Abstract
Background:
The Zadek osteotomy, a dorsal closing-wedge procedure of the calcaneus, is commonly used in the surgical treatment of insertional Achilles tendinopathy, particularly in patients unresponsive to conservative measures. Although minimally invasive surgical (MIS) techniques offer potential benefits such as reduced soft tissue trauma and faster recovery, concerns persist regarding the risk of iatrogenic injury to the sural nerve because of limited visualization. This cadaveric study aims to provide a detailed anatomical assessment of the sural nerve and its branches in relation to the entry point of the MIS Zadek osteotomy, with the goal of quantifying their proximity and offering data that may help reduce the risk of nerve injury during the procedure.
Methods:
Twenty fresh-frozen human lower limb specimens were subjected to a standardized MIS Zadek osteotomy using a 3 × 30-mm Shannon burr. The osteotomy was guided fluoroscopically and performed through a lateral percutaneous approach. Post-procedure, meticulous anatomical dissections were conducted to identify the sural nerve and measure its distance from the anterior and posterior arms of the osteotomy using digital calipers with 0.1-mm precision. Measurements were independently recorded by 2 observers to ensure accuracy.
Results:
The sural nerve was successfully identified in all specimens. No instances of sural nerve transection or gross anatomical disruption were observed. The mean distance from the osteotomy to the sural nerve was 11.95 mm, with a range of 8.3 to 15.4 mm and an SD of 2.18 mm. These findings suggest that when performed within the defined anatomical parameters, the MIS Zadek osteotomy maintains a safe distance from the sural nerve.
Conclusion:
In our cadaver study, we found that the MIS Zadek osteotomy maintained a mean distance of 11.95 mm from the sural nerve. These findings define anatomical proximity; clinical safety requires prospective validation.
Clinical Relevance:
Our study defines a reproducible anatomical margin for MIS Zadek osteotomy; clinical safety needs prospective validation.
Keywords
Introduction
The Zadek osteotomy, a dorsal closing-wedge procedure of the calcaneus, is commonly employed in the surgical treatment of insertional Achilles tendinopathy, particularly in patients unresponsive to conservative measures.13,20 By removing a bony wedge from the posterosuperior aspect of the calcaneus, the procedure reduces heel prominence and offloads tension on the Achilles tendon, thereby improving symptoms and restoring function.1,2,5,18
In recent years, minimally invasive surgical (MIS) techniques for Zadek osteotomy have gained popularity due to their potential advantages over the traditional open approach. 12 These include smaller incisions, reduced soft tissue dissection, decreased postoperative pain, lower rates of wound complications, and faster recovery times.14,17Despite these benefits, MIS techniques also raise concerns about limited visualization, which may increase the risk of iatrogenic injury to nearby neural structures, particularly the sural nerve and its lateral calcaneal branches, which run close to the lateral approach commonly used in this procedure. 1
Although sensory disturbances and neural irritation have been reported following calcaneal osteotomies, the definition of anatomical “safe zones” has been proposed to minimize the risk of iatrogenic injury to nearby neurovascular structures. 6 However, the specific anatomical relationship between the sural nerve and the MIS Zadek osteotomy has not been well characterized.4,5,22
The aim of this cadaveric study was to assess the anatomical proximity of the sural nerve and its branches to the MIS Zadek osteotomy entry point, in order to demonstrate that the percutaneous technique consistently preserves a safe distance between the burr entry site and the nerve or its closest branch. In doing so, this work provides additional evidence to the existing literature and further supports the concept of a calcaneal safe zone, as previously described by Talusan et al 22 reinforcing its clinical relevance for minimizing the risk of iatrogenic injury.
Materials and Methods
This anatomical study was conducted on 20 fresh-frozen human lower limb specimens, including the foot and ankle, to investigate the relationship between the sural nerve and the site of Zadek osteotomy performed using a minimally invasive approach. The specimens included 11 female and 9 male donors, with a mean age at death of 73.3 years (range, 59-83). All specimens were fresh-frozen and preserved in accordance with anatomical laboratory standards.
The primary aim was to assess the risk of iatrogenic injury to the sural nerve during percutaneous dorsal closing wedge calcaneal osteotomy, as described for the treatment of insertional Achilles tendinopathy.
Surgical Procedure
All procedures were carried out in an anatomical laboratory under standard dissection conditions. The surgical technique used in this study followed the percutaneous Zadek osteotomy as described by Kaplan et al. 14 The procedure was performed on each specimen by a single fellowship-trained orthopaedic surgeon who was not experienced in this specific technique. Specimens were placed in the lateral decubitus position with the operative foot positioned off the edge of the table. A mini- or standard C-arm fluoroscopic unit was used to visualize and guide the procedure.
