Abstract
Study Design
Descriptive cross-sectional study.
Objective
The mandibular canal (MC) exhibits surgically significant anatomical variations in its course and terminal segment among different ethnic groups. The aim of this study was to document a surgically relevant position of the MC, its variants, and related anatomical structures in dentate patients from a select Kenyan population.
Methods
351 hemi mandibular cone-beam computed tomography (CBCT) scans from 202 patients were used to evaluate the MC and mental foramen (MF) for normal morphology, anatomical variations, and their linear relationship to various reference points.
Results
The most frequently encountered course of the MC was the progressive descent type seen in 241 (68.7%) scans. Accessory MC were observed in 15 (4.3%) scans. Accessory MF were observed in 29 (8.3%) scans. The mean diameter of the MC was 3.36 ± .39 mm. The orientation of the MC was more lingual towards the angle of the mandible and more buccal towards the MF. The most frequent position of the main MF in relation to the second premolar was anterior (53.3%). The average distance from the MF to the inferior border of the mandible was 12.17 ± 1.91 mm. The anterior loop of the mental nerve was observed in 18 (5.1%) scans and its mean length was 4.83 ± .89 mm.
Conclusions
Our study revealed significant variations in the position, size, and course of the MC and MF. This knowledge should assist oral surgeons to avoid inadvertent injury to the inferior alveolar neurovascular bundle in the local population.
Introduction
The mandibular canal (MC) is a bilateral bony channel that originates from the mandibular foramen and runs longitudinally towards the mental foramen (MF). It serves as a conduit for the inferior alveolar neurovascular bundle (IANB). 1 In its course, it relates to the roots of the mandibular premolars and molars.
Inadvertent IANB injury has been reported in various fields of dentistry including orthodontics, endodontics, restorative dentistry, and oral and maxillofacial surgery. 2 An in-depth understanding of the intraosseous course and position of the neurovascular bundle is a prerequisite to performing mandibular surgical procedures. These procedures include but are not limited to dental implant placement, third molar surgery, bilateral sagittal split ramus osteotomy (BSSRO), bone grafting, placement of fracture fixation screws, and mandibular jaw resection. 3
Various studies have tried to map out the course of the MC in their populations essentially to form a guide to surgical approaches to the mandible.4,5 The intraosseous pathway of the MC has been reported as lingual to the roots of the third and second molars, below the roots of the first molar, and buccal to the premolar roots. 6 Worthington 7 described 3 configurations of the MC; a straight projection, a progressive curve, and a catenary-like canal. The MF is most commonly found below the second premolar in line with its longitudinal axis and less commonly located between the premolars. 8 The prevalence of accessory MC has been reported to range from .08% to 43.0%. 9
The anterior loop of the mental nerve (ALMN) is the anterior and inferior extension beyond the MF of the IAN and its curving back to the MF forming a loop. 10 The identification of this benign anatomical variation is essential for surgical planning, especially for the placement of dental implants in the mental foramen region. This will help to prevent iatrogenic injury to the mental nerve and to ensure effective surgery in this region. 10 The prevalence of ALMN has been reported to range from 0% 11 to 88%. 12 A maximum length of 11 mm has been reported. 12
CBCT scans are accurate three-dimension (3D) imaging modality of dental and maxillofacial structures without magnification or superimposition. The images of maxillofacial structures produced are undistorted and of high resolution. There are many planes for reformatting the images that allow for interactive viewing. Significantly fewer radiation doses are involved in taking CBCT scans, compared to conventional medical-grade computed tomography scans. 13 These factors make CBCT scans the most appropriate investigative tool for this study.
Materials and Methods
The data used in this descriptive cross-sectional study was obtained from a private imaging facility called Dental and Maxillofacial Imaging Centre (DAMIC) located in Nairobi, Kenya with approval from the Kenyatta National Hospital/University of Nairobi Ethics, Research and Standards committee. Consecutive sampling was used to select a sample of 351 hemi CBCT scans from 202 patients from DAMIC’s electronic database.
Inclusion Criteria
1. Age >20 years old. 2. Full mandibular arch CBCT scan. 3. Presence of at least 2 of the following 3 teeth: second premolar, first molar, and second molar.
Exclusion Criteria
1. Presence of supernumerary teeth, bone pathology, impacted teeth, or fractures obscuring visualization in the region of interest or changing the position of the MC or MF.
All images had been acquired using a CS 9300® CBCT unit (Carestream Dental, Carestream Health Inc 150 Verona St Rochester NY 14608, USA) with a thin film transistor sensor and charge-coupled device detector technology. The jaw program pane selected was single jaw full acquisition (10 × 5 cm) for lower jaw exam and voxel size of 180 μm. The set tube current and voltage were 4 milliamperes (mA) and 85 or 90 kilovoltage (kV) respectively. The CBCT unit height had been adjusted and a chin guide utilized while scanning to ensure that the occlusal plane was horizontal. The detector completed a full scan of the patient’s head in an average of 8.01 seconds. CS Imaging software (Carestream Dental, Carestream Health Inc 150 Verona St Rochester NY 14608, USA) was used to capture, process, and store the original two-dimension (2D) projection views and the reconstructed 3D data.
This data was retrieved from DAMIC’s electronic database and used to reconstruct and analyze each jaw in the orthogonal plane using a computer CS 3D visualization and measurement software. The variables of the study were assessed, and attention given to the selected reference points for purposes of standardization. Both sides of the mandible were studied independently. Patient contact and consent were not required for this study. The parameters assessed included: 1. The topographical course of the mandibular canal according to the Worthington classification 2. The diameter of the MC 3. The distance between the MC and the buccal cortical plate (BCP), lingual cortical plate (LCP), inferior border of the mandible (IBM), second premolar root apex, first molar distal root apex, and second molar distal root apex 4. The presence of accessory mandibular canals and accessory mental foramina 5. The position of the main mental foramen in relation to the second premolar 6. The presence and length of the anterior loop of the mental nerve
Data Analysis
Categorical variables were summarized using percentages and frequencies while continuous variables were summarized using the mean and standard deviation. Independent samples t test and chi-square test were used to analyze the distance between the MC and the BCP, LCP, IBM, root apex of the second premolar, distal root apex of the molar and distal root apex of the second molar to determine whether there was a statistically significant difference between males and females. A P-value <.05 was considered statistically significant.
Minimizing Errors and Biases
All measurements on the sampled CBCT images were carried out in the orthogonal plane by the principal investigator after training, familiarization, and calibration in manipulating the software and taking morphometric measurements by an oral and maxillofacial radiologist. To assess inter-observer variability, every 35th CBCT image had repeat morphometric measurements done by the radiologist. An overall intraclass correlation coefficient (ICC) of .989 (P < .001) demonstrated excellent agreement of the measurements for inter-observer variability.
Results
A total of 351 hemi mandibular CBCT scans from 202 patients were retrieved and included in this study. 142 scans were from 81 (40.1%) male and 209 scans were from 121 (59.9%) female patients giving a male to female ratio was .7:1. The mean age was 40.4 ± 14.2 years with an age range from 20 to74 years. The median age was 39 years (IQR 28.0 – 50.0). There were 180 (51.3%) right side and 171 (48.7%) left side scans.
