Abstract
Study Design:
A case report with 2 year follow up.
Objective:
The aim of this paper is to present a case of bilateral TMJ ankylosis with coexisting dentofacial deformity and occlusal cant, and 2 years follow-up evaluation for changes and relapse in the facial skeletal and airway.
Methods:
The patient was planned preoperatively by computer simulation for bilateral interposition arthroplasty and surgical jigs, coronoidectomy, detachment of masseter and medial pterygoid muscles from ramus, LeFort 1 osteotomy, temporary maxillomandibular fixation, counter-clockwise rotation of the maxillomandibular complex, maxillary fixation and iliac crest graft, reconstruction of bilateral TMJ with custom-made total joint prosthesis, dermal fat interposition in the joint, reattachment of muscles, maxillomandibular fixation, and active physiotherapy.
Results:
Average ramal length improved by 28.35 mm (81%) in the immediate postoperative and 25.6 mm (73.45%) at 2 years, showing 2.75 mm (4.4%) vertical bone resorption at the angle region. Point A advanced by 1.3 mm, but showed 4.5% horizontal relapse; Point B advanced by 10.2 mm, but showed 9.5% relapse at 2 years. Pogonion advanced by 26.3 mm (70%) but presented 7 mm (10.9%) horizontal relapse; and menton by 28.6 mm (89%) with 5.4 mm (8.9%) relapse at 2 years. The mean mandibular plane angle decreased by 33.5° (42%) after surgery and by 32° (40%) at 2 years. Pharyngeal airway increased by 49% after surgery and by 75.6% at 2 years follow-up.
Conclusion:
This computer simulated approach for the management of bilateral TMJ ankylosis with facial deformity and occlusal cant improves aesthetics, function and airway in a single surgery, thereby reducing the management cost and time, and deliver precise results.
Temporomandibular joint (TMJ) ankylosis is a debilitating condition that causes restricted mouth opening, and poses difficulty in breathing, mastication, and speech. It is a challenge to correct the facial deformity, obstructive sleep apnea, restore the normal anatomy and function of the joint and prevent reankylosis. During the last 25 years, major advancements have been made in TMJ diagnostics and management to treat and rehabilitate the TMJ. An understanding of the medio-lateral extent of the ankylotic chunk, the safety zone toward the cranial base, approximation of the nearby vessels and their safe distance, if needed through CT angiography, prevent any damage to the adjacent internal maxillary artery.
Computer-assisted surgical simulation (CASS) is a helpful tool in achieving accuracy in many maxillofacial surgical applications, including dentofacial deformities, acquired traumatic or pathological defects. Virtual surgery using CAD CAM allows the surgeon to attempt the TMJ arthroplasty, virtually position the TMJ total joint replacement (TJR) prostheses, and transfer the osteotomy cuts in the planned positions in the operation theater, allowing an accurate snap fit of the prosthesis. CASS enabled TMJ reconstruction with patient-specific TMJ TJR has significantly improved the quality of treatment, by reducing the surgical time and enhancing the accuracy of orthognathic surgical procedures. 1
The aim of this paper is to present 2 years follow-up of a case of bilateral TMJ ankylosis with coexisting dentofacial deformity and occlusal cant, managed in a single stage surgery by computer-aided surgical simulation, counter-clockwise rotation of maxillomandibular complex, customized joint reconstruction, to assess the changes and relapse in the facial skeletal and airway.
Case Presentation:
A 22 year old young girl visited our outpatient clinic with a chief complaint of small lower jaw, retruded chin and limited mouth opening for the last 15 years. After institutional ethical approval she was included in the study. She presented a history of being apparently asymptomatic 15 years back when she met with trauma due to fall from height. After a few days of trauma, she was noted with reduced mouth opening for which she visited some nearby private hospital and was managed conservatively by medication. After few months, her mouth opening reduced gradually to nil. She underwent ankylosis release surgery for limited mouth opening at a nearby hospital 2 years back, and visited us for her facial deformity correction.
