Abstract
Background:
Kaposi’s sarcoma is a common malignancy in HIV patients. Oral manifestation of AIDS-associated Kaposi’s sarcoma occurs in up to 65% of HIV/AIDS patients and is a poor prognostic factor. We report the case of a patient with a progressive bulky manifestation of oral Kaposi’s sarcoma.
Case Presentation:
A 48-year-old male presented with dysphagia due to progressive indolent swelling of the palate. Intraoral inspection revealed an uneven, partially ulcerated, livid mass, approximately 5 cm in diameter, extending antero-posteriorly from the superior vestibulum to the soft palate and across the hard palate, thereby overgrowing remaining teeth and the alveolar arch. Serological testing revealed an HIV infection, and further tests showed HHV8-positivity. The patient underwent surgical debulking of the oral lesions and, following complete remission, received full mouth reconstruction with an implant-supported prosthesis.
Conclusions:
Understanding the relation of HIV and HHV8-infection in terms of disease onset and clinical presentation is important to increase awareness of oral Kaposi’s sarcoma and ensure subsequent appropriate management of affected patients. Clinical staging represents the most important factor for choosing the optimal treatment. The introduction of combined antiretroviral therapy has proven to be efficient in curing oral Kaposi’s sarcoma, while several additional locoregional treatment options, including debulking surgery, may be necessary for symptom relief or to improve cosmesis. Radiotherapy should be applied restrictively due to potentially severe toxic mucosal reactions, whereas additional chemotherapy must be considered in severe cases that present with widespread disseminated disease. A multidisciplinary approach to the treatment of functionally and aesthetically impairing oral Kaposi’s sarcoma is highly recommended.
Keywords
Background
Kaposi’s sarcoma (KS) is the most common neoplasm of people who live with human immunodeficiency virus (HIV) today. Caused by human herpes virus 8 (HHV8) infections, it is a multifocal proliferative condition that can be subdivided into 4 clinical presentations: classic KS, endemic KS (African), iatrogenic KS (immunosuppression-/transplant-associated), and epidemic KS (HIV-related), an acquired immunodeficiency syndrome (AIDS)-defining condition. While the transmission of HHV8 in endemic areas can occur horizontally from mother to child, 1 it remains unclear how the transmission of HHV8 occurs in the epidemic setting, and several hypotheses have been postulated in the past: transmission via saliva, 2 via the fecal-oral route, 3 or via sexual intercourse. 4
Although widespread use of combined antiretroviral therapy (cART) has led to a marked decrease in its incidence, KS still represents one of the most common malignancies in HIV patients. Oral manifestation of AIDS-associated KS occurs in up to 65% of HIV patients and is a poor prognostic factor. This article gives an overview of current management options for HIV-associated KS patients and reports the case of a 48-year old patient with progressive bulky manifestation of oral KS. The patient underwent surgical debulking of the oral lesions and was started on cART. Following complete remission, he received full mouth reconstruction with implant-supported prosthesis.
Case Presentation
Ethical approval was obtained from the ethics committee Nordwest and Central Switzerland to report a KS case with literature review to describe the dignity and differential diagnosis of this entity. Written informed consent was obtained from the patient for the publication of the case description and photo material.
A 48-year-old male presented at the emergency department of our hospital with dysphagia due to progressive, indolent swelling of the palate. Some weeks ago, purulent discharge from both ears led to the diagnosis of acute otitis media and was treated by his family doctor. Under antibiotic treatment with Amoxicillin/Clavulanic acid, the patient concomitantly developed high fevers, a presumably allergic skin reaction, and gross, livid-bluish, slowly growing skin lesions in the oral cavity, on his upper lip, and his neck, and later in course in his groin area and left calf. The patient had no significant family or past medical history and, apart from the ongoing antibiotic therapy, did not take any medication, and denied alcohol or tobacco abuse. On physical examination, he was well oriented and appeared to be in good physical condition. Local findings included palpable, enlarged, submandibular, and supraclavicular lymph nodes. Intraoral inspection revealed an impressive, uneven, partially ulcerated, livid mass, which was approximately 5 cm in diameter, extending antero-posteriorly from the superior vestibulum to the soft palate and across the hard palate, thereby overgrowing remaining teeth and the alveolar arch (Figure 1A). The tongue was moist without any coating. The upper lip was notably protruding due to the underlying neoplasia and demonstrated a livid, extraoral skin lesion measuring approximately 0.5 cm in diameter. Three additional cutaneous lesions of the same kind were found in the retroauricular, supraclavicular, temporal, and inguinal regions, as well as on his right calf.
