Abstract
Objective
Infection following cochlear implantation is medically and economically devastating. The cost-effectiveness (CE) of colonization screening and decolonization for infection prophylaxis in cochlear implantation has not been examined.
Study Design
An analytic observational study of data collected from purchasing records and the literature.
Methods
Costs of Staphylococcus aureus colonization screening and decolonization were acquired from purchasing records and the literature. Infection rates after cochlear implantation and average total costs for evaluation and treatment were obtained from a review of the literature. A break-even analysis was performed to determine the required absolute risk reduction (ARR) in infection rate to make colonization screening or decolonization CE.
Results
Nasal screening ($144.07) is CE if the initial infection rate (1.7%) had an ARR of 0.60%. Decolonization with 2% intranasal mupirocin ointment ($5.09) was CE (ARR, 0.02%). A combined decolonization technique (2% intranasal mupirocin ointment, chlorhexidine wipes, chlorhexidine shower, and prophylactic vancomycin: $37.57) was CE (ARR, 0.16%). Varying infection rate as high as 15% demonstrated that CE did not change by maintaining an ARR of 0.16%. CE of the most expensive decolonization protocol was enhanced as the cost of infection treatment increased, with an ARR of 0.03% at $125,000.
Conclusions
Prophylactic S aureus decolonization techniques can be CE for preventing infection following cochlear implantation. Decolonization with mupirocin is economically justified if it prevents at least 1 infection out of 5000 implants. S aureus colonization screening needed high reductions in infection rate to be CE.
Prevention of postoperative infection remains a challenge for all surgeons. Orthopedic surgeons are particularly vigilant in establishing effective and cost-conscious infection prophylaxis protocols due to their work with prosthetic implants. 1 Cochlear implantation represents a similar challenge for otolaryngologists. Advancements in preoperative planning and surgical techniques have minimized rates of postoperative cochlear implant (CI) infection. 2 In part, this has contributed to the uncertain evidence for the role of prophylactic antibiotics for CI surgery.3,4
Furthermore, the cost-effectiveness of infection prophylaxis has not represented a chief concern in CI surgery, because many CI infections may be managed without implant removal.5,6 However, evidence suggests that infections directly related to surgical intervention, such as skin flap infection, nearly always result in hardware explantation.7,8
Standard infection prevention protocols are followed before and during CI surgery. One such protocol utilized by health care facilities in general and otolaryngologists in particular includes Staphylococcus aureus colonization screening and decolonization.9-11 While S aureus is not the major pathogen responsible for all types of CI infections, such as otitis media, mastoiditis, or meningitis, 2 S aureus is the most common organism responsible for postoperative CI infections (46%-79%).5,12 Additionally, S aureus is the most prevalent organism found in biofilms on the surface of explanted CIs. 13 However, there is limited knowledge that S aureus decolonization reduces the rate of postoperative CI infection.
Amid the uncertain role of antibiotic prophylaxis in CI surgery, we investigate whether S aureus colonization screening and decolonization are economically justifiable. We hypothesize that colonization screening is not a cost-effective component of infection prophylaxis for CI surgery; however, we posit that the decolonization protocols are independently cost-effective.
Methods
The economic model utilized in this cost analysis was modified from a break-even analysis first described by Hatch et al to determine the cost-effectiveness of vancomycin powder for infection prophylaxis in total shoulder arthroplasty ( Figure 1 ). 1 This equation yields the final infection rate required to make a given protocol cost-effective (ie, break-even) while using variables for the initial infection rate, the total cost of treating an infection, and the cost of a prophylactic protocol. A break-even model was employed rather than other cost-effectiveness models because of its adaptability. We recognize that the values of the variables incorporated into cost-conscious decision making are constantly changing. A CI surgeon or implant center can easily incorporate the values that reflect their practice into each variable in this break-even model to determine cost-effectiveness.

