Abstract
Nasal deformities due to trauma are more challenging to correct with rhinoplasty than nasal deformities of nontraumatic causes. Nasal osteotomy is an essential procedure for bone deviations. Preoperative planning is vital in these cases, but it is challenging to comprehend 3-dimensional (3D) structures of the nasal bone on 2-dimensional facial photographs and computed tomography images. We used a 3D-printing technique to fabricate real-size facial bone models with similar physical properties and texture as the actual bone. Furthermore, we established a precise surgical plan using simulated osteotomy on the 3D-printed model. Fused deposition modeling–type desktop 3D printer with polylactic acid filaments was used. A surgical plan was established using simulated osteotomy in 11 cases, and the actual surgery was performed as planned in 10 cases (90.9%). The 3D-printed model and stimulated osteotomy were useful for precise planning of osteotomy to correct nasal deformities due to trauma.
Keywords
Trauma to the nose often causes comminuted fractures because of the structural characteristics of the thin and plate-shaped nasal bone. If the fracture is not appropriately managed, it can create complex bone deformities and consequent external nasal deformities. Correcting nasal deformities with complex underlying malunion fractures due to trauma to straighten the nose and to restore nasal function is a great challenge for doctors performing corrective rhinoplasty. 1
Preoperative thin-slice computed tomography (CT) is essential for evaluation and surgical planning, but it is challenging to comprehend 3-dimensional (3D) structures on 2-dimensional CT images or facial photographs. Because the shape, thickness, and degree of nasal deformities due to trauma vary widely across patients, precise preoperative evaluation and surgical planning are mandatory. 2 Osteotomy is an essential procedure for nasal bone deformities, and choosing the type of osteotomy for the actual surgery is the vital part of preoperative planning. 3 However, the accuracy of preoperative osteotomy planning for predicting the actual surgical outcomes is questionable.
Recently, 3D printing has been employed in the field of medicine, and its indications are gradually expanding. 4 However, since expensive 3D printers, filament materials, and professional modeling software programs are required for 3D printing, there are many limitations to its clinical application. To overcome these limitations, we used fused deposition modeling (FDM)–type desktop 3D printer to fabricate a real-size precise simulation model with similar physical properties as the nasal bone, using a free rendering software program. Furthermore, we performed simulated osteotomy on this model to precisely plan the actual osteotomy. The purpose of this study was to evaluate the usefulness of performing preoperative osteotomy on a 3D-printed model to correct nasal deformities due to trauma and to introduce an easily applicable and reproducible 3D-printing protocol for fabricating the simulation model.
Methods
Approval was obtained from the Institutional Review Board of Samsung Changwon Hospital before reviewing the medical records of patients who had undergone preoperative osteotomy on a 3D-printed model and rhinoplasty to correct nasal bone deformities due to trauma.
Fabricating 3D-Printed Simulation Models
DICOM (Digital Imaging and Communications in Medicine) data of axial images with a slice thickness of 0.6 mm were extracted from the CT scan of all patients. The 3D facial bone model was fabricated using InVesalius 3.3.1 (CTI), which is a free software program, and the model was saved in the Standard Triangle Language format. To reduce the time required to fabricate 3D model, the parts of the skull model that are not essential for simulated osteotomy were removed using Meshmixer 3.5 (Autodesk), which is a free 3D rendering program. The final 3D model was printed with 3DP-110F (Cubicon), and polylactic acid (PLA) filament was selected owing to its similarity in texture and physical properties to the nasal bone after fabrication ( Figure 1A ). The time required for printing varied from 8 to 10 hours, depending on the size of the output model, and the material cost for each model was about the US$3.
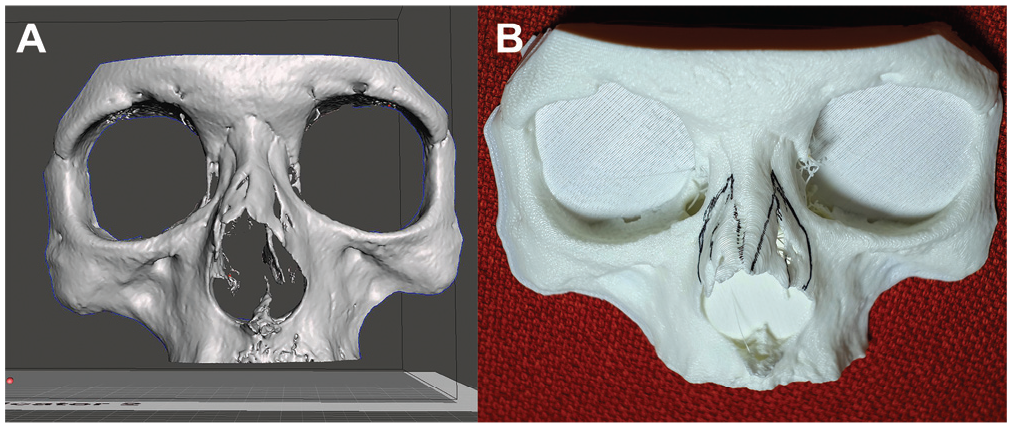
Fabrication of a real-size nasal bone model for simulation osteotomy. (A) Three-dimensional (3D) image of the anterior portion of the facial skeleton of a patient with deviated nasal bony dorsum due to previous nasal bone fracture. (B) Three-dimensional printed model for simulated osteotomy printed by fused deposition modeling–type 3D printer with the polylactic acid filament.
