Abstract
Study Design:
Case report.
Objective:
By reporting such a rare vascular variation of the radial artery, we aim to make other surgeons aware of comparable vascular variations in radial forearm free flap harvesting.
Methods:
In this case report, we present an 84-year-old male patient, with a rare distal branching of the radial artery into the deep palmar branch, approximately 7 cm from the wrist. In order to visualize the vascular variation, intraoperative photo documentation took place.
Results:
The radial free flap harvesting was successful and no postoperative complications were noted.
Conclusions:
Distal branching of the radial artery into the deep palmar branch may occur in radial forearm free flap harvesting. Since no restrictions in flap perfusion and/or hand perfusion were observed in our case, we recommend radial forearm free flap raising in the traditional way. No changes concerning the design and the positioning of the skin paddle need to be made.
Keywords
Introduction
The fasciocutaneous radial forearm flap (RFF) was first described by Yang et al in 1981 1 and became known as the “Chinese flap.” 2 Soon after, in 1982, Mühlbauer et al described the technique of flap raising and its advantages to the European audience. 3 Over the years, the RFF became the workhorse flap in head and neck surgery 2 due to its many indications, reliable anatomy, the low level of long-term donor side morbidity 4 the long and high-caliber vascular pedicle 3 and the ease of flap raising. 4 Additionally, the flap survival has been reported to be approximately 97% for RFF, 4 –6 with relatively few complications. 4
Anatomically, the brachial artery usually divides into the ulnar and radial artery. Both arteries form the superficial and deep palmar arch, which are responsible for the blood supply to the digits. 4 Deviations from the course of the radial artery have been described in only a few cases. 7 The incidence of anatomical variations in the radial artery ranges from 4.3% to 9%. 8,9 In these cases, a high origin of the radial artery from the brachial artery occurred most frequently. Accessory branches of the radial artery are the rarest anatomical variant, with an estimated average prevalence of 0.5%. 10 The most frequently observed branches of the radial artery in the forearm are the radial recurrent artery and various muscular branches. 11 However, artery loops, stenosis, hypoplasia, and abnormal origin are more prevalent than branches. 10
If an RFF is planned, a preoperative Allen’s test for the screening of the hand circulation is mandatory. 4 Because of the high reliability of the arterial system of the forearm, preoperative imaging is only taken into consideration if there is a pathological Allen’s test result and the other side can not be considered as an alternative. 12 In such cases, alternative flaps may be necessary. In the rare event of complications, total hand ischemia, digital ischemia, chronic vascular insufficiency, hypothenar hammer syndrome and/or cold intolerance in the digits have been reported but have not been observed by the authors themselves yet. 13
Because complications are possible, it is important to be aware of potential anatomical variations of the radial artery during the raising of an RFF. In this paper, we present 1 patient with rare branching pattern of the radial artery into the deep palmar branch, approximately 7 cm proximal to the first wrist crease.
The Case
An 84-year-old male patient presented with a pre-auricular/temporal sarcoma of the soft tissue on the left side, pT1 pN0 L0 V0 Pn1 G2 R0 (TNM 8th Edition). A 2-step surgical procedure was planned and realized. First the radical resection with temporary coverage was performed. Since the final histopathological result of the initial surgery revealed a close margin situation, reconstructive surgery using an RFF was combined with a circumferential resection to increase the histological safety margins.
Prior to the surgical procedure, an Allen’s test was performed on both arms. The result showed an adequate ulnar supply of the deep palmar arch for both sides. During the Allen’s test, no deviations were noted. Since the Allen’s test demonstrated normal blood circulation for both hands, the left (non-dominant) hand was chosen for flap harvesting.