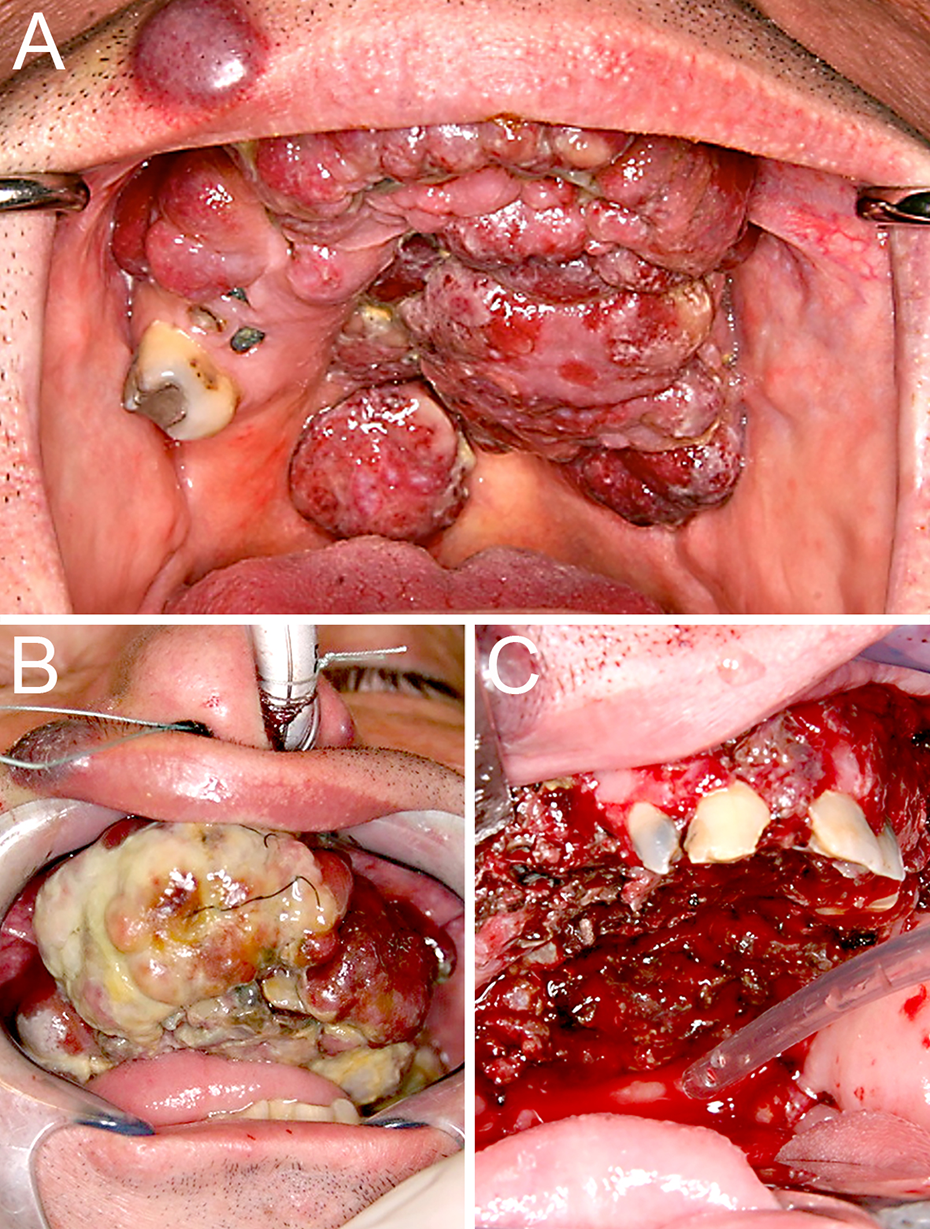
Initial presentation and during inpatient care. A. Oral KS extending antero-posteriorly from the superior vestibule to the soft palate, with areas overgrowing normal dentition. Cutaneous tumor involvement of the upper lip, of retroauricular, supraclavicular, temporal, and inguinal regions, as well as of the right calf is also observed. B. Picture directly before debulking. After tissue biopsy and hospitalization for a few days, increasing swelling of the palatal tumor. C. intraoperative image after debulking of the tumor.