She presented with a retruded mandible, a vertically deficient lower third of face and a retrognathic chin with limited mouth opening of 2 cm maximum and obstructive sleep apnoea. She was examined radiographically through CT scans of mandible, maxilla, TMJs with 1 mm cuts, which demonstrated bilateral TMJ ankylosis with a short posterior maxillary vertical height. These Digital Imaging and Communications in Medicine (DICOM) images were converted to Standard Tessellation Language (STL) with the help of a software (Imprint, Materialise). Dental models were prepared from dental impressions and scanned via a lab scanner, and their STL files were incorporated in the patient’s virtual model. She was virtually planned on Proplan, Materialise software for surgery according to Movahed and Wolford’s protocol 2 that included resection of ankylotic chunk, coronoid process, fixation of TMJ TJR with Le Fort 1 osteotomy and counter-clockwise rotation (CCWR) of maxillomandibular complex. (Figure 1A to D) to correct the associated deformity. The surgical jigs were designed on freeform geomagic software (Figure 1E) and printed in dental resin using Formlabs 3D printer (Figure 1F to H). The customized TMJ TJR implants were simulated for their loading scenarios in Ansys software to understand the structural integrity of the implant for different loading conditions. 3
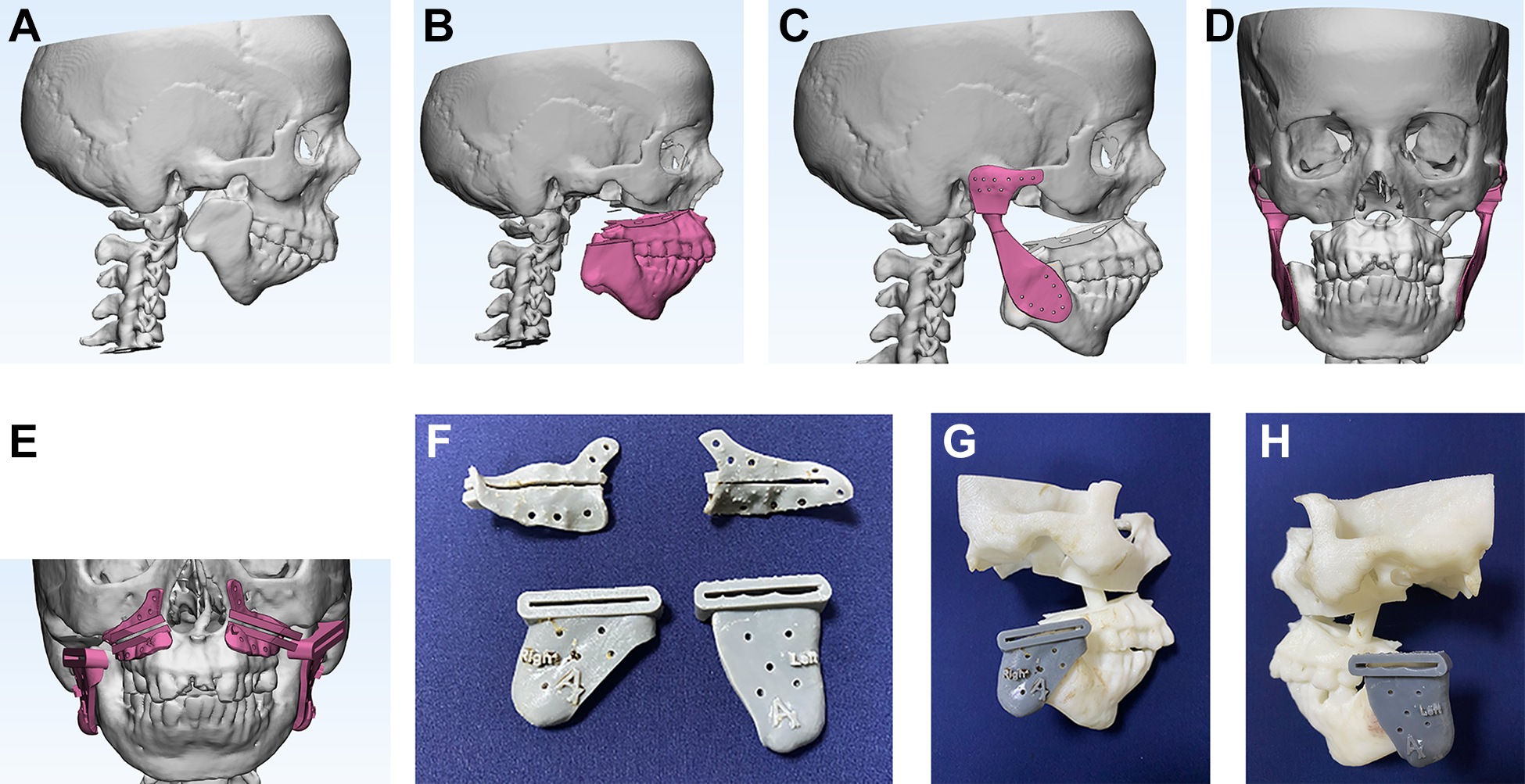
A. Pre-op 3D CT. B. Surgical planning with counter-clockwise maxillomandibular rotation. C. Customized TMJ TMJR with counter-clockwise maxillomandibular rotation. D. Bilateral customized TMJ TMJR. E. Designing of Maxillary and mandibular jigs. F. 3D printed maxillary and mandibular jigs. G. Right jig placed on model. H. Left jig placed on model.