In assessing the course of the MC, the progressive descent type was seen in 241 (68.7%) scans, the catenary-like type in 77 (21.9%) scans, and the straight projection type in 33 (9.4%) scans (Figure 1). Sample images from the study showing CBCT reconstructions of the mandible with nerve tracings showing variations in the course of MC observed: A – Progressive descent, B – Catenary-like, C – Straight projection.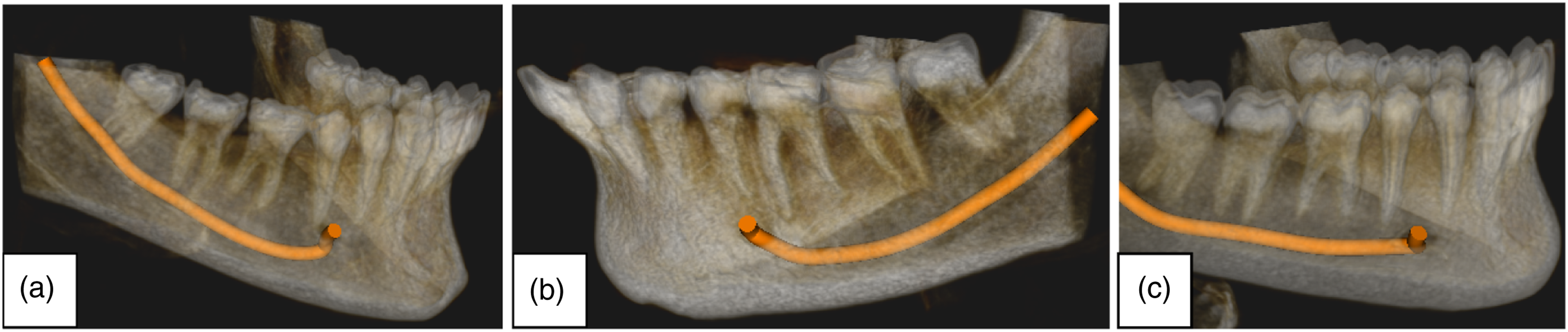
Chi-square analysis showed no statistically significant difference in the occurrence of the 3 courses of the MC between the genders (catenary-like P = .176, progressive descent P = .906, straight projection P = .083).
Accessory MC were observed in 15 (4.3%) CBCT scans (Figure 2). Of these 5 (33.3%) were males and 10 (66.7%) were females. The probability of this observation was not statistically significant (χ
2
, df, P = .330, 1, .566). Sample images from the study showing CBCT reconstructions of A – Right mandible and B – Left mandible demonstrating accessory MCs observed.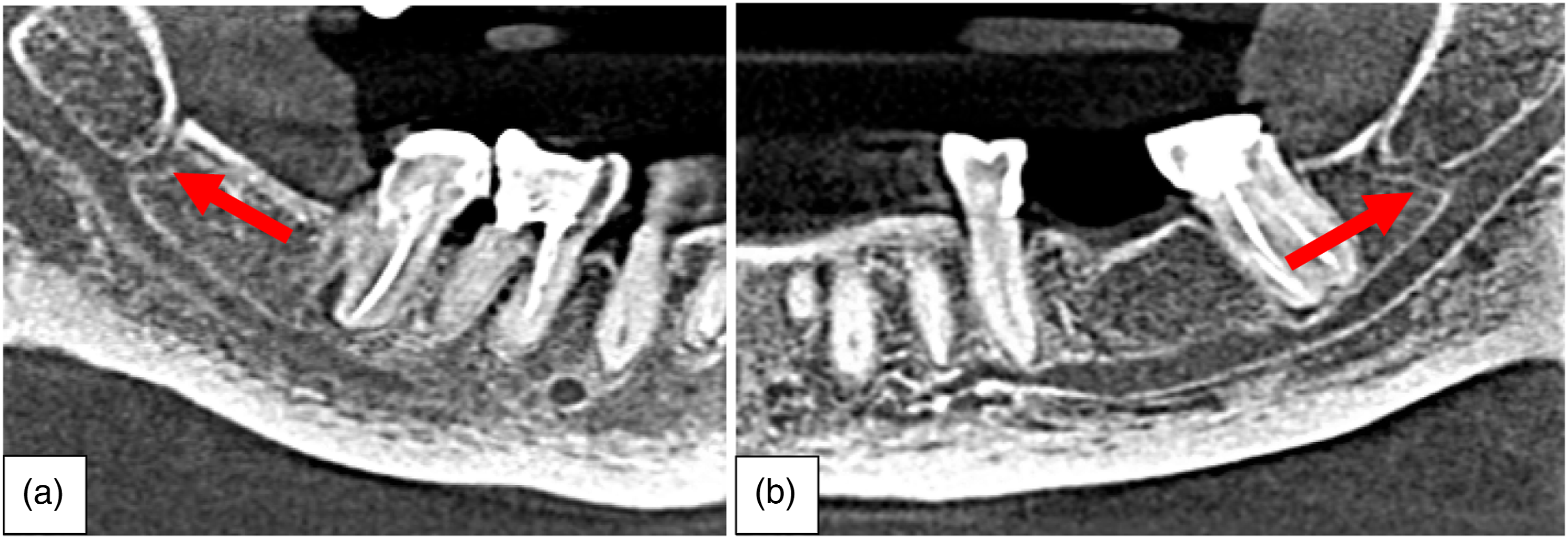
Accessory MF were observed in 29 (8.3%) scans (Figure 3). Of these, 11 (37.9%) were males and 18 (62.1%) were females. The probability of this observation was assessed using chi-square test and no statistically significant difference was found (χ
2
, df, P = .084, 1, .772). Sample images from the study showing CBCT reconstructions of the mandible demonstrating the main MF and accessory MF observed.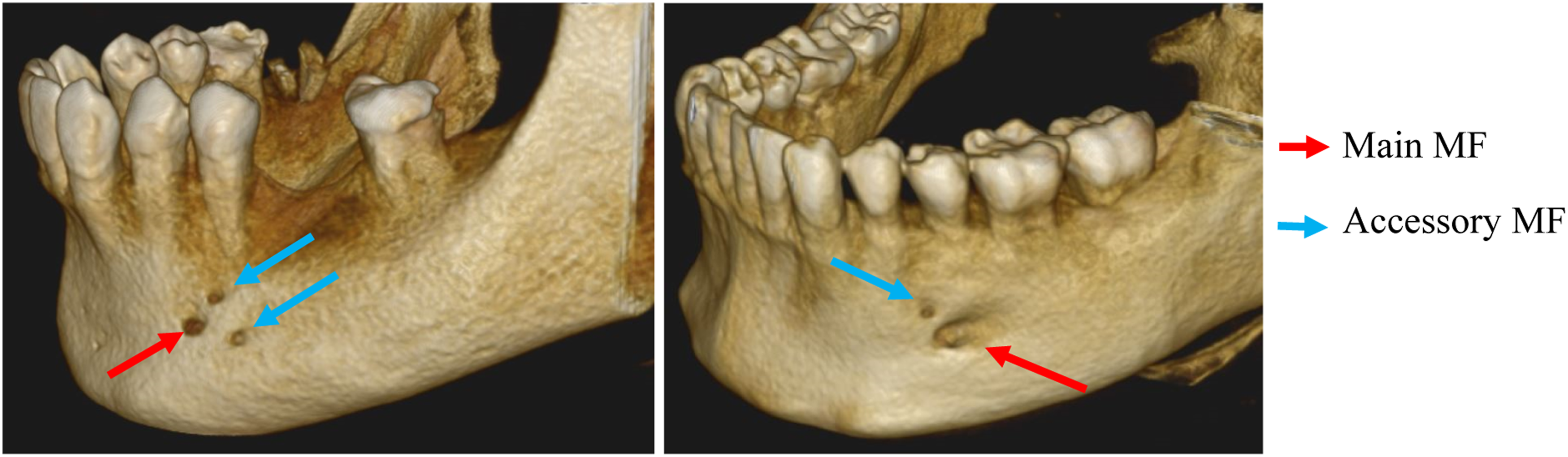
Only 1 CBCT scan showed both accessory MC and accessory MF in the same patient. This finding was not statistically significant (χ 2 , df, P = .053, 1, 1.000).