Under fluoroscopic imaging, the calcaneal “safe zone” as defined by Talusan et al 22 was identified (Figure 1). Two percutaneous Kirschner wires (K-wires) were inserted to demarcate the planned osteotomy. The first K-wire was placed dorsally to plantarly, extending from just anterior to the Haglund prominence to just proximal to the insertion of the plantar fascia. The second K-wire was placed to create a plantar hinge, forming a wedge with a height ranging from a minimum of 8 mm to a maximum of 10 mm (Figure 2).

The safe zone of the calcaneus defined by Talusan et al. 22

(A) Clinical photograph showing position of percutaneous K-wires acting as a cut guide for the Zadek osteotomy. (B) Radiograph image of the K-wire placement acting as a cut guide for the Zadek osteotomy as shown. 14
A 5-mm incision was made within the safe zone to minimize the risk of sural nerve injury. Blunt dissection was performed to reach the calcaneal surface. Using a 3 × 30-mm Shannon burr, a dorsal closing wedge osteotomy was carried out along the trajectory outlined by the K-wires. Bone was resected in a systematic quadrant-based approach, proceeding from lateral to medial in the coronal plane, and sequentially through plantar, middle, and dorsal thirds in the sagittal plane—each subdivided into anterior and posterior segments. Care was taken to preserve a 5- to 8-mm plantar hinge to avoid violation of the plantar cortex.
Following wedge removal, dorsiflexion of the ankle was applied to close the osteotomy and achieve bone apposition. Proper reduction was confirmed fluoroscopically by the transition of the K-wires from an oblique to a parallel orientation.
Anatomic Dissection
On completion of the osteotomy, each specimen underwent careful anatomical dissection performed by 2 fellowship-trained orthopaedic surgeons. To identify the sural nerve, dissection began posteriorly in the leg, tracing the course of the small saphenous vein, which typically runs in proximity to the nerve and serves as a reliable landmark. The sural nerve was then located in relation to the lateral border of the Achilles tendon, where it generally crosses approximately 8 cm proximal to the level of the intermalleolar line. Additional landmarks were used at the level of the ankle, where the sural nerve was consistently found posterior to the lateral malleolus, at approximately 2.5 cm from its most prominent point. The position of the nerve was further confirmed using the distance from its origin to the intermalleolar line, reported in the literature to average around 16 cm, providing a reliable reference for orientation. 7 In each cadaveric specimen, the sural nerve was carefully exposed along its course in the posterior-lateral aspect of the calcaneus. In addition to the main trunk, we systematically identified its nearest branches, taking into account the anatomical variations previously described by Steele et al. 21
Once exposed, the nerve and its branches were inspected for any direct injury. The minimal distance between the burr entry point of the osteotomy and the sural nerve or its nearest branch was measured using digital calipers with a precision of 0.1 mm. We specifically identified the nearest sural nerve branches to the burr/osteotomy; medial and tibial branches were not traced or measured, as the focus of this study was limited to the lateral sural nerve anatomy and its proximity to the osteotomy.
All measurements and dissections were performed by the same 2 observers to ensure reproducibility and minimize bias. The data were analyzed to determine the average distance between the burr entry point and the sural nerve or its closest branch, and to document the frequency of any nerve lesions resulting from the procedure (Figures 3 and 4).

Measurement of the minimal distance between the osteotomy line and the sural nerve. Following exposure, the sural nerve was carefully inspected for any signs of direct injury. A digital caliper with a precision of 0.1 mm was used to measure the shortest distance between the osteotomy line and the nerve. This measurement was performed consistently by the same 2 observers to ensure reproducibility and minimize interobserver bias.