Surgical Procedure:
After surgical preparation and draping under general anesthesia, the ear canals were gently packed with cotton gauze. Exposure of the TMJ was done through Alkayat & Bramley incision. The designed surgical jigs were seated onto the ramus through retromandibular incision after stripping the pterygomasseteric sling, masseter and medial pterygoid muscles and the planned osteotomy was marked. Coronoidectomy was performed from the anterior aspect of the coronoid into the sigmoid notch, using a retractor medial to the coronoid to protect the soft tissues while cutting. The same procedure was followed on the other side.
A standard LeFort I osteotomy was performed using the printed jigs. Temporary maxillomandibular fixation was done before mobilizing the maxillomandibular complex in a downward and forward direction. Maxilla was rotated counter-clockwise as planned and fixation was done using 4 plates and screws at the buttresses (Figure 2A to D). Iliac crest bone graft was used to cover the surgical defect created after maxillary rotation. The customized glenoid fossa and TMJ TJR were then inserted and fixed with more than 5 screws. After thorough irrigation with betadine solution, the masseter and medial pterygoid muscles were reattached to the mandible. Abdominal fat graft harvested through a suprapubic incision, was packed around the articulating area and the incisions were closed in layers.
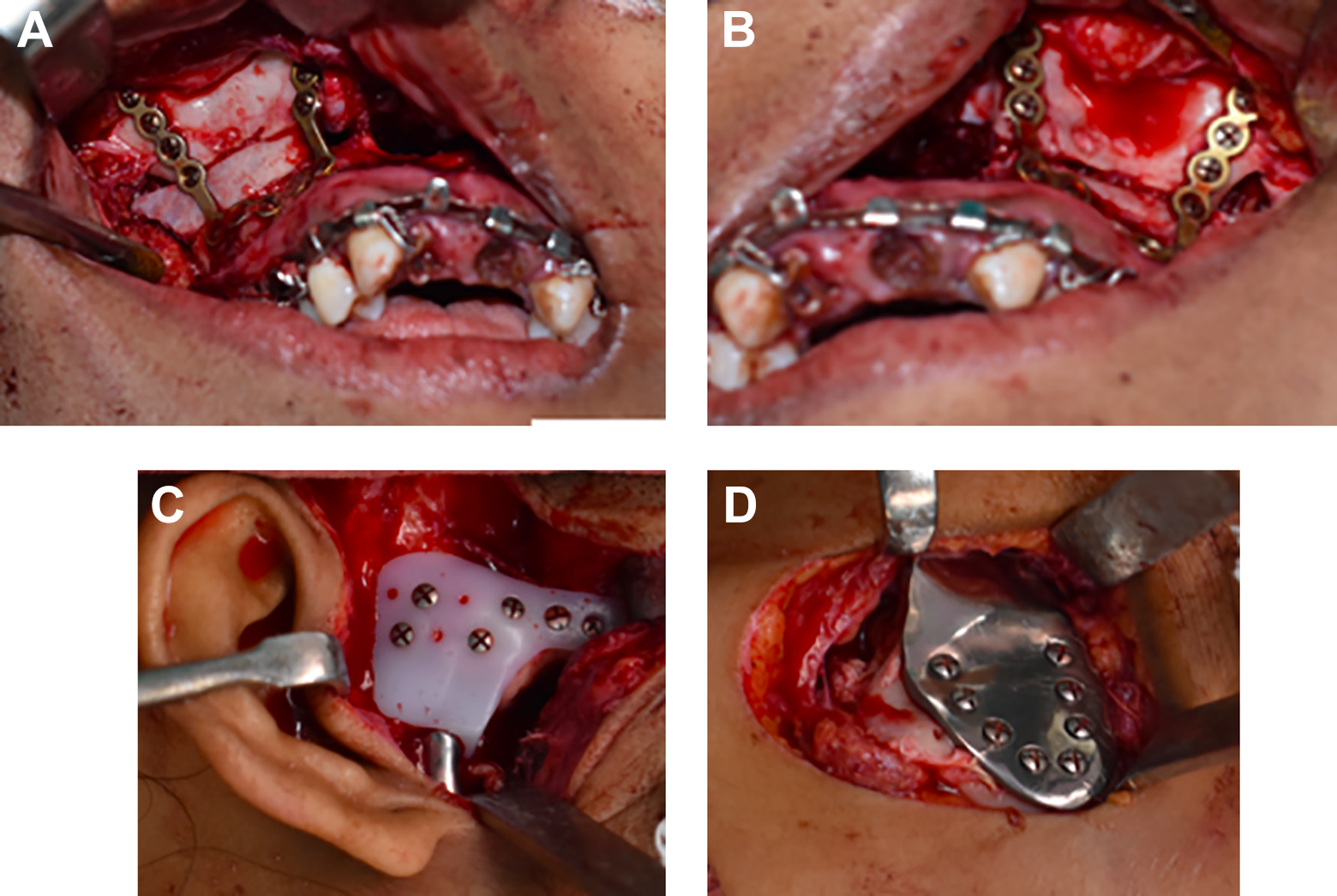
A. Le Fort I osteotomy, bone grafts, and fixation (right). B. Le Fort I osteotomy, bone grafts, and fixation (left). C. Customized glenoid fossa in position. D. Customized condylar head with ramal extension.