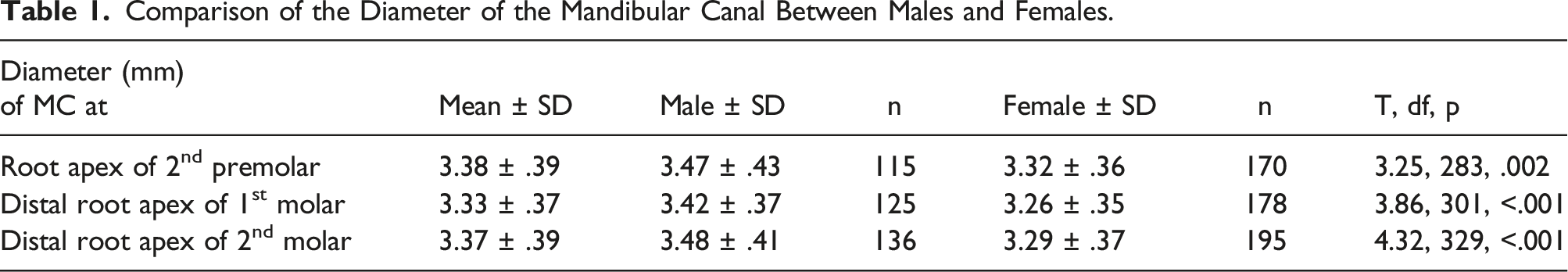
The diameter of the MC was 3.38 ± .39 mm at the root apex of the second premolar, 3.33 ± .37 mm at the distal root apex of the first molar, and 3.37 ± .39 mm at the distal root apex of the second molar (Figure 4). The overall mean diameter was 3.36 ± .39 mm. It was greater in males at all the reference points, a finding that was statistically significant at all 3 points (Table 1). Sample images from the study showing the diameter of the MC as measured at A – second premolar root apex, B – first molar distal root apex, and C – second molar distal root apex. Comparison of the Diameter of the Mandibular Canal Between Males and Females.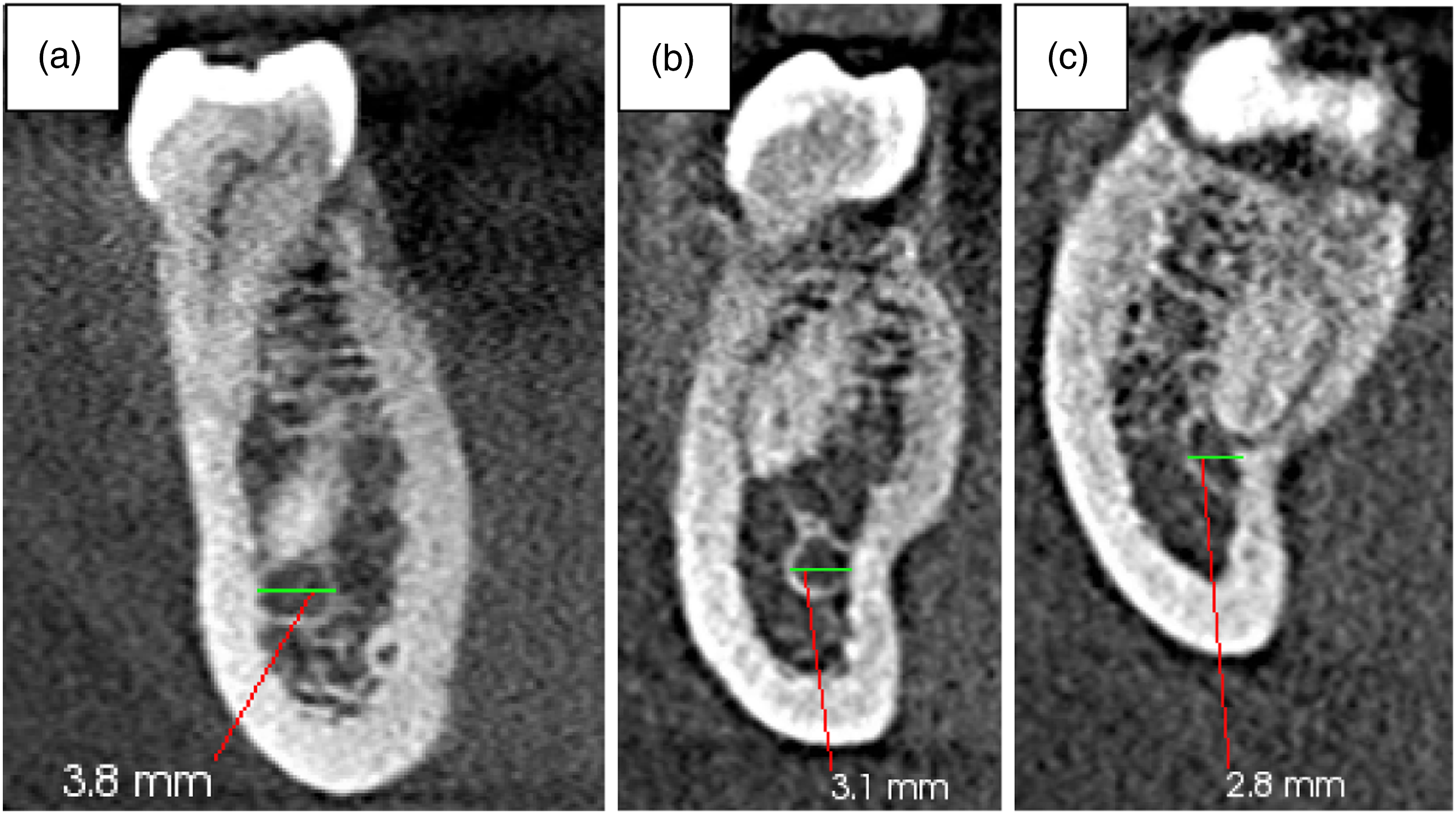
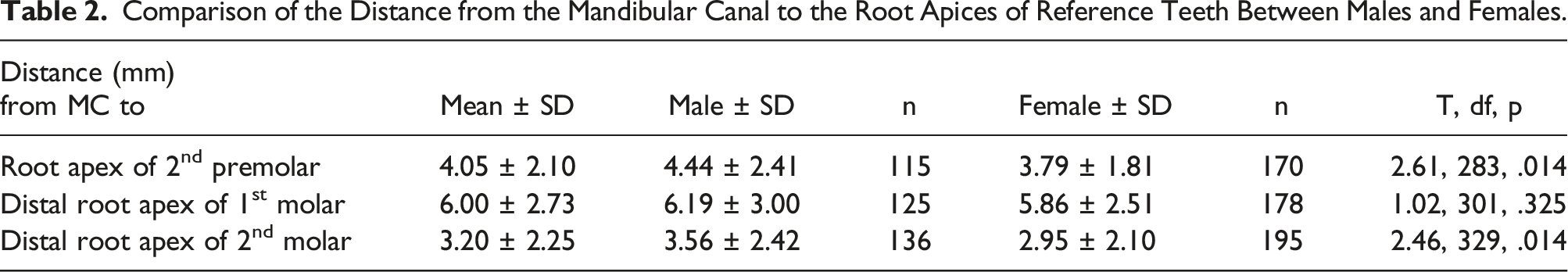
The mean distance between the MC and the root apices of reference teeth was 4.05 ± 2.10 mm at the root apex of the second premolar, 6.00 ± 2.73 mm at the distal root apex of the first molar and 3.20 ± 2.25 mm at the distal root apex of the second molar (Figure 5). This distance was longer in males at all reference points, a finding that was statistically significant at the root apex of the second premolar and the distal root apex of the second molar (Table 2) Sample images from the study showing the distance as measured from the MC to A – second premolar root apex, B – first molar distal root apex, and C – second molar distal root apex. Comparison of the Distance from the Mandibular Canal to the Root Apices of Reference Teeth Between Males and Females.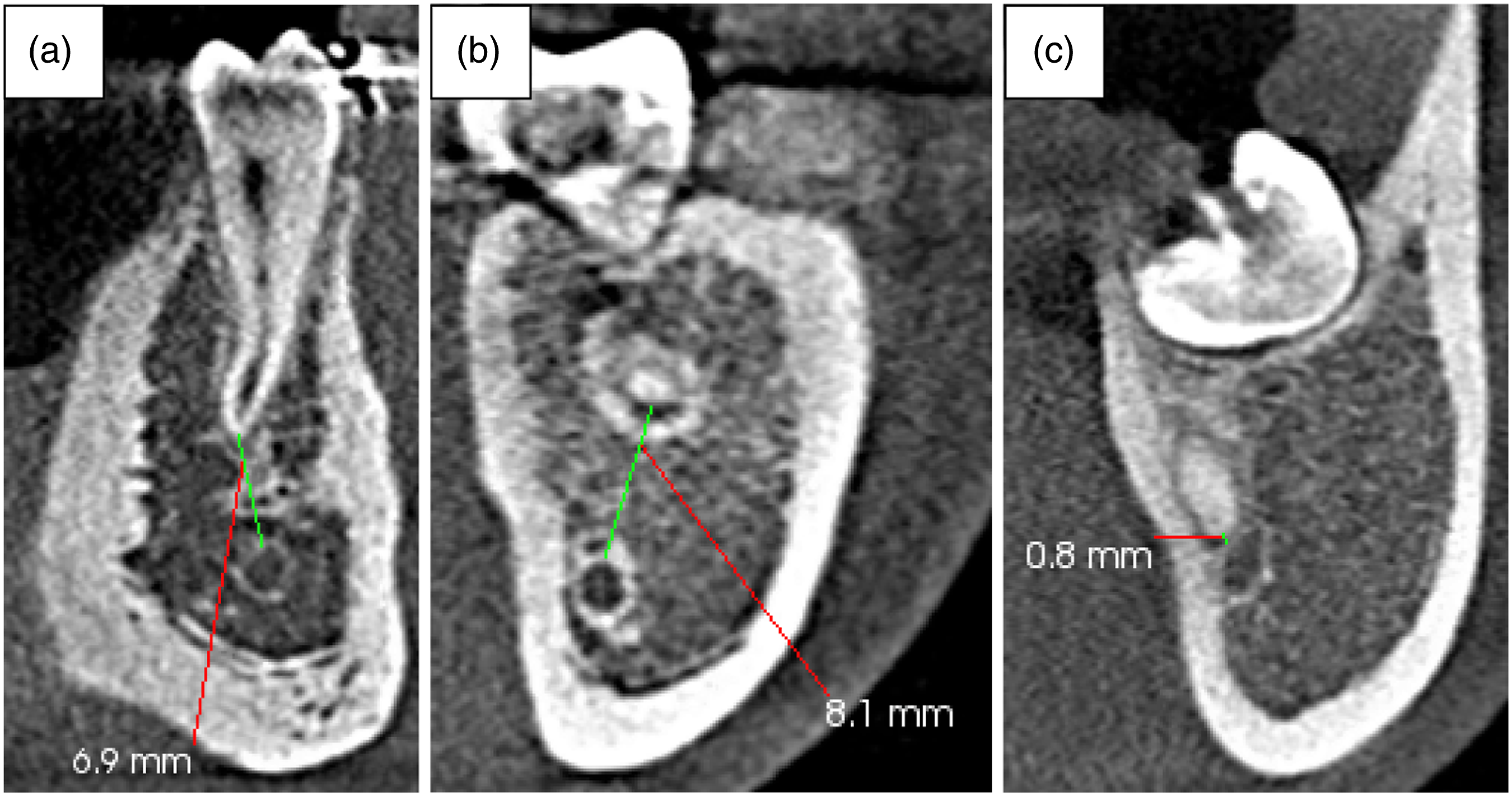

