Abstract

Nasal airway obstruction (NAO) is one of the most frequently presenting symptoms in a typical otolaryngology practice. Therapies to correct nasal valve collapse (NVC) 1 include invasive functional rhinoplasty procedures involving lateral wall grafting with autologous 2 or synthetic nonabsorbable graft materials 3 and nonsurgical solutions such as nasal strips or cones. Recently, a minimally invasive procedure that entails placement of an absorbable nasal implant to support upper and lower lateral cartilage was developed to address NVC. 1
Case Report
The patient was a 53-year-old white man with a 3-year history of NAO. The patient underwent prior septoplasty and turbinate reduction procedures. Examination using the modified Cottle maneuver revealed NVC was a contributor to the patient’s symptoms. The patient completed the Nasal Obstruction Symptom Evaluation (NOSE) instrument at baseline and at subsequent follow-up visits. The patient had a baseline NOSE score of 65, indicative of severe NAO symptoms. 4 Surgical correction consisting of functional rhinoplasty using cartilaginous grafts, suturing techniques, or an absorbable implant was offered. The patient opted for and received the absorbable implant as part of a clinical study. The study protocol and informed consent were reviewed and approved by the governing ethics committees and the Federal Institute for Drugs and Medical Devices (BfArM) prior to subject enrollment, and the study was registered on clinicaltrials.gov (NCT02188589). The study was supported with research funding by Spirox (Redwood City, California).
The implant comprises a 70:30 blend of poly-L-lactide (PLA), predominantly cylindrical, and measures approximately 1 mm in diameter and 24 mm in length (Latera; Spirox). The implant is introduced through an endonasal insertion technique using a delivery tool consisting of a 16-gauge cannula.
The target location of the implant was identified to provide maximum support to the upper and lower lateral cartilages ( Figure 1A ) at the area of maximal collapse. A skin hook was used to evert the alar rim, and the delivery device cannula was used to pierce the vestibular skin in the area of a conventional marginal incision. The cannula was advanced toward the vestibular lining and the caudal edge of the lower lateral cartilage. The implant was fully deployed in the target location.
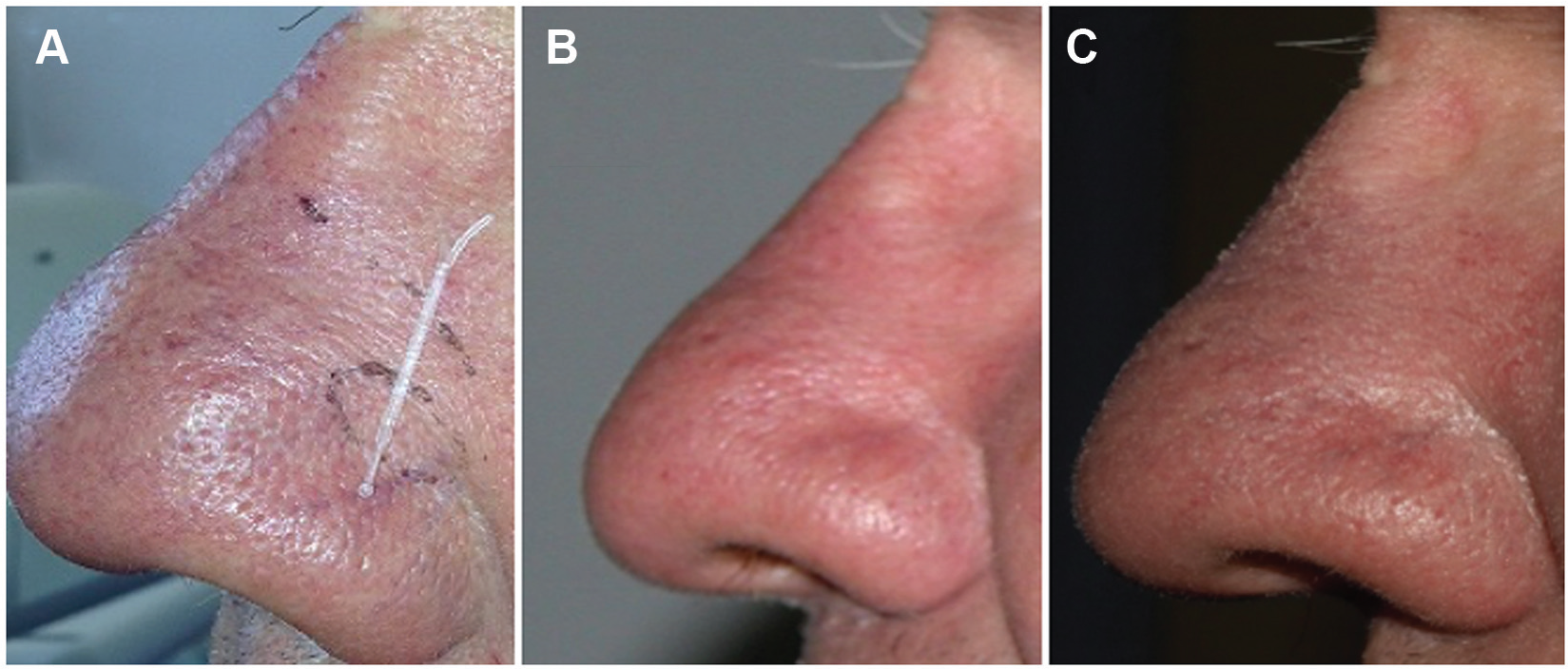
Patient marking during planning phase (A), baseline image (B), and 24 months postprocedure (C). Note that the indentation at the bridge of the nose is due to eyeglass wear and not a cosmetic effect of the implant.