Orthopantomogram was done postoperatively (Figure 3). Intermaxillary fixation was recommended for at least 2 weeks for the masticatory muscles to get reattached. CT scan was done in the immediate postoperative week. Figure 4A and B present her preoperative images and Figure 4C and D present her 2 years postoperative images and mouth opening.
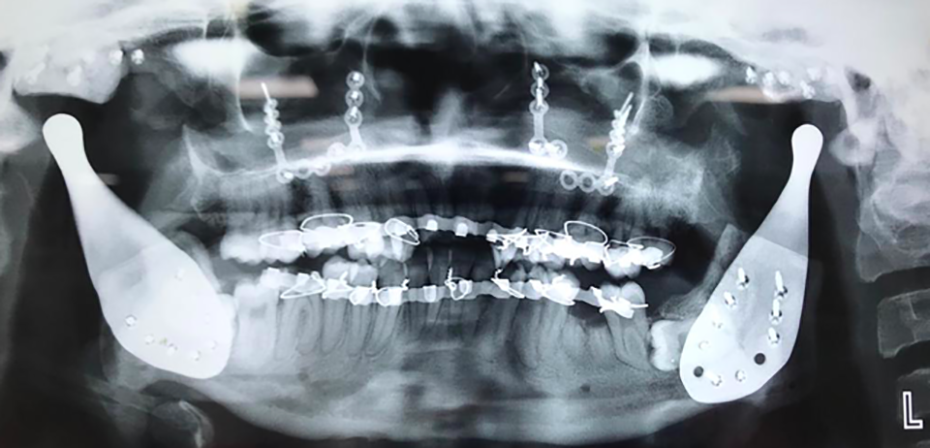
Postoperative orthopantomogram showing both TMJR.
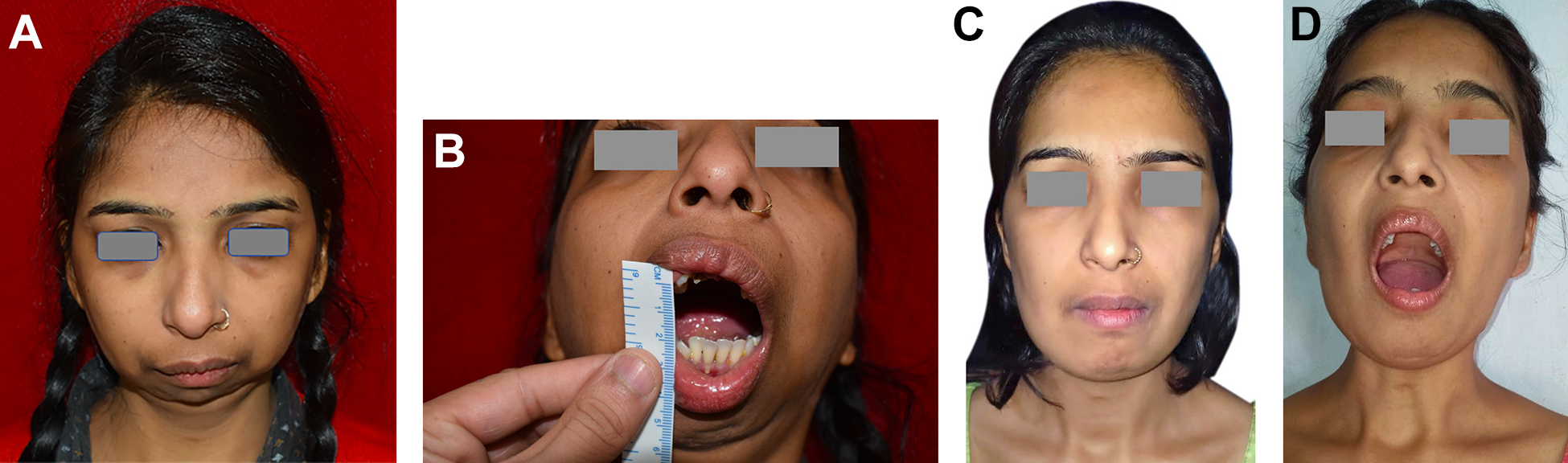
A. Preoperative front view of the patient. B. Preoperative mouth opening. C. Two years postoperative front view of the patient. D. Postoperative mouth opening at 2 years follow-up.