The mean distance between the MC and BCP was 4.24 ± 1.51 mm at the root apex of the second premolar, 6.36 ± 1.75 mm at the distal root apex of the first molar, and 5.94 ± 1.84 mm at the distal root apex of the second molar (Figure 6). This distance was longer in males at all reference points, a finding that was statistically significant at all points (Table 3). Sample images from the study showing the distance as measured from the MC to BCP at A – second premolar root apex, B – first molar distal root apex, and C – second molar distal root apex. Comparison of the Distance from the Mandibular Canal to the Buccal Cortical Plate Between the Genders.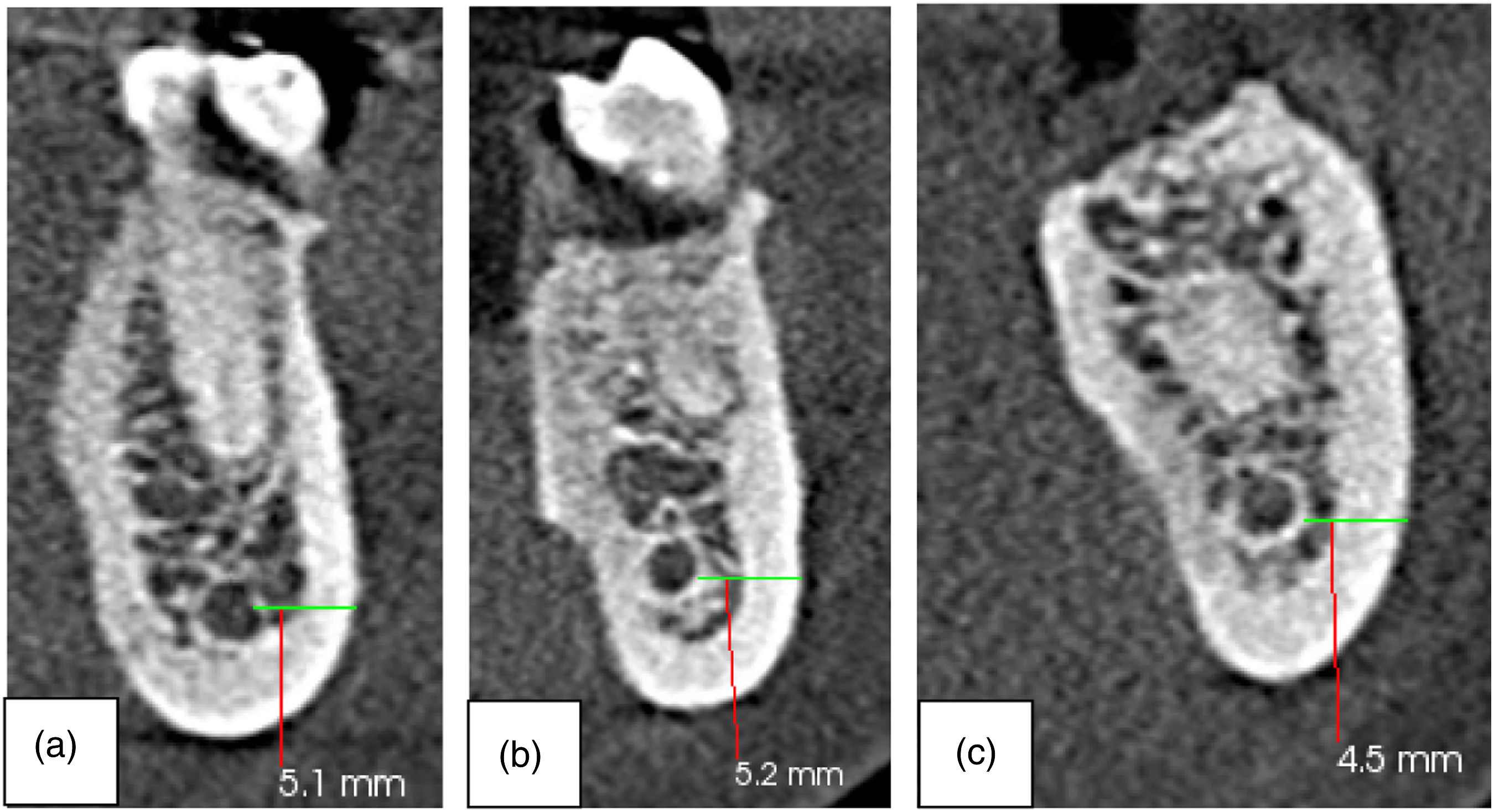

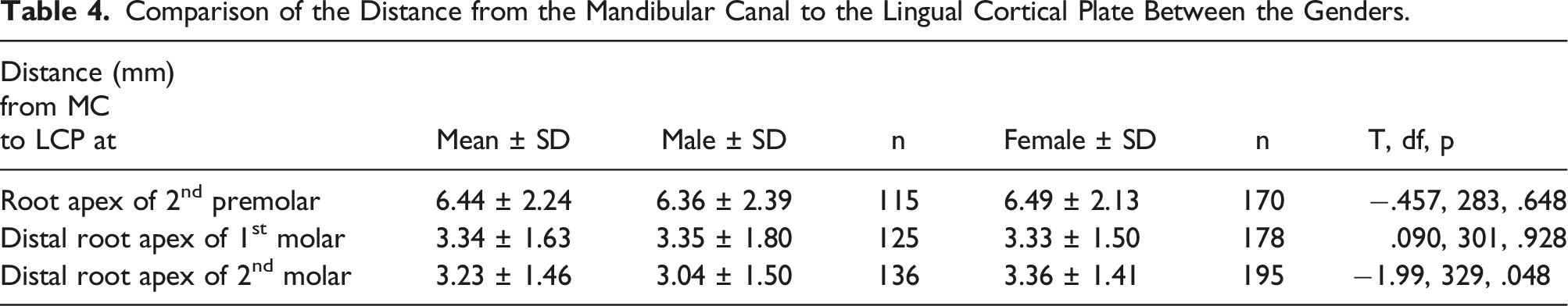
The mean distance between the MC and LCP was 6.44 ± 2.24 mm at the root apex of the second premolar, 3.34 ± 1.63 mm at the distal root apex of the first molar, and 3.23 ± 1.46 mm at the distal root apex of the second molar (Figure 7). This distance was shorter in males than females except at the distal root apex of the first molar. The difference between the genders was statistically significant only at the distal root apex of the second molar (Table 4). Sample images from the study showing the distance as measured from the MC to LCP at A – second premolar root apex, B – first molar distal root apex, and C – second molar distal root apex. Comparison of the Distance from the Mandibular Canal to the Lingual Cortical Plate Between the Genders.