Follow-up visits occurred at 1 week and 1, 3, 6, 12, 18, and 24 months postprocedure. Throughout the 2-year follow-up period, no adverse events were reported, and the patient did not require intranasal steroids, external nasal device usage, surgeries, or other treatments. The NOSE score improved from a preoperative classification of severe to postoperative classification of mild for all follow-up time points (week 1 = 25, month 1 = 25, month 3 = 15, month 6 = 5, month 12 = 5, month 18 = 20, and month 24 = 25). Although the NOSE scores fluctuated across the follow-up time points (5 to 25), all of the scores were indicative of mild symptoms. Cosmetic changes were assessed using 4 photographic views obtained under both static and full inhalation (frontal view, left side, right side, and chin up). An independent physician reviewer assessed cosmetic changes by comparing baseline images to follow-up images. This evaluation confirmed the absence of cosmetic changes from baseline to all follow-up time points ( Figure 1B , static baseline and Figure 1C , 24 months postprocedure).
Discussion
This case report presents a patient with persistent nasal obstruction symptoms due to NVC. The patient was treated with an absorbable implant to support the upper and lower lateral cartilages. Recently, a meta-analysis was conducted by Rhee et al 5 of studies covering conventional invasive surgical procedures, such as septoplasty, turbinate reduction, and functional rhinoplasty, for treatment of NAO. The meta-analysis showed mean improvement from a baseline NOSE score of 42 points. The patient in this case study achieved lasting benefits through 24 months with average NOSE score improvement of 48 points. Future studies will need to confirm the benefit of this new technology, including objective assessments of NVC such as the grading system for lateral nasal wall insufficiency proposed by Lipan and Most. 4
In contrast to spreader grafts and batten grafts, this technique can be completed in a minimally invasive manner and does not require donor cartilage harvesting, shaping, and invasive surgical placement. In addition, use of an absorbable copolymer that is incorporated into tissue over time may lower risks associated with extrusions compared to nonabsorbable alloplastic materials that are associated with high extrusion rates. While the absorbable implant presents these advantages, understanding the long-term improvement beyond the absorption profile of the implant 2 has not been fully evaluated. However, as this case study suggests, patient improvement may continue past the absorption profile. Here we report on a successful case study with 24-month follow-up using a minimally invasive technique to provide support to the lateral cartilages as an alternative to functional rhinoplasty in this patient with NVC.
Author Contributions
Disclosures
Footnotes
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