Postoperative Assessment:
Patient was followed up for 2 years, and her postoperative CT scan was repeated. All 3 CT scans were superimposed and changes were analyzed (Figure 5A to C). Cephalometric measurements were recorded from each of the CT data. Frankfort horizontal plane (FHP) 4 was created from Porion (P) to Orbitale (Or), and perpendicular to this, a vertical plane (VP) was created passing through both the porions. Horizontal distances were measured in mm from this vertical plane to point A, point B, Pogonion (Pg), Menton (Me) and Gonion (Go) (Figure 5D). Bilateral ramal lengths, intergonial width, SNA, 5 SNB, ANB, occlusal plane, palatal plane, gonial angles, and mandibular plane angles were measured.
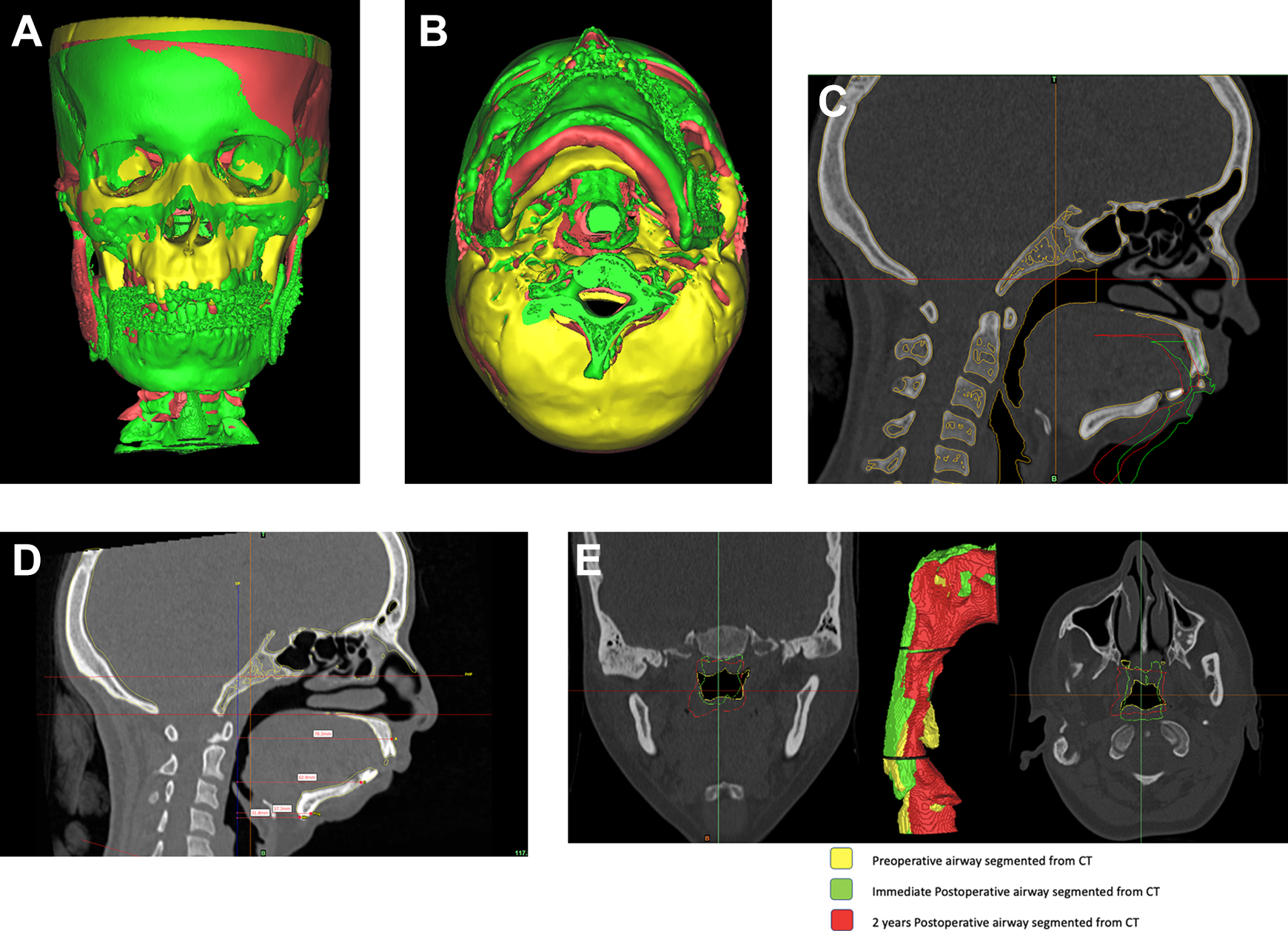
Overlapped preoperative (yellow), immediate postoperative (green) and 2 years postoperative (red) 3D CT images for comparison. (A) Front view, (B) bottom view, (C) sagittal view, (D) variables assessed on CT, (E) preoperative airway (yellow) with superimposed postoperative (green) and 2 years postoperative (red).
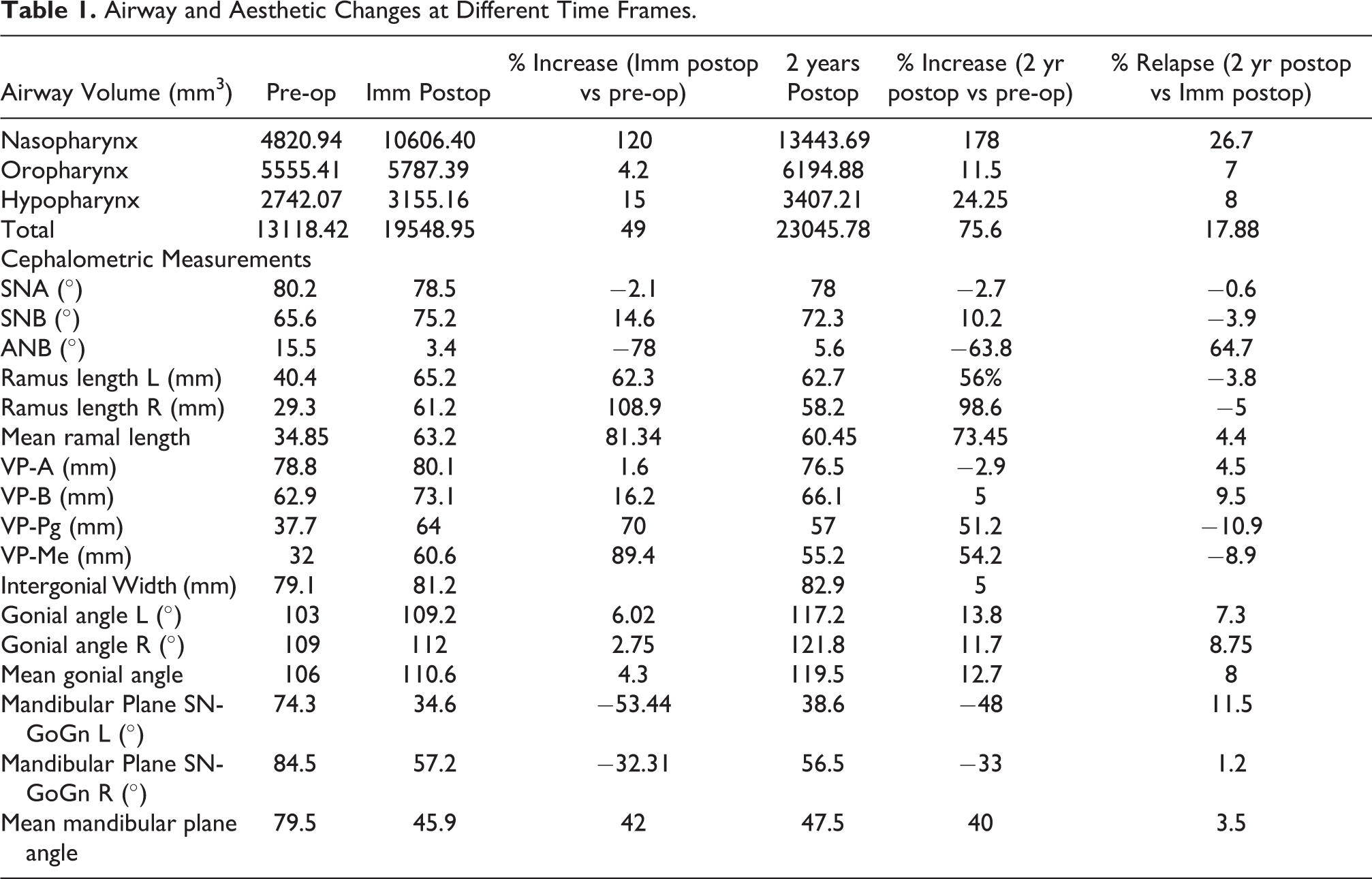
SNA decreased by 2.1%, while SNB increased by 14.6% and ANB decreased by 78%. There was a relapse of 0.6% at SNA and 3.9% at SNB at 2 years follow-up (Table 1). Average ramal length improved by 28.35 mm (81%) in the immediate postoperative and by 25.6 mm (73.45%) at 2 years postop, showing 2.75 mm (4.4%) vertical bone resorption at the angle region.
Airway and Aesthetic Changes at Different Time Frames.