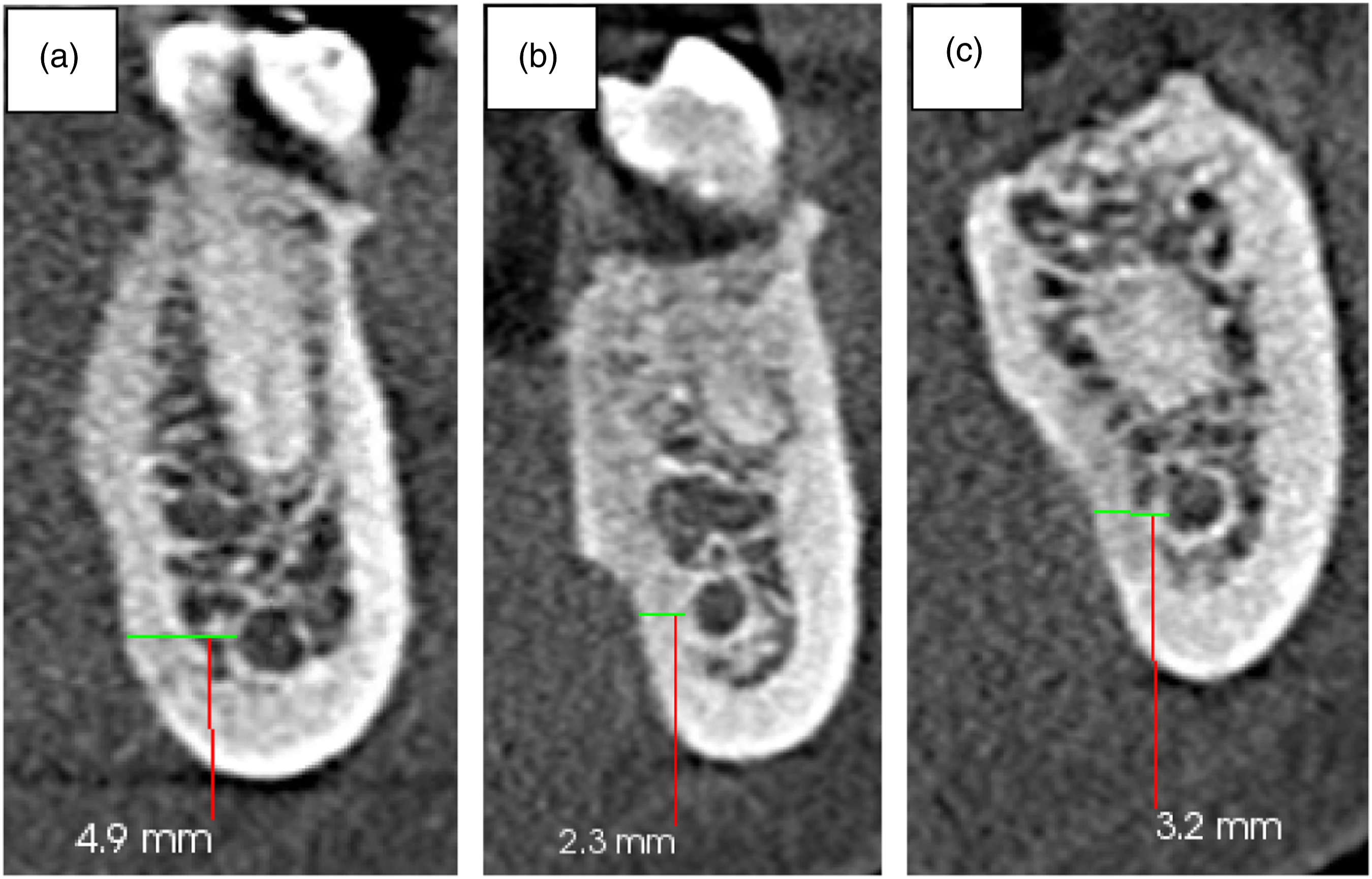

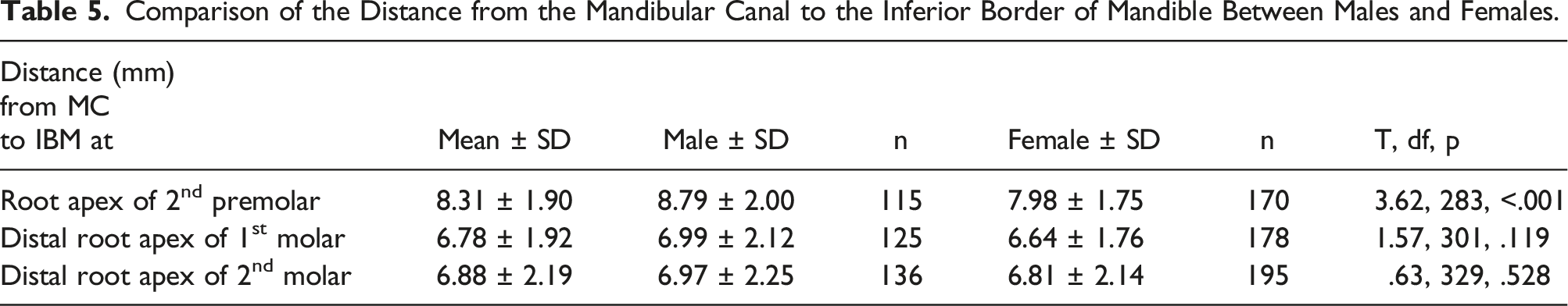
The mean distance between the MC and IBM was 8.31 ± 1.90 mm at the root apex of the second premolar, 6.78 ± 1.92 mm at the distal root apex of the first molar, and 6.88 ± 2.19 mm at the distal root apex of the second molar (Figure 8). This distance was longer in males than females, a finding that was statistically significant only at the root apex of the second premolar (Table 5). Sample images from the study showing the distance as measured from the MC to IBM at A – second premolar root apex. B – first molar distal root apex and C – second molar distal root apex. Comparison of the Distance from the Mandibular Canal to the Inferior Border of Mandible Between Males and Females.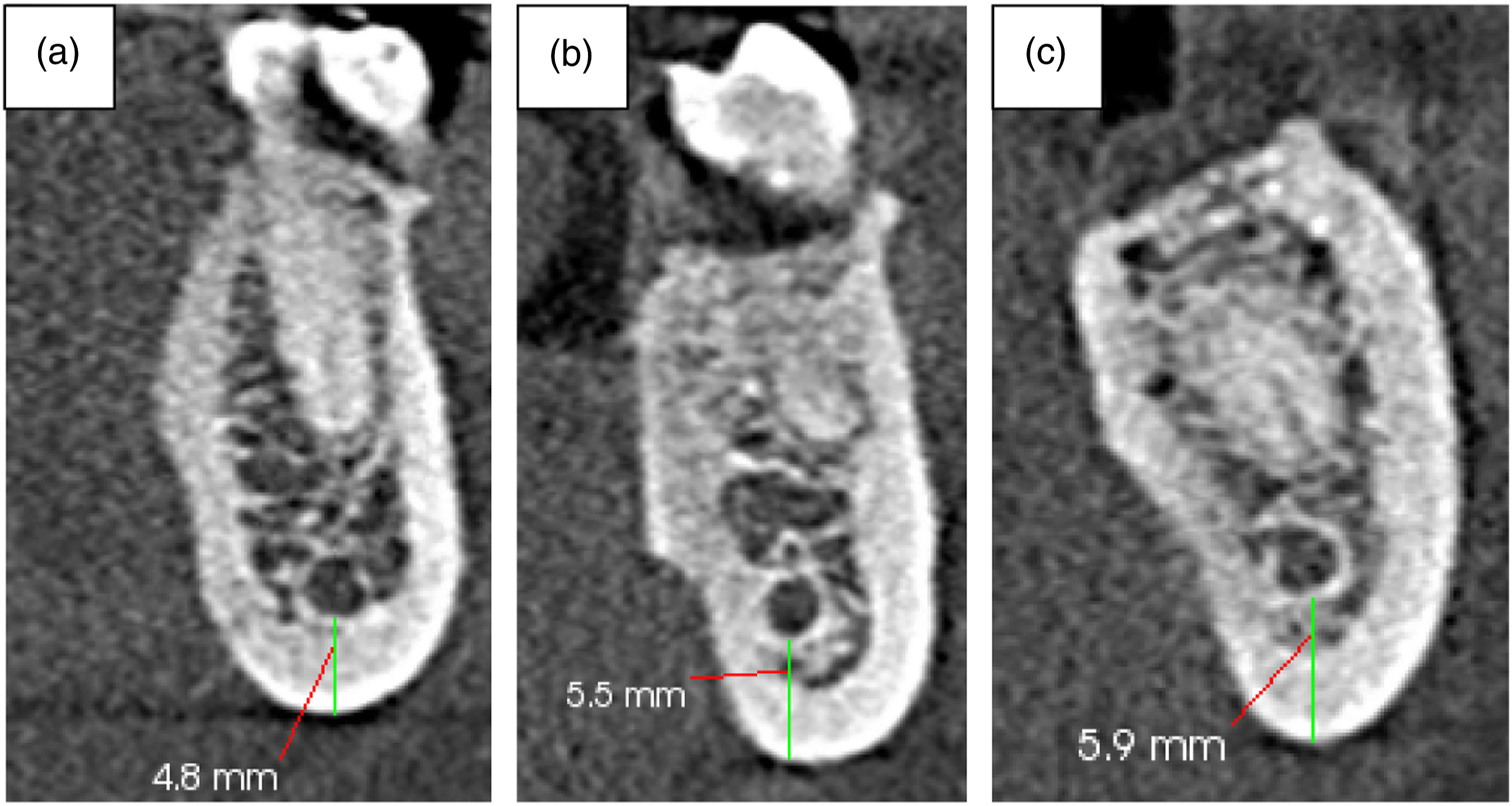

The most frequent position of the main MF in relation to the second premolar was anterior (187, 53.3%), followed by below (121, 34.5%) and the least frequent position was posterior (43, 12.3%) (Figure 9). Chi-square analysis showed no statistically significant difference in the position of the MF in relation to the second premolar between the genders (Anterior P = .166, Below P = .112, Posterior P = .841) Sample images from the study showing the different positions of the main MF in relation to the second premolar observed: A – Anterior, B – Below, C – Posterior.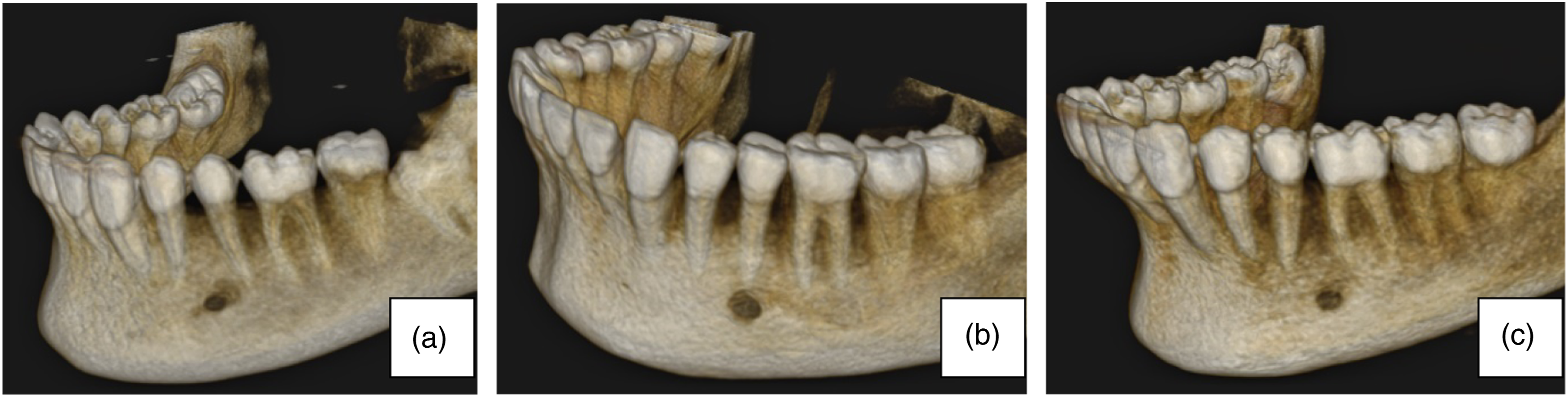