Laboratory findings were all normal, except for a mild elevation in C-reactive protein levels at 22.6 mg/l (reference <10.0) and a CD4 cell count at 22/µl. Serological testing revealed the diagnosis of an HIV infection with a viral load of 94,462 copies/ml. Further tests showed HHV8-positivity with a viral load of 3252 copies/ml, but were negative for Hepatitis B or C. A PET-CT scan showed increased 5 fludeoxyglucose uptake into respective oral lesions, multiple lymph nodes of head and neck, as well as lymph nodes in the groin and the cecum. Subsequent histological colonoscopic findings as well as biopsies of lymph nodes and oral lesions with further immunohistochemical tests confirmed the diagnosis of KS. The patient was in CDC category C3 (AIDS), and after resistance testing, antiretroviral therapy with Emtricitabine, Tenofovir, and Ritonavir-boosted Lopinavir was started immediately.
Because of an acute airway compromise and impairment in swallowing the patient underwent electrosurgical tumor-debulking of his oral lesions with epiperiosteal complete resection in the superior vestibular regions and volume-reducing resection in the region of the hard and soft palate (Figure 1B and C). To prevent bleeding of highly vascularized oral KS lesions, an electric monopolar cutting loop was used. Small residual tumor nodules in the soft palatal region were left behind with the intention of preserving important anatomical structures, thus preventing functional damage (Figure 1C).
After clean and unremarkable wound healing, the patient was discharged 4 weeks after initial presentation. He was given detailed instructions on the modes of administration and how to continue cART; furthermore, he was educated about his medical condition and the required social behavior associated with AIDS. He was also informed about signs and symptoms of local infection and immune reconstitution inflammatory syndrome, as well as the possible side effects of his prescribed medication that would require immediate medical evaluation.
Follow-up Care, After-treatment, and Secondary Reconstruction
After discharge, the patient had monthly follow-up appointments for 6 months and quarterly thereafter for infectiological as well as oncological check-ups. One month after surgical tumor-debulking, the patient was scheduled for dental and prosthodontic treatment as well as evaluation and surgical planning for full mouth reconstruction. Remaining root tips (Figure 2A) were removed and intermediate dentures were provided. Under cART, the remaining soft palate lesions rapidly shrank in size and eventually regressed completely during the course of treatment. A small root tip remnant demarking regio 23 could be removed uneventfully under local anesthesia in the 1 year follow-up (Figure 3A and B). Two years after initial presentation, infectious disease and immunological examination revealed a fully suppressed HIV load (<20 copies/ml), CD4 counts of 292 cells/µl, negative HHV8 loads, and no evidence of remaining oral, integumental, or inguinal KS lesions. Clinically stable and in complete remission, the patient received full mouth reconstruction by means of an implant-retained complete upper overdenture (LOCATOR® Implant Attachment System; Zest Anchors, Escondido, USA) and mandibular implant-supported single tooth crowns. Bony augmentation in the maxilla was achieved by sinus floor augmentation with anorganic bovine bone (Bio-Oss®; Geistlich, Baden-Baden, Germany) covered by a collagen membrane (Bio-Gide®; Geistlich), and was followed by immediate insertion of 4 maxillary titanium implants (SLActive®, SP, ∅4.1 mm RN; Straumann, Basel, Switzerland). Mandibular bone was sufficiently high and wide to allow for the placement of 4 mandibular implants of the same kind 4 weeks later (Figure 2B). The post treatment results from 2 years after the initial presentation are shown in Figure 4, with the hard palate free of oral KS lesions and 4 maxillary titanium implants (Figure 4A) and the full mouth reconstruction with implant-retained overdenture (Figure 4B).