There was a very slight change in the position of point A (1.3 mm advanced), but it was 10.2 mm at point B (16.2%). At 2 years follow-up, point A showed 4.5% horizontal relapse and point B showed 9.5% relapse. The counter-clockwise maxillomandibular rotation allowed pogonion to advance by 26.3 mm (70%) while menton point advanced by 28.6 mm (89%). There was some resorption noted in the symphysis region, maybe because of the soft tissue pressure leading to a 10.9% relapse in the chin at pogonion and 8.9% at menton point.
Postoperatively, the mean gonial angles increased by 4.3% in the immediate postop phase, and finally 12.7% at the 2 years follow-up. An increase of about 5% was seen in the intergonial width at 2 years.
The mean mandibular plane angle decreased to 33.5° (42%) in the immediate postop phase, and 40% at the 2 years follow-up, showing a relapse of 3.5%, due to remodeling of bilateral angles and resolution of the antegonial notches.
Pharyngeal airway changes were assessed by superimposing the preoperative pharyngeal airway with the 2 postoperative airways segmented from respective CT scan data set (Figure 5E). Airway volume was measured as nasopharyngeal, oropharyngeal and hypopharyngeal airway as described by Giralt-Hernando et al. 6 Nasopharynx was measured from soft tissue pharyngeal wall at the level of FHP-PNS-Sphenoid bone, oropharynx up to most anterior point of C3, and hypopharynx up to soft tissue pharyngeal wall FH-PNS parallel to most anterior pole of body of C4 at an automatic threshold set for pharyngeal airway. Pharyngeal airway was seen to increase by 49% immediate postoperatively and by 75.6% at 2 years follow-up. The nasopharyngeal, oropharyngeal and hypopharyngeal airway increased to 120%, 4%, 15% respectively in the immediate postoperative phase and 178%, 11.5% and 24% at 2 years follow-up, showing a total relapse of 17.88 in the posterior pharyngeal airway, with 26.7% relapse in nasopharyngeal airway, 7% in oropharyngeal airway and 8% in hypopharyngeal airway (Table 1).