The mean distance between the MF and IBM was 12.17 ± 1.91 mm (Figure 10). This distance was found to be found to be longer in males than females, a finding that was statistically significant (t, df, P = 9.85, 349, <.001). Sample images from the study showing the distance as measured from the MF to the IBM A – Right side, B – Left side.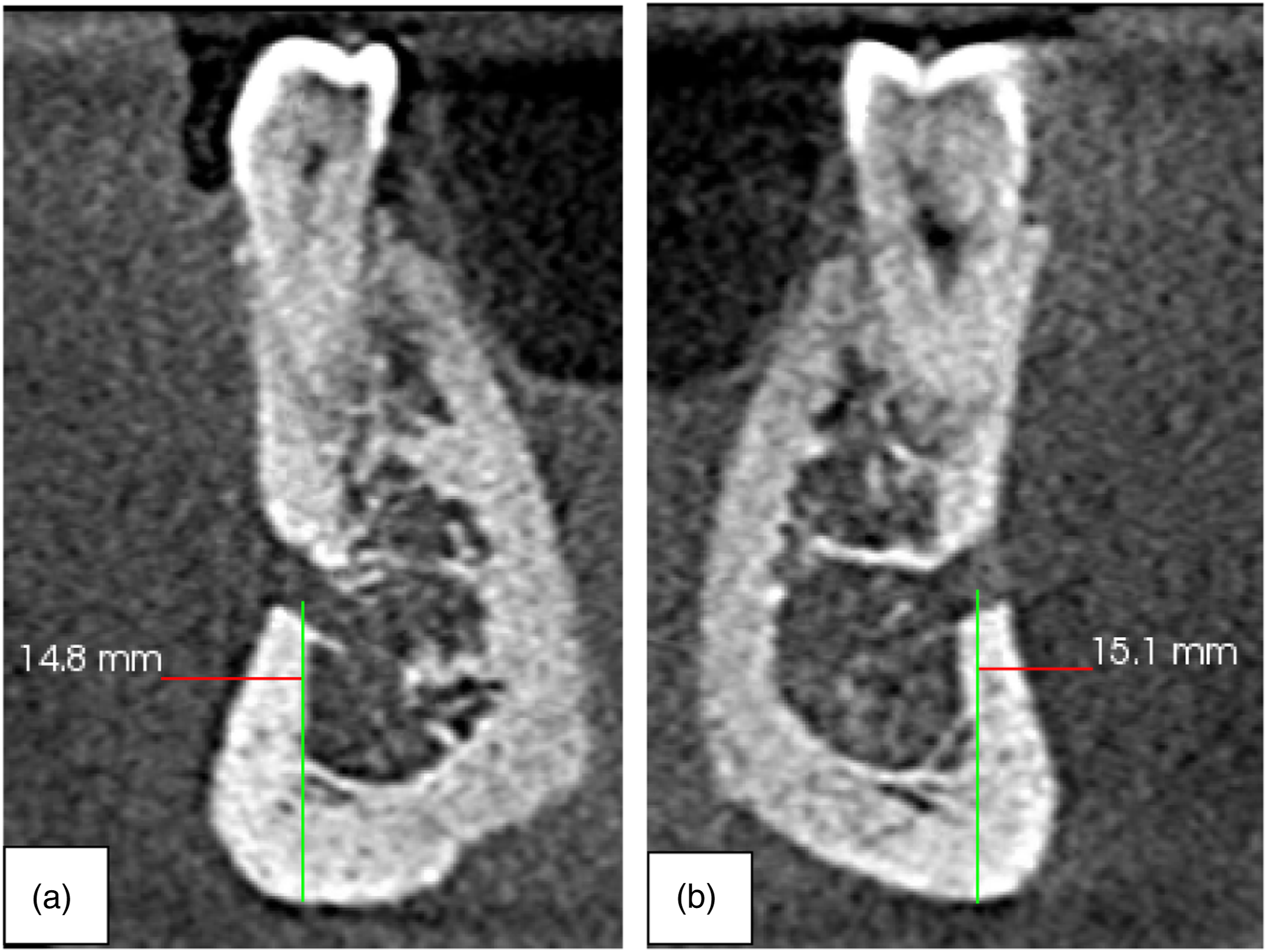
The ALMN was observed in 18 (5.1%) CBCT scans studied (Figure 11). Of these, 6 (33.3%) were male patients and 12 (66.7%) were female patients. The probability of this observation was assessed using chi-square test and no statistically significant difference was found (χ
2
, df, P = .40, 1, .527). The mean length of the ALMN was measured and found to be 4.83 ± .89 mm. There was no statistically significant difference in the length of the ALMN between the genders. Sample images from the study showing CBCT reconstructions of the mandible demonstrating the anterior loop of the mental nerve (ALMN) A – voxel size 180 μm, B – voxel size 7.7 mm.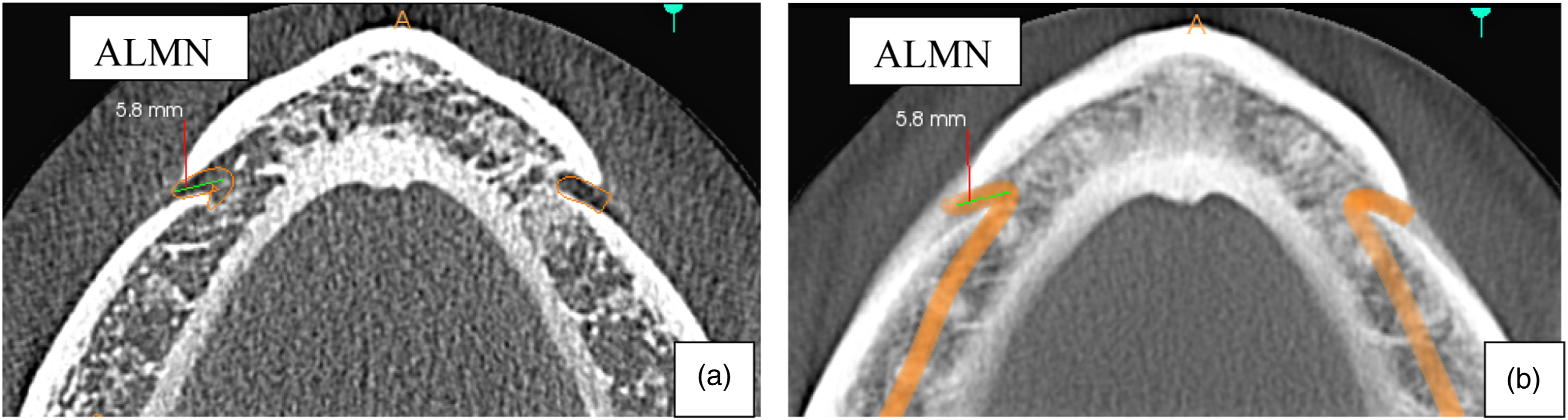
Discussion
