Abstract
A case of a blowout fracture with sever post traumatic emphysema is described in this study. The clinical presentation, diagnosis and management of orbital emphysema associated with blowout fractures are discussed, and the literature reviewed. This case highlights the importance of proper diagnostic measures and necessary treatment when dealing with orbital trauma patients. The clinical examination of motility, visual acuity and pupillary affect are primarily the most important factors of deciding suitable therapy. In an emergency, time is of the essence to reduce the risk of permanent vision loss.
Introduction
Orbital trauma may result in blowout fractures due to the increased pressure to the surrounding bone in the orbit. 1,2 This is most likely explained by the thin bone defining its anatomy and its closeness to the maxillary and ethmoid sinuses. 3 Another theory is that increased pressure applied to the infraorbital rim, directs the transmission of force directly to the orbital floor causing a blowout fracture. 4
The abnormal presence of air in the orbit, orbital emphysema, is a regular finding in orbital fractures. 5 In the broken barrier between the sinuses and the orbit, the air passes through the openings into the orbital space. Orbital emphysema can induce an elevation of the intraorbital pressure causing serious complications such as central retinal artery occlusion and ischemic optic neuropathy. 3 Therefore, the physician must be aware of typical signs of emphysema and thoroughly examine the patient with careful monitoring.
We report a case of a blowout fracture in an adult female who developed a pronounced emphysema after blowing her nose and therefore contribute our experience to the literature which is reviewed.
Case Report
This case report has adhered to the tenets of the 1964 Declaration of Helsinki. Written informed consent for the publication of this report has been obtained from the patient. Approval from an ethical committee was not required for this case report.
A 46-year-old female presented to the Department of Surgical Sciences, Plastic & Oral and Maxillofacial Surgery, Uppsala University Hospital, with 3-day history of periorbital swelling and painful motility of the left eye. History revealed that the patient, under the influence of alcohol, fell on an inhouse gate during New Year’s Eve. On admission, at another local hospital, a 2 cm laceration was noticed on the skin corresponding to the infraorbital rim. There were no evident signs of concussion, so the laceration was closed with sutures with no radiology completed.
One day after the trauma, the patient reported an increased swelling of the periorbital tissue (Figure 1). Due to the increase of pressure and pain during movement of the eye, she returned to the emergency room 3 days later, whereas a computed tomography examination of the midface was performed, and a blowout fracture was diagnosed showing severe signs of emphysema with resulting exophthalmos according to the Hertel index 6 (Figure 2). The emphysema was orbital, subconjunctival and subcutaneous. The inferior rectus muscle was clearly herniated into the maxillary sinus, but with no clear impingement (Figure 3A to C).
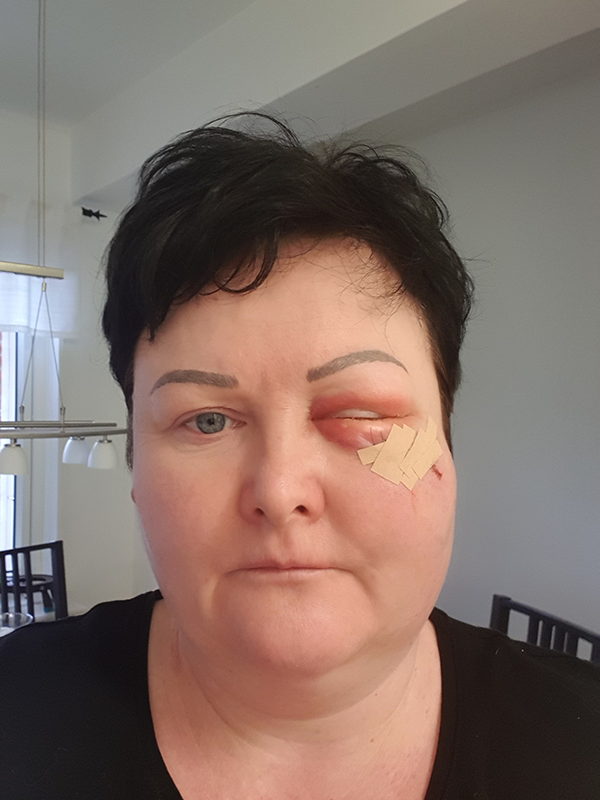
Day 1 after trauma. Periorbital swelling.
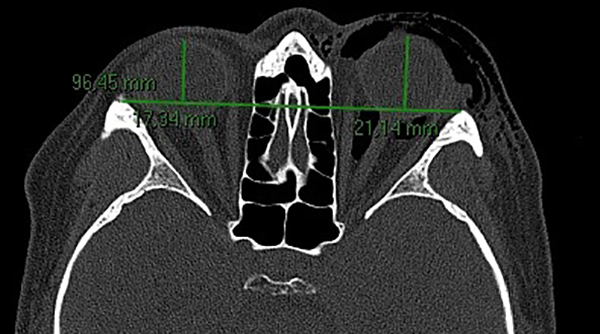
Radiological examination showed an exophthalmos according to the Hertel index.