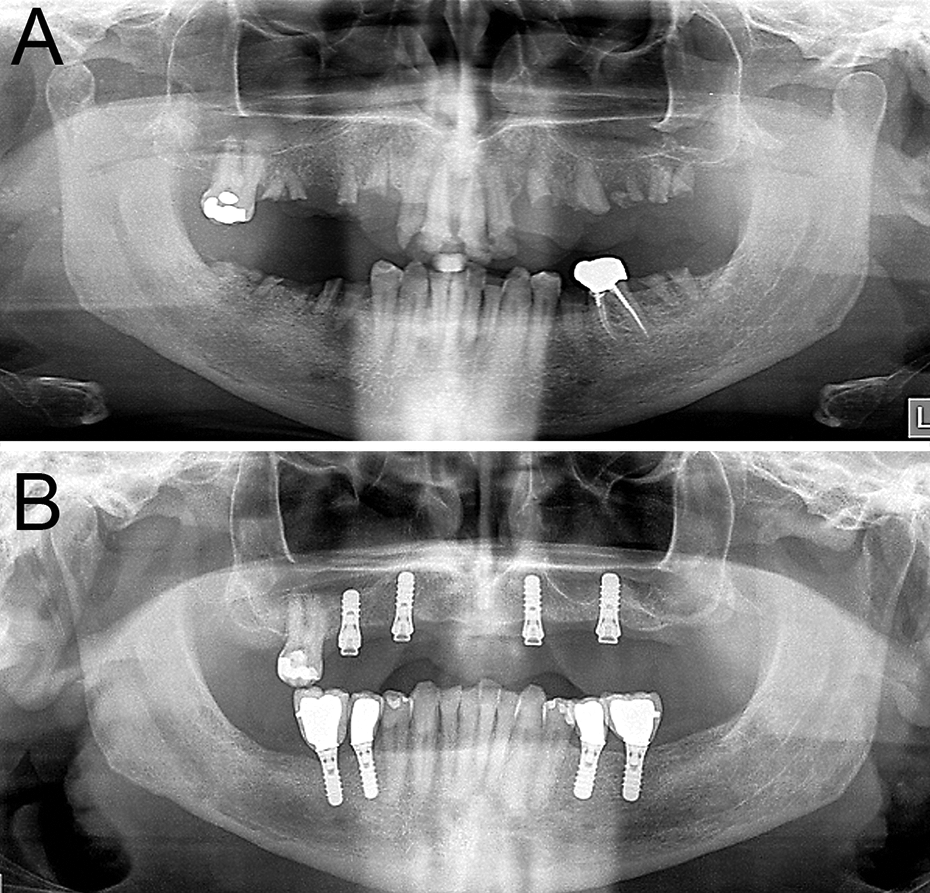
Orthopantomographic findings. A. Status post oral KS ablation prior to dental restoration. B. Status post full mouth reconstruction 2 years after initial presentation.
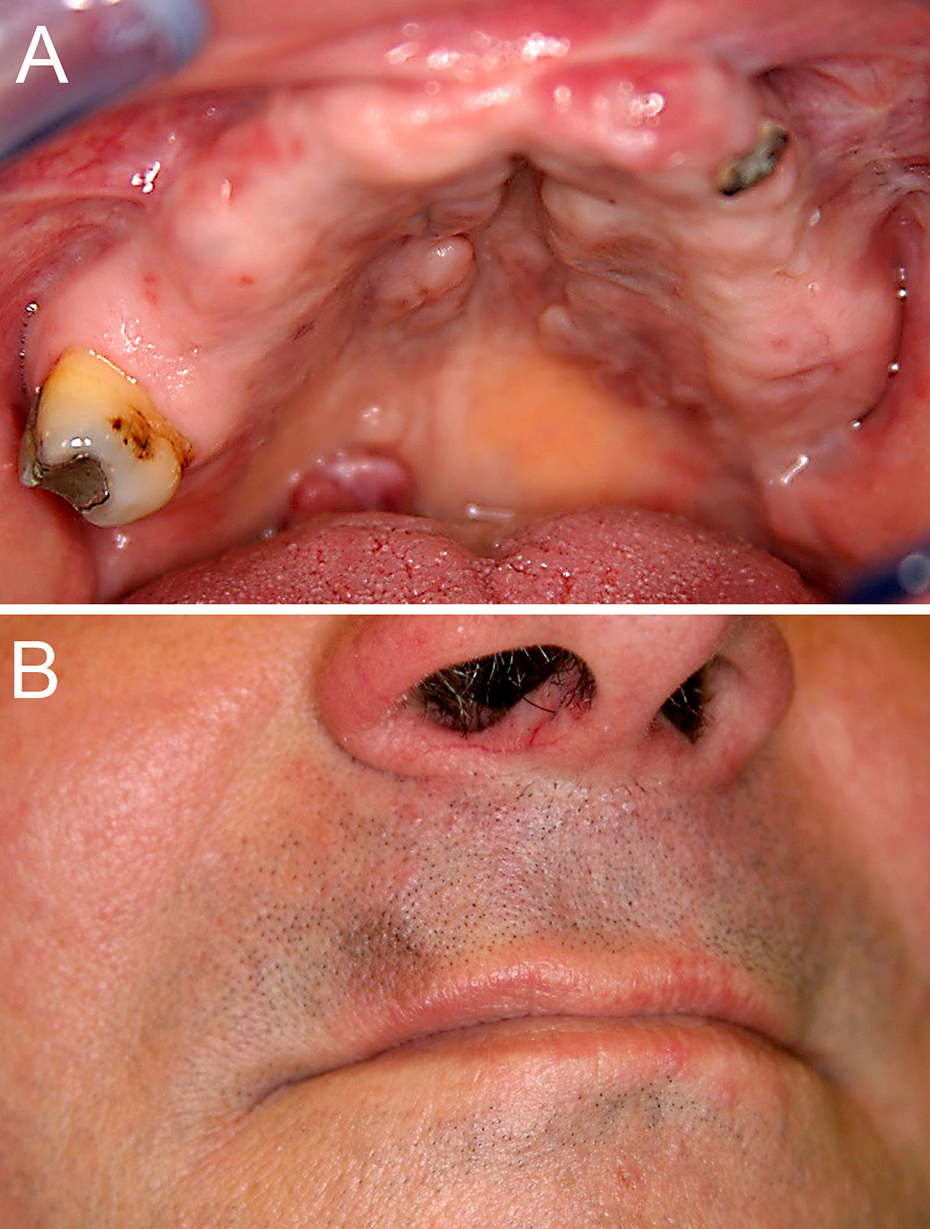
Results during treatment process with cART (1 year after initial presentation). A. Hard palate almost free of oral KS lesions, 1 root tip residue regio 23. B. Tumor on the upper lip almost completely resolved, minor discoloration.