Surgical Simulation
Before the actual surgery, we determined the part of the nasal bone to be cut to straighten the nose during the simulated osteotomy on the model (see Supplemental Videos S1-S2 in the online version of the article). A skilled operator (Y.G.J.) marked the required osteotomy line on the 3D-printed model ( Figure 1B ). Subsequently, medial and intermediate osteotomies were performed using a 4-mm straight osteotome, and lateral osteotomy was performed using a guarded osteotome ( Figure 2 ). If the osteotomy mentioned above did not correct the nose properly, root osteotomy was also performed on the model. The surgical plan obtained using this simulation was compared with the osteotomy performed during the actual surgery. Aesthetic results at 6 postoperative months were evaluated by anthropometric measurement methods and evaluation by 2 independent physicians ( Figure 3 ). The patient and 2 evaluators were satisfied with the surgical results, which were graded as “success” when the corrected angle of deviation was less than 5 degrees. If not, they were graded as “failure.”
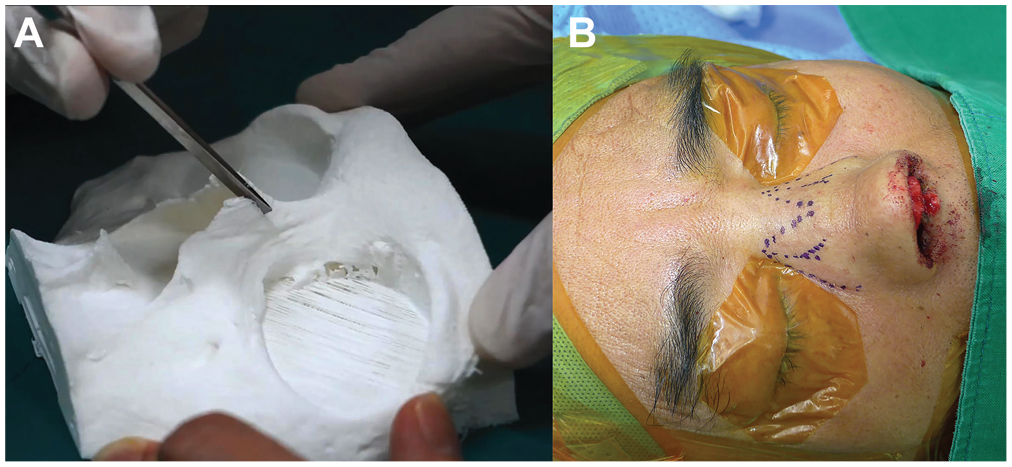
Preoperative stimulated osteotomy on a 2-dimensional printed model. (A) Simulated medial osteotomy with a 4-mm osteotome. (B) Intraoperative view of corrective rhinoplasty for patient 8 with the surgical marking for bilateral medial, intermediate, and lateral osteotomies.
