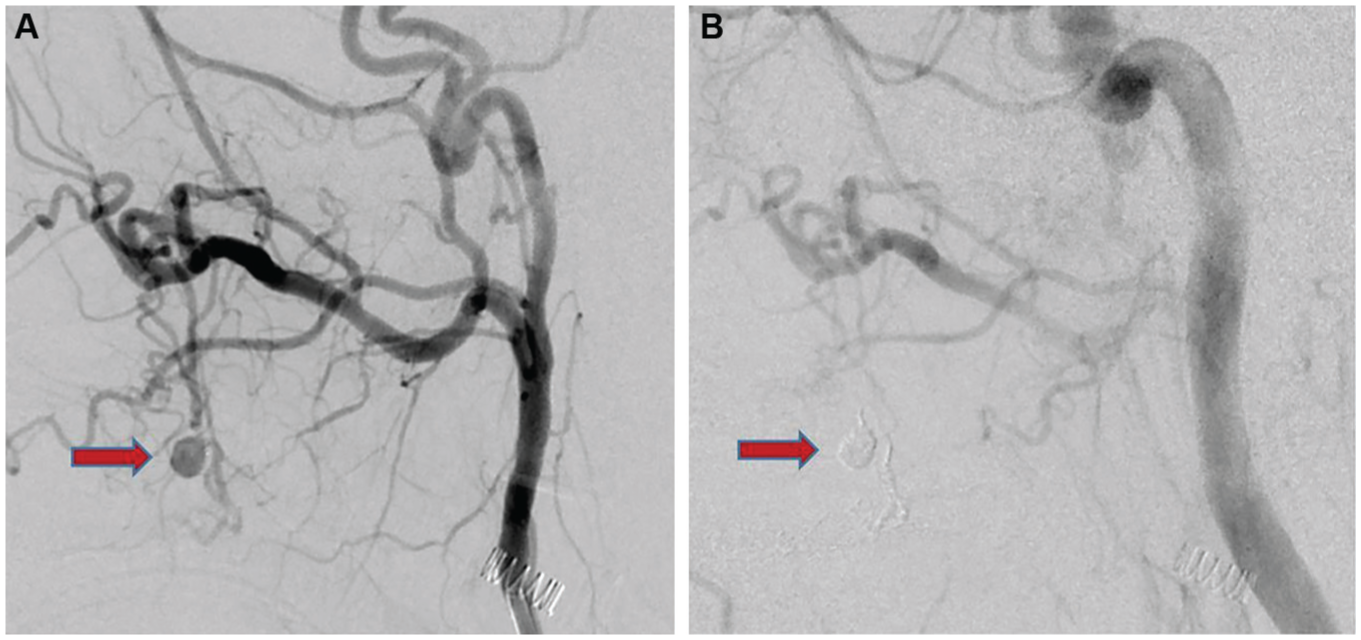
Angiogram of the left external carotid system demonstrating pseudoaneurysm (arrow) of the descending branch of the internal maxillary artery (A) before and (B) after embolization.
Discussion
As opposed to the widespread recognition of carotid pseudoaneurysm and subsequent “blowout” in the neck following RT for metastatic cervical disease, 1 the potential for sinonasal pseudoaneurysm is less well recognized in spite of being described in the literature as a possible complication of RT for NPC.2,3 In certain cases, a sentinel bleeding event may alert the clinician to this possibility (ie, case 2). However, some sentinel bleeding events may be mistaken for the more common mucosal irritation related to CRT causing epistaxis, thus putting the patient at risk for a catastrophic event (ie, case 1).
The etiology of RT-induced pseudoaneurysm is likely a result of weakening arterial walls secondary to RT-induced ischemic injury of the vasa vasorum of the vessel wall and premature atherosclerosis.4,5 Anatomic location may also play a predisposing role, as RT-induced pseudoaneurysms tend to occur more commonly for NPC than other primary tumors of the head and neck region. 5 This could be due to the infiltrating nature of the NPC or the close proximity of the internal carotid artery and cavernous sinus to advanced tumors (ie, T3 and T4 tumors). Moreover, skull base ORN is a strong predisposing factor for pseudoaneurysm, as presented in both cases here. 5
Advanced endovascular techniques have made the treatment of carotid artery or other major arterial pseudoaneurysms more successful and safer for patients, presuming that they are identified before a catastrophic bleeding event occurs.2,3 Maintaining a high suspicion of a potential underlying pseudoaneurysm is the key in this patient population.
Conclusion
Arterial pseudoaneurysm is a rare but potentially lethal complication of RT for NPC. Epistaxis in this patient population can signify a sentinel bleeding event and should be rapidly and thoroughly evaluated.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