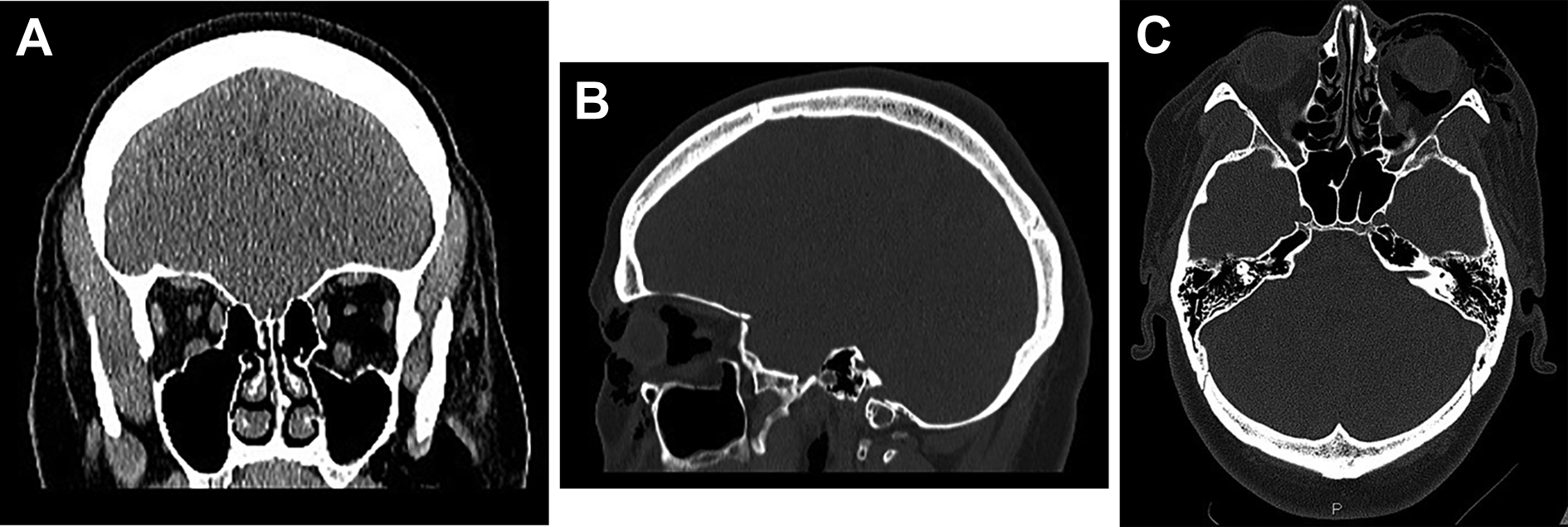
(A). Orbital floor fracture with clear herniation of the inferior rectus muscle. (B) and (C) Emphysema in the intraconal, subconjunctival and subcutaneous space.
The patient confirmed several attempts of blowing her nose after the initial trauma.
Initial ophthalmic examination revealed intraocular pressure being 18 mmHg and 25 mmHg in the right and left eye respectively. There was a mild limitation of extraocular motility of the left eye upon supraduction and a minor limitation upon infraduction. During supraduction, the patient experienced diplopia. A pupillary defect was absent and visual acuity was normal.
Since the intraocular pressure was not significantly elevated and the vision not clearly impaired, the patient was advised not to blow her nose and prescribed a topical antiglaucoma drug (timolol 0.5% twice daily) and prophylactic antibiotics (amoxicillin 500 mg × 3 for 1 week). One-day follow-up revealed a decrease of pressure to 14 mmHg on both eyes, a clear decrease of periorbital swelling and the absence of diplopia upon supraduction. However, there were still mild and painful limitations of motility superiorly, signs of exophthalmos, herniation and rounding of the rectus muscle and therefore an indication for repair and reduction of the fracture was present.
The fracture was exposed through a transconjunctival incision and repaired with an orbital floor titanium mesh high-density polyethylene sheet implant (MEDPOR; ©Stryker 2020, Michigan, USA). Intraoperative CT scans showed good positioning (Figure 4A, B). Forced duction test was normal. At the 1-month follow-up, the emphysema was resolved, and the patient had normal eye motility without diplopia or any signs of exophthalmos.