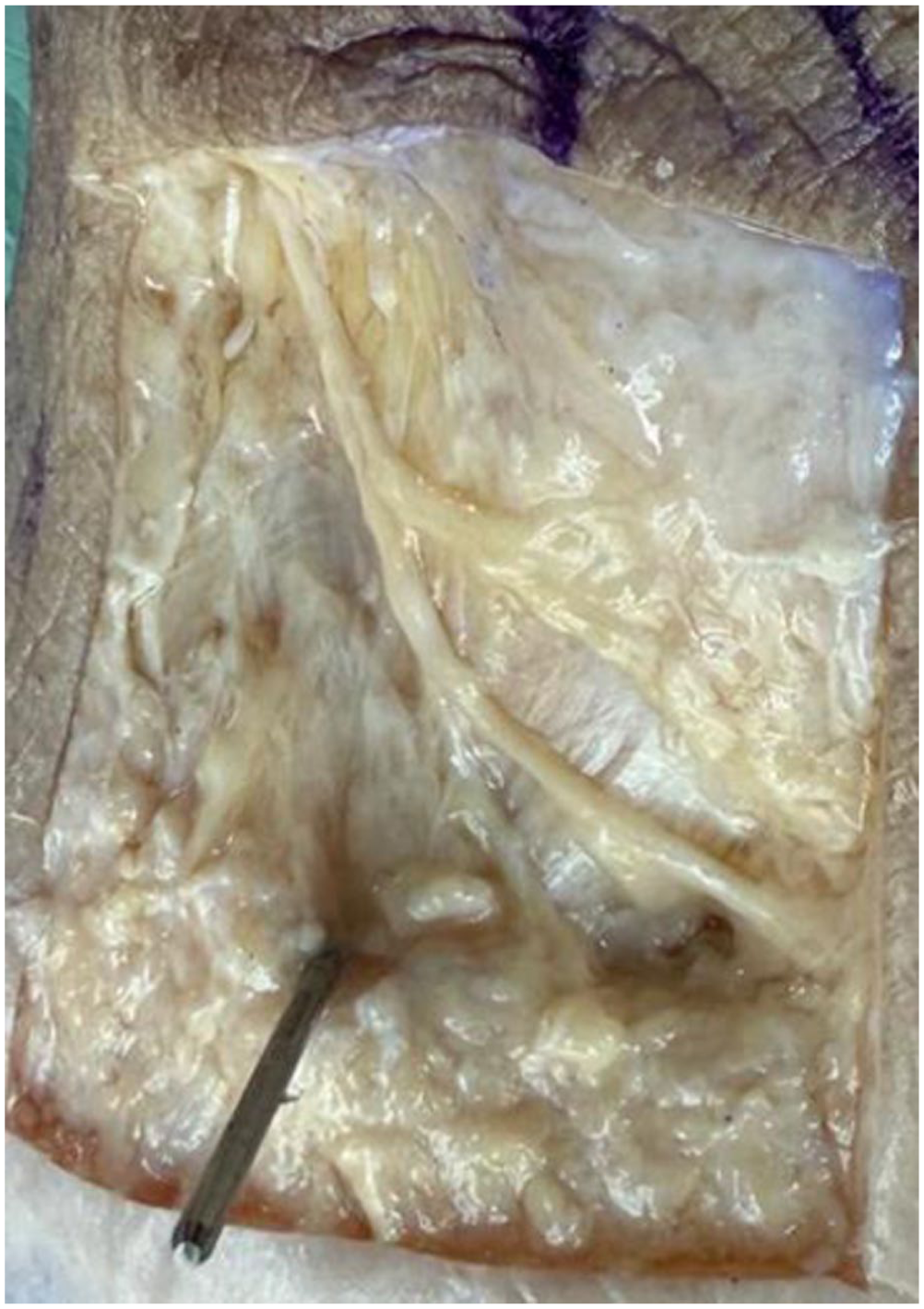
Anatomical specimen following percutaneous Zadek osteotomy and dissection. The image shows the entry point of the osteotomy, marked by a Kirschner wire (K-wire), and the closest branch of the sural nerve. The nerve and its branches were isolated to illustrate their spatial relationship to the osteotomy entry site.
Statistical Analysis
All statistical analyses were performed using Python (Python Software Foundation) with the SciPy and NumPy libraries. Normality of the continuous variables was assessed by visual inspection of histograms and Q-Q plots, as well as by the Shapiro-Wilk test. Descriptive statistics, including mean, SD, skewness, and kurtosis, were calculated to summarize the distribution of the data (Figures 5 and 6). The Shapiro-Wilk test did not reject the null hypothesis of normality (P = .29), indicating that the data were consistent with a normal distribution. A significance level of α = 0.05 was adopted for all statistical tests.

Histogram of the measured distances. Histogram illustrating the distribution of the distances between the drill entry point and the sural nerve. The data appear approximately symmetric and close to a normal distribution.

Q-Q plot of the measured distances. Quantile-quantile (Q-Q) plot comparing the observed distribution of the distances with the theoretical normal distribution. Data points closely follow the reference line, supporting the assumption of normality.