Equation used to calculate the break-even infection rate. Cp , cost of protocol; Ct , total cost of treating an infection; IRf , breakeven infection rate; IRi , initial infection rate; Stotal , total annual surgical procedures. Adapted from Hatch et al. 1
For the current study, these values were determined from our institution’s purchasing records and the literature. As this study was a financial analysis and did not involve protected health information, Institutional Review Board approval was not required. The difference between the initial and final infection rates is reported as the absolute risk reduction (ARR), which is the percentage by which a protocol must reduce the initial infection rate to economically justify its prophylactic application.
Literature values for baseline infection rates of CIs are as high as 8.3%, although we elected to use a more conservative value of 1.7% for the current study.3,5,6 The average cost of revision following infection has been reported to be between $24,000 and $100,000, and for our calculations, we used the lower, more conservative reported cost.14,15 A literature value of $117.00 was used for the cost of S aureus colonization screening. 16 By using the consumer price index for medical care per the Bureau of Labor Statistics, the colonization screening cost was adjusted for inflation to the May 2017 level of $144.07 so that this value could be accurately compared with costs of decolonization protocols obtained from our institution.
Various S aureus decolonization protocols were obtained from the literature.17-21 We reviewed our institution’s purchasing records to determine the cost of each protocol. In addition, we created a new combination protocol to include in our analysis to entirely encompass the range of potential decolonization costs ( Table 1 ).
Cost-effectiveness of S aureus Colonization Screening and Prophylactic S aureus Decolonization Treatment for Cochlear Implantation a
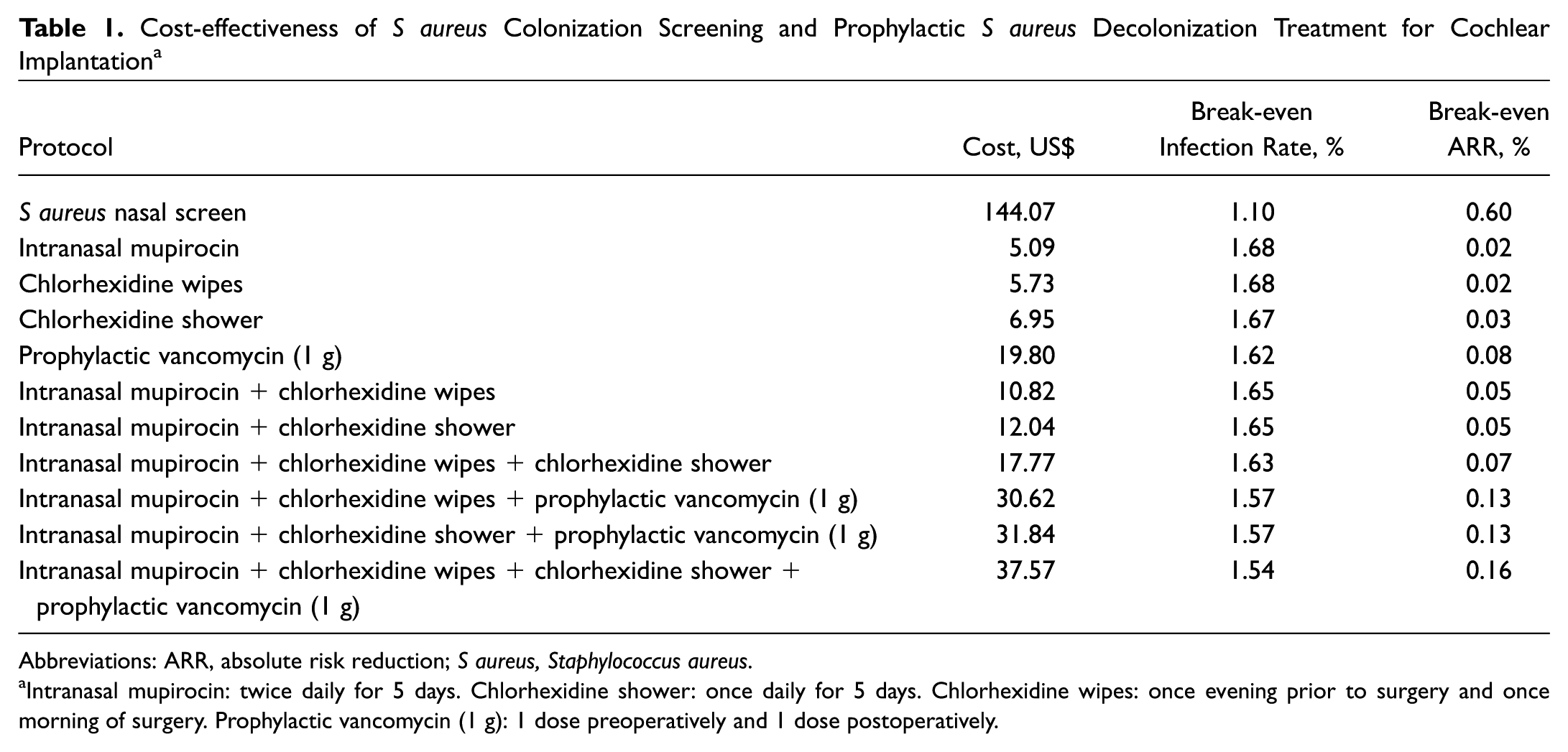
Abbreviations: ARR, absolute risk reduction; S aureus, Staphylococcus aureus.