A 6 cm × 4 cm skin paddle was marked in the usual manner and raised subfascial in an ulnar to radial direction. The radial artery could be palpated, dissected, and ligated. The skin incision was expanded to approximately 1 cm radial to the artery; the superficial branch of the radial nerve was identified and looped. While keeping a safe distance to the radial artery, the fascia was incised and the raising of the flap was continued. At this stage, anomalous distal branching of the radial artery was observed (Figure 1A). The lumen of this artery was noticeably larger than the lumen of the radial artery, and seemed to be the deep palmar branch (DPB) of the radial artery (Figure 1B and C). The DPB could be palpated and followed to the dorsal side of the forearm and the radial fossa. The incision to the antecubital fossa followed in order to dissect the pedicle from distal to proximal between the brachioradialis and the flexor carpi radialis muscle (Figure 1A). The large distal branch was temporary clamped to ensure a sufficient blood supply to the hand (Figure 1A). Since there were no signs of inadequate perfusion, the distal branch was ligated and the flap was raised in the conventional way. Small subcutaneous bleedings could be seen during the raising of the flap, which proved adequate flap perfusion at all times. No further anatomic variations occurred. The flap was anastomosed to the superior thyroid artery and a direct branch of the internal jugular vein. The patient made an uneventful recovery; the flap perfusion showed no limitations postoperatively. A, Yellow loop: superficial branch of the radial nerve; left red loop: deep palmar branch; right red loop: distal branch of the radial artery into the DPB. The incision to the antecubital fossa and the dissection of the pedicle (white arrow) from distal to proximal between the brachioradialis and the flexor carpi radialis muscle has been performed and the deep palmar branch of the radial artery has been clamped (black arrow). B, Schematic representation of the anatomical variation. Distal branching of the radial artery (RA) into the deep palmar branch (DPB), approximately 7 cm proximal to the wrist crease. BA indicates brachial artery; UA, ulnar artery; CIA, common interosseus artery; SB, superficial branch of the radial nerve. C, Yellow loop shows the superficial branch of the radial nerve, left red loop/white arrow the deep palmar branch and right red loop/black arrow the distal branch of the radial artery into the DPB. The RFF has already been raised.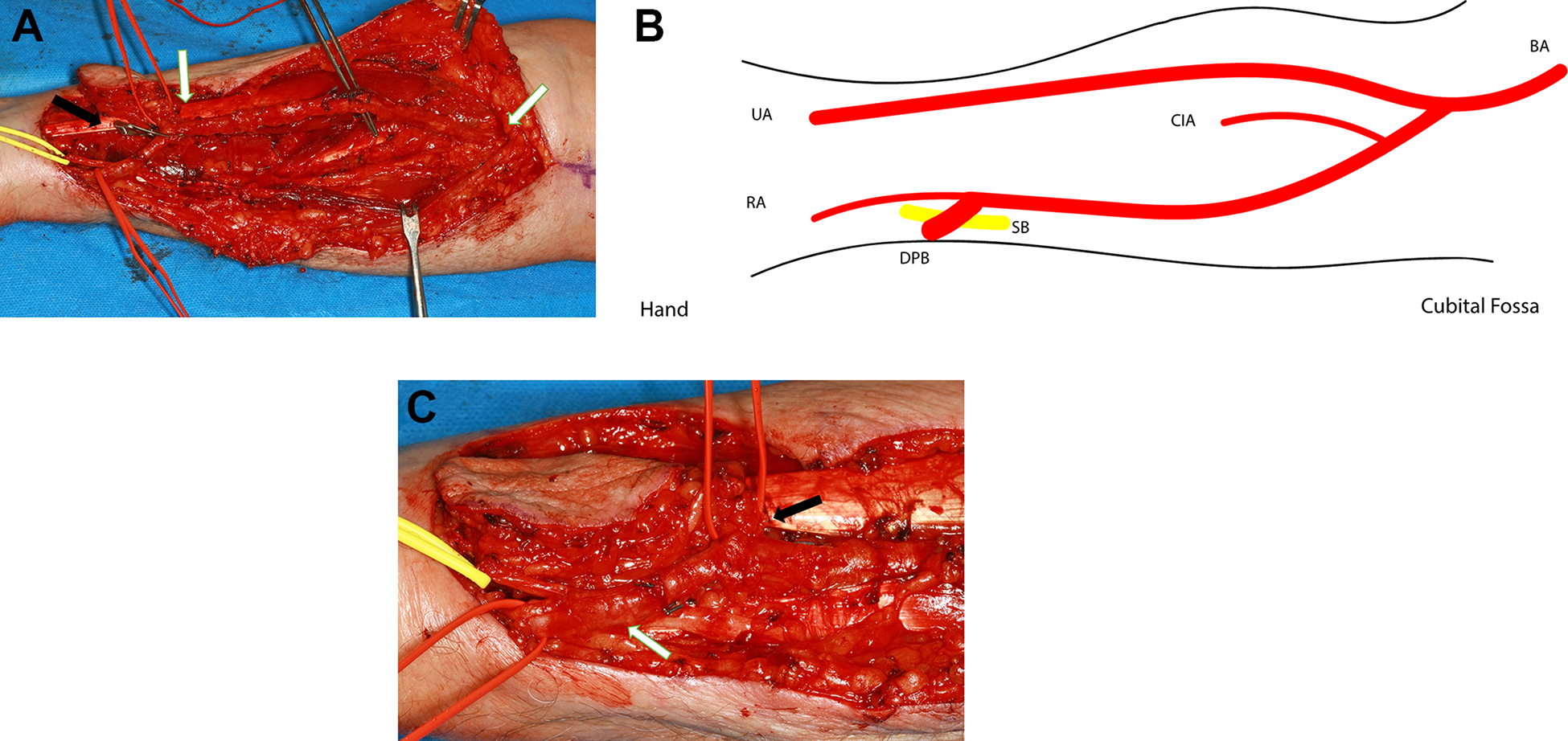
Discussion
Distal branching of the radial artery has rarely been described in the literature and can potentially interfere with the raising of the RFF. On the other hand, anatomical variations of the arterial system of the forearm occur more frequently. The typical distal branching of the brachial artery can only be found in 70% of the cases, where the bifurcation is usually located 1 cm distal to the antecubital fossa. 12 Since most variations occur at the origin of the radial artery, it is important to follow the radial artery to the brachial artery before any branches are ligated. 12 Here, a high origin of the radial artery is the most frequent variation, 8,9 which should not compromise the flap raising. Besides that, the most commonly described variations in the literature are a superficial dorsal antebrachial artery and duplication of the radial artery, 8,12,14 which also do not interfere with the flap raising.