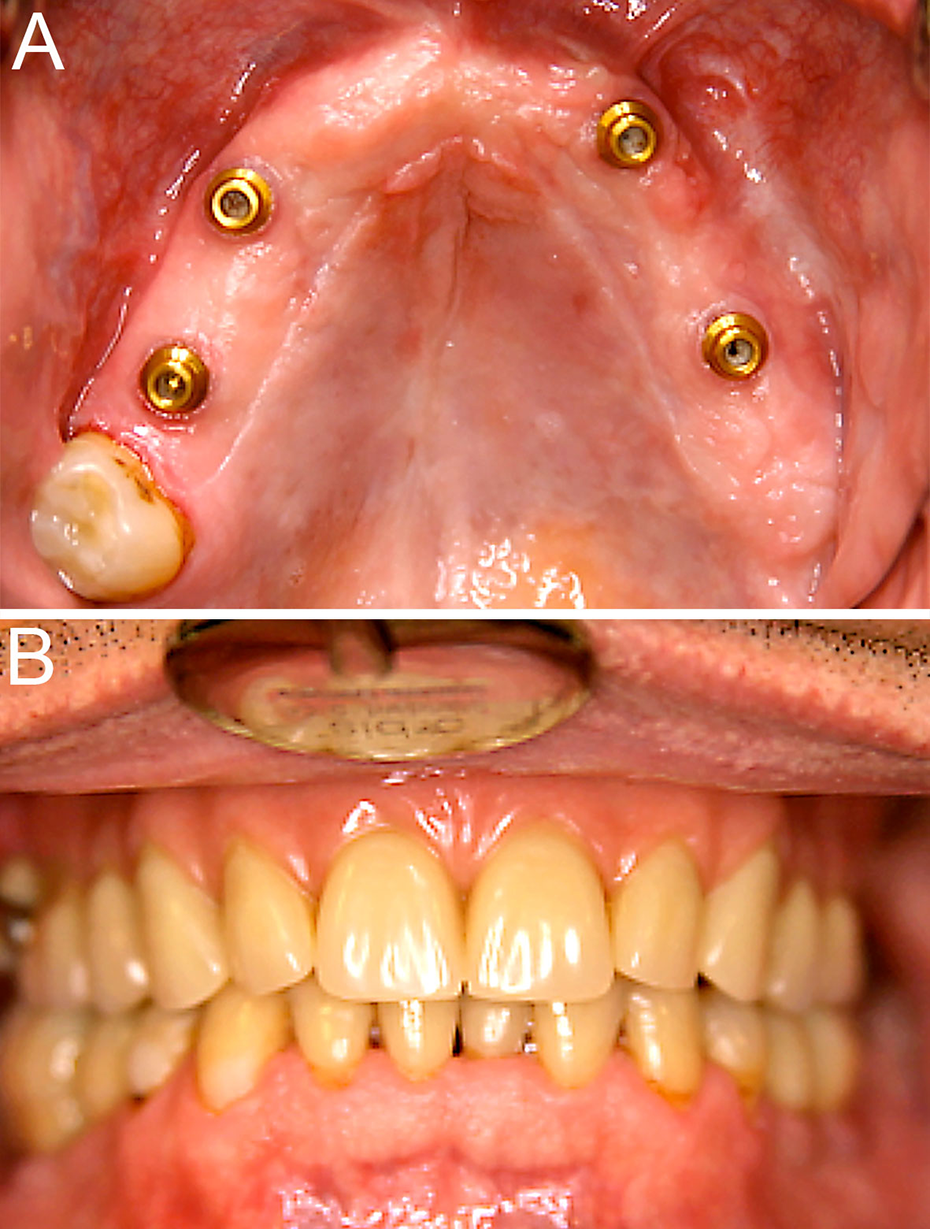
Post treatment results (2 years after initial presentation). A. Hard palate free of oral KS lesions, 4 maxillary (and 4 mandibular) titanium implants. B. Full mouth reconstruction with implant-retained overdenture.
Histopathology
The overview image (40× H&E) of the biopsy of the intraoral tumor mass shows a densely cellular subepithelial tumor consisting of spindle cells with numerous slit-like spaces containing erythrocytes; some ectatic vessels are present at the edge of the lesion (Figure 5A). Spindle-shaped tumor cells (400× H&E) with mild cytologic atypia form slit-like vascular spaces filled with erythrocytes; some tumor cells contain intracytoplasmic eosinophilic hyaline globules (arrow) characteristic of KS (Figure 5B). The globules most likely represent phagocytosed erythrocyte fragments (Figure 5B).