Significant anatomical variations of the course of the MC and the terminal segment of the IANB have been reported to various extents among different ethnic groups and populations. In the past, studies on the MC and its variants were limited to cadaver, dry skull and 2D imaging studies. The limitations of these techniques are well documented. CBCT studies of the MC represent a relatively new area of research, and most studies have been conducted in the last few years. Increased interest in this subject has been driven by greater frequency of placement of endosseous dental implants, advanced orthognathic surgery procedures, and the need to avoid morbidity associated with IANB injury during surgical procedures
The most frequently observed course of the MC was the progressive descent type, a finding similar to that from a Nepalese study of 150 CBCT scans. 14 The progressive descent type is not favorable for placement of implants in the second M region as the MC is closest to the root apices and at risk of inadvertent encroachment. The catenary-like type provides the most amount of space for implant placement especially in the first molar region while the straight projection type is the least favorable for placement of implants posterior to the MF. Similar to this study, Mirbeigi 6 found no relationship between gender and the pattern of the MC course.
The Prevalence of Bifid and Trifid Mandibular Canals in Literature.
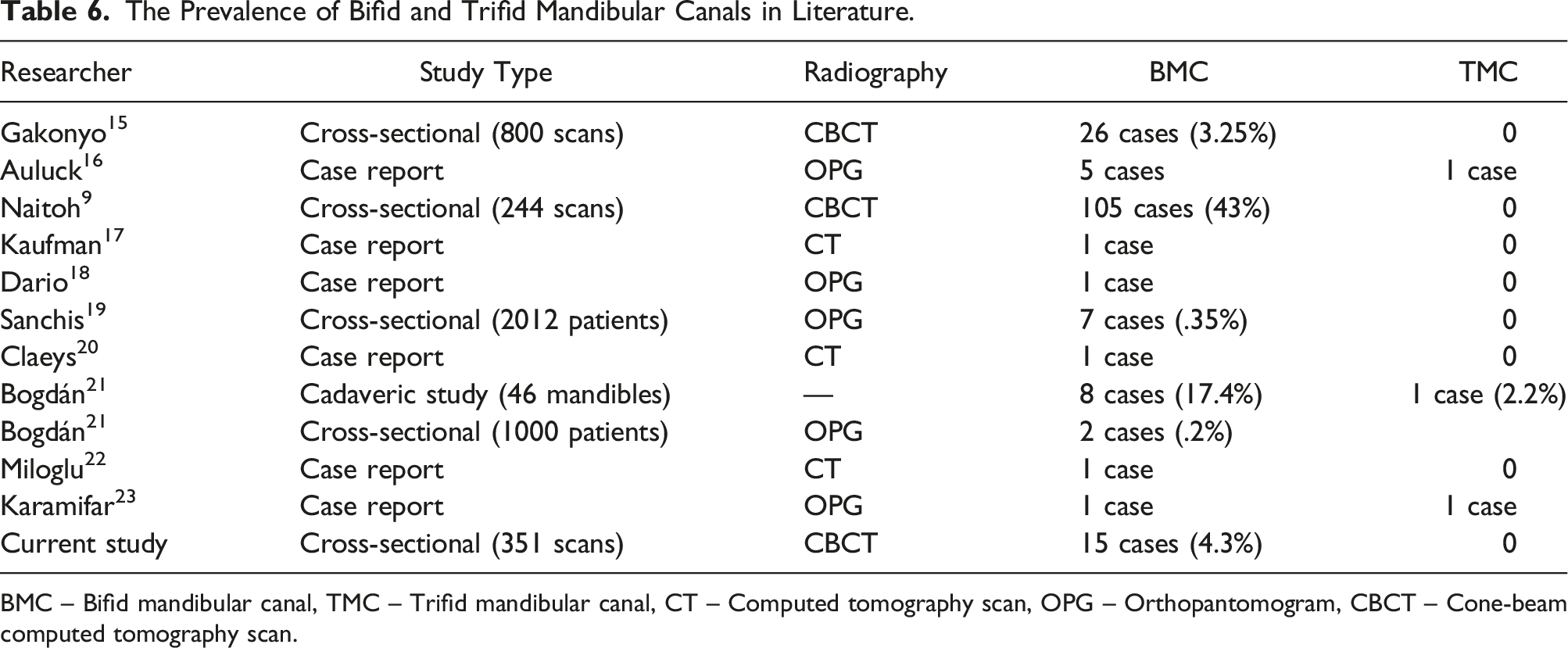
BMC – Bifid mandibular canal, TMC – Trifid mandibular canal, CT – Computed tomography scan, OPG – Orthopantomogram, CBCT – Cone-beam computed tomography scan.