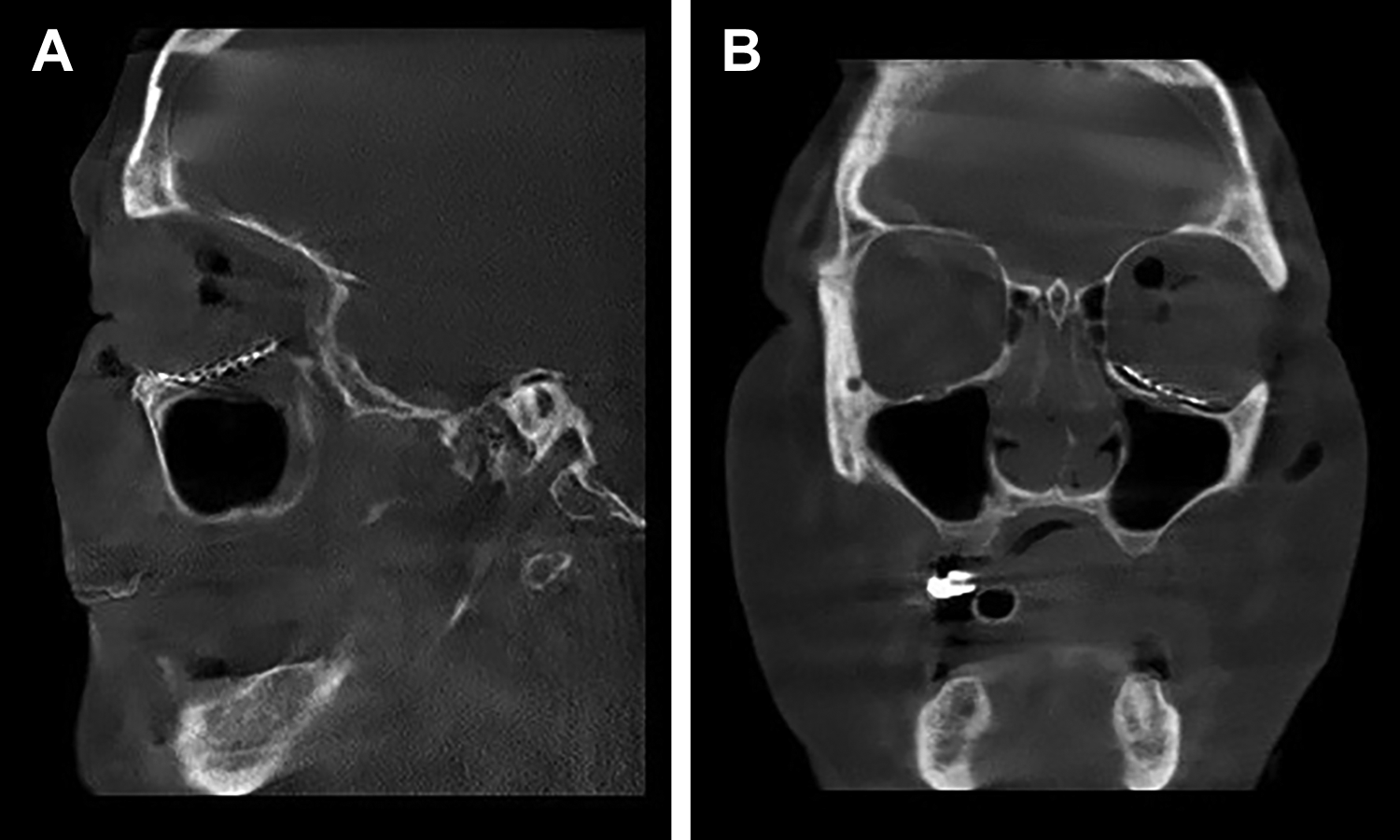
(A) and (B). Outcome of reconstruction of the orbital floor.
Discussion
This paper describes a severe self-induced orbital emphysema due to nose blowing. Furthermore, it also represents the importance of proper diagnostic measures; radiological examination with a CT scan was not performed. A missed measure, potentially endangering the patients’ vision.
Orbital fractures may be solitary but often involved in a complex of larger midface fractures. Orbital fractures often involve the sinuses superiorly (frontal) inferiorly (maxillary) and medially (ethmoid). Nontraumatic events such as nose blowing, and sneezing have been described to induce blowout fractures. 7 A similar case was published of such outspread emphysema; however, it was presented a few hours after the initial trauma. 8
Orbital emphysema is commonly detected in orbital fractures (specificity of 99.6%) and is usually not severe or long-lasting enough to cause visual compromise. 5,9,10 However, orbital emphysema is considered a medical emergency and may cause serious complications depending on the intraorbital pressure. 11 Increases of pressure may cause damage to the optic nerve and occlusion of the central retinal artery. 7 The normal pressure in the orbital space ranges from 15 to 20 mmHg. 1 Previous reports have described that pressure exceeding 65 to 70 mmHg is threatening to the optic nerve and retinal artery. 3,12 Animal studies show that if the elevated pressure exceeds 105 mmHg and lasts more than 105 minutes, damage to the retina may occur and could result in partial vision loss. 13 –15
The pathophysiology of the orbital emphysema has been discussed in the literature and it is believed that the emphysema is directly correlated to the communication between the orbit and sinuses formed after trauma. 5,7,16 The elevated pressure during the Valsalva maneuver may exceed 66 mmHg and is also believed to contribute to the flow of air into the orbit. 17
A study on cadavers shows that pressure causing any rupture of the orbital periosteum differs between younger and older patients, which is 70 to 100 mmHg and 10 to 15 mmHg respectively. 1
In this case the emphysema was severely outspread in the periorbital tissue but also posterior to the bulb, between the orbital rectus muscles endangering the optic nerve.