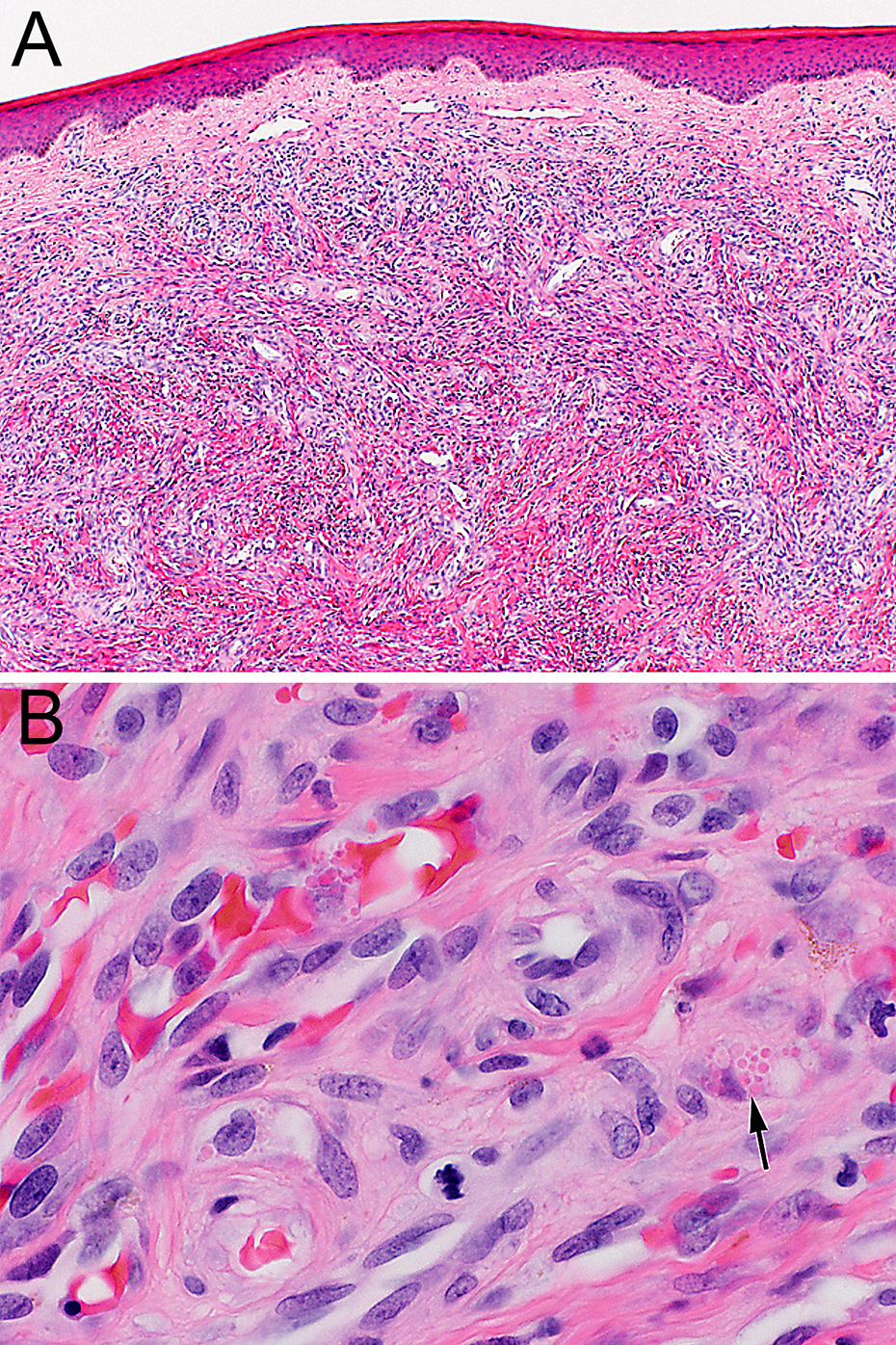
Histopathological findings. (A) Overview image (40× magnification, H&E stain) and (B
Discussion and Conclusions
As demonstrated by this case, HIV-infected patients frequently present with common skin disorders, such as adverse cutaneous drug reactions, which, in the case of aminopenicillins, are increased tenfold when compared to the general population. 6,7 Clinical presentation of KS may vary from single, small, localized cutaneous lesions to extensive and widely disseminated disease, involving the gastrointestinal tract from the oral mucosa to the rectum, and later in the course other viscera. Oral manifestation of KS is associated with higher mortality rates (relative hazard 3.4 [95% CI 1.6–7.1]; p = 0.0011) when compared with cutaneous lesions alone. Oral KS frequently occurs, especially in HIV patients, who show oral involvement in up to 65%. 8,9 With the palate (95%) and gingiva (23%) representing the most commonly affected sites, intraoral lesions as the initial site of manifestation occur in up to 22% of all oral KS patients, 10 and in 77% of all HIV-infected oral KS patients. 11 In 45% of all cases, oral and extraoral manifestations of KS can be found concomitantly. 10
Although not always pigmented oral KS lesions typically appear as brownish-livid, vascular macules progress to nodular growth that result in periodontal disease, loss of teeth, and even alveolar bone destruction later in the course. 12 –15 The condition may also be accompanied by facial lymphedema, another indicator of poor prognosis. 16
As demonstrated by this case, oropharyngeal lesions may grow to sizes that compromise the patient’s airway or impair swallowing. After implementation of cART, practitioners should be especially aware of potentially lethal KS flares as a result of immune reconstitution inflammatory syndrome (IRIS). 17 These cannot accurately be predicted and one should be prepared to undertake appropriate life-supporting measures as soon as any signs and symptoms of IRIS have been recognized. 18 This patient demonstrated an increase in enoral tumorous lesions with the introduction of cART, however, oral KS lesion flare with further airway compromise was avoided by electrosurgical tumor debulking in general anesthesia.