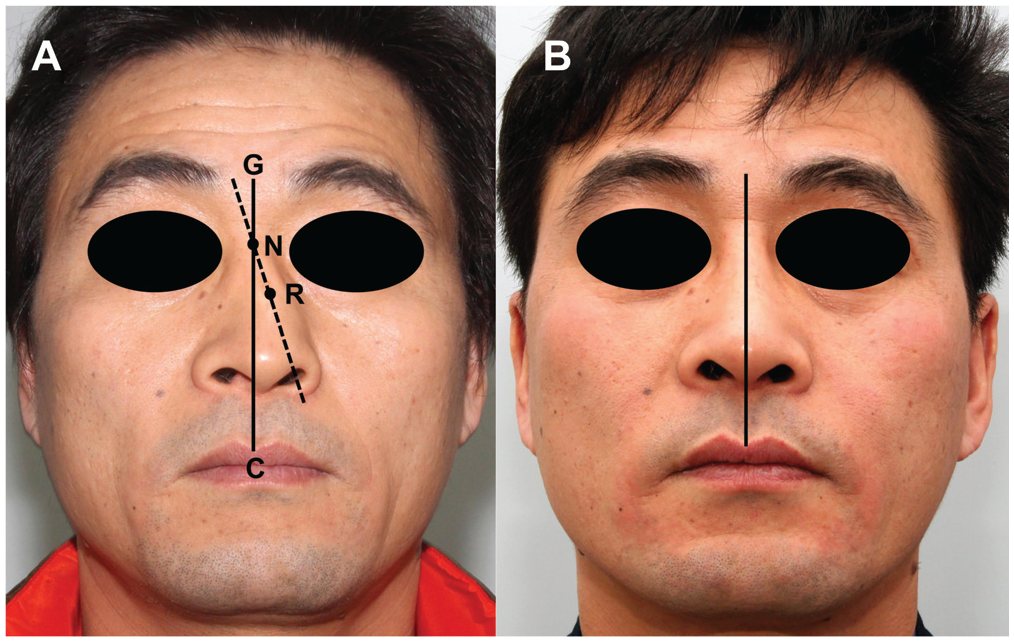
Anthropometric measurement methods. (A) The acute angle between the CG and NR lines was measured in subject 12, and the measured angle was 17.5 degrees. (B) Postoperative view of the same subject. The deviation angle was improved to 2 degrees. G, glabella; C, the center point of the upper lip; N, nasion; R, rhinion.
Results
Eleven patients were enrolled in this study from November 2016 to January 2019. All patients were men with a mean age of 38.9 (18-59) years.
Table 1
summarizes the details of the preoperative stimulated osteotomy and osteotomy during the actual surgery. The osteotomy was performed in 10 out of 11 patients (90.9%) precisely as planned, but the actual osteotomy differed from the stimulated osteotomy in 1 patient, in whom the plan to perform bilateral medial, lateral, and root osteotomies was switched to bilateral medial and lateral osteotomies (
Figure 4
). The mean deviation angle before surgery was 11.75 ± 2.59 (9-17) degrees, and the mean angle after surgery improved significantly to 2.08 ± 1.16 (0-4) degrees (
Detailed Information about the Enrolled Patients.
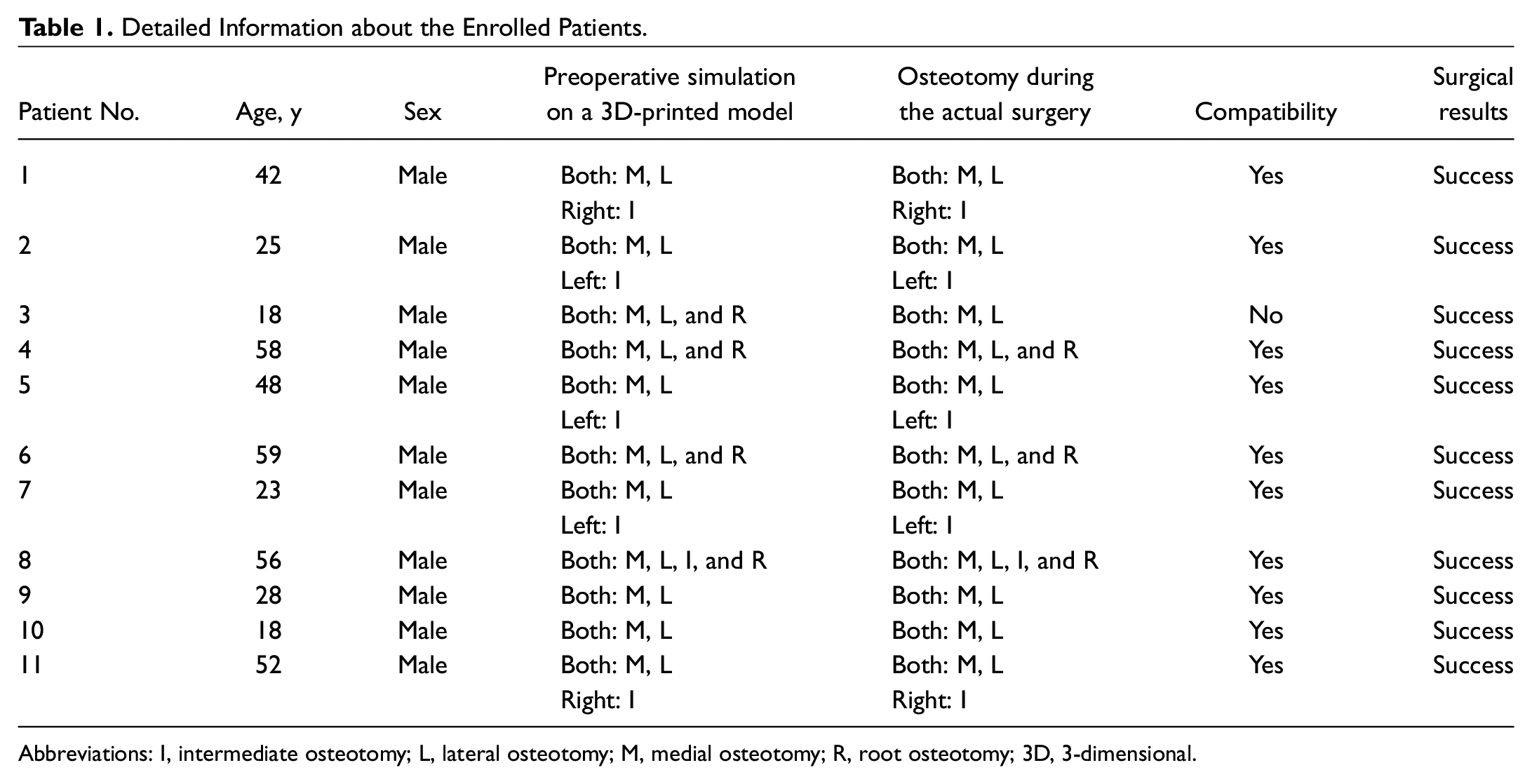
Abbreviations: I, intermediate osteotomy; L, lateral osteotomy; M, medial osteotomy; R, root osteotomy; 3D, 3-dimensional.
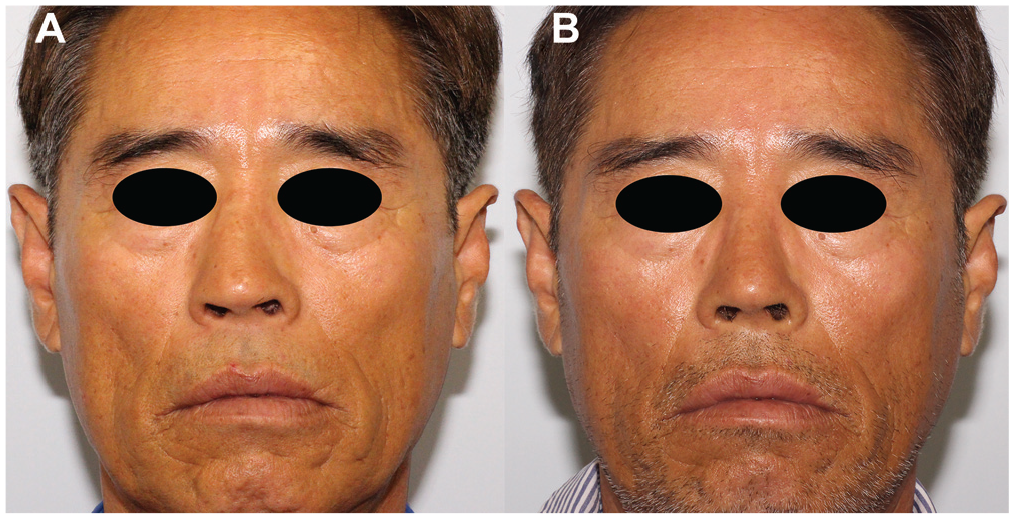
(A) Preoperative facial photograph of the subject 8 with a nasal deformity due to trauma. (B) Facial photograph 6 months after corrective rhinoplasty following a simulated osteotomy. The nose of the patient that deviated to the right was successfully corrected.
Discussion
Compared to the previous trial of the 3D-printing method for rhinoplasty, 5 we tried to introduce a simple protocol that can be easily followed by anyone using FDM-type 3D printer, cost-effective PLA filament, and a free rendering software program. The models fabricated using the FDM printer precisely matched the actual nasal bone and had similar physical characteristics. In previous cases of nasal deformities due to trauma, fracture fragments were irregularly united, and it was difficult to predict the type of osteotomy to be used accurately. When we employed this model to simulate osteotomy, a precise surgical plan concerning the type of osteotomy was established in 91% of the patients. In particular, the root osteotomy was preoperatively planned in 4 patients and performed in 3 patients. Many beginners are unfamiliar with this technique and are reluctant to apply it during the actual surgery. Our 3D printed model can help by predicting the application of the method before surgery. Given the advantages mentioned above, this method could be of great help to physicians who are not experienced with osteotomy and resident physicians in training. Besides, this technique can be applied to the planning of rhinoplasty for the nontraumatic crooked nose and wide bony dorsum.
Conclusion
We fabricated a 3D-printed simulation model with the same size and similar properties as the nasal bone at an affordable price and established a precise surgical plan using simulated osteotomy.
Author Contributions
Disclosures
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