Intranasal mupirocin: twice daily for 5 days. Chlorhexidine shower: once daily for 5 days. Chlorhexidine wipes: once evening prior to surgery and once morning of surgery. Prophylactic vancomycin (1 g): 1 dose preoperatively and 1 dose postoperatively.
Results
At the cost of $144.07, S aureus nasal screening would be cost-effective only if the initial infection rate of cochlear implantation (1.7%) had an ARR of 0.60% ( Table 1 ). The least costly decolonization protocol, 2% intranasal mupirocin ointment costing $5.09 at our institution, was determined to be cost-effective with an ARR of 0.02%. A combined decolonization technique with 2% intranasal mupirocin ointment, chlorhexidine wipes, chlorhexidine shower, and prophylactic vancomycin (2 doses of 1 g intravenous) was the most expensive decolonization option at $37.57, though still cost-effective with an ARR of 0.16%.
The break-even analysis was also applied with a range of infection rates due to the fact that the rate of infection varies in the literature, as well as by institution and surgeon. For these calculations, the cost of revision following infection and the cost of the most expensive decolonization protocol were held constant. Varying infection rate to as high as 15% demonstrated that the cost-effectiveness of the most expensive decolonization protocol did not change, maintaining an ARR of 0.16% ( Table 2 ).
Initial and Final Infection Rates a
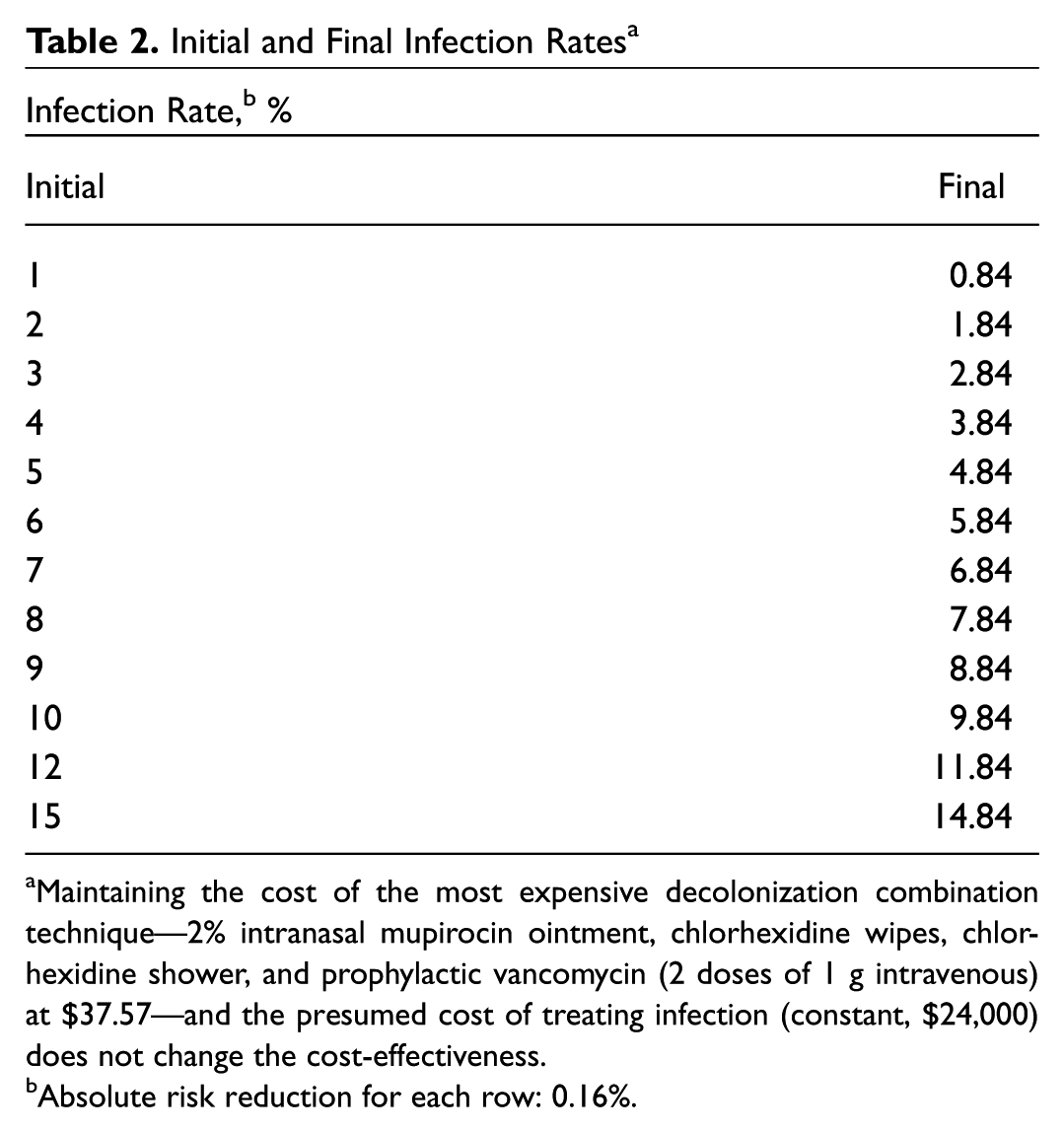
Maintaining the cost of the most expensive decolonization combination technique—2% intranasal mupirocin ointment, chlorhexidine wipes, chlorhexidine shower, and prophylactic vancomycin (2 doses of 1 g intravenous) at $37.57—and the presumed cost of treating infection (constant, $24,000) does not change the cost-effectiveness.
Absolute risk reduction for each row: 0.16%.
We also examined how variations in cost of revision affected the outcome of the break-even analysis. For these calculations, the initial rate of infection and the cost of the most expensive decolonization protocol were held constant. The results of these analyses showed that increasing the cost of treating infection enhanced the cost-effectiveness of the most expensive decolonization protocol, with an ARR of 0.04% at $100,000, the highest cost of treating infection reported in the literature ( Table 3 ).