Improved treatment success and management of HIV following the introduction of effective antiretroviral therapies has led to a decreased incidence of KS. 5 Treatment options of KS need to be evolved individually based on the stage of the disease and can include systemic to locoregional therapy. According to the literature, signs of disseminated KS as well as CD4 cell counts are strong predictors for survival, whereas the extent of mucosal or cutaneous involvement is not correlated with prognosis. 19
While treatment with cART, as implemented in this case, has yielded promising response rates in KS, 20 –22 additional treatment with systemic chemotherapy should be considered in rapidly progressive disease or severe cases that include widespread skin lesions, extensive oral and/or visceral manifestation, or IRIS-induced flare of KS lesions. 23 According to the literature, therapy-naive patients show a similar improvement in survival and morbidity with cART, chemotherapy, or cART plus chemotherapy. 24,25 Thus, in this case, it was decided to initially refrain from chemotherapy and await the response to cART.
By identifying 4 prognostic factors (i.e., age, occurrence of KS at or after AIDS onset, presence of co-morbidity, and CD4 cell count), Stebbing et al created a simple prognostic index, ranging from 0 to 15, for AIDS-associated KS. 26 According to this index, low risk patients should initially be treated with cART alone, reserving chemotherapy only for progressive disease.
Angiogenesis plays a crucial role in the development of KS, and represents another therapeutic target. The additional application of anti-angiogenic therapy, for example with Bevacizumab, a monoclonal antibody and VEGF-inhibitor or Captopril, was shown to be advantageous in a subset of patients. 27,28
Although none of the locoregional treatments can prevent the emergence of new tumor lesions, such treatments, including excision surgery, laser therapy, radiation therapy, intralesional chemotherapy, cryotherapy, or photodynamic treatment, serve to control local tumor growth or improve cosmesis, as reviewed by Di Lorenzo et al. 23
Even though cutaneous as well as oral lesions respond well to radiation, the latter should only be used in a restrictive manner in the case of oral KS, where mild (63–66%), moderate (15–18%), or severe (16–22%) toxic mucosal reactions were reported to occur. 29,30 In addition, radiotherapy is not recommended for very acute symptoms because of the relative time delay in response. Similarly, the efficacy of intralesionally delivered chemotherapeutic agents such as vinblastine is not adequate for large, life-threatening lesions in acute cases. 31 Surgical tumor removal may be of particular importance in oral KS when the goal is to obtain an open airway (and to avoid tracheostomy). Moreover, as in the case presented, surgery can be supportive to restore functional swallowing by ablation of the tumor mass. Although Thariat et al and other authors showed that limited excision alone may be sufficient to cure immunocompetent patients, a multimodal treatment regimen should always be initiated for oral KS. 32 –34
In conclusion, understanding the close relation of HIV and HHV8-infection in terms of disease onset and clinical presentation is important to increase awareness of oral KS and ensure subsequent appropriate management of oral KS patients. Clinical staging represents the most important factor for choosing the optimal treatment. The introduction of cART has been proven to be efficient in curing oral KS, while several additional locoregional treatment options, including debulking surgery, may be necessary for symptom relief or to improve cosmesis. Radiotherapy should be applied restrictively for oral KS due to potentially severe toxic mucosal reactions, whereas additional chemotherapy has to be considered in severe cases of oral KS that present with widespread disseminated disease. A multidisciplinary approach to the treatment of functionally and aesthetically impairing oral KS is highly recommended.
Footnotes
Acknowledgment
The authors would like to thank Dr. Selina Ackermann for editorial assistance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