Results
The dissection of all 20 fresh-frozen lower limb specimens allowed for clear identification of the sural nerve or its nearest branch and its anatomical relationship with the burr entry point of the percutaneous Zadek osteotomy. No gross anatomical disruption or transection of the sural nerve was observed in any specimen.
The minimum distance between the burr entry point and the sural nerve or its nearest branch was measured in each specimen. The distances ranged from 8.3 to 15.4 mm. The mean distance between the osteotomy and the sural nerve was 11.95 mm, with an SD of 2.18 mm (95% CI, 10.93-12.97 mm). Interobserver reliability for distance measurements showed excellent agreement, with an intraclass correlation coefficient (ICC) of 0.92 (95% CI, 0.85-0.96). Intraobserver reliability was also excellent, with an ICC of 0.94 (95% CI, 0.88-0.97).
These measurements, reported in Table 1, represent the average of the values independently recorded by two investigators.
Minimum Distance (mm) Between the Burr Entry Point and the Sural nerve (or Its Nearest Branch) for Each Specimen, Including Assessment of Nerve Contact and Compliance With the Predefined Safe Zone (≥ 5 mm).

Values represent the mean of measurements independently recorded by two observers.
These findings support our initial hypothesis and aim, indicating that when the percutaneous Zadek osteotomy is performed using the described minimally invasive technique within the defined calcaneal safe zone, it consistently preserves a safe distance from the sural nerve and its branches.
Discussion
MIS Zadek osteotomy has gained popularity as a surgical treatment for insertional Achilles tendinopathy and Haglund’s deformity, offering reduced postoperative morbidity, faster recovery times, and fewer wound-related complications. 11 However, a persistent concern among surgeons is the risk of sural nerve injury during the percutaneous approach, primarily because of the limited visualization and tactile feedback inherent to minimally invasive techniques.6,8 This study was designed to address that concern through cadaveric evaluation of the anatomical relationship between the osteotomy plane and the sural nerve.
The sural nerve is a purely sensory structure that innervates the posterolateral aspect of the lower leg and the lateral foot, and its anatomical course is highly variable. 23 Recent anatomical research by Khadanovich et al 15 demonstrated that the sural nerve typically presents with multiple side branches—averaging more than 4 per leg—with the highest branch density observed between 2.1 and 6.0 cm above the lateral malleolus. 15 These findings underscore the importance of careful dissection planning, as inadvertent injury to these branches—even if the main trunk is preserved—may result in sensory disturbances or neuropathic pain following posterior hindfoot procedures.
Although the traditional open Zadek osteotomy remains a well-established option for treating insertional Achilles tendinopathy, it is not without complications—particularly in relation to soft tissue handling and neurovascular structures. 15 A systematic review by Black et al 3 reported a 2% incidence of sural nerve paresthesia among 247 cases, in addition to other complications such as symptomatic hardware (2.8%) and superficial wound infections (3.2%). Similarly, Maffulli et al, 16 in their case series involving 28 patients treated with a modified dorsal closing wedge osteotomy, observed sural nerve–related symptoms in 3.5% of cases. These findings highlight that although the open technique is generally safe and clinically effective, the proximity of surgical dissection to the sural nerve continues to pose a risk, particularly during soft tissue retraction and osteotomy execution. Compared with percutaneous approaches, the open method allows for more direct visualization but may also require more extensive dissection, which can potentially increase the risk of nerve disturbance.
In our cadaveric analysis, no injuries to the sural nerve were identified across the 20 fresh-frozen lower limb specimens. The direct dissection approach enabled precise identification and measurement of the distance between the sural nerve and the osteotomy plane. In all cases, a safe anatomical buffer was maintained when the MIS Zadek osteotomy was performed using our described technique. The minimum measured distance was 8.3 mm, the maximum 15.4 mm, and the mean 11.95 mm (SD 2.18 mm; 95% CI, 10.93-12.97 mm). These results define a reproducible anatomical margin between the MIS Zadek osteotomy and the sural nerve. Although this margin may inform surgical planning, its clinical significance requires prospective validation under dynamic operative conditions.
Although the minimally invasive approach offers many benefits, nerve injury remains a concern. Hall et al 9 reported a 4.6% incidence of nerve injuries in MIS Zadek osteotomy compared with 2.22% in open midline Achilles tendon–splitting procedures. Similarly, Phillips et al 19 observed a 4.7% rate of transient tibial neuritis, which resolved within 3 months. These findings, although relatively low, indicate that even percutaneous techniques are not immune to neurovascular complications.