Although a slight asymmetry was observed, the patient was very satisfied with the postoperative facial aesthetics, and jaw function. Comparison was made between the previous planned and postoperative Standard Tessellation Language (.STL files), which demonstrated 98.8% accuracy. However, the 2 years follow-up showed resorption in the chin prominence, indicating a need for sliding genioplasty both for improving chin prominence and correction of the slight asymmetry observed.
Discussion:
The standard protocol for management of TMJ ankylosis by Kaban 2009 includes 7 steps. 7 Cases with associated facial deformity are either managed by a Le Fort I osteotomy and its inferior positioning ipsilaterally or bilaterally for correction of occlusal cant along with inverted L osteotomy of ramus or with pre-arthroplastic mandibular or maxillomandibular distraction osteogenesis (DO). 8 –11
Use of stock Biomet TMJ TJR with simultaneous correction of the facial deformity using Le Fort I osteotomy guided by digital templates has been studied, 12,13 but with reported problems of poor fit due to its straight design, making its perfect adaptation difficult. In other words, it is the recipient bone which has to be modified to fit the prosthesis instead of the prosthesis fitting the bone. 14 Distorted anatomy as in TMJ ankylosis makes it even more difficult to achieve a stable reconstruction with the stock TMJ TJR, resulting in its micromotion.