Prevalence of Accessory MF in Literature.

MF – Mental Foramen.
Ikeda 27 reported the average diameter of the MC to be 3.4 mm, findings in line with this study at 3.36 mm. In contrast, Hamid 28 reported smaller mean diameters of 2.7 mm on CT scan measurement and 2.9 mm on electronic digital calipers measurement of sections of 5 adult Sudanese cadaveric mandibles. The variance from the current study could be attributed to the cadaver mandibles undergoing some degree of shrinkage resulting in the smaller values. Differences in body sizes between the populations considered may also be a contributing factor. Several diseases of the bone can affect the MC diameter by increasing or decreasing its size as seen in osteolytic malignant diseases and lesions exhibiting perineural spread. 29 Any changes in the diameter of the MC in a cancer patient should be considered when planning resection margins. Knowledge of the average diameter of the normal MC will help in detecting any abnormal changes in its size, further underscoring the importance of this study.
The findings from this study on the distance of the MC from the root apices of the reference teeth suggest a catenary-like course of the MC. This may imply that morphometric assessment of the course of the MC is more objective than the observational assessment that was done. Further inference from this finding is that longer endosseous implants can be placed in the body of the mandible region compared to the mental and angle of mandible areas. Sharma 25 reported the MC being closest to the roots of the second molar but noted the distance between the MC and periapex of mandibular teeth increased gradually anteriorly with the longest distance being from the periapex of the second premolar. This is consistent with a progressive descent course and may suggest that the difference from the current study constitutes ethnic differences in anatomical structures between the study populations.
The findings from this study are in keeping with other studies in the assertion that the MC orientation is more lingual towards the angle of the mandible and more buccal towards the MF.8,30 The buccolingual orientation of the MC is an important parameter that requires in-depth analysis before BSSRO and monocortical plating. Similarly, the decision to orient an endosseous implant either buccally or lingually to avoid encroachment into the canal is largely dependent on knowledge of the buccolingual thickness of the mandible and the position of the MC.
In this study, the distance between the MC and the IBM progressively increased from posterior to anterior. This finding was consistent between the genders and similar to findings by Shrestha 14 and Nemati. 31 Surgeons must possess a good understanding of the position of the MC relative to the IBM as, during mandibular plating procedures, inappropriate positioning of the plate could lead to encroachment into the MC and neurovascular damage.
The tooth position of the MF provides a quick landmark to the surgeon or anesthetist in identifying the mental nerve and administering a mental nerve block. However, aberrant tooth positions do exist and can lead to failed anesthesia when tooth position is used as the only guide in administering a mental block. Moiseiwitsch 32 in a North American Caucasian population and Mbajiorgu 33 in a black Zimbabwean population concluded that the MF was commonly located anterior to the second premolar, findings in agreement with the current study. On the other hand, Shankland 34 in an Asian Indian population and Oguz 35 in a Turkish population reported that the MF was located most of the time directly below the second premolar. These results indicate ethnic and racial differences in the position of the MF. Surgeons would do well to have epidemiological knowledge of the position of the MF in their local populations. Nonetheless, a radiographic guide remains an important tool in localizing the MF.
The mean distance from the MF to the IBM in this study showed minimal variance from studies by Loyal 36 in a Kenyan cadaveric study, Sheikhi 37 in a CBCT study on an Iranian population, and Neiva 12 in a Caucasian American dry skull study. Further to this, the distance was longer in males than in females, a statistically significant finding. This finding of gender dimorphism in the distance between the MF and IBM agrees with findings from several other studies.37,38 Knowledge of the morphometric relationship of the MF to surrounding landmarks is important in implant surgery especially when the reference teeth or radiographic images are not available.
The prevalence of the ALMN has been reported to range from 0% 11 to 88%. 12 A maximum length of 11 mm 12 has been reported. These findings demonstrate considerable variance from those of the current study. Iatrogenic damage to the ALMN can lead to discomfort of unspecified duration in the lower labial gingiva and lip. Damage rates to the ALMN have been reported in the range of 17 – 38% during genioplasty 39 and 8.5 – 24% when placing implants. 40 Observing a fixed distance anterior to the MF is not safe, and the ALMN length should be determined for each individual to avoid injury to the mental nerve. CBCT scans allow for assessment of the mandible with precision and reliability in determining the presence and length of the ALMN. 41
Limitations
The study was carried out in 1 private CBCT imaging facility thus limiting the ability to use the results to make inferences in the general population. Systemic medical conditions afflicting the patients that could have affected the bone quality and quantity were also not known. Further, the observational nature of the study could not allow for an objective assessment of age changes in the mandibular canal. Lastly, standardization could not be done to the extent of the same radiographer having taken all the CBCT scans rather to all scans having being taken on the same CBCT machine.
Conclusions
Anatomic variations of the MC and related surrounding structures can greatly influence surgical treatment modalities in the mandible. This study will be helpful to surgeons in avoiding inadvertent encroachment in to the MC and injury of the IANB during mandibular surgeries. Considering the limitations of the study, further multicentric CBCT studies should be designed and carried out in the general population to refine these results.
Supplemental Material
Supplemental Material - Morphology and Variant Anatomy of the Mandibular Canal in a Kenyan Population: A Cone-Beam Computed Tomography Study
Supplemental Material for Morphology and Variant Anatomy of the Mandibular Canal in a Kenyan Population: A Cone-Beam Computed Tomography Study by Andrew Okiriamu, Fawzia Butt, Florence Opondo, and Fredrick Onyango in Craniomaxillofacial Research & Innovation
Supplemental Material
Supplemental Material - Morphology and Variant Anatomy of the Mandibular Canal in a Kenyan Population: A Cone-Beam Computed Tomography Study
Supplemental Material for Morphology and Variant Anatomy of the Mandibular Canal in a Kenyan Population: A Cone-Beam Computed Tomography Study by Andrew Okiriamu, Fawzia Butt, Florence Opondo, and Fredrick Onyango in Craniomaxillofacial Research & Innovation
Footnotes
Acknowledgments
We wish to express our gratitude to Mr Wycliffe Ayieko of the University of Nairobi, Public Health department, for carrying out all the statistical analysis in this research. We would also like to thank the management at Dental and Maxillofacial Imaging Centre (DAMIC) Nairobi for allowing us to use data from their electronic database in this research.
Declaration of conflicting interests
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