Cost of Treating Infection and Final Infection Rate. a
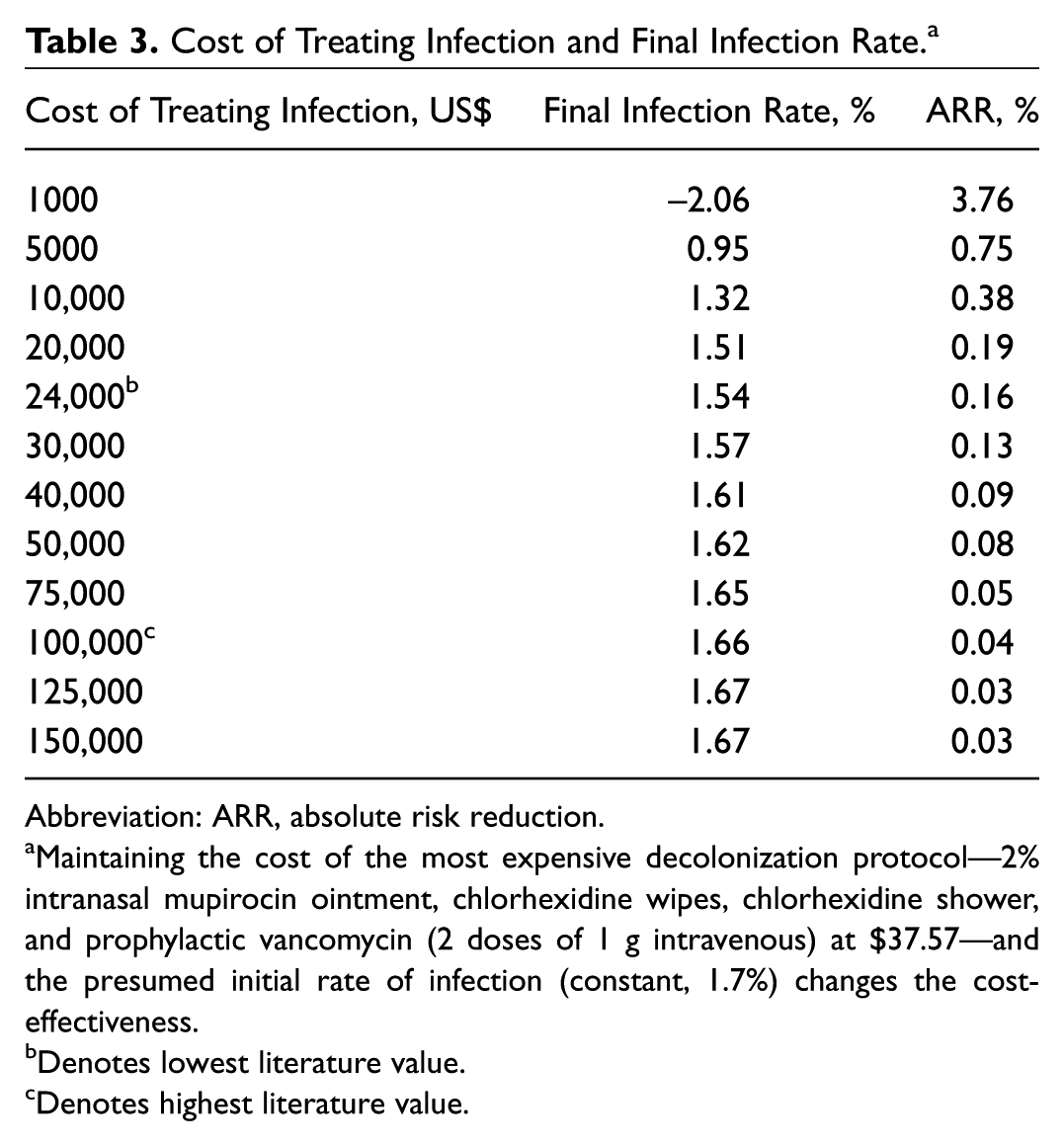
Abbreviation: ARR, absolute risk reduction.
Maintaining the cost of the most expensive decolonization protocol—2% intranasal mupirocin ointment, chlorhexidine wipes, chlorhexidine shower, and prophylactic vancomycin (2 doses of 1 g intravenous) at $37.57—and the presumed initial rate of infection (constant, 1.7%) changes the cost-effectiveness.
Denotes lowest literature value.
Denotes highest literature value.