The unusual branching of the radial artery in the present case was first discovered intraoperatively, and made the extension of the skin paddle difficult to determine. The radial artery could be palpated regularly at the wrist level, and a preoperatively performed Allen’s test showed no irregularities. The deep palmar branch (DPB) was discovered after the radial incision had been made and preparation of the skin paddle had been performed. The branch ran from the dorsal side of the forearm crossing the superficial radial nerve (Figure 1C). At this stage, an extension of the skin paddle and an inclusion of the DPB was impossible. The DPB was clamped to ensure a sufficient blood supply to the hand and to the skin paddle. After an adequate perfusion of the hand and the skin paddle could be confirmed, the deep palmar branch was ligated. The case demonstrates the importance of caution with large arterial branches during flap raising in patients with vascular variations before the dissection is completed. Otherwise, there is a risk of inadequate blood circulation, which can have severe negative consequences for the patient. 13
Due to the high reliability of the arterial system, a negative Allen’s test result is considered sufficient preoperatively. 2,12,15 The Allen’s test is a good and valid screening test for the arterial blood flow of the hand, but it cannot provide reliable predictions concerning the vascular anatomy of the forearm/hand. 10,16 In case of a pathological Allen’s test, preoperative plethysmography and Doppler ultrasonography scanning are recommended. 16 In the present case, it might have been possible to palpate the DPB preoperatively while carrying out the Allen’s test. In this case, further diagnostics could have been performed, as recommended in other studies 12,16 to verify the potential anatomic variation preoperatively and adjust the flap design or consider an alternative flap. Breik et al presented a similar case with anomalous distal branching of the radial artery into the deep palmar branch. 12 Along with the challenge of determining the skin paddle, the securing of the skin paddle perfusion was highlighted. These 2 factors were also our main concerns during the flap raising. Since no restrictions in flap perfusion and/or hand perfusion were observed in our case, we recommend RFF raising in the traditional way. No changes concerning the design and the positioning of the skin paddle should be made.
In conclusion, prior to microsurgical reconstruction with an RFF, surgeons should be aware of possible anatomical variations of the radial artery and the resulting flap design. Additionally, in case of an anatomical variation, the dissection of the pedicle should be completed, and the arterial branch should be clamped to prevent poor blood circulation to the hand/skin paddle before dividing any large branches of the radial artery.
Footnotes
Acknowledgement
We thank Franz Hafner for his photographic documentation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient’s Consent
Written consent from the patient was obtained in order to include the photographs in the publication.