To the best of the authors knowledge, 5 cases of blindness due to orbital emphysema have been reported on PubMed. Only 1 case reported a significantly increased intraocular pressure with 80 mmHg, 2 cases between 15 and 20 mmHg and in 2 cases no pressure measurement was reported. 13,18 –21
In the last 10 years, only 4 cases of isolated orbital floor fractures caused by trauma, with severe orbital emphysema, without involvement of the medial wall, have been reported on PubMed
Chart of Previously Reported Cases Summarizing the Etiologies, Clinical Findings and Management of Orbital Floor Fractures with Emphysema.
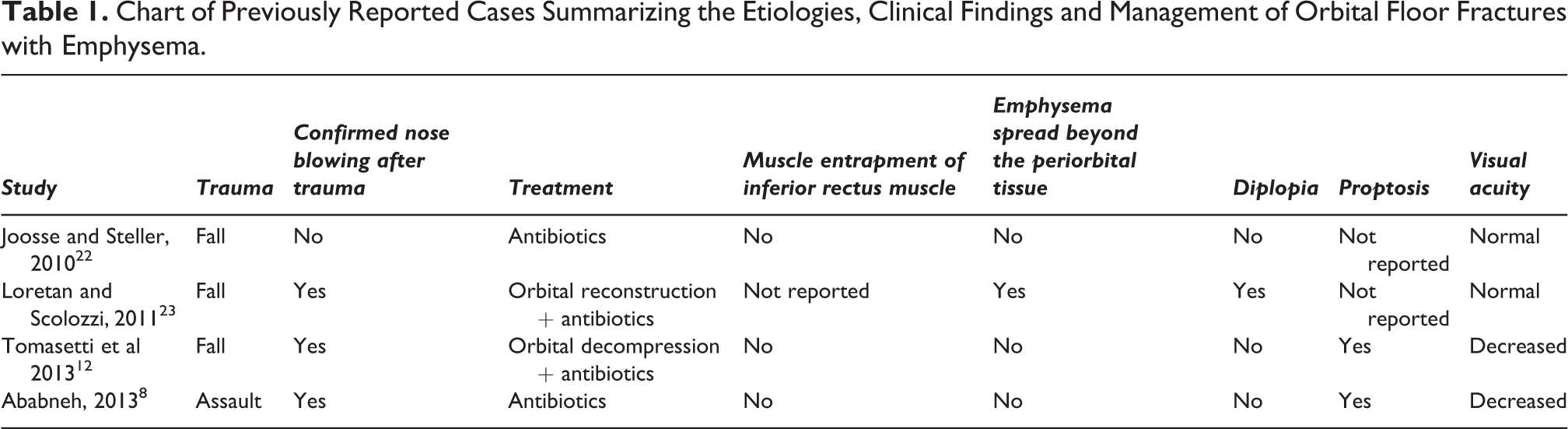
This case differs by the fact that the fracture was not diagnosed on the initial examination. The emphysema could have been prevented if a CT scan was performed identifying the fracture, whereas suitable instructions would have been given to the patient.
Most cases of orbital emphysema usually resolve spontaneously within 7 to 10 days and need no medical intervention. 11,24,25 A physician should however take into consideration that emphysema may serve as a pathway for potential infection via the superior orbital fissure and into the subarachnoid space. 5
There are several surgical procedures suggested in the literature to treat the tension of an emphysema, including lateral canthotomy, orbital decompression and transconjunctival blepharoplasty. One should outweigh the risk of potential complications such as scarring, orbital hemorrhage and ectropion. 11,12
Conclusion
Orbital emphysema is often judged as a benign sequela of an orbital fracture and controlled with patient compliance avoiding the Valsalva maneuver. However, if the fracture is not initially correctly diagnosed, the emphysema may increase violently and endanger the optic nerve with potential loss of vision. The clinical examination of motility, visual acuity and pupillary affect are primarily the most important factors of deciding suitable therapy. The literature shows low evidence of how much intraconal pressure the optic nerve sheet can tolerate. Also, in an emergency with an impact on the optic nerve, the time spent to measure the intraconal pressure may endanger the outcome as therapies such as lateral canthotomy may be preferred to reduce the risk of permanent vision loss.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