Discussion
The main organisms that cause infection in CI surgery are derived from the skin flora present at the site of surgical implantation. S aureus is one of the most common infective agents, and it is of particular importance because it tends to form biofilms when it comes into contact with implants. Biofilms pose a serious clinical challenge because they confer resistance to host immune defenses and antibiotic penetration, which allows for the prolonged survival and proliferation of bacteria. 22 This can result in undesirable and, often, detrimental postoperative sequelae, such as persistent otitis media, mastoiditis, bacterial meningitis, and other major infections. 5
Treatment of major CI infections frequently requires costly inpatient hospital stays, intravenous antibiotics, and surgical intervention, such as drainage, debridement, and implant removal. Implant removal is undesired because it causes significant emotional and physical distress due to deafness. Antimicrobial and surgical treatment without implant removal is the preferred treatment modality, but it is usually not possible nor indicated, especially when the suspected organism is a drug-resistant strain such as methicillin-resistant S aureus. 23 Furthermore, when the infection is directly related to the primary surgery itself, as in the case of skin flap infections, explantation is often the preferred treatment.7,8
Upon explantation, an appropriate antibiotic regimen is initiated for 1 to 3 months, after which reimplantation may be attempted. However, reimplantation is costly and sometimes physically impossible due to extensive scarring of tissues. While the reported rate of CI infectious complications remains relatively low at 1.7% to 4.1%,5,12,23-25 financially and physically devastating infections resulting from S aureus represent the most common source.5,12
Such infections can possibly be minimized by implementing cost-effective prophylactic decolonization protocols. The general efficacy of these protocols is supported by meta-analytic and prospective randomized trial data.11,26,27 Use of intranasal mupirocin combined with chlorhexidine soap has demonstrated a risk reduction of health care–acquired S aureus infections of up to 60% in surgical cases. 11 Utilization of mupirocin ointment alone has also demonstrated a significant reduction in S aureus infections, with rates decreasing by nearly half. 27
This break-even analysis demonstrates that prophylactic S aureus decolonization techniques require only mild reductions in infection rates and thus may be highly cost-effective for preventing infection following cochlear implantation. Meanwhile, S aureus colonization screening requires a large reduction in the initial infection rate to be cost-effective. At our institution’s price point, decolonization with mupirocin is economically justified if it prevents at least 1 infection out of 5000 implants. In contrast, S aureus colonization screening needs high reductions in the infection rate to be cost-effective, and those patients found to have S aureus colonization would still need treatment.
The utility of the break-even analysis is that it provides a simple economic model to determine the cost-effectiveness of prophylactic protocols for CI complications, even when infection rates in CI are prohibitively low to perform a randomized controlled trial. For example, the present analysis found that S aureus decolonization has an ARR as low as 0.02%. To appreciate this result in a clinical trial with a power of 80% and an alpha of 0.05, the required sample size would need to be 15,366,400 patients. The most expensive decolonization protocol in the present study, with an ARR of 0.16%, would require a sample size of 760,000 patients.
There is considerable variability within the literature regarding the rate of CI infection as well as the cost of revision.3,5,6,14 However, this research demonstrates that the initial infection rate does not affect ARR, even when the cost of revision and the cost of colonization screening or decolonization are manipulated. Nevertheless, ARR does change appreciably as cost of revision changes. However, the true practicality of the break-even analysis used in this study is that it allows for practices and institutions to use their own data to determine for themselves if universal colonization screening or decolonization is a cost-effective policy.
This work was an economic decision analysis and, as such, has several important limitations. The cost data used were for a single institution and may not reflect the costs within health care as a whole. Furthermore, this analysis used historic data and, as such, may not be applicable as rates of drug resistance change. This work also did not differentiate among age groups (eg, pediatric, adult, geriatric), individual patient risk factors, and whether surgery was bilateral, unilateral, or revision. Epidemiologic data were also not fully encompassed in this research. For example, the present analysis did not control for variances in S aureus colonization rates, which have considerable weight regarding a practice’s or institution’s decision for universal screening protocols. Moreover, neither the variability in the dominant organism found in CI infections nor the variability of institutional antibiograms was considered. While adverse reactions to most decolonization protocols are rare and commonly limited to local irritation, 11 the economic model used in this analysis is not capable of incorporating the economic implications of these reactions. This work does suggest an area for further prospective study for examining clinical and economic benefits.
Author Contributions
Disclosures
Footnotes
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
This article was presented at the AAO-HNSF 2018 Annual Meeting & OTO Experience; October 7-10, 2018; Atlanta, Georgia.