In contrast, a customized TMJ replacement unit intraoperatively readily fits to its planned position, saving on the surgical time, needs less manipulation and thereby allows faster healing. Such individualized prostheses, combined with abdominal free fat graft to prevent heterotopic bone formation in the reconstructed joint. 14 Wolford et al 15 in their 20-year follow-up study of 56 patients of Techmedica total joint prostheses, found statistically significant improvements in incisal opening, jaw function, TMJ pain, and diet, with 85.7% patients reporting significant improvement in their quality of life.
Selective modification of the occlusal plane may be required in patients with either an high occlusal plane (HOP) or low occlusal plane (LOP) to re-establish proper jaw function and better esthetics. 16 Surgical decrease of occlusal plane, decreases the mandibular plane, increases the inclination of upper incisors but decreases that of the lower incisors, causing anterior rotation of pogonion, posterior movement of the paranasal region, increases the posterior facial height, and upper airway to around 40% of the total mandibular advancement. We observed an increase of 49% in the airway in the immediate postoperative phase and 75.6% at 2 years postoperative.
The correction of LOP facial type by clockwise rotation of the maxillomandibular complex (downward and backward rotation) is a well-accepted technique. However, counter-clockwise rotation CCWR (upward and forward rotation) for the correction of HOP facial type has not been supported as an acceptable treatment modality for questionable postsurgical stability due to increased posterior facial height; causing stretching of the suprahyoid, pterygoid, and masseteric muscles; and adverse effects on the TMJs. This instability can be overcome by use of rigid fixation of the mobilized segments. We observed a horizontal relapse of 10.9% at pogonion and 8.9% at menton at 2 years follow-up.
Wolford demonstrated significant and positive effect of CCWR of the maxillomandibular complex on the oropharyngeal airway and the facial balance. 1 When studied in 47 female patients with irreversible end-stage TMJ pathology and co-existing dentofacial deformity, it led to a stable and immediate increase in the oropharyngeal dimension. 15 We also observed an increased nasopharyngeal, oropharyngeal and hypopharyngeal airway by 120%, 4%, 15% respectively in the immediate postoperative phase and by 178%, 11.5% and 24% at the 2 years follow-up. Nasopharyngeal airway volume improved the most with the maxillomandibular counter-clockwise rotation not only in the immediate postoperative phase but continued to improve with mandibular function and restoration of normal pattern even in the 2 year follow-up.
Concomitant custom-made TMJ TJR, CCWR and simultaneous maxillary osteotomies could significantly improve patients’ pain, dysfunction, deformity, and airway problems in a single surgery when performed in end-stage TMJ disease. 17,18
CASS improves surgical accuracy by transferring the presurgical virtual plan to the operative site through surgical splints. 19,20 The protocol to perform TMJ arthroplasty and orthognathic surgery as a single operation in cases of TMJ disorders was proposed by Movahed and colleagues. 2 They performed virtual surgical simulation in 7 TMJ ankylosis patients with mandibular deformities, and the mean difference between the virtual plan and actual results ranged from 0.64 ± 0.20 to 1.90 ± 0.85 mm, with satisfactory changes in the facial profile, postoperative pharyngeal airway and mouth opening. 21 In our case, the mean difference between the virtual plan and actual results was also in the same range.
The advantages of concomitant TMJ TJR & CCWR in cases with TMJ pathology and dentofacial deformities have been listed as 1) 1 operation and general anesthetic; 2) balances occlusion, TMJ, and neuromuscular structures at the same time; 3) decreases overall treatment time 4) eliminates unfavorable TMJ sequelae when correcting the deformity alone and 5) avoids iatrogenic malocclusion when performing TMJ surgery alone. 1 The single stage TMJ TJR & CCWR serves as a “low-cost approach” as it saves on the cost of a second surgical intervention, and no additional loss of work hours due to the second surgery.
Conclusion
CASS enabled single stage surgery allows designing of customized joints, perform multiple surgeries in a single sitting with improved quality of treatment, enhanced accuracy of surgical results, improved airway, function and better aesthetics, thereby reducing the management cost and time.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Department of Health Research, multidisciplinary unit, DHR Human resource development grant 12016/07/2017-H and Anatomiz 3D.