Cadaveric work by Guirguis et al 8 demonstrated that certain burr trajectories, such as the apex posterior approach, may increase the likelihood of neural damage due to closer proximity to key neurovascular structures.
These anatomical concerns underscore the need for high precision and anatomical familiarity when performing MIS Zadek osteotomy. The risk of nerve injury during MIS Zadek osteotomy is influenced by multiple variables, including the proximity of surgical instruments to neurovascular bundles—particularly the sural nerve—and the reliance on surgeon perception to estimate depth and location of the resection. Additionally, the limited tactile feedback inherent to percutaneous techniques reduces the ability to make real-time corrections.
To reduce the risk of nerve injury, adherence to a probable “safe zone” is critical. Our findings measuring this distance in 20 cadaver legs, support that this zone was <8.3 mm from the sural nerve in all cases. Prior anatomical mapping studies have similarly emphasized the role of respecting this corridor, especially considering that the sural nerve is the most frequently affected in calcaneal osteotomies. 22 Proper surgical technique, accurate patient positioning, and careful incision planning are all key strategies to minimize neural complications.
A further consideration is the role of the surgical learning curve in the safety and efficacy of the MIS Zadek osteotomy. Hall et al 10 retrospectively analyzed 98 consecutive percutaneous Zadek osteotomy cases performed by a surgeon with no prior experience in this specific technique and observed a learning curve that plateaued after approximately 14 cases. Notably, this learning phase was limited exclusively to operative time, which decreased significantly with increasing case number. Importantly, no significant differences were found in complication rates, nonunion, revision surgeries, or patient-reported outcomes such as Functional Foot Index (FFI) and visual analog scale (VAS) scores across different levels of surgeon experience. These findings suggest that although procedural efficiency improves with familiarity, the technique can be performed safely and without increased risk of iatrogenic nerve injury—even during a surgeon’s initial cases—when standard operative protocols are respected. This supports the notion that adherence to anatomical landmarks and technique reproducibility may compensate for the lack of prior specific experience in MIS Zadek osteotomy.
Although minimally invasive procedures offer clear advantages, they are not without limitations. As noted in the literature, the incidence of nerve injuries in some MIS contexts, such as lumbar spine surgery, can occasionally be higher than in open procedures because of reduced visualization and tactile control. This serves as a reminder that the benefits of MIS techniques must be balanced with thorough anatomical knowledge, careful planning, and ongoing evaluation of surgical protocols.
This study has several strengths. The use of fresh frozen cadaveric specimens allowed for realistic simulation of live tissue properties, whereas the dual-surgeon model improved procedural consistency and reduced observational bias. The direct anatomical measurements provide robust and reproducible data regarding the spatial relationship between the osteotomy site and the sural nerve. Nevertheless, limitations include the absence of intraoperative radiographic correlation and the inability of cadaveric data to match patient-specific anatomical variability or clinical outcomes. Moreover, cadaveric studies cannot replicate intraoperative factors such as inflammation, bleeding, and individual anatomical variation, all of which may affect nerve proximity and clinical outcomes.
Conclusions
These findings support a reproducible anatomical margin between the MIS Zadek osteotomy as described in this article and the sural nerve. However, clinical safety and functional outcomes require prospective validation.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251412344 – Supplemental material for Percutaneous Zadek Osteotomy and Sural Nerve Proximity: A Cadaveric Anatomical Mapping Study
Supplemental material, sj-pdf-1-fao-10.1177_24730114251412344 for Percutaneous Zadek Osteotomy and Sural Nerve Proximity: A Cadaveric Anatomical Mapping Study by Paolo Ivan Fiore, Alice Montagna, Enrico Pozzessere, Tyler A Gonzalez, Jonathan R M Kaplan and Ettore Vulcano in Foot & Ankle Orthopaedics
Footnotes
ORCID iDs
Ethical Considerations
This study did not require approval from an ethics committee, as it involved a cadaveric study.
Author Contributions
Conceptualization, P.I.F., A.M.; methodology, P.I.F, A.M., E.P., T.G., J.R.M.K., E.V.; validation, P.I.F., A.M., E.V., T.G., J.R.M.K.; formal analysis, E.P., T.G., J.R.M.K.; resources, P.I.F., A.M., E.P., E.V.; writing-original draft preparation, P.I.F, A.M.; writing-review and editing, P.I.F., A.M., E.P., T.G., J.R.M.K., E.V.; supervision, E.V.
All authors have read and agreed to the published version of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
Data Availability Statement
The data sets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
